Wastewater Surveillance
Wasting no time: CDC adapts wastewater surveillance to stay vigilant for emerging threats
The COVID-19 pandemic made the value of sewage clear. For epidemiologists, CDC’s National Wastewater Surveillance System (NWSS) provides invaluable insights by helping identify community infection trends before they appear in clinical cases. In 2022, NWSS enhanced detection of SARS-CoV-2 and its variants. But perhaps equally critical were efforts to adapt wastewater surveillance for other emerging infectious disease challenges.
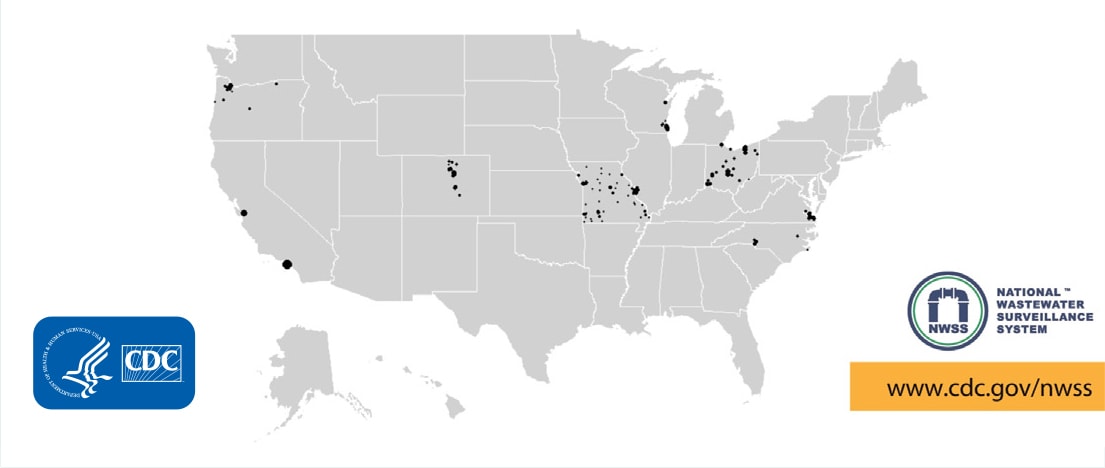
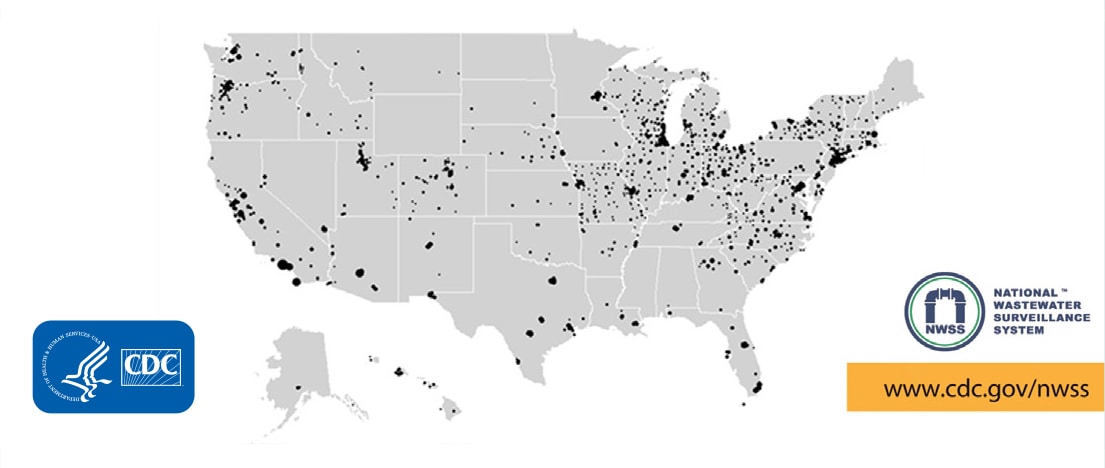
CDC’s National Center for Emerging and Zoonotic Infectious Diseases (NCEZID) launched NWSS in September 2020 to track the presence of SARS-CoV-2 in community-level wastewater samples collected from sewersheds across the United States. Building on initial investments, CDC worked with public health, utility, private sector, academic, and federal partners to track SARS-CoV-2 and scale the surveillance system to include an estimated 1,200 testing sites across the United States, including in territories and on tribal lands.

Amy Kirby, PhD, MPH, National Wastewater Surveillance System
Team Lead for CDC’s NCEZID Waterborne
Disease Prevention Branch, Division of Foodborne,
Waterborne, and Environmental Diseases
“One of the strengths of wastewater surveillance is that it is very flexible. We’ve structured the NWSS platform to rapidly adapt to changing public health needs. As new needs arise, we are prepared to test, adapt, and expand on the strong foundation we’ve built.’’

Building National Wastewater Surveillance
Since 2020, hundreds of communities have started reporting wastewater data to CDC’s National Wastewater Surveillance System to track COVID-19.
