FluView Summary ending on July 25, 2020

Note: CDC is tracking the COVID-19 pandemic in a weekly publication called COVIDView.
All data are preliminary and may change as more reports are received.
A description of the CDC influenza surveillance system, including methodology and detailed descriptions of each data component is available on the surveillance methods page.
Additional information on the current and previous influenza seasons for each surveillance component are available on FluView Interactive.
Viruses
Severe Disease
All data are preliminary and may change as more reports are received.
A description of the CDC influenza surveillance system, including methodology and detailed descriptions of each data component is available on the surveillance methods page.
Additional information on the current and previous influenza seasons for each surveillance component are available on FluView Interactive.
Key Points
- Nationally, influenza activity remains low.
- CDC will continue to track influenza activity year-round as always, but as flu activity remains low, an abbreviated FluView will be published weekly during the remainder of the 2019-2020 season.
- More detailed interpretation of data and COVID-19 specific information can be found in COVIDView
U.S. Virologic Surveillance:
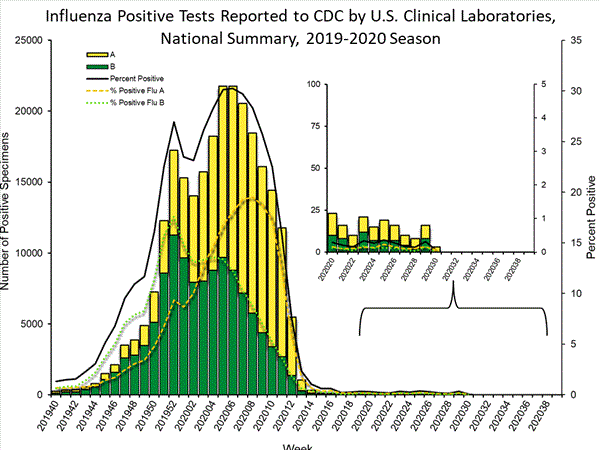
Clinical Laboratories
Data from clinical laboratories (the percentage of specimens tested that are positive for influenza) are used to monitor whether influenza activity is increasing or decreasing.
| Week 27
|
Data Cumulative since September 29, 2019 (week 40) |
|
|---|---|---|
| No. of specimens tested | 22,324 | 1,303,970 |
| No. of positive specimens (%) | 180 (0.8%) | 247,785 (19.0%) |
| Positive specimens by type | ||
| Influenza A | 105 (58.3%) | 132,461 (53.5%) |
| Influenza B | 75 (41.7%) | 115,324 (46.5%) |
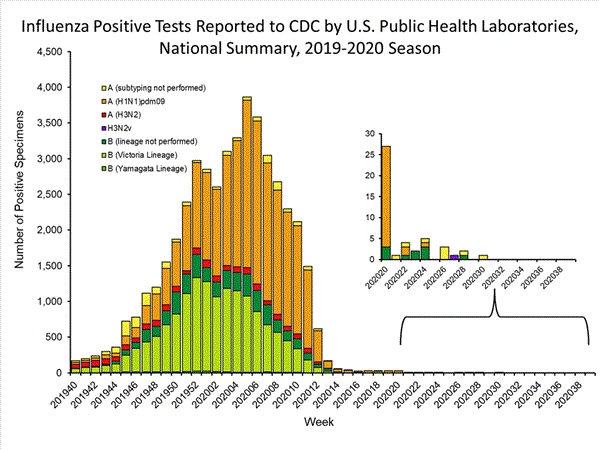
Public Health Laboratories
Data from public health laboratories are used to monitor the proportion of circulating viruses that belong to each influenza subtype/lineage.
