Influenza Vaccination Coverage Among Health Care Personnel — United States, 2018–19 Influenza Season
The Advisory Committee on Immunization Practices (ACIP) recommends that all health care personnel (HCP) receive an annual influenza vaccination to reduce influenza-related morbidity and mortality among HCP and their patients and to reduce absenteeism among HCP (1-4). CDC conducted an opt-in Internet panel survey of 2,386 U.S. HCP to estimate influenza vaccination coverage during the 2018–19 influenza season. Overall, 81.1% of HCP reported receiving influenza vaccination during the 2018–19 season, similar to reported coverage in the previous four influenza seasons (5). As in past seasons, the highest coverage (97.7%) was among HCP with workplace vaccination requirements and the lowest (42.1%) among those working in settings where vaccination was not required, promoted, or offered on-site. Although the proportions of HCP who reported an employer vaccination requirement and various vaccination incentives did not change, vaccination coverage increased from the 2017-18 to the 2018-19 season among those who worked in locations where vaccination was available at the worksite at no cost for >1 day (7.2 percentage points) and among those with vaccination available for 1 day only (5.1 percentage points). Vaccination coverage decreased 5.5 percentage points among those working in settings where vaccination was not required, promoted, or offered on-site. Implementing workplace strategies shown to improve vaccination coverage among HCP, including active promotion of on-site vaccinations at no cost, can help ensure HCP and patients are protected against influenza (6).
An Internet panel survey of HCP was conducted for CDC during March 26–April 18, 2019, to provide estimates of influenza vaccination coverage among HCP during the 2018–19 influenza season. Similar surveys have been conducted since the 2010–11 influenza season, and survey methodology has been described previously (7). Respondents were recruited from two preexisting national opt-in Internet sources: Medscape, a medical website managed by WebMD Health Professional Network,* and general population Internet panels operated by Dynata (formerly known as Survey Sampling International (SSI)). † Responses were weighted to the distribution of the U.S. population of HCP by occupation, age, sex, race/ethnicity, work setting, and Census region. ‡ Because the study sample was based on HCP from opt-in Internet panels rather than probability samples, statistical tests were not conducted. § A change of at least 5 percentage points between estimates has consistently been used with this survey to denote an increase or decrease; estimates with smaller differences were considered similar (8, 9).
Among the 2,512 persons who started the survey from either source (Medscape or Dynata) and met eligibility criteria based on responses to the screening questions (i.e., were not screened out due to employment status, work setting, occupation, race, or incomplete response to the screening questions), 2,432 (96.6%) individuals completed the survey. || Forty-five respondents (1.9%) with completed surveys who reported working in “other health care settings” were excluded because examination of their survey responses indicated that they were either unlikely to have contact with patients or unlikely to have worked in one of the health care settings of interest for this analysis; one additional respondent was excluded because they did not provide a reliable response to the vaccination question. The final analytic sample included 2,386 HCP.
Overall, 81.1% of HCP reported having received an influenza vaccination during the 2018–19 season, similar to reported coverage in the previous four seasons (77.3%–79.0%) (Figure 1) (Figure 2). Vaccination coverage in the 2018–19 season was similar to that in the 2017–18 season among HCP in all work settings (Figure 1) and occupation groups (Figure 2). As in previous seasons, coverage in the 2018–19 season was highest among HCP working in hospital settings (95.2%) followed by those working in ambulatory care (79.8%), other clinical settings (77.9%), and long-term care settings (67.9%) (Figure 1). Overall, vaccination coverage in 2018–19 was higher among physicians (96.7%), nurses (91.8%), pharmacists (91.5%), and nurse practitioners and physician assistants (91.0%), and lower among other clinical HCP (85.8%), assistants and aides (72.5%), and nonclinical HCP (75.5%) (Figure 2).
