Valley Fever (Coccidiomycosis) Awareness
What You Need to Know
- Valley fever is a respiratory infection similar to pneumonia.
- It’s caused by a fungus found in soil in certain places, including the southwestern United States and south-central Washington state.
- The most common symptoms are cough and fever that often go away on their own in weeks or months.
- Valley fever is often misdiagnosed. This can delay treatment for some patients that need it.

Valley fever is a fungal lung infection that can be devastating. Learning about Valley fever can help you and your doctor recognize the symptoms early.
Valley fever, also called coccidioidomycosis, is caused by a fungus that lives in the soil. About 20,000 cases are reported in the United States each year, mostly from Arizona and California. The number of cases is increasing.
Valley fever can be misdiagnosed because its symptoms are similar to those of other respiratory illnesses, including pneumonia.
From Soil to Lungs
Coccidioides, the fungus that causes Valley Fever, is found in soil in the Pacific Northwest and southwestern United States (see map), and parts of Mexico, Central America, and South America. The fungus might also live in similar areas with hot, dry climates, and the geographic range may be expanding because of climate change. Public health officials and researchers continue to investigate to see if it is found in other areas.
People can get Valley fever by breathing in the spores from this fungus. Pets can also become infected. Valley fever does not spread from person to person or between people and animals.
Common Symptoms May Lead to Delayed Diagnosis
Some people who are exposed to the fungus never have symptoms. Other people may have symptoms that include:
- Fatigue (tiredness)
- Cough
- Fever
- Shortness of breath
- Headache
- Night sweats
- Muscle aches or joint pain
- Rash on upper body or legs
Many people get better on their own within weeks or months without any treatment. However, some people need treatment to reduce symptoms or stop them from getting worse.
Valley fever is often misdiagnosed as an infection caused by a bacteria or virus. This causes delays in the necessary antifungal treatment and sometimes contributes to the unnecessary use of other medicines. Delayed treatment can be life-threatening and costly for some people.
People who develop severe infections or whose infections spread to other parts of their body often require hospitalization and may need to take antifungal treatment for a long time.
People at Risk
Valley fever is a serious, costly illness
- Nearly 75% of people with Valley fever miss work or school
- As many as 40% of people who get Valley fever are hospitalized
- The average cost of a hospital stay for a person with Valley fever is almost $50,000
- About 60–80% of patients with Valley fever are given one or more rounds of antibiotics before receiving a correct diagnosis and appropriate treatment
Anyone can get Valley fever if they live in, work in, or travel to an area where the fungus lives in the environment. Valley fever can affect people of any age, but it’s most common in adults aged 60 and older. Also, the following groups of people may be at higher risk for developing the severe forms of Valley fever:
- People with weakened immune systems, which may include people who:
- Have HIV
- Have had an organ transplant
- Are taking medicines such as corticosteroids or tumor necrosis factor (TNF) inhibitors
- People who are pregnant
- People who have diabetes
Data suggest that risk of Valley fever infection may be greater for people of American Indian or Alaska Native descent, and risk of severe disease may be greater among people who are Black or Filipino. Researchers are working to understand why the risks may be greater for these groups.
Awareness Is Key
In areas where the fungus that causes Valley fever is in the environment, it’s difficult to completely avoid exposure. There is no vaccine to prevent infection. That’s why knowing about Valley fever is one of the most important ways to avoid delays in diagnosis and treatment.
People who have symptoms of Valley fever and live in, work in, or have visited an area where the fungus is in the environment should ask their doctor to test them for Valley fever. Healthcare providers should be aware that Valley fever symptoms are similar to those of other respiratory illnesses and should consider testing for Valley fever in patients with pneumonia symptoms who live in or have traveled to an area where the fungus that causes Valley Fever lives.
What CDC Is Doing
- Raising awareness. CDC, state and local health departments, and other agencies are working together to create resources and educate the public and healthcare providers about Valley fever to reduce delays in diagnosis and treatment and to improve people’s health.
- Surveillance. In many states, healthcare providers and laboratories are required to report Valley fever cases to public health authorities. Disease reporting allows government officials to monitor trends in Valley fever cases and expansion from climate change, and to examine the economic costs of the disease.
- Advanced molecular detection. CDC has been developing new tools that make it faster and easier to detect Coccidioides, the fungus that causes Valley fever, in the environment. CDC is also using whole genome sequencing on environmental and patient samples to investigate new areas where this fungus is living and causing illness.
- Research on testing and treatment. CDC is studying new laboratory tests to diagnose Valley fever faster and is assisting other health agencies with studies to understand the best treatment for Valley fever.
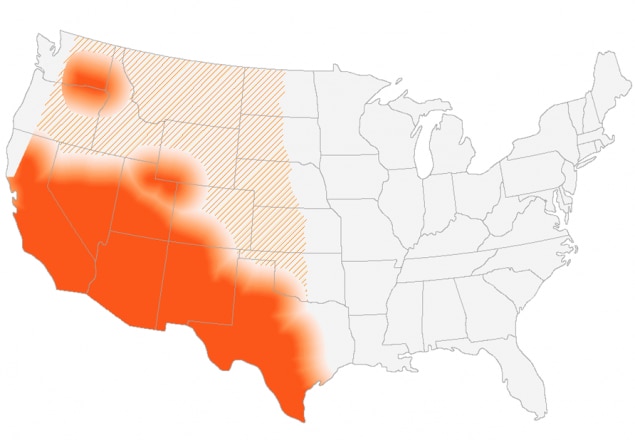
This map shows CDC’s current estimate of where the fungus that causes Valley fever lives in the environment in the United States. The fungus is not distributed evenly in the shaded areas, might not be present everywhere in the shaded areas, and can also be outside the shaded areas. Darker shading shows areas where the fungus is more likely to live. Diagonal lines show the potential range of the fungus.
Join CDC in sharing information to increase awareness in your community about fungal diseases during Fungal Disease Awareness Week, September 18–22, 2023. New resources for 2023 will be available soon.