| Week 27 | Data Cumulative since September 29, 2019 (week 40) |
|
|---|---|---|
| No. of specimens tested | 356 | 81,392 |
| No. of positive specimens | 35 | 43,456 |
| Positive specimens by type/subtype | ||
| Influenza A | 31 (88.6%) | 24,822 (57.1%) |
| (H1N1)pdm09 | 28 (96.6%) | 22,324 (92.6%) |
| H3N2 | 1 (3.4%) | 1,780 (7.4%) |
| Subtyping not performed | 2 | 718 |
| Influenza B | 4 (11.4%) | 18,634 (42.9%) |
| Yamagata lineage | 0 (0.0%) | 238 (1.6%) |
| Victoria lineage | 0 (0.0%) | 14,198 (98.4%) |
| Lineage not performed | 4 | 4,198 |
While influenza B/Victoria viruses predominated earlier in the season, during recent weeks, influenza A(H1N1)pdm09 viruses have been reported more frequently than B/Victoria viruses nationally and in all surveillance regions. For the season, A(H1N1)pdm09 viruses are the predominant virus nationally. Regional and state level data about circulating influenza viruses can be found on FluView Interactive.
The predominant virus also varies by age group. Nationally, for the season overall, influenza B viruses are the most commonly reported influenza viruses among persons 5-24 years, while influenza A viruses are the most commonly reported influenza viruses among persons 0-4 years and 25 years and older. In the most recent three weeks, influenza A viruses are the most commonly reported influenza viruses in all age groups.
Additional virologic surveillance information for current and past seasons:
Surveillance Methods | FluView Interactive: National, Regional, and State Data or Age Data
Influenza Virus Characterization
CDC performs genetic and antigenic characterization of U.S. viruses submitted from state and local health laboratories using Right Size Roadmap submission guidance. These data are used to compare how similar the currently circulating influenza viruses are to the reference viruses used for developing new influenza vaccines and to monitor evolutionary changes that continually occur in circulating influenza viruses. Antigenic characterization data are based on an animal model (influenza-naive ferrets), and do not reflect pre-existing protection provided by past influenza infections and vaccinations. Additional antigenic characterization studies involving people vaccinated with current influenza vaccines are conducted later in the season; these data account for pre-existing protection in different populations against circulating influenza viruses. Genetic and antigenic characterization data are not used to make calculations about vaccine effectiveness (VE). CDC conducts VE studies each year to measure the benefits of flu vaccines in people. Interim estimates of 2019-2020 flu vaccine effectiveness have been released.
CDC genetically characterized 2,463 influenza viruses collected in the U.S. from September 29, 2019, to April 4, 2020.
| Virus Subtype or Lineage | Genetic Characterization | ||||
|---|---|---|---|---|---|
| Total No. of Subtype/Lineage Tested |
Clade | Number (% of subtype/lineage tested) |
Subclade | Number (% of subtype/lineage tested) |
|
| A/H1 | 896 | ||||
| 6B.1A | 896 (100%) | ||||
| A/H3 | 510 | ||||
| 3C.2a | 480 (94.1%) | 2a1 | 480 (94.1%) | ||
| 2a2 | 0 | ||||
| 2a3 | 0 | ||||
| 2a4 | 0 | ||||
| 3C.3a | 30 (5.9%) | 3a | 30 (5.9%) | ||
| B/Victoria | 965 | ||||
| V1A | 965 (100%) | V1A | 0 | ||
| V1A.1 | 60 (6.2%) | ||||
| V1A.3 | 905 (93.8%) | ||||
| B/Yamagata | 92 | ||||
| Y3 | 92 (100%) | ||||
CDC antigenically characterizes a subset of influenza viruses by hemagglutination inhibition (HI) or neutralization based Focus Reduction assays (FRA). Antigenic drift is evaluated by comparing antigenic properties of cell-propagated reference viruses representing currently recommended vaccine components with those of cell-propagated circulating viruses. CDC antigenically characterized 547 influenza viruses collected in the United States from September 29, 2019, to April 4, 2020. These data are not used to make calculations about vaccine effectiveness (VE). CDC conducts VE studies each year to measure the benefits of flu vaccines in people.
