Steroid Creams Can Make Ringworm Worse
You should not treat rashes that might be ringworm with creams that contain steroids. Talk to your healthcare provider if you think you might have ringworm or if you have ringworm that is not getting better with antifungal treatment.
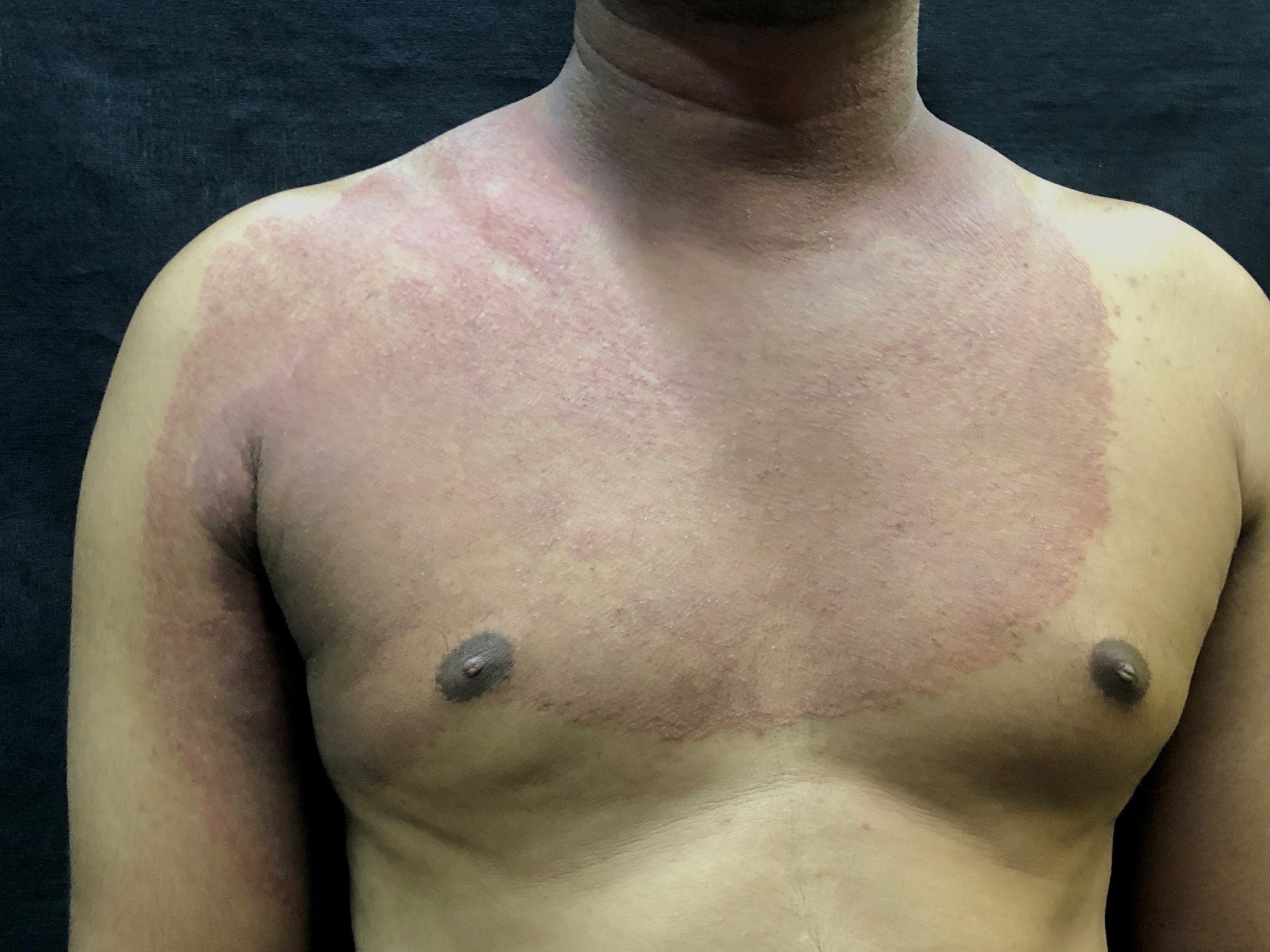
Corticosteroid use can lead to ringworm rashes covering large areas of the body.
