4.2 Congenital Malformations of the Nervous System: Neural tube defects
Congenital anomalies of the nervous system: Neural tube defects
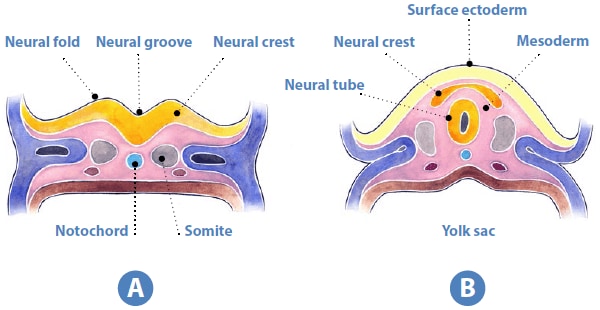
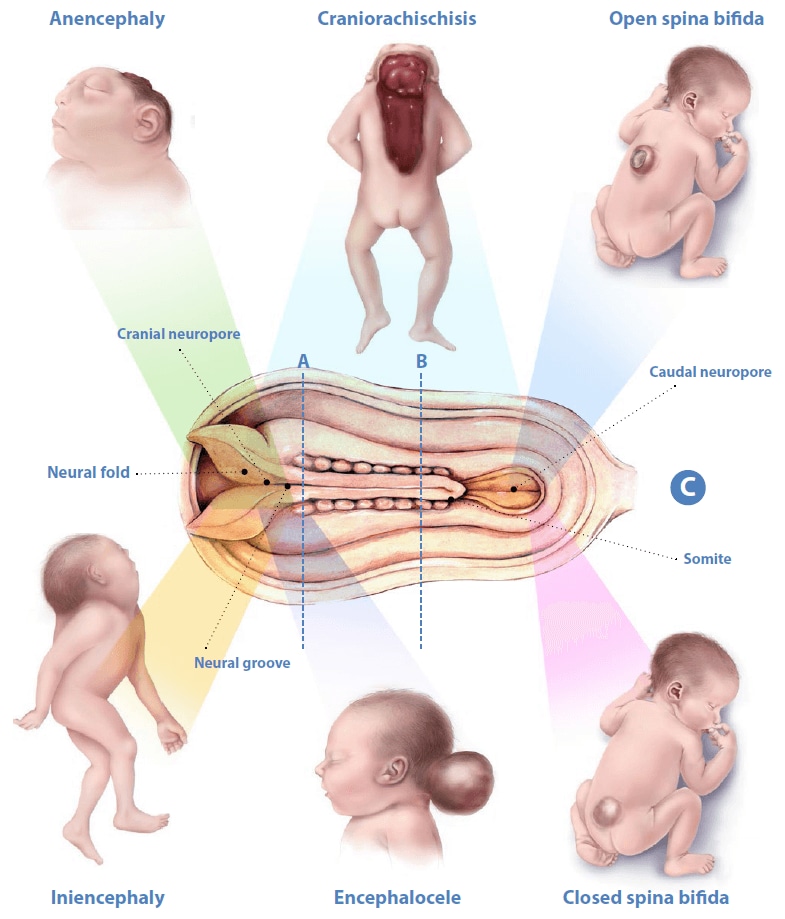
Neural tube defects affect the brain and spinal cord, and are among the most common of the congenital anomalies (see Fig. 4.1). Panel A shows a cross section of the rostral end of the embryo at approximately three weeks after conception, showing the neural groove in the process of closing, overlying the notochord. The neural folds are the rising margins of the neural tube, topped by the neural crest, and demarcate the neural groove centrally. Panel B shows a cross section of the middle portion of the embryo after the neural tube has closed. The neural tube – which will ultimately develop into the spinal cord – is now covered by surface ectoderm (later, the skin). The intervening mesoderm will form the bony spine. The notochord is regressing. Panel C shows the developmental and clinical features of the main types of NTDs. The diagram in the centre is a dorsal view of a developing embryo, showing a neural tube that is closed in the centre but still open at the cranial and caudal ends. The dotted lines marked A and B refer to the cross sections shown in panels A and B. Shaded bars point to the region of the neural tube relevant to each defect.
The most prevalent types of NTDs are anencephaly, encephalocele and spina bifida. In anencephaly, the absence of the brain and calvaria can be total or partial. Craniorachischisis is characterized by anencephaly accompanied by a contiguous bony defect of the spine and exposure of neural tissue. In open spina bifida, a bony defect of the posterior vertebral arches (in this case, the lower thoracic vertebrae) is accompanied by herniation of neural tissue and meninges and is not covered by skin. In iniencephaly, dysraphia in the occipital region is accompanied by severe retroflexion of the neck and trunk. In encephalocele, the brain and meninges herniate through a defect in the calvaria. In closed spina bifida, unlike open spina bifida, the bony defect of the posterior vertebral arches (in this case, the lumbar vertebrae), the herniated meninges and neural tissue are covered by skin.