Influenza A Viruses
- A (H1N1)pdm09: 212 A(H1N1)pdm09 viruses were antigenically characterized by HI with ferret antisera, and 175 (82.5%) were antigenically similar (reacting at titers that were within 4-fold of the homologous virus titer) to cell-propagated A/Brisbane/02/2018-like reference viruses representing the A(H1N1)pdm09 component for the 2019-20 Northern Hemisphere influenza vaccines. The decrease in the percent of A(H1N1)pdm09 viruses similar to A/Brisbane/02/2018 is due to some of the recent viruses selected for testing having a single amino acid change that is antigenically distinguishable in antigenic assays using ferret sera. Similar viruses were observed last season as well and these represented a small proportion of virus circulating. We have observed an increase in the proportion of H1N1pdm09 viruses with this change late in the US season.
- A (H3N2): 86 A(H3N2) viruses were antigenically characterized by FRA with ferret antisera, and 40 (46.5%) were antigenically similar to cell-propagated A/Kansas/14/2017-like reference viruses representing the A(H3N2) component for the 2019-20 Northern Hemisphere influenza vaccines.
Influenza B Viruses
- B/Victoria: 201 B/Victoria lineage viruses, including viruses from both co-circulating sub-clades, were antigenically characterized by HI with ferret antisera, and 120 (59.7%) were antigenically similar to cell-propagated B/Colorado/06/2017-like reference viruses representing the B/Victoria component for the 2019-20 Northern Hemisphere influenza vaccines.
- B/Yamagata: 48 B/Yamagata lineage viruses were antigenically characterized by HI with ferret antisera, and all 48 (100%) were antigenically similar to cell-propagated B/Phuket/3073/2013-like reference viruses representing the B/Yamagata component for the 2019-20 Northern Hemisphere influenza vaccines.
CDC also assesses susceptibility of influenza viruses to the antiviral medications including the neuraminidase inhibitors (oseltamivir, zanamivir, and peramivir) and the PA endonuclease inhibitor baloxavir using next generation sequence analysis supplemented by laboratory assays. Viruses collected in the United States since September 29, 2019, were tested for antiviral susceptibility as follows:
| Antiviral Medication | Total Viruses* |
A/H1 | A/H3 | B/Victoria | B/Yamagata | ||
|---|---|---|---|---|---|---|---|
| Neuraminidase Inhibitors |
|||||||
| Oseltamivir | Viruses Tested |
2,433 | 885 | 502 | 954 | 92 | |
| Reduced Inhibition |
1 (0.04%) | (0.0%) | (0.0%) | 1 (0.1%) | (0.0%) | ||
| Highly Reduced Inhibition |
4 (0.2%) | 4 (0.5%) | (0.0%) | (0.0%) | (0.0%) | ||
| Peramivir | Viruses Tested |
2,433 | 885 | 502 | 954 | 92 | |
| Reduced Inhibition |
(0.0%) | (0.0%) | (0.0%) | (0.0%) | (0.0%) | ||
| Highly Reduced Inhibition |
5 (0.2%) | 4 (0.5%) | (0.0%) | 1 (0.1%) | (0.0%) | ||
| Zanamivir | Viruses Tested |
2,433 | 885 | 502 | 954 | 92 | |
| Reduced Inhibition |
2 (0.1%) | (0.0%) | (0.0%) | 2 (0.2%) | (0.0%) | ||
| Highly Reduced Inhibition |
(0.0%) | (0.0%) | (0.0%) | (0.0%) | (0.0%) | ||
| PA Endonuclease Inhibitor | Baloxavir | Viruses Tested |
2,541 | 884 | 584 | 978 | 95 |
| Reduced Susceptibility |
(0.0%) | (0.0%) | (0.0%) | (0.0%) | (0.0%) | ||
* Six influenza viruses showed reduced or highly reduced inhibition by at least one neuraminidase inhibitor. Four A(H1N1)pdm09 viruses showed highly reduced inhibition to oseltamivir and peramivir while showing normal inhibition to zanamivir. In addition, one B/Victoria virus showed highly reduced inhibition to peramivir and reduced inhibition to oseltamivir and zanamivir, while another influenza B/Victoria virus showed reduced inhibition to zanamivir.