Overall, in the 2018-19 season vaccination coverage (97.7%) was highest among HCP working in settings where vaccination was required (Table). Among HCP whose employers did not have a requirement for vaccination, coverage was higher among those who worked in locations where vaccination was available at the worksite at no cost for >1 day (83.2%) than among those with vaccination available for 1 day only (75.6%) or among those who worked in locations where their employer did not provide influenza vaccination on-site at no cost but actively promoted vaccination through other mechanisms¶ (75.6%). Having an employer vaccination requirement was reported more frequently (44.8%) than having vaccination available at the worksite at no cost for >1 day (14.4%) or having vaccination available for 1 day only (11.3%). Vaccination coverage increased from the 2017-18 to the 2018-19 season among those who worked in locations where vaccination was available at the worksite at no cost for >1 day (7.2 percentage points) and among those with vaccination available for 1 day only (5.1 percentage points). Vaccination coverage (42.1%) was lowest among those working in settings where vaccination was not required, promoted, or offered on-site, which accounted for 16.6% of HCP. Vaccination coverage among this group was 5.5 percentage points lower in 2018-19 than in the 2017-18 season.
The overall influenza vaccination coverage among HCP was 81.1% during the 2018–19 influenza season, similar to coverage during the previous four seasons (5). As in past seasons, the highest coverage was associated with workplace vaccination requirements. Vaccination coverage has plateaued since the 2014-15 season (ranging from 77.3% to 79.0%), as the proportion of HCP reporting an employer vaccination requirement has remained relatively stable (37.8% to 44.8%) (5, 6). Although the proportions of HCP who reported various vaccination incentives did not change, vaccination coverage increased from the 2017-18 to the 2018-19 season among those who worked in locations where vaccination was available at the worksite at no cost for >1 day (7.2 percentage points) and among those with vaccination available for 1 day only (5.1 percentage points). During those seasons, vaccination coverage decreased 5.5 percentage points among those working in settings where vaccination was not required, promoted, or offered on-site. Recommendations found in the Guide to Community Preventive Services, which include actively promoted on-site vaccination at no cost, can be used by health care employers to increase influenza vaccination coverage among HCP (6), and thereby protect HCP and patients against influenza. HCP in long-term care settings continued to have lower influenza vaccination coverage. Long-term care employers can use CDC’s long-term care web-based toolkit**, which provides access to resources, strategies, and educational materials for increasing influenza vaccination among HCP and reducing influenza-associated morbidity and mortality among patients in long-term care settings.
* Persons who worked in a place where clinical care or related services were provided to patients, or whose work involved face-to-face contact with patients or who were ever in the same room as patients.
† Respondents were recruited from two preexisting national opt-in Internet sources: Medscape, a medical website managed by WebMD Health Professional Network, and general population Internet panels operated by Dynata (formerly Survey Sampling International).
‡ Weights were calculated based on each occupation type, by age, sex, race/ethnicity, work setting, and U.S. Census region to represent the U.S. population of health care personnel.
§ Physicians, dentists, nurse practitioners, physician assistants, nurses, allied health professionals, pharmacists, and students in a medical-related field.
|| Technicians/technologists; emergency technicians, paramedics, and EMTs; and assistants/aides.
¶ Administrative support staff/managers, housekeeping and food service staff, and other nonclinical support staff.
** Ambulatory care (physician’s office, medical clinic, and other ambulatory care setting).
†† Dentist office or dental clinic, pharmacy, laboratory, public health setting, health care education setting, emergency medical services setting, or other setting where clinical care or related services was provided to patients.
‡‡ Rurality was defined using ZIP codes where more than 50% of its population resides in either a Non-Metro County and/or a rural Census Tract, according to the U.S. Health Resources & Service
Administration’s definition of rural population
§§ Includes all respondents who indicated that their employer required them to be vaccinated for influenza.
|||| Employer made influenza vaccination available on-site for >1 day during the influenza season at no cost to employees. Restricted to respondents without an employer requirement for vaccination.
¶¶ Employer made influenza vaccination available on-site for 1 day during the influenza season at no cost to employees. Restricted to respondents without an employer requirement for vaccination.
*** Influenza vaccination was promoted among employees through public identification of vaccinated persons, financial incentives or rewards to individuals or groups of employees, competition between units or care areas, free or subsidized cost of vaccination, personal reminders to be vaccinated, or publicizing of the number or percentage of employees receiving vaccination. Restricted to respondents without an employer requirement for vaccination or on-site vaccination.
