Continue to check our website for further updates on when we will reopen. When the museum reopens, all visitors will need to make reservations at least a week in advance. Walk-in visits are no longer permitted.
Teen Newsletter: Tribal Health
June 2022
The David J. Sencer CDC Museum Public Health Academy Teen Newsletter introduces teens to different public health topics that CDC studies. Each newsletter provides an Introduction, explains CDC’s Work, breaks down the topic using the Public Health Approach, gives you a behind the scenes look at historical items Out of the CDC Museum Collection, and offers a live Teen Talk where teens can learn from CDC experts.
Be sure to join the live Newsletter Teen Talk on June 21, 2022, at 8pm ET.

Currently, there are 574 federally recognized American Indian and Alaska Native (AI/AN) tribes spread across the United States. AI/AN tribes are diverse groups of people with unique cultures, languages, histories, and practices.
Although AI/AN people have many differences, they often share similar experiences with and approaches to maintaining the health and wellness of their communities. For many thousands of years, AI/AN people have practiced the art of medicine and wellness. Therefore, it is no surprise that they have made substantial contributions to public health.

Swinomish Tribe Assesses Climate Change Impact
AI/AN communities have innate strengths and resilience rooted in tribal culture and traditional ways of life. However, AI/AN culture and traditions have been severely disrupted by colonialism, loss of land, and policies (such as assimilation, relocation, and tribal termination) resulting in historical trauma, contributing to higher rates of chronic disease and underlying risk factors.
Did you know that AI/AN people have higher rates of chronic diseases compared to other ethnic groups in the United States? AI/AN people
- Are more likely to be smokers
- Have a greater prevalence of obesity
- Are twice as likely to be diagnosed with diabetes
- Diabetes is the leading cause of kidney failure, a costly condition that requires dialysis or kidney transplantation for survival. Kidney failure from diabetes among Native Americans has historically been the highest of any race. The Indian Health Service (IHS) has been working to address this by using population health and team-based approaches.
- Have unique cancer patterns

Cancer Disparities in the American Indian and Alaska Native Populations
Cancers with higher incidence rates compared to non-Hispanic whites:
- Lung
- Liver
- Stomach
- Kidney
- Colorectal
American Indian and Alaskan Native Incidence Trends
Data from 1999 to 2015 showed significant increases in the following
Average percent per year
- Kidney cancer
- Male: 2.4%
- Female: 1.6%
- Liver cancer
- Male: 3.3%
- Female: 4.2%
- Breast cancer
- Female: 0.9%
Steps to lower cancer incidence rates
- Provide culturally appropriate, community-based interventions to support healthy behaviors
- Decrease exposure to cancer risk factors, such as commercial tobacco and alcohol
- Increase access to preventative health services (vaccines, cancer screening)
https://www.cdc.gov/cancer/research/cancer-in-american-indian-and-alaska-native-people.html
There are multiple centers at CDC that work on tribal health.
- CDC’s Center for State, Tribal, Local, and Territorial Support (CSTLTS) aids 574 federally recognized tribes and works to help develop their public health infrastructure to ensure healthy living.
CSTLTS’s Office of Tribal Affairs and Strategic Alliances (OTASA) works to provide funding towards developing cross-cutting tribal public health infrastructure.
For hundreds of tribes, CSTLTS and OTASA work to:- Coordinate grants and cooperative agreements with tribes and public health organizations
- Improve tribal public health infrastructure through the Tribal Public Health Capacity Building and Quality Improvement Agreement
- Provide surveillance, infection control, and epidemiology support
- Host annual Tribal Advisory Committee meetings with the Agency for Toxic Substances and Disease Registry (ATSDR) to discuss issues and consult with tribal leaders
- Provide COVID-19 preparedness and response resources
- CDC’s National Center for Chronic Disease Prevention and Health Promotion (NCCDPHP) focuses on specific issues such as chronic diseases, diabetes, COVID-19, cancer, smoking, and healthy aging.NCCDPHP’s Division of Population Health (DPH) works to improve the nation’s health by providing state and local data on chronic diseases, risk factors, and outcomes. DPH partners with AI/AN communities to promote health, prevent disease, and strengthen cultural connections to improve health and promote wellness.