A total of 556 additional viruses (211 A(H1N1)pdm09, 32 A(H3N2), and 313 B) collected in Alabama, Alaska, Florida, Illinois, Iowa, Louisiana, Massachusetts, Michigan, Nevada, New York, North Carolina, Pennsylvania, South Dakota, Virginia and Wisconsin were analyzed for resistance to neuraminidase inhibitors by pyrosequencing assay. Three (1.4%) of the 211 A(H1N1)pdm09 viruses tested had the H275Y amino acid substitution in the neuraminidase and showed highly reduced inhibition by oseltamivir and peramivir. No molecular markers associated with reduced or highly reduced inhibition by neuraminidase inhibitors were detected in A(H3N2) and type B viruses tested.
Novel Influenza A Virus
One human infection with a novel influenza A virus was reported by Hawaii. This person was infected with an influenza A(H3N2) variant (A(H3N2)v) virus. The patient is a child < 18 years of age, was not hospitalized, and has recovered from their illness. While no exposure to swine has been reported to date, an investigation is ongoing into the source of the patient’s infection. This is the first influenza A(H3N2)v virus infection detected in the United States since 2018.
Influenza viruses that circulate in swine are called swine influenza viruses when isolated from swine, but are called variant viruses when isolated from humans. Seasonal influenza viruses that circulate worldwide in the human population have important antigenic and genetic differences from influenza viruses that circulate in swine.
Early identification and investigation of human infections with novel influenza A viruses are critical so that the risk of infection can be more fully understood and appropriate public health measures can be taken. Additional information on influenza in swine, variant influenza infection in humans, and strategies to interact safely with swine can be found at http://www.cdc.gov/flu/swineflu/index.htm.
Additional information regarding human infections with novel influenza A viruses can be found at http://gis.cdc.gov/grasp/fluview/Novel_Influenza.html.
Outpatient Illness Surveillance
ILINet
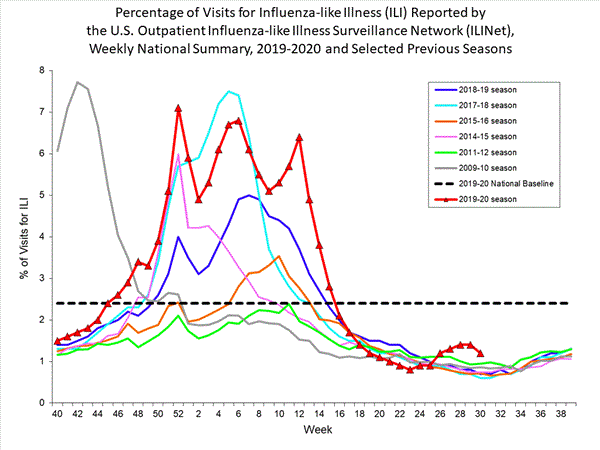
Nationwide during week 30, 1.2% of patient visits reported through the U.S. Outpatient Influenza-like Illness Surveillance Network (ILINet) were due to influenza-like illness (ILI). This percentage is below the national baseline of 2.4%.
Note: In response to the COVID-19 pandemic, new data sources will be incorporated into ILINet as we move into summer weeks when lower levels of influenza and other respiratory virus circulation are typical. Starting in week 21, increases in the number of patient visits will be seen as new sites are enrolled and the percentage of visits for ILI may change in comparison to previous weeks. While all regions remain below baseline levels for ILI, these system changes should be kept in mind when drawing conclusions from these data. Any changes in ILI due to changes in respiratory virus circulation will be highlighted here.
On a regional level, the percentage of outpatient visits for ILI ranged from 0.9% to 2.8% during week 27. Compared to last week, the percent of outpatient visits for ILI increased slightly in region 7, but decreased in all other regions. All regions reported a percentage of outpatient visits for ILI below their region-specific baselines.