FIGURE 1. Percentage of health care personnel who received influenza vaccination, by work setting* — Internet panel surveys,† United States, 2010–11 through 2018–19 influenza seasons
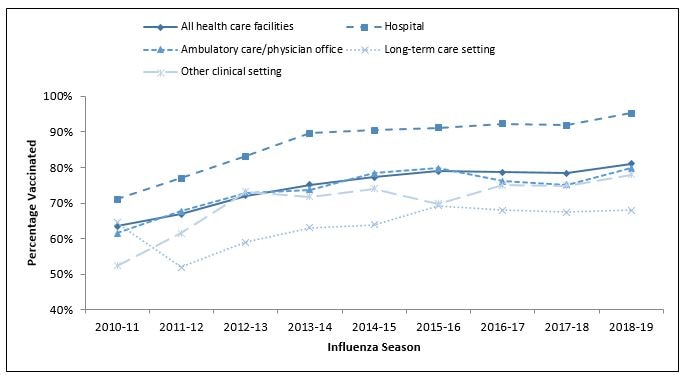
* Respondents could select more than one work setting. The “ambulatory care/physician office” category includes physician’s office, medical clinic, and other ambulatory care settings. The “other clinical setting” category includes dentist office or dental clinic, pharmacy, laboratory, public health setting, emergency medical services setting, or other setting where clinical care or related services were provided to patients.
† Respondents were recruited from two preexisting national opt-in Internet sources: Medscape, a medical website managed by WebMD Health Professional Network, and general population Internet panels operated by Dynata.
FIGURE 2. Percentage of health care personnel who received influenza vaccination, by occupation* — Internet panel surveys,† United States, 2010–11 through 2018–19 influenza seasons
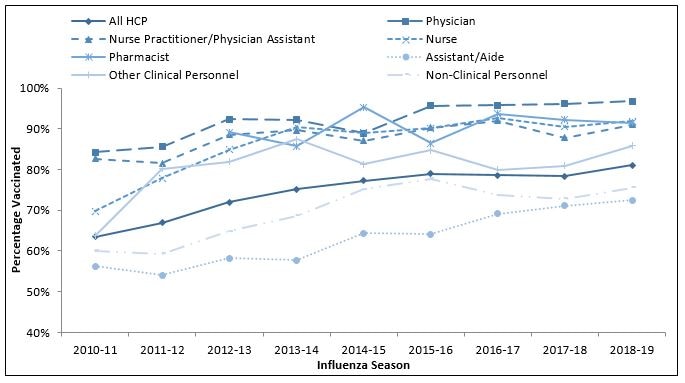
* In the 2010–11 season, dentists were included in the physician category. Before the 2012–13 season, separate data on pharmacists were not collected. Other clinical personnel category includes allied health professionals, technicians, and technologists. Nonclinical personnel category includes administrative support staff members or managers and nonclinical support staff members (e.g., food service workers, laundry workers, janitors, and other housekeeping and maintenance staff members).
† Respondents were recruited from two preexisting national opt-in Internet sources: Medscape, a medical website managed by WebMD Health Professional Network, and general population Internet panels operated by Dynata.
The findings in this report are subject to at least three limitations. First, the study used a nonprobability sample of volunteer members of Medscape and SSI/Dynata Internet panels, which might affect the generalizability of these findings to the U.S. population of HCP. Second, vaccination status was self-reported and might be subject to recall bias. Finally, coverage findings from Internet survey panels have differed from population-based estimates from the National Health Interview Survey in past influenza seasons, although trends in coverage were similar across seasons.
Authors: Barbara Bardenheier, PhD, MPH, MA1; Megan C. Lindley, MPH1; Xin Yue, MPS, MS1,2; Ivy Oyegun, MPH1,3; Sarah W. Ball, ScD, MPH4; Rebecca Devlin, MA4; Marie A. de Perio, MD, FIDSA5; A. Scott Laney, PhD6; Peng-Jun Lu, MD, PhD1; Rebecca V. Fink, MPH4
1Immunization Services Division, National Center for Immunization and Respiratory Diseases, CDC; 2Leidos, Reston, VA; 3Eagle Medical Services, LLC, Atlanta, GA; 4Abt Associates, Inc., Cambridge, Massachusetts; 5 Division of Surveillance, Hazard Evaluations, and Field Studies, National Institute for Occupational Safety and Health, CDC; 6 Division of Respiratory Health, National Institute for Occupational Safety and Health, CDC.
