Mozambique Country Profile

Mozambique Country Profile
Discover more about CDC’s work in Mozambique by viewing our detailed country profile
Country Overview
CDC has been working with the Government of Mozambique since 2000 and continues to support the country’s response to the HIV epidemic. CDC works closely with Mozambique’s Ministry of Health to deliver high quality HIV prevention and treatment services; strengthen laboratory, HIV surveillance, infrastructure, and workforce capacity; and enhance the country’s response to tuberculosis, the leading cause of death for people living with HIV.
Per Capita GNI
$500
(2022)
Population (million)
32.96
(2022)
Under 5 Mortality
69.6/1,000 Live Births
(2021)
Life Expectancy
59.3 Years
(2021)
Estimated HIV Prevalence
11.6%
(Ages 15-49): (2022)
Estimated AIDS Deaths
40,000
(Age≥15) (2022)
TB Treatment Success Rate
94%
(2020)
Estimated TB Incidence
361/100,000
(2021)
Estimated Orphans Due to AIDS
1,300,000
(2022)
TB patients with known HIV-status who are HIV-positive
25%
(2021)
Reported Number Receiving Antiretroviral Therapy (ART)
1,853,566
(Age≥15) (2022)
Strategic Focus
The Centers for Disease Control and Prevention (CDC) has been providing support to Mozambique’s public health sector since 2000, in order to help develop the country’s response to the dual HIV and Tuberculosis (TB) epidemic. CDC supports implementation of key HIV and TB interventions and provides technical assistance (TA) to the Ministry of Health (MOH) in scaling up evidence-based interventions. CDC works closely with the MOH and implementing partners in addressing the country´s immediate needs, and supports building of long-term capacity to mitigate the impact and HIV epidemic control.
Strengthening Health System Capacity: CDC works closely with the MOH to deliver high quality HIV prevention and treatment services; strengthen laboratory, surveillance, infrastructure, and workforce capacity; and develops operational research in all 11 provinces, with intensified efforts in those where HIV prevalence rates are highest. CDC is supporting the MOH to improve the availability, accessibility, quality, and use of service-delivery data; conducting HIV surveillance and behavioral surveys; designing and improving systems to support routine program monitoring; and strengthening and expanding the health management information systems (HMIS) infrastructure.
Supporting Integrated HIV Prevention and Treatment Services: CDC supports the delivery of antiretroviral therapy (ART) as part of the national program that reaches 914,000 patients , and is helping to rapidly scale-up viral load (VL) and drug resistance assessments to leverage the country’s capacity to reach the United Nations Programme on HIV/AIDS (UNAIDS) 90-90-90 goals in 2020. CDC also supports the provision of HIV counselling and testing, prevention of mother-to-child HIV transmission services in more than 800 health facilities, and voluntary medical male circumcisions (VMMC) at over 50 fixed and mobile sites to further increase the control of the HIV epidemic.
Responding to HIV & Tuberculosis (TB) Epidemics: CDC supports the MOH in its response to the national TB burden, the leading cause of death for those living with HIV. CDC provides technical assistance in the development of national policies and strategies, training materials, and mentoring and supervision activities. As a result, our work is dramatically improving the laboratorial and clinical capacity for TB/HIV diagnostics and treatment. CDC implementing partners are also working with key populations, such as miners, prisoners, and healthcare workers and working with families of TB patients to improve detection of TB and HIV.
Key Activities and Accomplishments
Increasing Access to Antiretroviral Treatment: Through the development of national policies, including the National Accelerated Response to HIV, access to treatment has been dramatically increasing. In FY2017, CDC with other USG agencies continued to support the expansion of the “Test and Start” policy.
Prevention of Mother-to-Child Transmission of HIV: Identifying and treating HIV-positive pregnant women is the most effective approach to eliminate new infections among infants. CDC’s support for ensuring pregnant women receive HIV treatment makes it possible for thousands of babies to be born HIV-free. CDC supports MOH to make HIV testing and treatment available to all HIV exposed infants.
Voluntary Medical Male Circumcision: With lifelong benefits, this low-cost procedure reduces the risk of female-to-male sexual transmission of HIV by approximately 60%. The service also adds value by connecting men to health care and offering a package of services, including education on safer sex, and HIV testing and counselling services, with links to HIV treatment services for those that are HIV-positive.
Viral Load Monitoring Expansion: Access to high quality VL monitoring is considered essential for controlling the HIV epidemic, and is a top priority for CDC in Mozambique. Since 2016, according to the Mozambique MOH, CDC´s contribution resulted in the expansion of viral monitoring to 12 referral laboratories, leveraging the national capacity to perform approximately 74,000 VL tests per month. VL monitoring has increased substantially, from under 2,000 tests performed per month in September 2015 to over 50,000 tests performed in December 2017.
Detection and Access of Miners and Prisoners to HIV and TB Treatment: Mine workers and prisoners have some of the highest rates of TB, HIV and TB/HIV in Africa. CDC implementing partners are identifying and referring for treatment miners with HIV and TB. Through mid-2018, almost 600 miners were screened with over 30% being found to have HIV and TB. CDC is supporting screening prisoners, identifying 360 persons with TB disease each in 2016 and 2017, up 3-fold compared with 2015.

