Global Stories

COVID-19’s global spread has resulted in an unprecedented need for infection prevention and control (IPC) in healthcare facilities. Without such measures, COVID-19 can spread rapidly among healthcare workers and patients, putting them at risk and interrupting essential healthcare services. To help slow the spread of COVID-19, CDC, the University of Washington International Training and Education Center for Health (UW I-TECH), and the Kenya Ministry of Health (MOH) partnered in two consecutive, rapid IPC capacity national assessments of healthcare facilities.

Haiti has the highest rate of human rabies in the Western Hemisphere, and street dogs with rabies are a major problem. Every week on average, two people in Haiti die of rabies. To control rabies in Haiti, NCEZID focuses on strengthening surveillance, vaccinating dogs, and providing better treatment to people after dog bites.
In Uganda, several recent human cases of infection with Marburg virus have surfaced with links to Egyptian fruit bats, and people in nearby villages have experienced devastating outbreaks. CDC worked with Ugandan experts to put GPS units on the bats’ backs to track their movements.

Only 2% of people in Sierra Leone have access to clean, readily available drinking water. Public health officials and partners in Sierra Leone asked CDC to help strengthen the country’s water, sanitation, and hygiene workforce to combat diseases and better prepare for future disasters or outbreaks.
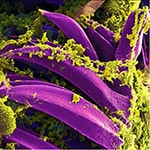
NCEZID scientists teamed up with the Uganda Virus Research Institute and its Arua Field Station to strengthen the prevention, detection, and control of plague in Uganda. Arua Field Station staff have been instrumental in engaging with communities, health care workers, and traditional healers to promote the early detection of plague, which is a rare but fatal infection.
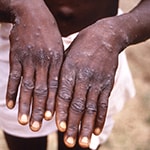
The Democratic Republic of the Congo (DRC) has one of the world’s highest rates of human monkeypox, a rare but serious re-emerging illness that kills up to 1 in 10 infected people. NCEZID scientists are evaluating the effectiveness of a new smallpox vaccine to prevent infection in health care workers and laboratorians in DRC who are regularly exposed to monkeypox.

Cholera kills an estimated 95,000 people each year and sickens 2.9 million more. As part of the Ending Cholera Initiative launched by the Global Task Force for Cholera Control, CDC is helping Kenya and Tanzania develop national plans to end cholera by 2030.

NCEZID has collaborated with the government of Indonesia to build a state-of-the-art research laboratory capable of performing cutting-edge diagnostic work. Partnering with Indonesia has led to the first isolation of West Nile and Zika viruses and completion of a Zika virus seroprevalence study.

Each year in India, nearly 60,000 babies die from sepsis related to antibiotic-resistant (AR) infections. NCEZID is sharing its expertise in infection prevention and control and lessons learned from combating AR in US hospitals to stop the spread of these pathogens around the world.

Healthcare personnel in Nigeria save lives every day and put their lives at risk when caring for patients with deadly infections, such as Ebola and Lassa fever. Although some hospitals in Nigeria have specialists responsible for ensuring that infection prevention and control measures are in place to protect these personnel, few of these specialists are appropriately trained to serve in this role. To fill this need for training, Nigerian infection prevention and control experts are working with CDC’s International Infection Control Program (IICP) in the Division of Healthcare Quality and Promotion out of the National Center for Emerging and Zoonotic Infectious Diseases and other international partners.
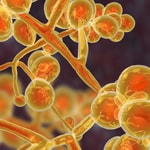
Disease knows no borders, as demonstrated by the emergence and movement of C. auris around the world. The challenge of an emerging threat like C. auris requires an urgent and comprehensive response at all levels – local, state, federal, and international. To date, it has been detected in more than 20 countries, including the United States. Using whole genome sequencing, CDC scientists identified four different groups of C. auris that have emerged since 2009 in different parts of the world. In response, CDC is working with other countries to improve detection and implement aggressive control measures.

In India, bacteria that cause common infections, such as urinary tract and bloodstream infections, are becoming resistant to nearly all antibiotics. This resistance is due to a combination of factors: uncontrolled access to antibiotics, gaps in infection prevention and control (IPC) practices, and high rates of communicable diseases. Antibiotic resistance, or AR, is a serious problem throughout the country, and threatens to reduce the usefulness of antibiotics both in India and around the world.

Sometimes, the work of a global disease detective starts just hours after a training session ends. That was the case for a group of Kenyan Field Epidemiology and Laboratory Training Program (FELTP) residents in May 2017, when a Nairobi hospital reported an outbreak of suspected cholera among patients. Four of the patients had attended a wedding in Nairobi.
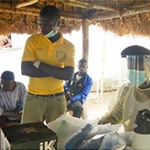
Sierra Leone was one of the three countries hardest hit by the 2014 Ebola outbreak. The severity of the outbreak highlighted the need for immediate international response to save lives and stop the spread to the United States and other countries. To assist with the crisis in Sierra Leone, CDC deployed a team from its International Infection Control Program out of the National Center for Emerging and Zoonotic Infectious Diseases Center’s Division of Healthcare Quality Promotion.

In the mountainous country of Georgia, the healthcare system is dominated by private corporations, which manage approximately 90% of the hospital beds. Rarely are healthcare personnel trained in infection prevention and control (IPC) practices such as hand hygiene and injection safety. Gaps in IPC practices can lead to widespread, healthcare-associated infections (HAIs) and outbreaks that could spread infectious diseases throughout Georgia and across borders, threatening global public health.

Uganda is a focal point for emerging and re-emerging infectious diseases. Many mosquito-borne viruses, known as arboviruses, were discovered in Uganda and continue to circulate. Outbreaks of viral hemorrhagic fevers, including Ebola, Marburg, and yellow fever occur periodically, and plague remains endemic in the highlands of the West Nile region.

Every year, six million children die before their 5th birthday. CDC and partners are working to answer the critical question of why. CDC’s Division of High-Consequence Pathogens and Pathology (DHCPP) out of the National Center for Emerging and Zoonotic Infectious Diseases (NCEZID) has teamed up with domestic and international partners to map the causes of child mortality in developing countries.

An estimated 59,000 people die from rabies each year, nearly half of whom are children. Rabies claims the life of one person every 9 minutes, putting it among the deadliest of all global zoonotic diseases, or diseases that are transmitted between animals and people. In response to Haiti’s rabies epidemic, CDC’s Poxvirus and Rabies Branch (PRB) began a series of interventions to address rabies prevention and containment in Haiti.

Collaboration is the key to success when tackling any complex issue. CDC’s Division of High-Consequence Pathogens and Pathology (DHCPP) discovered just how critical collaboration can be when they launched a project in Ethiopia to tackle some of the country’s dangerous yet neglected zoonotic pathogens.

The 2014 Ebola epidemic was the largest in history, with widespread transmission in multiple West African countries. The first case was reported in Guinea in March 2014, and the disease quickly spread into the neighboring countries of Liberia and Sierra Leone. If the virus reservoir is determined, CDC and other international health partners will be able to issue stronger guidance to local groups about the origins of Ebola virus transmission, making such a widespread outbreak less likely to occur in the future.