4.9f Limb Deficiency: Longitudinal Preaxial (Tibia, Radius, First Ray) (Q71.31, Q71.4, Q72.31, Q72.5)
Fig. 4.39. Longitudinal preaxial
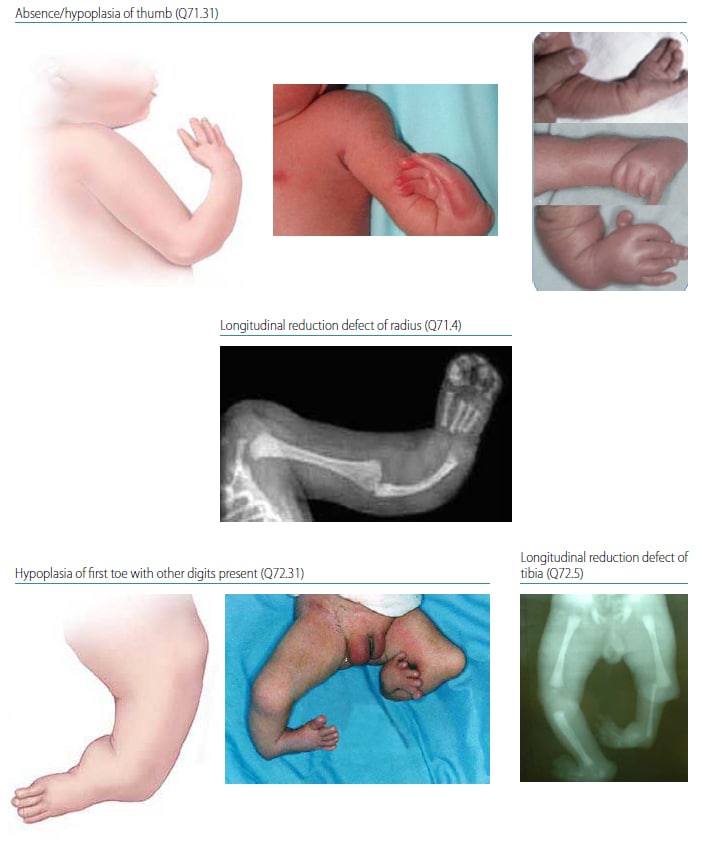
Preaxial limb deficiency is characterized by the absence or hypoplasia of the “preaxial” segments (those on the side of the thumb or big toe side) of the upper or lower limb (see Fig. 4.39). Preaxial limb deficiencies include:
- hypoplasia/absence of the thumb (sometimes of the second finger)
- hypoplasia/absence of the radius
- hypoplasia/absence of the big toe (sometimes of the second toe)
- hypoplasia/absence of the tibia.
Radiographs are strongly recommended to confirm the diagnosis and characterize the bone anatomy.
Relevant ICD-10 codes
Q71.31 Absence or hypoplasia of thumb (other digits intact)
Q71.4 Longitudinal reduction defect of radius
Clubhand (congenital)
Radial clubhand
Absence of radius
Q72.31 Absence or hypoplasia of first toe with other digits present
Q72.5 Longitudinal reduction defect of tibia
Absence of tibia
Note: Avoid using the generic Q71, Q72 or Q73 codes for longitudinal preaxial limb deficiencies. These generic codes include other limb deficiencies.
Diagnosis
Prenatal. Longitudinal preaxial limb deficiencies might be diagnosed or strongly suspected prenatally. However, they can be missed. Moreover, the distinction from other limb deficiencies might be difficult and error-prone. For this reason, a prenatal diagnosis should always be confirmed postnatally.
When this is not possible (e.g. termination of pregnancy or unexamined fetal death), the programme should have criteria in place to determine whether to accept or not accept a case based solely on prenatal data.
Postnatal. The newborn examination can identify a longitudinal preaxial limb deficiency and distinguish it from other limb deficiencies (e.g. longitudinal postaxial defects). An accurate and complete diagnosis requires a detailed physical examination aided by radiography to characterize completely the bony anatomy.
Clinical and epidemiologic notes
Radial deficiency is often associated with hypoplasia or aplasia of the thumb and a bowing of the ulna (so-called radial club hand, angulated to the radial side of the wrist). Isolated thumb hypoplasia or triphalangeal thumb is the mildest manifestation of a preaxial deficiency.
Radial deficiencies are commonly associated with other anomalies such as in the VATER/VACTERL association, as well as several genetic syndromes. Some possible genetic diagnoses include trisomy 18, Fanconi anaemia, Holt-Oram syndrome and TAR syndrome. Of note, several genetic conditions with radial deficiency present also haematologic abnormalities (Diamond-Blackfan anaemia, Fanconi anaemia, TAR syndrome), some of which can be suspected with simple blood tests (although normal findings do not exclude the diagnosis).
Thalidomide and valproate are known teratogens associated with longitudinal preaxial defects (as well as other types of limb deficiency).
Longitudinal preaxial defects of the lower limb include absence or hypoplasia of the first toe with or without hypoplasia or absence of the tibia. Tibial deficiencies are less common than radial deficiencies. They are often associated with equinovarus deformities, and there might be fibular hypoplasia/aplasia. Tibial deficiencies occur most often as an isolated, unilateral malformation with the fibula present.
Absence of the tibia and preaxial polydactyly of the first toe is more common among infants of diabetic mothers. Absence of the tibia is also part of the spectrum of skeletal effects produced by exposure to thalidomide. The affected child would usually have other skeletal and visceral anomalies.
Prevalence of preaxial limb deficiencies is around 0.75 per 10 000 births. It is the second most prevalent limb deficiency subtype, after transverse terminal defects.
Inclusions
Q71.3 Absence or hypoplasia of thumb
Q71.4 Longitudinal reduction defect of radius
Q72.31 Absence or hypoplasia of first toe with other digits present
Q72.5 Longitudinal reduction defect of tibia
Related codes
Q87.20 Holt-Oram syndrome
Q87.25 Thrombocytopenia absent radius syndrome
Q87.26 VACTERL association
Q86.82 Congenital malformations due to thalidomide
Q91.0–Q91.2 Trisomy 18
D61.0 Fanconi anaemia with absent radius
Exclusions
Q71.5 Longitudinal reduction defect of ulna
Q72.6 Longitudinal reduction defect of fibula
Q71.6 Congenital cleft hand
Q72.7 Split foot
Checklist for high-quality reporting
| Longitudinal Preaxial Defects – Documentation Checklist |
Describe in detail, including:
|
Suggested data quality indicators
| Category | Suggested Practices and Quality indicators |
| Description and documentation | Review sample for documentation of key descriptors:
|
| Coding |
|
| Clinical classification |
|
| Prevalence |
|
| Key visuals | Distinguishing longitudinal preaxial defects from longitudinal postaxial defects (side-by-side comparison):
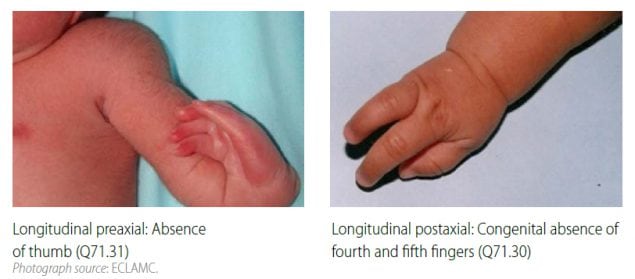 |