As partnerships and programs are built and expanded in Indian Country, DPH also aims to address the social determinants of health that are fundamental to success and sustainability of the work. Visit the sections below to learn how the CDC and tribal communities are working together to achieve these goals.
- Good Health and Wellness in Indian Country (GHWIC)
- Tribal Epidemiology Centers Public Health Infrastructure (TECPHI)
- Tribal Practices for Wellness in Indian Country (TPWIC)
- CDC’s National Center for Emerging and Zoonotic Infectious Diseases (NCEZID) is committed to protecting people from domestic and global health threats.
DPEI’s Arctic Investigations Program (AIP) has collaborated with the Alaska Native Tribal Health Consortium, the State of Alaska, and other partners for more than 45 years to tackle infectious disease threats using state-of-the-art laboratory diagnostics, epidemiology, outbreak investigations, and targeted research. By focusing on reducing and preventing infectious diseases that disproportionately affect AI/AN people, AIP helps everyone living in Alaska enjoy healthier and longer lives.
By the Numbers
- 40% of federally recognized American Indian tribes are located in Alaska
- 20% of rural homes in Alaska lack in-home running water and sanitation
- 90% reduction in vaccine-type invasive pneumococcal disease in Alaska Native children after conjugate vaccines were introduced
- 0 cases of acute hepatitis B infections in western Alaska since 1995 (region previously had highest rate in US)
Furthermore, many tribal people, like Seh Welch and Delight Satter, represent their community’s values and beliefs through their work at CDC. Their contributions while working at CDC help form more direct connections with tribal nations. Learn about their involvement in the video below.
Public health problems are diverse and can include infectious diseases, chronic diseases, emergencies, injuries, environmental health problems, as well as other health threats. Regardless of the topic, we take the same systematic, science-based approach to a public health problem by following four general steps.
For ease of explaining and understanding the public health approach for tribal health, let’s focus on the COVID-19 case investigation and contact tracing program of the Spirit Lake Tribe in North Dakota.
- Surveillance (What is the problem?). In public health, we identify the problem by using surveillance systems to monitor health events and behaviors occurring among a population.
CDC continuously collects data related to COVID-19, including cases among AI/AN persons – one of the racial and ethnic minority groups at highest risk for the disease. CDC found that in 23 selected states, the cumulative incidence of laboratory-confirmed COVID-19 cases among AI/AN was 3.5 times that of non-Hispanic whites.
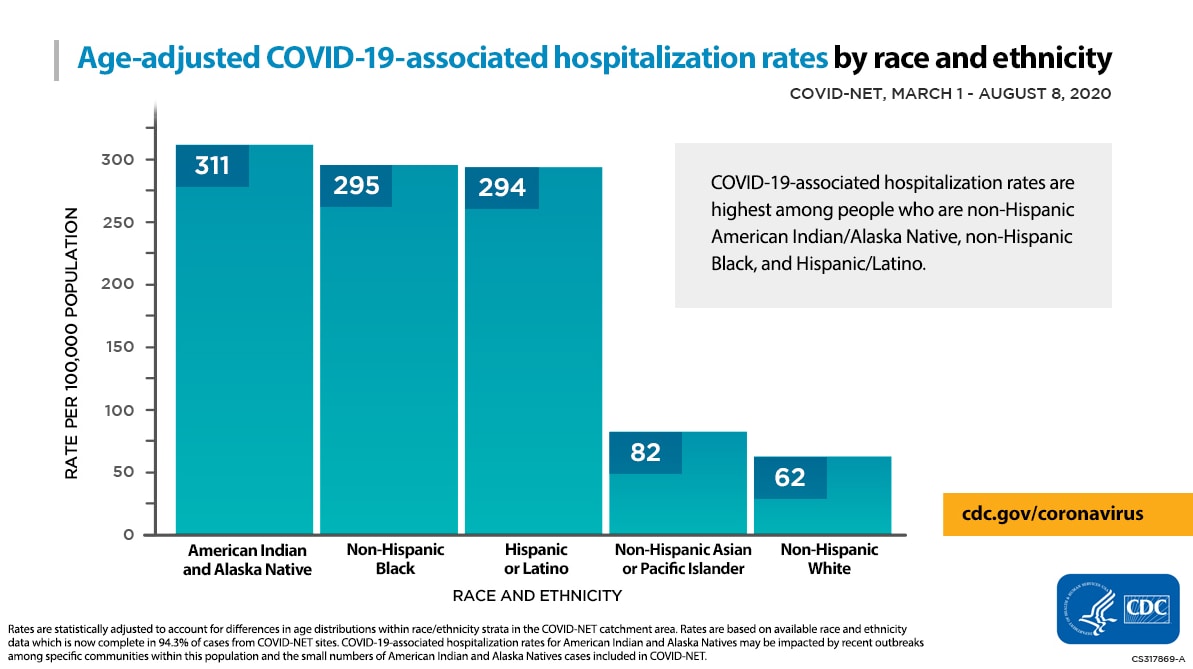
Age-adjusted COVID-19-associated hospitalization rates by race and ethnicity
COVID-NET, March 1-August 8, 2020Rate per 100,000 population
- American Indian and Alaska Native: 311
- Non-Hispanic Black: 295
- Hispanic or Latino: 294
- Non-Hispanic Asian or Pacific Islander: 82
- Non-Hispanic White: 62
COVID-19-assocaited hospitalization rates are highest among people who are non-Hispanic American Indian/Alaska Native, non-Hispanic Black, and Hispanic/Latino.
Rates are statistically adjusted to account for differences in age distributions within race/ethnicity strata in the COVID-NET catchment area. Rates are based on available race and ethnicity data which is now complete in 94.3% of cases from COVID-NET sites. COVID-19-associated hospitalization rates for American Indian and Alaska Natives may be impacted by recent outbreaks among specific communities within this population and the small numbers of American Indian and Alaska Natives cases included in COVID-NET.