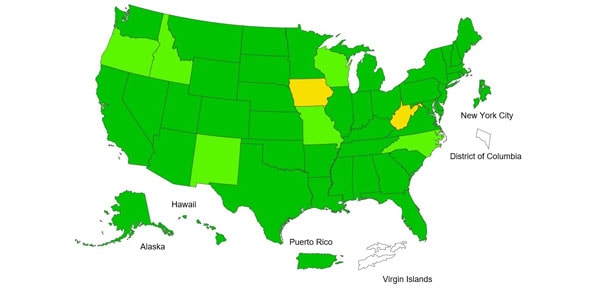
ILI Activity Map
Data collected in ILINet are used to produce a measure of ILI activity* by state.
During week 30, the following ILI activity levels were experienced:
- Moderate – Puerto Rico.
- Low –One state (Louisiana).
- Minimal –New York City and 49 states (Alabama, Alaska, Arizona, Arkansas, California, Colorado, Connecticut, Delaware, Florida, Georgia, Hawaii, Idaho, Illinois, Indiana, Iowa, Kansas, Kentucky, Maine, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, Montana, Nebraska, Nevada, New Hampshire, New Jersey, New Mexico, New York, North Carolina, North Dakota, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, South Carolina, South Dakota, Tennessee, Texas, Utah, Vermont, Virginia, Washington, West Virginia, Wisconsin, and Wyoming).
- Data were insufficient to calculate an ILI activity level from the U.S. Virgin Islands and the District of Columbia.
*Data collected in ILINet may disproportionally represent certain populations within a state, and therefore, may not accurately depict the full picture of influenza activity for the whole state. Differences in the data presented here by CDC and independently by some state health departments likely represent differing levels of data completeness with data presented by the state likely being the more complete.
Additional information about medically attended visits for ILI for current and past seasons:
Surveillance Methods | FluView Interactive: National, Regional, and State Data or ILI Activity Map
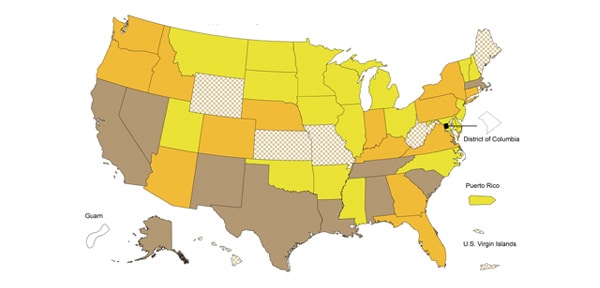
Geographic Spread of Influenza as Assessed by State and Territorial Epidemiologists
The influenza activity reported by state and territorial epidemiologists indicates geographic spread of influenza viruses but does not measure the severity of influenza activity.
During week 24, the following influenza activity was reported:
- Local – Puerto Rico and seven states (Arizona, Indiana, Louisiana, Maryland, North Carolina, Oklahoma and Wisconsin)
- Sporadic – the District of Columbia, the U.S. Virgin Islands and 33 states (Alabama, Alaska, Arkansas, California, Colorado, Connecticut, Florida, Georgia, Hawaii, Idaho, Illinois, Iowa, Maine, Massachusetts, Michigan, Minnesota, Missouri, Montana, Nebraska, Nevada, New Jersey, New York, North Dakota, Ohio, Pennsylvania, South Carolina, South Dakota, Tennessee, Texas, Utah, Washington, West Virginia, and Wyoming)
- No Activity – 10 states (Delaware, Kansas, Kentucky, Mississippi, New Hampshire, New Mexico, Oregon, Rhode Island, Vermont and Virginia)
- Guam did not report.
Additional geographic spread surveillance information for current and past seasons:
Surveillance Methods | FluView Interactive
Influenza-Associated Hospitalizations:
The Influenza Hospitalization Surveillance Network (FluSurv-NET) conducts all age population-based surveillance for laboratory-confirmed influenza-related hospitalizations in select counties in the Emerging Infections Program (EIP) states and Influenza Hospitalization Surveillance Project (IHSP) states.
As in previous seasons, patients admitted for laboratory-confirmed influenza-related hospitalization after April 30, 2020 will not be included in FluSurv-NET. Data on patients admitted through April 30, 2020 will continue to be updated as additional information is received.