*Physicians, nurse practitioners, physician assistants, nurses, dentists, pharmacists, allied health professionals, technicians, and technologists were recruited from the current membership roster of Medscape. Additional information on Medscape is available.
†Assistants, aides, and nonclinical personnel (such as administrators, clerical support workers, janitors, food service workers, and housekeepers) were recruited from general population Internet panels operated by Dynata. Additional information on Dynata and its incentives for online survey participants is available.
‡Population control totals of U.S. health care personnel by occupation and work setting were obtained from the Bureau of Labor Statistics, U.S. Department of Labor, Occupational Employment Statistics, May 2016 National Industry-Specific Occupational Employment and Wage Estimates. Population control totals by other demographic characteristics were obtained from the U.S. Census Bureau, Current Population Survey Monthly Labor Force Data, September 2018.
§Additional information on obstacles to inference in nonprobability samples is available at: Report Of the Aapor Task Force on Non-Probability Sampling and AAPOR Guidance on Reporting Precision for Nonprobability Samples. While the estimates reported here have variance, there has been no attempt to quantify the size of the variance.
||A survey response rate requires specification of the denominator at each stage of sampling. During recruitment of an online opt-in survey sample, such as the Internet panels described in this report, these numbers are not available; therefore, a response rate cannot be calculated. Instead, the survey completion rate is provided.
¶ Employer promoted influenza vaccination among employees through public identification of vaccinated persons, financial incentives or rewards to individual persons or groups of employees, competition between units or care areas, free or subsidized cost of vaccination, personal reminders to be vaccinated, or publicizing of the number or percentage of employees receiving vaccination.
- Centers for Disease Control and Prevention (CDC). Immunization of health-care personnel: recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR Recomm Rep. 2011;60(RR-7):1-45.
- Hayward AC, Harling R, Wetten S, et al. Effectiveness of an influenza vaccine programme for care home staff to prevent death, morbidity, and health service use among residents: cluster randomised controlled trial. BMJ. 2006;333(7581):1241-1244.
- Lemaitre M, Meret T, Rothan-Tondeur M, et al. Effect of influenza vaccination of nursing home staff on mortality of residents: a cluster-randomized trial. J Am Geriatr Soc. 2009;57(9):1580-1586.
- Saxen H, Virtanen M. Randomized, placebo-controlled double blind study on the efficacy of influenza immunization on absenteeism of health care workers. Pediatr Infect Dis J. 1999;18(9):779-783.
- Black CL, Yue X, Ball SW, et al. Influenza vaccination coverage among health care personnel – United States, 2017-18 influenza season. MMWR Morb Mortal Wkly Rep. 2018;67(38):1050-1054.
- Worksite: Seasonal influenza vaccinations using interventions with on-site, free, actively promoted vaccinations – healthcare workers. Community Preventive Services Task Force website. https://www.thecommunityguide.org/findings/worksite-seasonal-influenza-vaccinations-healthcare-on-site. Accessed June 26, 2019.
- Black CL, Yue X, Ball SW, et al. Influenza vaccination coverage among health care personnel – United States, 2013-14 influenza season. MMWR Morb Mortal Wkly Rep. 2014;63(37):805-811.
- Kahn KE, Black CL, Ding H, et al. Influenza and Tdap vaccination coverage among pregnant women – United States, April 2018. MMWR Morb Mortal Wkly Rep. 2018;67(38):1055-1059.
- Kahn KE, Black C, Ding H, et al. Pregnant women and Tdap vaccination, Internet panel survey, United States, April 2017. https://www.cdc.gov/vaccines/imz-managers/coverage/adultvaxview/pubs-resources/tdap-report-2017.html. Accessed June 26, 2019.