View Larger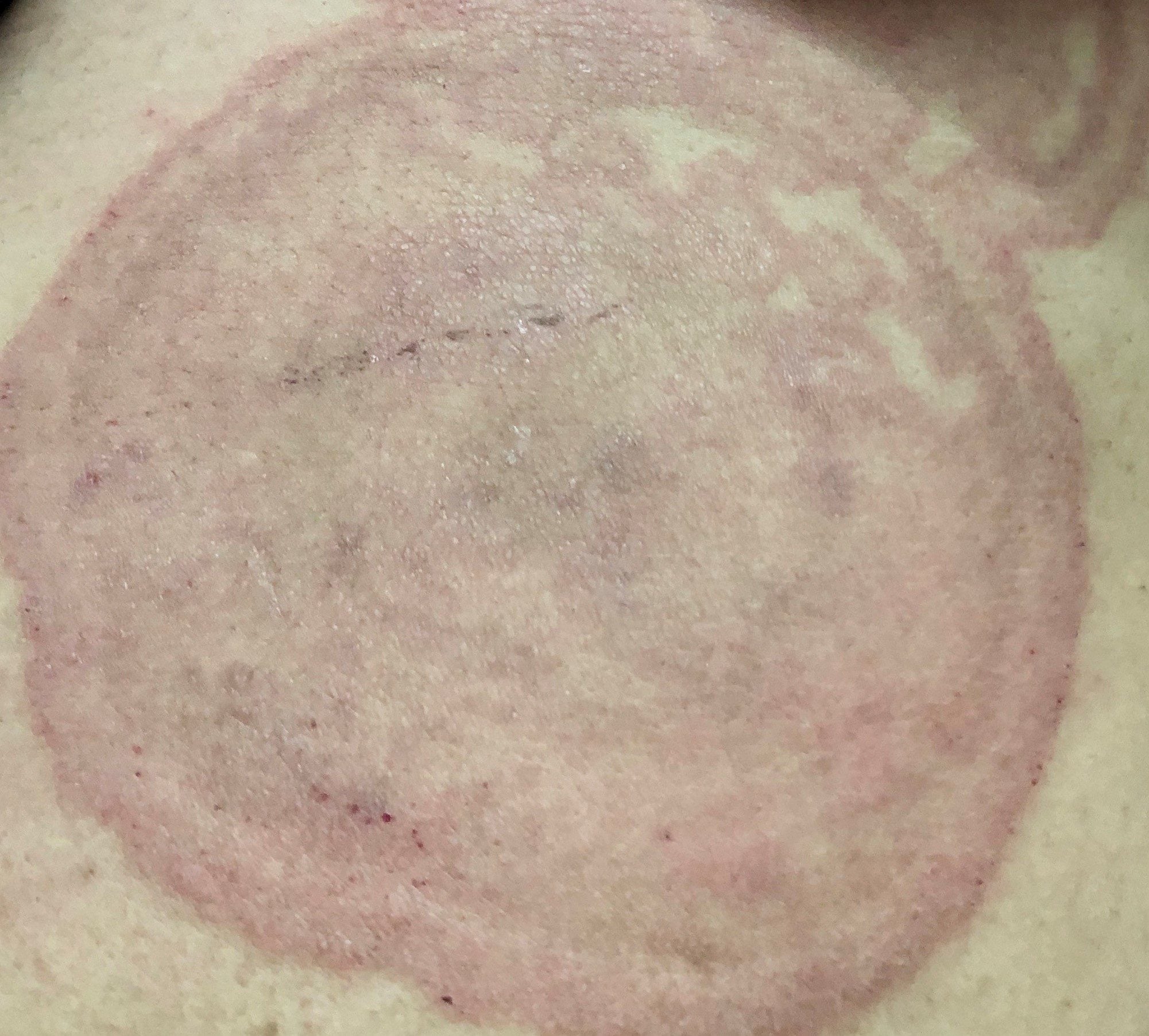
Corticosteroid medications can cause unusual patterns in ringworm rashes, like this “double-edged” pattern that is several inches wide.
View Larger
Long-term use of combination corticosteroid creams can cause severe redness and burning with ringworm.
View LargerPhoto credit: Dr. Shyam Verma, India
Do not use steroid creams to treat rashes that may be ringworm
Ringworm is a very common cause of skin rashes. People might have a skin rash that they do not realize is caused by ringworm. For this reason, people sometimes apply over-the-counter creams or ointments containing medications called corticosteroids (or “steroids” for short) to their rash. Steroid creams can be helpful for some skin problems and can even temporarily reduce ringworm symptoms like itching and redness. However, steroid creams don’t kill the fungus that causes ringworm.
Steroid creams can make ringworm worse because they weaken the skin’s defenses. Steroid creams can allow ringworm infections to spread to cover more of the body. Ringworm that has been treated with steroid creams can have an unusual appearance, making it hard for healthcare providers to diagnose. In rare cases, steroid creams can allow the fungus that causes ringworm to invade deeper into the skin and cause a more serious condition.
