Mycetoma
Mycetoma is a disease caused by certain types of bacteria and fungi found in soil and water. These bacteria and fungi may enter the body through a break in the skin, often on a person’s foot. The resulting infection causes firm, usually painless but debilitating masses under the skin that can eventually affect the underlying bone. Mycetoma can be caused by bacteria (actinomycetoma) or fungi (eumycetoma). The number of people with mycetoma worldwide is not known, but there were 17,607 cases reported in a 2017 review of scientific articles between 1950 and 2017. The actual number of cases is likely substantially higher.
Mycetoma affects people of all ages and is more common in men. This disease primarily affects poorer people in rural regions of Africa, Latin America, and Asia that are located near the equator and have dry climates. People affected by mycetoma often live in remote areas where they have limited access to healthcare and medications. Mycetoma can cause severe physical disabilities that can force people to stop working and cause stigma.
Mycetoma has rarely been reported in the United States in recent decades. A review of the literature from 1890 to 2020 showed fewer than 80 cases occurring in the United States. People who travel from the United States to areas where mycetoma has been reported are unlikely to get mycetoma. Developing mycetoma requires repeatedly exposing broken skin to soil and water that contain the microbes that cause mycetoma over long periods of time. Travelers are unlikely to have enough exposure to be at risk.
Diagnosis requires laboratory evaluation of a biopsy, or small tissue sample, of the infected area. The treatment for mycetoma includes antibiotics or antifungal medicine, depending on whether the disease is caused by bacteria or fungi. Surgery is sometimes needed to cut away the infected tissue. Wearing shoes might help prevent mycetoma.
Symptoms

Man with a swollen foot caused by mycetoma.
Symptoms are similar for bacterial and fungal mycetoma. Both appear as firm, painless masses under the skin. These masses usually appear on a person’s foot but can form anywhere on the body. The mycetoma masses start small, but over time they can grow larger, develop oozing sores, and cause the affected limb to become deformed or unusable. If mycetoma is not treated or if treatment fails, it can spread to other areas of the body. Long-term mycetoma can eventually destroy the underlying muscle and bone.
Risk & Prevention
Mycetoma is a health problem in equatorial regions of Africa, Latin America, and Asia known as the “mycetoma belt.” Fungal mycetoma (eumycetoma) is the most common type in Africa, while bacterial mycetoma (actinomycetoma) causes most cases in South and Central America and some Asian countries.
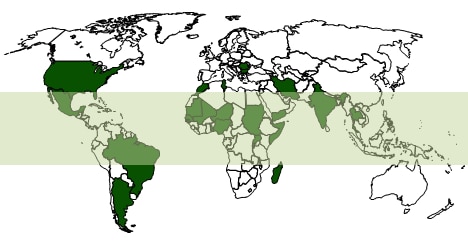
Countries shown in dark green indicate those in which cases of mycetoma have been reported in the medical literature. The mycetoma belt region is shaded in light green.
Mycetoma affects people of all ages and is more common in men. Many people with mycetoma work in agricultural jobs, such as farmers and livestock herders.
Health care providers and researchers believe that wearing shoes might prevent injuries that can lead to mycetoma. Shoes protect the feet while someone is walking or working outside in areas where the germs that cause mycetoma are common in water and soil. Early detection and treatment, before symptoms cause serious effects, can reduce disabilities from mycetoma and may cure the condition.
Transmission
The bacteria and fungi that cause mycetoma live in soil and water. These germs can enter the body through wounds or other small skin injuries, like a thorn prick. It is not known why some people develop mycetoma and others do not, but aspects of the environment and living conditions are likely involved. Mycetoma does not spread between people.
Diagnosis
A doctor can diagnose mycetoma by taking a small sample (biopsy) of the infected area of the body and sending it to a laboratory. The laboratory may examine the sample under a microscope, but this test may not always determine if the infection is caused by bacteria or fungi and cannot determine what type of bacteria or fungi is the cause of the mycetoma. A culture (growing the bacteria or fungi in the laboratory) can determine the specific type of bacteria or fungus causing the infection. A doctor may also do an imaging test such as an X-ray or ultrasound to diagnose mycetoma and see how much damage has taken place to muscle and bone. Patients can avoid long-term infection and amputation by seeking care and detecting and treating mycetoma early.
Treatment
Therapies that work against mycetoma are limited, may have to be taken for a long time, and can be expensive. The treatment for mycetoma depends on whether it is caused by bacteria (actinomycetoma) or fungi (eumycetoma).
- Actinomycetoma is usually treatable with antibiotics, and surgery is usually not needed.
- Eumycetoma is usually treated with long-term antifungal medicine, but treatment may not be completely effective. In this case, surgery or amputation are sometimes needed to cut away the infected tissue.
- Beer KD, Blaney DD, Kadzik M, Asiedu KB, Shieh W, Bower W, et al. A call to action for mycetomaexternal icon. Curr Fungal Infect Rep. 2018 Jul
- World Health Organization: Mycetomaexternal icon
- van de Sande WW. Global burden of human mycetoma: a systematic review and meta-analysisexternal icon. PLoS neglected tropical diseases. 2013 Nov;7(11):e2550.
- van de Sande WW, Fahal A, Ahmed SA, Serrano JA, Bonifaz A, Zijlstra E. Closing the mycetoma knowledge gapexternal icon. Med Mycol. 2017
- Zijlstra EE, van de Sande WW, Welsh O, Mahgoub el S, Goodfellow M, Fahal AH. Mycetoma: a unique neglected tropical diseaseexternal icon. Lancet Infect Dis. 2016 Jan;16(1):100-12.
- Hay R, Denning DW, Bonifaz A, Queiroz-Telles F, Beer K, Bustamante B, et al. The diagnosis of fungal Neglected Tropical Diseases (Fungal NTDs) and the role of investigation and laboratory tests: an expert consensus reportexternal icon. Trop Med Infect Dis. 2019 Dec