Where Blastomycosis Comes From
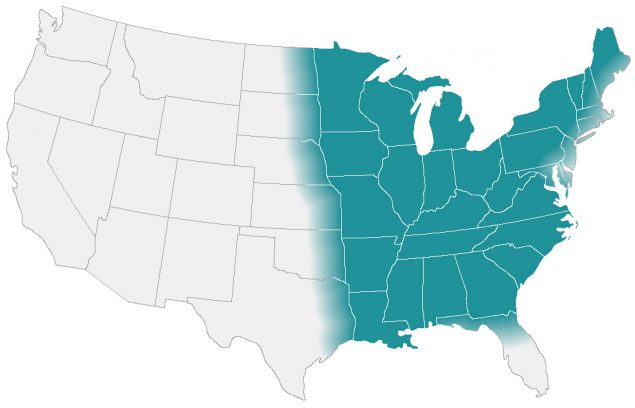
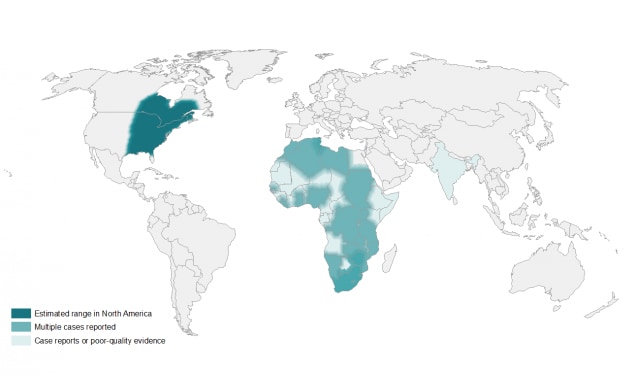
Blastomyces lives in the environment, particularly in moist soil and in decomposing plant matter such as wood and leaves. In the United States, the fungus mainly lives in the midwestern, south-central, and southeastern states, particularly in areas surrounding the Ohio and Mississippi River valleys, the Great Lakes, the Saint Lawrence River, and the western United States.1,2 The fungus also lives in Canada,3–4 and a small number of blastomycosis cases have been reported from Africa5 and India.6
These maps show CDC’s current estimate of where the fungi that cause blastomycosis live in the environment. These fungi are not distributed evenly in the shaded areas, might not be present everywhere in the shaded areas, and can also be outside the shaded areas.
Life cycle of Blastomyces
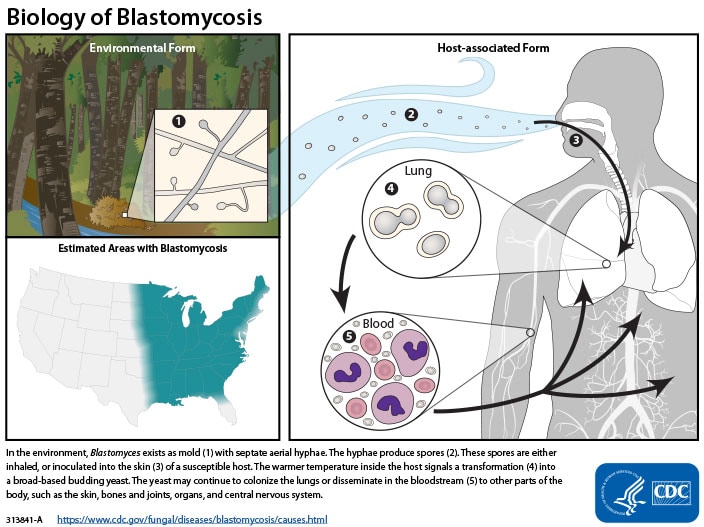
Blastomyces lives in the environment as a mold that produces fungal spores. The spores are too small to see without a microscope. When soil or plant material is disturbed, the tiny spores can be released into the air. When people or animals breathe in the spores, they are at risk for developing blastomycosis. After the spores enter the lungs, the body temperature allows the spores to transform into yeast. The yeast can stay in the lungs or spread through the bloodstream to other parts of the body, such as the skin, bones and joints, organs, and central nervous system (brain and spinal cord).
Click here for the PDF version of image [PDF – 1 page] for printing.
Environmental testing
Testing the environment for Blastomyces isn’t likely to be useful in most situations. When an environmental sample tests positive for Blastomyces, it isn’t necessarily a source of infection, and when a sample tests negative, that doesn’t necessarily mean that the fungus isn’t there. There are no publicly available tests to detect Blastomyces in the environment. Testing environmental samples for Blastomyces is currently only done for scientific research.
- Furcolow ML, Busey JF, Menges RW, Chick EW. Prevalence and incidence studies of human and canine blastomycosis. II. Yearly incidence studies in three selected states, 1960–1967. Am J Epidemiol. 1970;92(2):121–31.
- Bradsher RW, Chapman SW, Pappas PG. Blastomycosis. Infect Dis Clin North Am. 2003;17(1) 21-40, vii.
- Morris SK, Brophy J, Richardson SE, Summerbell R, Parkin PC, Jamieson F, et al. Blastomycosis in Ontario, 1994-2003. Emerg Infect Dis. 2006 Feb;12(2):274-9.
- Litvinov IV, St-Germain G, Pelletier R, Paradis M, Sheppard DC. Endemic human blastomycosis in Quebec, Canada, 1988-2011. Epidemiol Infect. 2013 Jun;141(6):1143-7.
- Cheikh Rouhou S, Racil H, Ismail O, Trabelsi S, Zarrouk M, Chaouch N, et al. Pulmonary blastomycosis: a case from Africa. ScientificWorldJournal. 2008 Nov 2;8:1098-103.
- Chakrabarti A, Slavin MA. Endemic fungal infections in the Asia-Pacific region. Med Mycol. 2011 May;49(4):337-44.