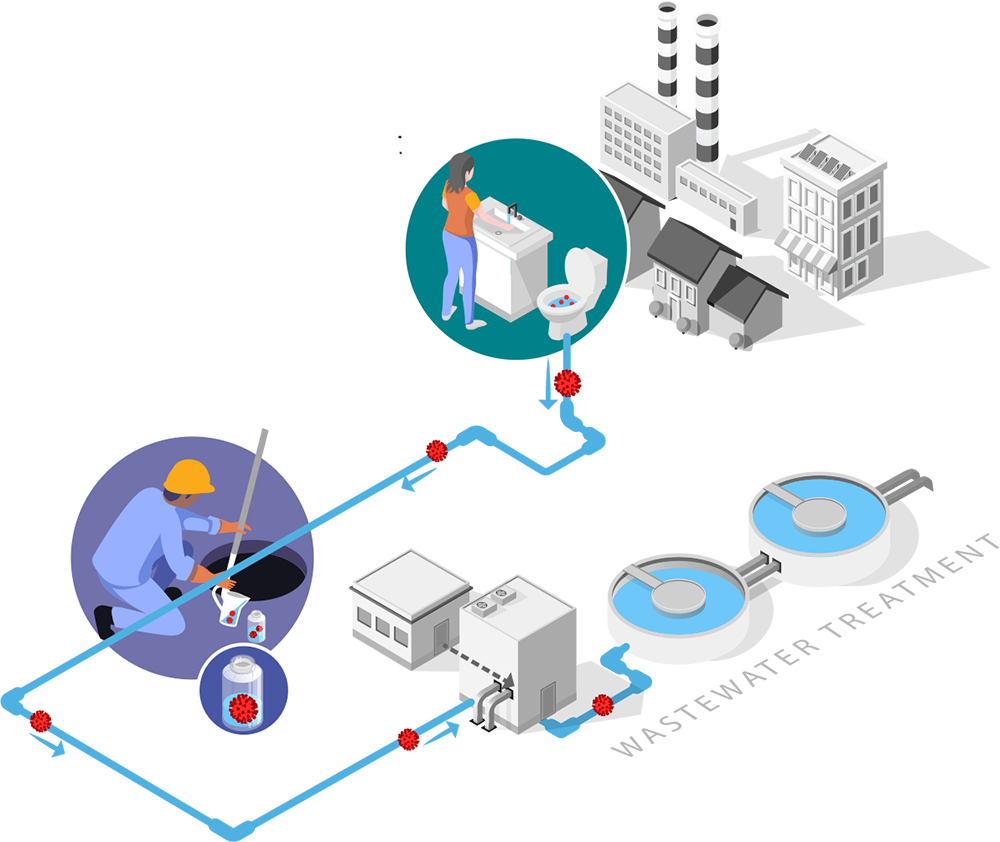
Wastewater Surveillance: How Does It Work?
Wastewater surveillance can help communities detect and prepare for increasing cases of COVID-19. Data are available quickly, 5 to 7 days after the toilet flush.
The system analyzed over 90,000 community-level samples from wastewater systems that serve more than 2 in 5 people in the United States (nearly 150 million people). Many public health agencies used these surveillance data to detect early evidence of SARS-CoV-2 variants in community wastewater. In fact, wastewater surveillance programs in California, Colorado, New York City, and Houston, Texas, were among the first to identify the Omicron variant. Wastewater test results combined with other surveillance efforts helped guide public health decisions.
In fall 2022, NWSS incorporated mpox testing into the existing surveillance network and has been providing data to health departments through CDC’s Data Collation and Integration for Public Health Event Response (DCIPHER) platform. Signals of mpox virus in community wastewater helped public health officials better understand the extent of the mpox outbreak and monitor the impact of large public events on local spread.
CDC and public health partners have been exploring ways to use NWSS to better respond to other threats detectable in wastewater, such as antimicrobial-resistant pathogens; foodborne pathogens like E. coli; respiratory viruses like influenza; and emerging pathogens like Candida auris. For example, in fall 2022, NWSS began supporting poliovirus testing in strategic sites as part of CDC’s New York State Polio Response, although poliovirus wastewater surveillance is currently not part of routine NWSS testing.
Wastewater surveillance is not only a valuable tool to guide public health decisions. It also offers an opportunity to better identify and address health inequities through efficient, non-invasive sampling that could support historically marginalized communities, including those with limited access to services. Expansion of NWSS capabilities, participation, and strengthened relationships with wastewater partners will help prepare communities to detect and track disease threats now and in years to come.
Wastewater surveillance provides a wealth of powerful data that could signal an important early warning of emerging infectious disease threats.
CDC is exploring the possibility and benefit of monitoring for other health threats detectable in wastewater, including antimicrobial-resistant pathogens, Shiga toxin-producing E. coli, norovirus, and influenza. Early detection and infection prevention and control measures are critical to prevent extensive transmission.