Transverse Terminal
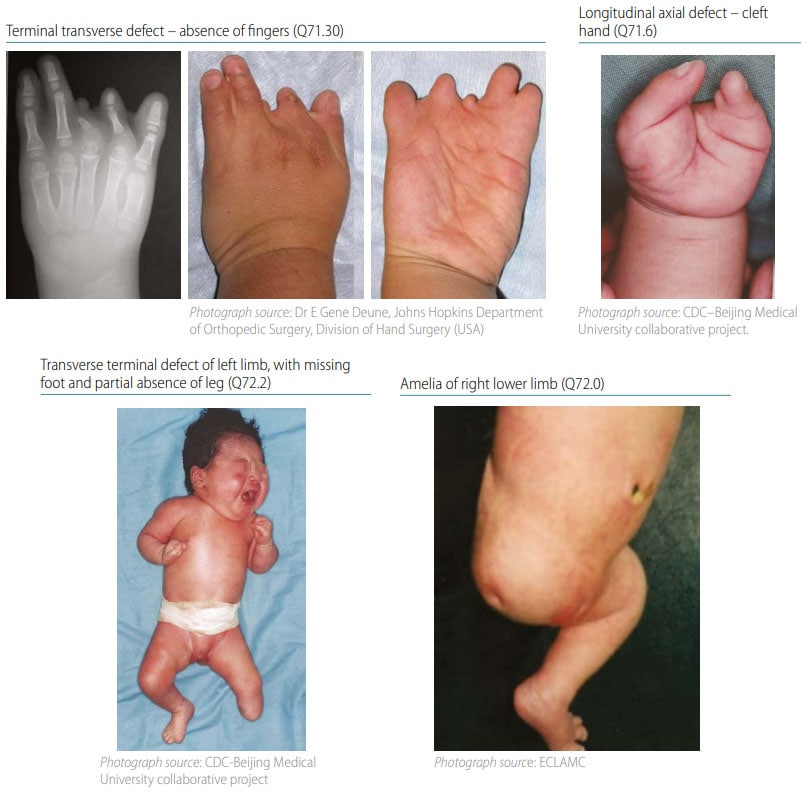
Terminal transverse limb deficiency is a congenital anomaly that appears as an “amputation” of an arm, leg, or digit/toe. The limb is missing the terminal (distal) segment(s), with preservation of all the segment(s) proximal to the missing segment (see Fig. 38). For example, if fingers are missing, the remainder of the hand, forearm and arm are all still present. Radiographs are strongly recommended and can be essential to confirm the condition and characterize the bony anatomy.
Fig. 38. Transverse terminal
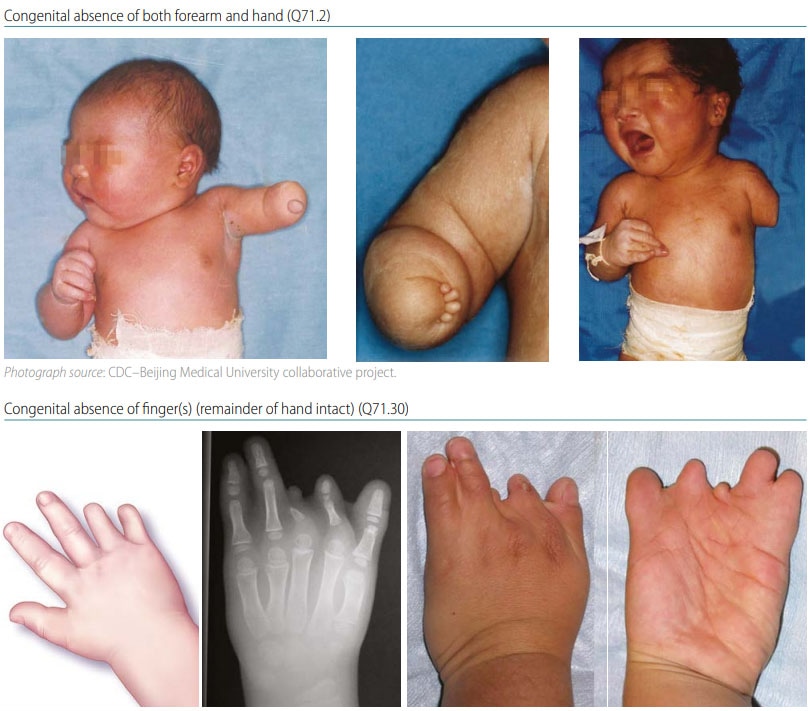
Photograph and x-ray source: Dr E. Gene Deune, Johns Hopkins Department of Orthopedic Surgery, Division of Hand Surgery
Diagnosis
Prenatal. Transverse terminal limb defects can be suspected prenatally but can easily be missed or misdiagnosed. Cases identified or suspected prenatally should be confirmed postnatally before inclusion in a surveillance programme.