The highest rate of hospitalization is among adults aged ≥ 65, followed by children aged 0-4 years and adults aged 50-64 years.
| Age Group | 2019-2020 Season Cumulative Rate per 100,000 Population |
|---|---|
| Overall | 68.2 |
| 0-4 years | 94.1 |
| 5-17 years | 24.6 |
| 18-49 years | 35.6 |
| 50-64 years | 90.2 |
| 65+ years | 179.7 |
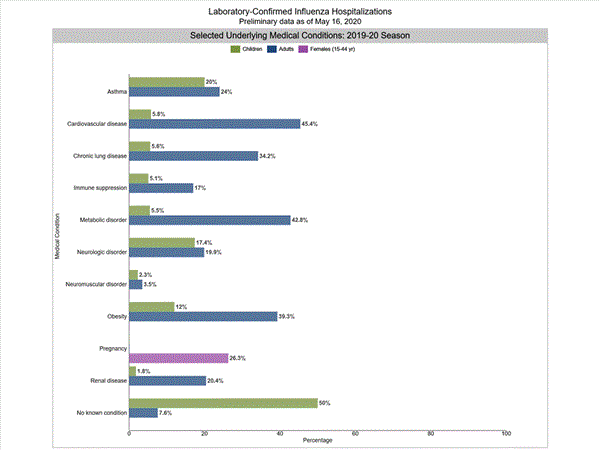
Among 3,433 hospitalized adults with information on underlying medical conditions, 92.3% had at least one reported underlying medical condition, the most commonly reported were cardiovascular disease, metabolic disorder, obesity, and chronic lung disease. Among 569 hospitalized children with information on underlying medical conditions, 48.5% had at least one underlying medical condition; the most commonly reported was asthma. Among 600 hospitalized women of childbearing age (15-44 years) with information on pregnancy status, 27.2% were pregnant.
Additional hospitalization surveillance information for current and past seasons and additional age groups:
Surveillance Methods | FluView Interactive: Rates by Age or Patient Characteristics
Pneumonia and Influenza (P&I) Mortality Surveillance
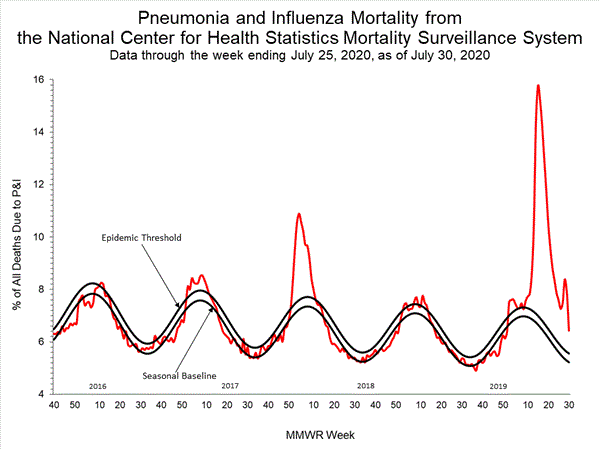
Based on National Center for Health Statistics (NCHS) mortality surveillance data available on July 30, 2020, 6.4% of the deaths occurring during the week ending July 25, 2020 (week 30) were due to P&I. This percentage is above the epidemic threshold of 5.6% for week 30.
Weekly mortality surveillance data include a combination of machine coded and manually coded causes of death collected from death certificates. Percentages of deaths due to pneumonia and influenza (P&I) are higher among manually coded records than more rapidly available machine coded records. Due to the additional time needed for manual coding, the initially reported P&I percentages are likely to increase as more data are received and processed.
While the percent of all deaths due to P&I has increased during weeks 9-13 (7.4-10.0%), the percent of all deaths with Influenza listed as a cause have decreased (from 1.0% to 0.7%) over this same time period. The increase in pneumonia deaths during this time period are likely associated with COVID-19 rather than influenza.
