TB and Children
TB in Children in the United States
TB disease in children under 15 years of age (also called pediatric tuberculosis) is a public health problem of special significance because it is a marker for recent transmission of TB. Also, of special significance, infants and young children are more likely than older children and adults to develop life-threatening forms of TB disease (e.g., disseminated TB, TB meningitis). Among children, the greatest numbers of TB cases are seen in children younger than 5 years of age, and in adolescents older than 10 years of age.
In 2021, U.S. state, local, and territorial health agencies reported a total of 7,882 TB cases to CDC.
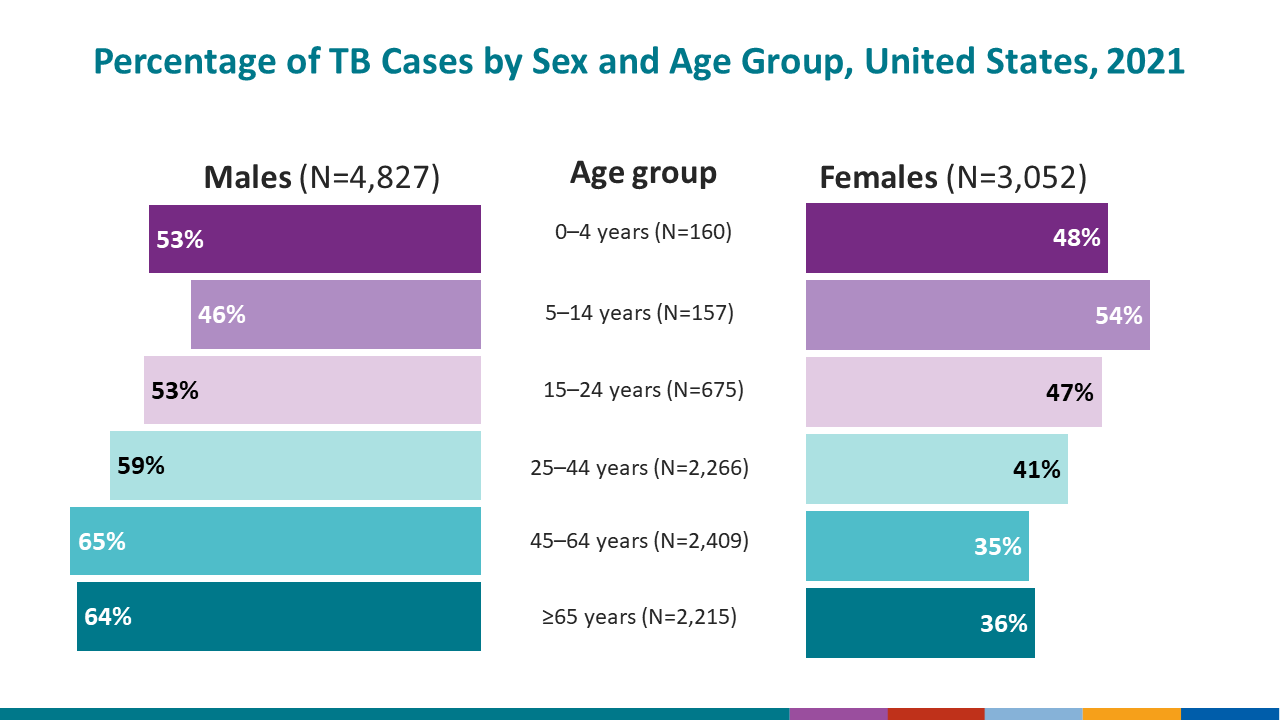
- In 2021, there were 317 cases of TB disease among children ages 14 years or younger in the United States.
- Overall, in 2021, 4% of U.S. TB cases occurred among children less than 15 years of age.
- Read more in Reported Tuberculosis in the United States, 2021.
Basic TB Facts
TB is caused by a bacterium called Mycobacterium tuberculosis. TB bacteria are spread from person to person through the air. The TB bacteria are put into the air when a person with TB disease of the lungs or throat coughs, speaks, or sings. People nearby may breathe in these bacteria and become infected.
People with TB disease of the lungs or throat can spread bacteria to others with whom they spend time every day. However, children are less likely to spread TB bacteria to others. This is because the forms of TB disease most commonly seen in children are usually less infectious than the forms seen in adults.
Not everyone infected with TB bacteria becomes sick. As a result, two TB-related conditions exist: latent TB infection and TB disease.
More: Basic TB Facts

Latent TB Infection
Persons with latent TB infection:
- Usually have a skin test or blood test indicating TB infection;
- Have TB bacteria in their bodies, but the bacteria are not active;
- Are not sick and do not have symptoms;
- Cannot spread bacteria to others; and
- Are often given medicine to prevent them from developing TB disease.
TB Disease
If TB bacteria become active in the body and multiply, the person will get sick with TB disease.
Persons with TB disease:
- Usually have a skin test or blood test indicating TB infection;
- Are sick from TB bacteria that are active (meaning that they are multiplying and destroying tissue in their body);
- Usually have symptoms of TB disease; and
- Must be given medicine to treat TB disease.