In late September 2020, the incidence of confirmed COVID-19 in the Spirit Lake Tribe in North Dakota began increasing rapidly, from approximately 300 new cases per day to approximately 2,260 cases on November 13, 2020.
- Risk Factor Identification (What is the cause?). After we’ve identified the problem, the next question is, “What is the cause of the problem?” For example, are there factors that might make certain populations more susceptible to diseases, such as something in the environment or certain behaviors that people are practicing?
Data from the COVID-19 pandemic has brought social and racial injustice and inequity to the forefront of public health. It has highlighted that health equity is still not a reality as COVID-19 has unequally affected many racial and ethnic minority groups, putting them more at risk of getting sick and dying from COVID-19. The term “racial and ethnic minority groups” includes people of color with a wide variety of backgrounds and experiences. Negative experiences are common to many people within these groups, and some social determinants of health have historically prevented them from having fair opportunities for economic, physical, and emotional health. Social determinants of health are the conditions in the places where people live, learn, work, play, and worship that affect a wide range of health risks and outcomes.Persisting racial inequity and historical trauma have contributed to disparities in health and socioeconomic factors between AI/AN and white populations that have adversely affected tribal communities. The elevated incidence of COVID-19 within this population might also reflect differences in reliance on shared transportation, limited access to running water, household size, and other factors that might facilitate community transmission.On October 20, 2020, the North Dakota Department of Health reported that contact tracing notification efforts were delayed. Because of the delay, COVID-19 patients were asked to notify their own contacts. The Spirit Lake sovereign nation in east central North Dakota is home to approximately 7,500 members of the Spirit Lake Tribe.In addition to contact tracing issues, on-site medical staffing and isolating patients posed major problems for the tribe because shared rooms and living spaces among multigenerational families were common. Another risk factor that made this population more susceptible was homelessness and/or unstable housing during this period. - Intervention Evaluation (What works?). Once we’ve identified the risk factors related to the problem, we ask, “What intervention works to address the problem?” We look at what has worked in the past in addressing this same problem and if a proposed intervention makes sense with our affected population.To address the problem, CDC assisted the Spirit Lake Tribe in building a tribally managed program for comprehensive COVID-19 case investigations, case notification, contact tracing, contact testing, and contact management to ensure timely implementation of these critical epidemic control measures.Through the Spirit Lake Tribe case investigation and contact tracing program, the tribe’s COVID-19 Incident Command System staff members conducted case investigations and contact tracing, provided COVID-19 education, followed up with patients regularly by telephone, and monitored daily symptoms of close contacts.Members of the Spirit Lake community served as contact tracers. Symptom monitoring was facilitated through CDC’s Text Illness Monitoring system (version TIM2), using a free, two-way text-messaging platform to ask enrolled contacts about daily COVID-19 symptoms. The system also alerted Spirit Lake Tribal Health authorities when participants reported symptoms or did not respond.