Tracking PEPFAR Impact Toward Global Targets
The U.S. Centers for Disease Control and Prevention (CDC) works with partners including host countries, local implementing partners, faith-based organizations, and other community-based organizations to measure progress towards HIV epidemic control in countries supported by the U.S. President’s Emergency Plan for AIDS Relief (PEPFAR).
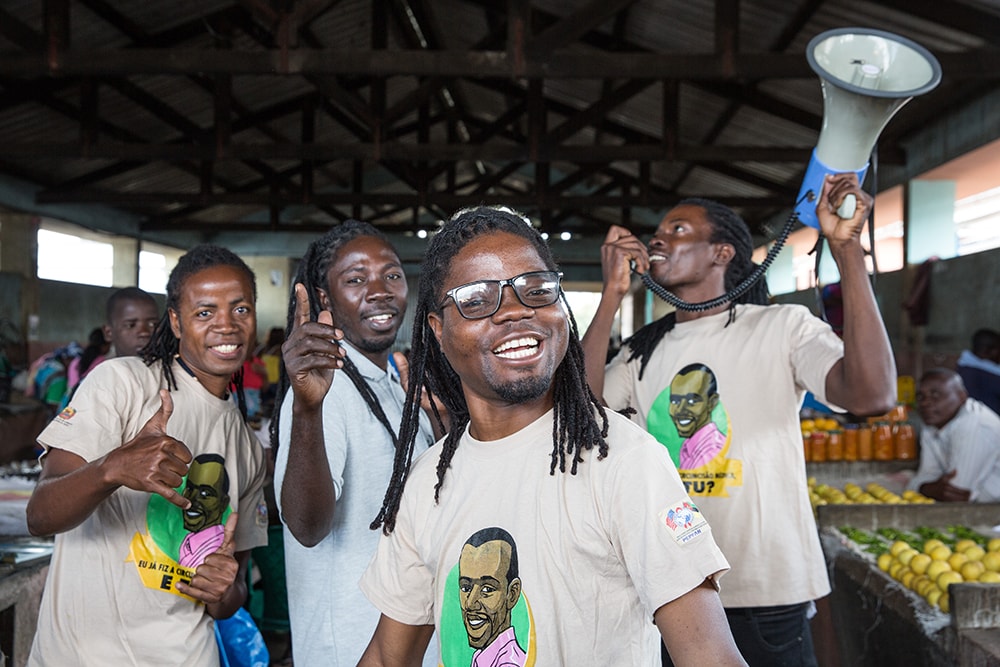
Voluntary Medical Male Circumcision Reduces New HIV Infections in Mozambique
HIV transmission can be prevented through highly effective interventions proven to work independently or in combination. The U.S. Centers for Disease Control and Prevention (CDC) supports HIV treatment and prevention strategies including Voluntary Medical Male Circumcision (VMMC), a medical procedure that reduces the risk of heterosexual HIV transmission by up to 60 percent.

CDC On the Frontlines
Over the past 20 years, the U.S. President’s Emergency Plan for AIDS Relief (PEPFAR) has saved millions of lives as a leader in the global response to two of the world’s deadliest infectious diseases – HIV and TB. As a key implementing agency of the U.S. President’s Emergency Plan for AIDS Relief (PEPFAR), CDC is at the forefront of these global efforts to treat and prevent these diseases.