Healthcare-Associated Fungal Meningitis:
Information for Patients
If you are at risk for fungal meningitis, go to the emergency room (ER) right away for testing, even if you do not have symptoms. Immediate testing and treatment can save your life.
Outbreak linked to procedures with epidural anesthesia in Matamoros, Mexico, 2023
Anyone who had a procedure under epidural anesthesia at River Side Surgical Center or Clinica K-3 in Matamoros, Mexico, from January 1 to May 13, 2023, is at risk for fungal meningitis.
Fungal meningitis is a rare, life-threatening fungal infection that causes swelling of the areas around the brain and spinal cord. People can get infected during medical procedures if all infection control practices are not followed.
Your First Steps
If you are at risk for fungal meningitis, go the nearest emergency room. If you do not have symptoms or your symptoms are mild, you have an opportunity to get tested and treated to prevent severe illness or death. Once symptoms start, fungal meningitis is harder to treat. Do not wait. Every moment counts.

Tips for before you go to the ER
- Bookmark, screenshot, or print CDC’s web page about the fungal meningitis outbreak to show ER staff and healthcare providers.
- Write down the phone number of your local health department so you and ER staff or healthcare providers can call if they have questions.
- Bring an overnight bag, including your cell phone charger, in case you need to stay at the hospital.
- Tell at least one friend or family member so they can bring you additional items or help with personal responsibilities, if needed.
- Plan on staying at the ER until you are seen by a healthcare provider. You may have to wait several hours because staff may need to first take care of other patients who need immediate attention.
If someone is having symptoms of fungal meningitis or experiencing a life-threatening emergency, call 911 or go to the ER without delay.
Getting Tested
When you arrive at the ER, tell staff that you need to be tested for fungal meningitis because you recently had epidural anesthesia at one of the clinics in Mexico involved in the current outbreak.
If any staff or healthcare providers have questions, show them CDC’s web page or connect them with your local health department.
Spinal tap
Healthcare providers will test you for fungal meningitis by performing a spinal tap. You may be nervous about the test, but most people do not feel pain when they have a spinal tap. Some people may feel pressure or a sharp feeling when the needle is inserted. You may be less worried when you know what to expect with each step. Remember that this test could potentially save your life.
What to expect
- The healthcare providers performing your spinal tap will:
- Ask you to either lay on your side with your knees pulled up against your chest or sit up and lean forward against some pillows.
- Clean an area around your lower spine with a liquid or moist wipes that kill germs.
- Use a tiny needle to inject a solution into the skin to make that area temporarily numb.
- Insert a hollow needle into a small space around your spine to collect fluid called cerebrospinal fluid (CSF).
- The fluid will be tested in a laboratory to determine if you have fungal meningitis.
- Test results normally come back quickly but may take longer.
Test results
- If you test negative for fungal meningitis:
- It is possible to test negative during the early phases of infection (called a false negative).
- Your healthcare provider may ask you to come back in 2 weeks to repeat the spinal tap.
- Watch for symptoms for at least 30 days after your spinal tap, whether or not you are scheduled to return for a second test.
- If you develop new or worsening symptoms (like fever, headache, stiff neck, nausea, vomiting, light sensitivity, confusion), you should return to the emergency room as soon as possible.
- If you test positive for fungal meningitis:
- You will be admitted to the hospital to begin treatment.
What to expect during treatment
When you are tested and get treatment early, your fungal meningitis can be cured.
In the hospital
- You will need to spend at least 2 weeks receiving treatment in the hospital. You will receive two antifungal medicines by IV (intravenous): amphotericin B and voriconazole.
- Possible side effects for amphotericin B include fever, chills, nausea, tiredness, and weakness.
- Possible effects for voriconazole include vision changes, black stools, itching, and blistering or peeling skin.
- Your healthcare team will order simple blood tests to see how your kidneys and liver are functioning while on these medicines.
- After 2 weeks, you may be able to switch to taking one oral medicine.
Staying in the hospital can be challenging, and it may be harder if you never developed symptoms.
Remember that the time you spend staying in the hospital and taking antifungal medicines at home is protecting you from severe complications and death. It may help you stay safe and healthy for years to come.
If you stop treatment too early or do not take medicines as prescribed, the infection can come back and cause severe disease and even death.
At home
- Spinal tap and blood tests will be repeated to determine when you can go home to continue oral treatment.
- You may need to continue to take oral medicines for at least 3-6 months.
- Continue to follow up as an outpatient as instructed by your healthcare provider.
About Fungal Meningitis
- Testing for fungal meningitis requires a spinal tap, also called a lumbar puncture.
- If you have fungal meningitis, treatment includes at least 2 weeks in the hospital and at least 3–6 months of medicine at home after you leave the hospital.
- The first few days or weeks that you are infected, you may not feel sick. Without testing and treatment, you could quickly become very ill.
- Early testing and treatment, especially before symptoms start, can prevent serious illness, complications, and death.
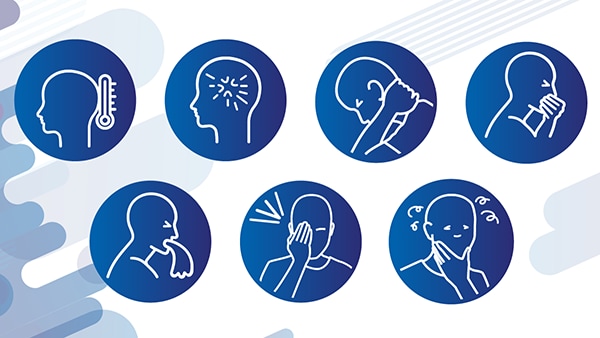
- Common symptoms include fever, headache, stiff neck, nausea, vomiting, light sensitivity, and confusion.
- Serious complications include strokes, bleeds in the brain, fluid in the brain, and too much pressure in the brain.
- Fungal meningitis infections cannot spread person to person.
Additional information about this outbreak is available: Fungal Meningitis Outbreak Associated with Procedures Performed under Epidural Anesthesia in Matamoros, Mexico