TB and Hispanic or Latino Persons
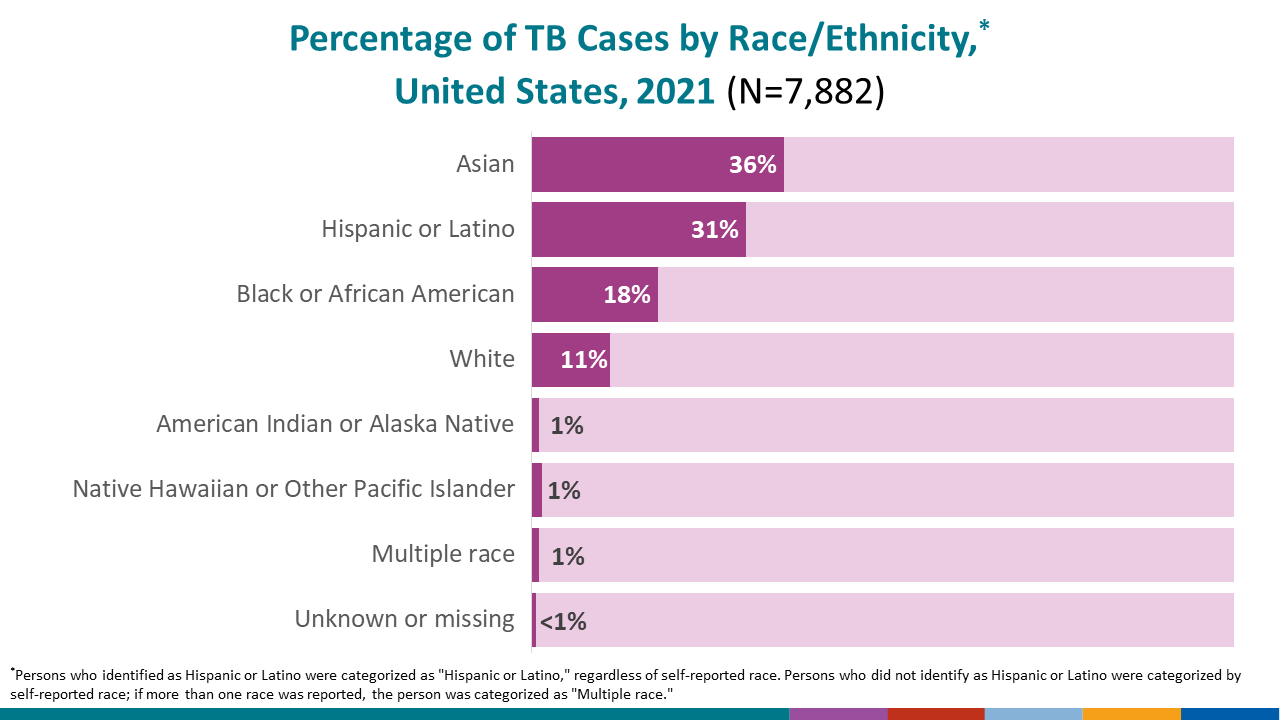
In 2021, a total of 7,882 TB cases were reported in the United States; however, Hispanic or Latino persons* continue to be affected by TB at a greater rate compared to White persons.
Several important factors contribute to the higher rates of TB among racial and ethnic minority groups, including Hispanic or Latino persons. These factors include being born in a country with a high rate of TB disease or travel to a country with a high rate of TB disease.
By the Numbers
In 2021, U.S. state, local, and territorial health agencies reported a total of 7,882 TB cases to CDC.
- TB disease was reported in 2,410 Hispanic or Latino persons in the United States, accounting for 30.6% of all people reported with TB nationally.
- The rate of TB disease among Hispanic or Latino persons is 3.8 cases per 100,000 persons.
- The TB case rate is 9 times higher for Hispanic or Latino persons than for non-Hispanic White persons.
- Read more in Reported Tuberculosis in the United States, 2021.
Prevention Challenges
TB is a challenging disease to diagnose, treat, and control. Dwindling resources and loss of public health capacity, including access to care, and maintaining clinical and public health expertise, add to the challenge. It is critical to reach those populations at highest risk for TB, and to identify and implement innovative strategies to improve diagnosis and treatment.
Ending TB will require a dual approach of maintaining and strengthening current TB control priorities, while increasing efforts to identify and treat latent TB infection in populations at risk for TB disease.

Similar to other racial and ethnic minority groups, Hispanic or Latino persons face a number of challenges that contribute to higher rates of TB. Challenges may include:
- Testing and Diagnosis
- Many people born outside of the United States have been given a vaccine for TB called BCG. Vaccination with BCG may cause a false positive reaction to a TB skin test. A positive reaction to a TB skin test might be due to the BCG vaccine itself or due to infection with TB bacteria. TB blood tests are the preferred method of TB testing for people who have received the BCG vaccine. TB blood tests are not affected by prior BCG vaccination and do not give a false-positive result in people who have received the BCG vaccine.

- Many people born outside of the United States have been given a vaccine for TB called BCG. Vaccination with BCG may cause a false positive reaction to a TB skin test. A positive reaction to a TB skin test might be due to the BCG vaccine itself or due to infection with TB bacteria. TB blood tests are the preferred method of TB testing for people who have received the BCG vaccine. TB blood tests are not affected by prior BCG vaccination and do not give a false-positive result in people who have received the BCG vaccine.
- Treatment Duration and Completion
- Treatment for TB disease can be lengthy. Patients are often unable or reluctant to take medication for several months. For people with TB disease, inadequate treatment can lead to treatment failure, relapse, ongoing transmission, and development of drug resistance.
- For people with latent TB infection, treatment for a condition with no symptoms of illness may not be a priority.
- Socioeconomic Factors
- People experiencing poverty, including those with limited access to quality health care, employment opportunities, housing, and transportation, and those who disproportionately experience adverse health outcomes. These factors can directly or indirectly increase the risk for TB disease and present barriers to treatment.
- Language and cultural barriers, including health knowledge, stigma associated with the disease, values, and beliefs may also place certain populations at higher risk. Stigma may deter people from seeking medical care or follow up care.
- HIV and Other Medical Conditions
-
- TB remains a serious threat, especially for people with human immunodeficiency virus (HIV). People with HIV are more likely than people who do not have HIV to get sick with other infections and diseases, including TB.
- Without treatment, as with other opportunistic infections, HIV and TB can shorten the life of the person infected.
- In addition to HIV, other underlying medical conditions may increase the risk that latent TB infection will progress to TB disease. For example, the risk is higher in people with diabetes, substance abuse (including injection of illegal drugs), silicosis, or those undergoing medical treatments with corticosteroids.
- TB remains a serious threat, especially for people with human immunodeficiency virus (HIV). People with HIV are more likely than people who do not have HIV to get sick with other infections and diseases, including TB.
* Note: Persons who identified as Hispanic or Latino were categorized as “Hispanic or Latino,” regardless of self-reported race. Persons who did not identify as Hispanic or Latino were categorized by self-reported race; if more than one race was reported, the person was categorized as “Multiple race.”
- TB Personal Survivor Stories (Spanish)
- Patient Education Materials Series (English, Spanish, Tagalog, Vietnamese)
- Questions and Answers About Tuberculosis (available in multiple languages)
- 12-Dose Regimen for Latent TB Infection-Patient Education Brochure & Medication Tracker (English, Chinese, Haitian Creole, Marshallese, Spanish, Tagalog, Vietnamese)
- Take on TB Infographic (English, Spanish)
- Video: 5 Things to Know about TB (English, Spanish)