Once infected with TB bacteria, children are more likely to get sick with TB disease and to get sick more quickly than adults. In comparison to children, TB disease in adults is usually due to past TB infection that becomes active years later, when a person’s immune system is weakened for some reason (e.g., HIV infection, diabetes).
Confirming the diagnosis of TB disease in children with a laboratory test can be challenging. This is because:
- It is difficult to collect sputum specimens from infants and young children; and
- The laboratory tests used to find TB in sputum are less likely to have a positive result in children; this is due to the fact that children are more likely to have TB disease caused by a smaller number of bacteria (paucibacillary disease).
For these reasons, the diagnosis of TB disease in children is often made without laboratory confirmation and instead based on combination of the following factors:
- Clinical signs and symptoms typically associated with TB disease,
- Positive tuberculin skin test (TST) or positive TB blood test (IGRA) result,
- Chest x-ray that has patterns typically associated with TB disease, and
- History of contact with a person with infectious TB disease.
Testing for TB in Children
In the absence of symptoms, usually the only sign of TB infection is a positive reaction to the TB skin test or TB blood test. TB skin testing is considered safe in children and is preferred over TB blood tests for children less than 5 years of age.
More: Testing for TB
All children with a positive test for TB infection, symptoms of TB, or a history of contact with a person with infectious TB disease should undergo a medical evaluation. Medical evaluations for TB disease include a chest x-ray and physical examination to exclude TB disease and must be done before beginning treatment for latent TB infection.
For more information on where to get a TB test, contact your State TB Control Program.
Signs and Symptoms of TB Disease in Children
Signs and symptoms of TB disease in children include:
- Cough;
- Feelings of sickness or weakness, lethargy, or reduced playfulness;
- Weight loss or failure to thrive;
- Fever; or
- Night sweats.
The most common form of TB disease occurs in the lungs, but TB disease can affect other parts of the body as well. Symptoms of TB disease in other parts of the body depend on the area affected. Infants, young children, and immunocompromised children (e.g., children with HIV) are at the highest risk of developing the most severe forms of TB such as TB meningitis or disseminated TB disease.
Treatment
A pediatric TB expert should be involved in the treatment of TB in children and in the management of infants, young children, and immunocompromised children who have been exposed to someone with infectious TB disease. It is very important that children or anyone being treated for latent TB infection or TB disease finish the medicine and take the drugs exactly as instructed.

Latent TB Infection Treatment
Treatment is recommended for children with latent TB infection to prevent them from developing TB disease. Infants, young children, and immunocompromised children with latent TB infection or children in close contact with someone with infectious TB disease, require special consideration because they are at increased risk for getting TB disease. Consultation with a pediatric TB expert is recommended before treatment begins.
Children over 2 years of age can be treated for latent TB infection with once-weekly isoniazid-rifapentine for 12 weeks. Alternative treatments for latent TB infection in children include 4 months of daily rifampin or 9 months of daily isoniazid. The regimens are equally acceptable; however, health care providers should prescribe the more convenient shorter regimens, when possible. Patients are more likely to complete shorter treatment regimens.
TB Disease Treatment
TB disease in children is treated by taking several anti-TB medicines for 4, 6, or 9 months, depending on the treatment regimen. CDC does not recommend the 4-month rifapentine-moxifloxacin TB treatment regimen for children who are younger than 12 years old or have a body weight below 40 kilograms.
If a child stops taking the drugs before completion, the child can become sick again. If drugs are not taken correctly, the bacteria that are still alive may become resistant to those drugs. TB that is resistant to drugs is harder and more expensive to treat, and treatment lasts much longer (up to 18 to 24 months).
More: Treatment
Vaccines
BCG, or bacille Calmette-Guérin, is a vaccine to prevent TB disease. BCG is used in many countries to prevent childhood TB disease. However, the BCG vaccine is not generally used in the United States, because of the low risk of infection with TB bacteria and the variable effectiveness of the vaccine. The BCG vaccine should only be considered for very select persons who meet specific criteria and in consultation with a TB doctor.
More: TB Vaccine (BCG)
- Testing for TB Infection
- The Difference Between Latent TB Infection and Active TB Disease (Fact Sheet)
- State TB Control Programs
- Diagnosis of Tuberculosis Disease (Fact Sheet)
- TB Vaccine (BCG)
- Treatment for Latent TB Infection and TB Disease
For Parents and their Families
- Questions and Answers about TB (Booklet)
- What Parents Need to Know About Tuberculosis (TB) Infection in Children – New Jersey Medical School Global TB Institute
- Tuberculosis Screening for International Adoptees Frequently Asked Questions (FAQs)
For Clinicians
- Reported Tuberculosis in the United States, 2021
- Epidemiology of Pediatric Tuberculosis in the United States, 1993–2017 (Slide Set)
- TB Guidelines: Treatment
- Guidelines for the Prevention and Treatment of Opportunistic Infections in Children with and Exposed to HIV
- Red Book Online – American Academy of Pediatrics
- Pediatric TB CD and Webinar – Southeastern National Tuberculosis Center
- Pediatric Tuberculosis: An Online Presentation – Francis J. Curry National Tuberculosis Center
- Cruz AT and Starke JR. Pediatric Tuberculosis Pediatrics in Review. 2010: 31 (1): 13–26