Additional pneumonia and influenza mortality surveillance information for current and past seasons:
Surveillance Methods | FluView Interactive
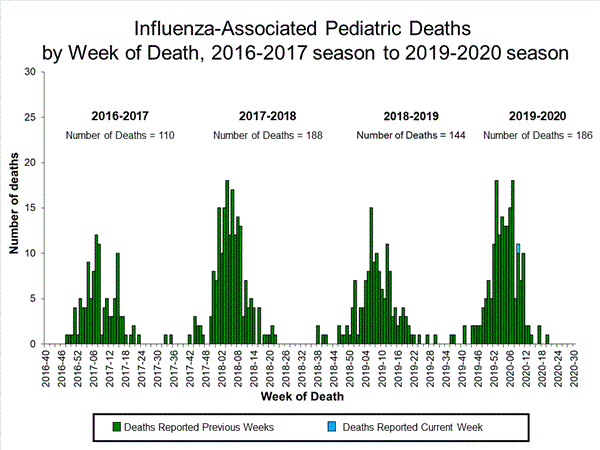
Influenza-Associated Pediatric Mortality
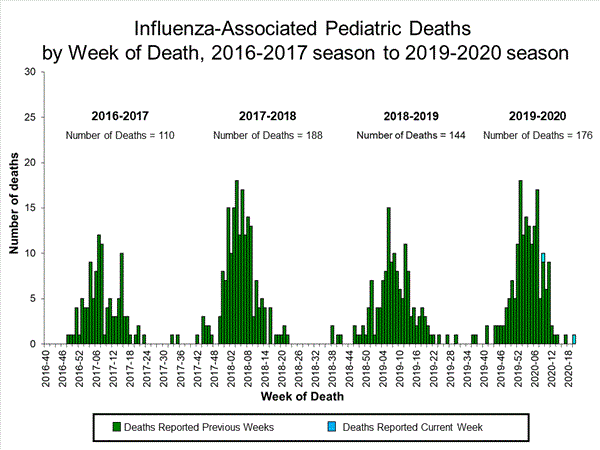
One influenza-associated pediatric deaths occurring during the 2019-2020 season was reported to CDC during week 30. This death was associated with an influenza A(H1N1)pdm09 virus and occurred during week 9 (the week ending February 29, 2020)
A total of 186 influenza-associated pediatric deaths occurring during the 2019-2020 season have been reported to CDC.
Additional pediatric mortality surveillance information for current and past seasons:
Surveillance Methods | FluView Interactive
Additional National and International Influenza Surveillance Information
FluView Interactive: FluView includes enhanced web-based interactive applications that can provide dynamic visuals of the influenza data collected and analyzed by CDC. These FluView Interactive applications allow people to create customized, visual interpretations of influenza data, as well as make comparisons across flu seasons, regions, age groups and a variety of other demographics.
National Institute for Occupational Safety and Health: Monthly surveillance data on the prevalence of health-related workplace absenteeism among full-time workers in the United States are available from NIOSH.
U.S. State and local influenza surveillance: Select a jurisdiction below to access the latest local influenza information.
World Health Organization:
Additional influenza surveillance information from participating WHO member nations is available through
FluNet and the Global Epidemiology Reports.
WHO Collaborating Centers for Influenza:
Australia, China, Japan, the United Kingdom, and the United States (CDC in Atlanta, Georgia)
Europe:
The most up-to-date influenza information from Europe is available from WHO/Europe and the European Centre for Disease Prevention and Control.
Public Health Agency of Canada:
The most up-to-date influenza information from Canada is available in Canada’s weekly FluWatch report.
Public Health England:
The most up-to-date influenza information from the United Kingdom is available from Public Health England.
Any links provided to non-Federal organizations are provided solely as a service to our users. These links do not constitute an endorsement of these organizations or their programs by CDC or the Federal Government, and none should be inferred. CDC is not responsible for the content of the individual organization web pages found at these links.
A description of the CDC influenza surveillance system, including methodology and detailed descriptions of each data component is available on the surveillance methods page.