An emerging international problem
In the United States, over-the-counter steroid creams are not very powerful, which is why they’re called “low potency.” But in some other countries, people can buy creams containing strong steroids without a prescription. Many of these steroid creams also contain antifungal and antibacterial medicines, and the labels say that the cream can be used to treat fungal infections. However, healthcare providers in India report seeing more cases of severe ringworm in people who have used these combination medications.1-6 These infections have been reported to cover large parts of the body, last for months or longer, and spread to family members.4
If you travel internationally, develop a rash, and think it might be ringworm, be aware that strong over-the-counter steroid creams containing combinations of antifungal and antibacterial medicines can make ringworm worse and can cause other health problems. If a healthcare provider in another country recommends a cream for a rash that might be ringworm, ask what medications are in the cream and whether it contains strong steroids.1
Information for healthcare professionals
Topical corticosteroid use without an antifungal agent is not recommended for ringworm infections (also called “tinea” or “dermatophytosis”). However, patients may have already applied corticosteroids on their own. For example, patients may have applied over-the-counter low-potency topical corticosteroids before seeking medical care. Others may have used higher-potency corticosteroids from:
- A prescription given because ringworm was misdiagnosed as another condition.
- Treatment for an unrelated condition.
- A previous prescription for a different problem.
- Purchase of high-potency steroids abroad.
Use of topical corticosteroids on ringworm can lead to:
- More or larger ringworm lesions.
- Atypical appearance, called tinea incognito, which may involve less erythema (redness), less scale, and indistinct lesion borders. Unusual shapes or patterns can mimic other conditions like atopic dermatitis (eczema).7,8
- Majocchi’s granuloma, in which the dermatophytes invade deeper than the epidermis (into the dermis or subcutaneous tissue).9
These conditions resulting from topical corticosteroid use on ringworm are sometimes referred to as steroid-modified tinea.1 Use of topical corticosteroids for ringworm also has led to thinning of the skin, striae (stretch marks), and pigment changes when applied to sensitive regions or through excessive or high-potency corticosteroid use.10
Combination antifungal and mid-potency corticosteroid creams are available by prescription in the United States. Healthcare providers should be aware that treatment failure has been reported with use of combination therapy for ringworm and the use of certain formulations is not recommended in children.11,12,15
The overuse of steroids to treat ringworm may contribute to antimicrobial-resistant ringworm infections, an emerging public health concern.
- Verma S. Steroid modified tinea. 2017 March 8.
- Verma S, Hay RJ. Topical steroid‐induced tinea pseudoimbricata: a striking form of tinea incognito. Int J Dermatol. 2015 Jan 20.
- Verma S. Emergence of recalcitrant dermatophytosis in India. Lancet Infect Dis. 2018 July 1.
- Bishnoi A, Keshavamurthy V, Dogra S. Emergence of recalcitrant dermatophytosis in India. Lancet Infect Dis. 2018 March 1.
- Kumar S, Goyal A, Gupta YK. Abuse of topical corticosteroids in India: concerns and the way forward. J Pharmacol Pharmacother. 2016 Jan.
- Ely JW, Rosenfeld S, Seabury Stone M. Diagnosis and management of tinea infections. Am Fam Physician. 2014 Nov 15.
- Arenas R, Moreno-Coutiño G, Vera L, Welsh O. Tinea incognito. Clinics in Dermatology. 2010 March.
- Wacker J, Durani BK, Hartschuh W. Bizarre annular lesion emerging as tinea incognito. 2004 Oct 22.
- İlkit M, Durdu M, Karakaş M. Majocchi’s granuloma: a symptom complex caused by fungal pathogens. Medical Mycology. 2012 July 01.
- Hengge UR, Ruzicka T, Schwartz RA, Cork MJ. Adverse effects of topical glucocorticosteroids. Journal of the American Academy of Dermatology. 2006 Jan.
- Alston SJ, Cohen BA, Braun M. Persistent and recurrent tinea corporis in children treated with combination antifungal/ corticosteroid agents. 2003 Jan.
- Wheat CM, Bickley RJ, Hsueh Y, Cohen BA. Current trends in the use of two combination antifungal/corticosteroid creams. The Journal of Pediatrics. 2017 Jul.
- Nenoff P, Verma SB, Vasani R, Burmester A, Hipler UC, Wittig F, Krüger C, et al. The current Indian epidemic of superficial dermatophytosis due to Trichophyton mentagrophytes-A molecular study. 2018 Dec 18.
- Singh A, Masih A, Monroy-Nieto J, Singh PK, Bowers J, Travis J, et al. A unique multidrug-resistant clonal Trichophytonpopulation distinct from Trichophyton mentagrophytes/Trichophyton interdigitale complex causing an ongoing alarming dermatophytosis outbreak in India: Genomic insights and resistance profile. Fungal Genet Biol. 2019 Dec
- American Academy of Pediatrics. Avoid the use of combination topical steroid antifungals for tinea corporis, Candida skin infections, and diaper dermatitis. 2021 Jan 27