- Implementation (How did we do it?). In the last step, we ask, “How can we implement the intervention? Given the resources we have and what we know about the affected population, will this work?”
Obtaining information from and maintaining contact with COVID-19 patients and their close contacts was challenging. Using Spirit Lake community members as investigators and contact tracers aided in outreach because of their knowledge of alternate methods to reach patients or contacts (in-home or family contacts) when locating information was incomplete. These community members also helped to improve response rates about COVID-19 exposures because they were trusted by the community and were able to provide culturally appropriate advice about the need to isolate or quarantine.Shared rooms and living spaces among multigenerational families or within whole households with cases or exposures in this community often hindered within-home quarantine and isolation and adherence to these measures. To address this challenge, program staff members distributed critical supplies (e.g., groceries, over-the-counter medications, thermometers, personal protective equipment, and cleaning supplies) and health literacy information (about daily temperature logs, isolation and quarantine procedures, and mask use) to each household.Approximately 100 persons (10%) identified through the case investigation and contact tracing program experienced homelessness or unstable housing during this period, necessitating the provision of temporary shelter and meals at a motel for these persons during isolation and quarantine.
The program required daily, continuous staffing to effect timely COVID-19 mitigation.
Despite the challenges, this tribally managed COVID-19 case investigation and contact tracing program effectively reached Spirit Lake tribal members to provide isolation, quarantine, symptom monitoring, and support services and contributed to timely case and contact management. This program might help guide similar programs in other tribes and the public health community.
Using The Public Health Approach helps public health professionals identify a problem, find out what is causing it, and determine what solutions/interventions work.
This month’s Out of the CDC Museum Collection features past exhibitions related to tribal health.
First is an exhibit of original artwork that was on exhibition at the David J. Sencer CDC Museum in 2006 – Through the Eyes of the Eagle: Illustrating Healthy Living for Children.
The Eagle Books exhibit featured the 65 original watercolors used in diabetes prevention stories for Native American children and all those interested in the road to healthy living. For thousands of years, Native Americans have told stories to pass on their history, knowledge, and culture to future generations. In the Eagle Books, a wise eagle is the tribal elder, who teaches traditional ways of health that children can remember and retell in their homes, schools, and communities.
A national tour of the exhibit began in October 2008 at the National Museum of the American Indian in Washington, DC and at the George Gustav Heye Center in New York, both Smithsonian Institution Museums. From 2009-14, the exhibition was displayed from coast to coast at 15 venues in 10 states. The final stop was Chickasaw Cultural Center in Sulphur, OK.


The Eagle Books were developed in response to the burden of diabetes among Native Americans and the lack of diabetes prevention materials for Native American children. CDC, the Indian Health Service, and the Tribal Leaders Diabetes Committee worked together to create this series. It is widely distributed in Native communities across the United States. There are four books for K–4 readers, plus three chapter books and a graphic novel for readers in grades 5–8. All books and activities can be ordered or downloaded for free.
The next two exhibitions were displayed together at the David J. Sencer CDC Museum from September 21, 2019 – May 1, 2020.