Postnatal. The newborn examination, aided by radiographs, confirms the diagnosis of terminal transverse limb deficiencies and distinguishes it from other limb reduction defects. It is important to underline the importance of a detailed examination and documentation, including imaging (photographs and radiographs).
Clinical and epidemiologic notes
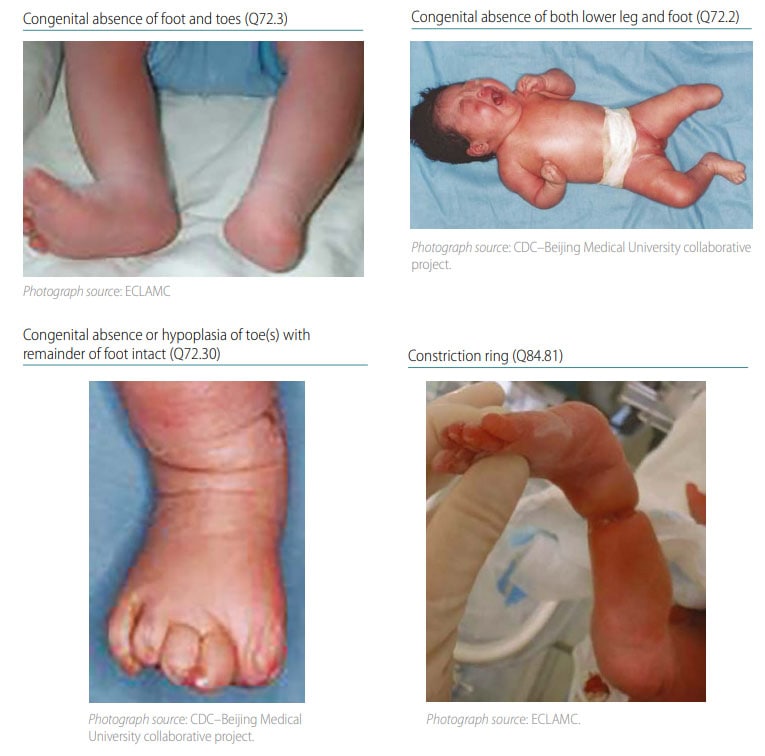
Terminal transverse deficiency includes a wide spectrum of limb deficiencies, with partial amputation of the distal limb. The terminal partial amputation can involve digits, toes, forearm, arm, leg, or thigh. Transverse deficiencies are the most common of the limb deficiencies.
- Most cases of terminal transverse deficiency occur sporadically as an isolated abnormality of one hand or foot in an otherwise healthy individual.
- Some cases of terminal transverse defects have been attributed to instances of “early amnion rupture disruption sequence”, also referred to as amniotic bands. The damage attributed to amniotic bands ranges from constriction of a limb to hypoplasia of digits with syndactyly, rudimentary digits, and absence of the limb distally from the site of the in utero amputation. Amniotic bands can also cause disruptions at other sites, such as the face and body wall.
- In cases of terminal deficiencies that involve the hand, proper digits are absent but the presence of small soft tissue nubbins arranged in a pattern suggest rudimentary digits.
- Transverse limb deficiency is seen in Adams–Oliver syndrome, a genetic condition with features that also include aplasia cutis congenita and other anomalies (e.g. congenital heart disease, brain calcifications).
- Transverse limb deficiency has been observed after maternal exposure to the medication misoprostol, taken to induce abortion.
- Make sure that the distal part of the limbs is affected and that proximal segments are present.
- Transverse terminal limb defects look like an amputation – the affected limb segment often ends abruptly, without any obvious relation to anatomical boundaries.
- Distinguish terminal deficiency from amelia (complete absence of the limb), and from “split hand” when the transverse terminal defect affects the central digits (see Fig. 39).
- If possible, take and attach radiographs, as these are very useful to confirm and describe the bony anatomy, thus characterizing precisely the level of the amputation and which specific bones are involved (i.e. missing).
- Look for and note the presence or absence of specific findings that can be associated with transverse limb deficiency, such as soft tissue nubbins, constriction rings, or amniotic bands.
Checklist for high-quality reporting
| Transverse Terminal Defects – Documentation Checklist |
Describe in detail, including:
|
Fig. 39. Distinguishing transverse terminal defects from longitudinal axial defects and amelia (side-byside comparison)