Continue to check our website for further updates on when we will reopen. When the museum reopens, all visitors will need to make reservations at least a week in advance. Walk-in visits are no longer permitted.
Teen Newsletter: January 2021 – HPV
The David J. Sencer CDC Museum (CDCM) Public Health Academy Teen Newsletter was created to introduce teens to public health topics. Each month will focus on a different public health topic that CDC studies. Newsletter sections: Introduction, CDC’s Work, The Public Health Approach, Special Feature, Out of the CDC Museum Collection, and Activities.
Be sure to join our live Newsletter Zoom on January 26, 2021, at 8pm, and check out all the activities (digital scavenger hunt—Goosechase, Zoom, social media challenge, and Ask a CDCer) at the end of each newsletter. Join in on the fun and win some prizes! Also, be on the lookout for the recently added activity, a pre-Zoom game (Kahoot) that will be emailed the day of the Zoom.
We are excited to announce a new newsletter activity prize category: Future CDCer, learn more below.
Human papillomavirus (HPV) is the most common sexually transmitted infection in the United States. HPV is so common that nearly all sexually active males and females get the virus at some point in their lives. Nearly 80 million Americans, most in their late teens and early 20s, are infected with HPV.
HPV is spread through intimate skin-to-skin contact. You can get HPV by having vaginal, anal, or oral sex with someone who has the virus.
There are many different types of HPV; approximately 200 types of HPV have been identified. Some types can cause health problems including genital warts and cancers. HPV types are often referred to as “non-oncogenic” (wart-causing) or “oncogenic” (cancer-causing).
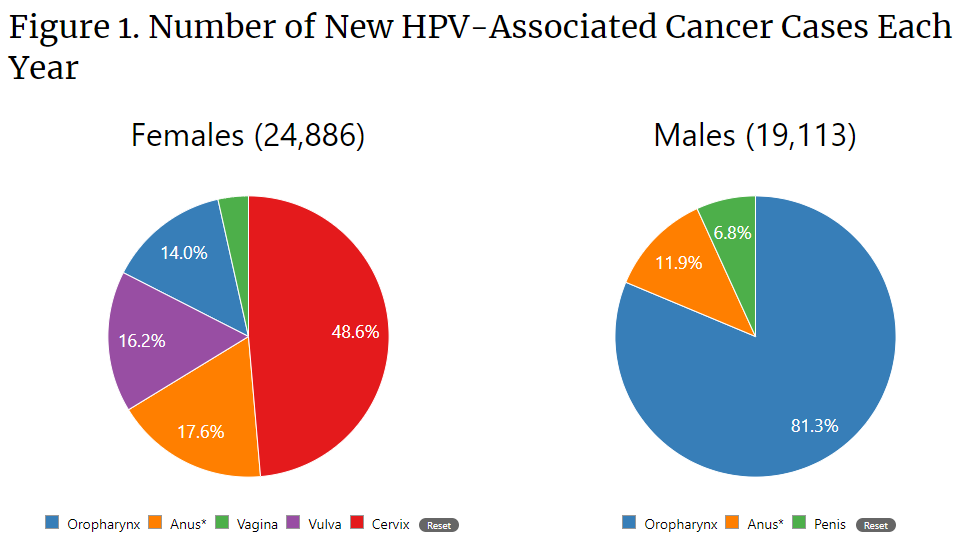
Although most HPV infections are asymptomatic and resolve on their own, HPV can cause cervical and other cancers including cancer of the vulva, vagina, penis, or anus. It can also cause cancer in the back of the throat, including the base of the tongue and tonsils (called oropharyngeal cancer). Every year in the United States, HPV is estimated to cause nearly 44,000 cases of cancer in males and females.
As you can see, HPV and related cancers do not only affect women. More than 4 out of every 10 cases of cancer caused by HPV occur among men.
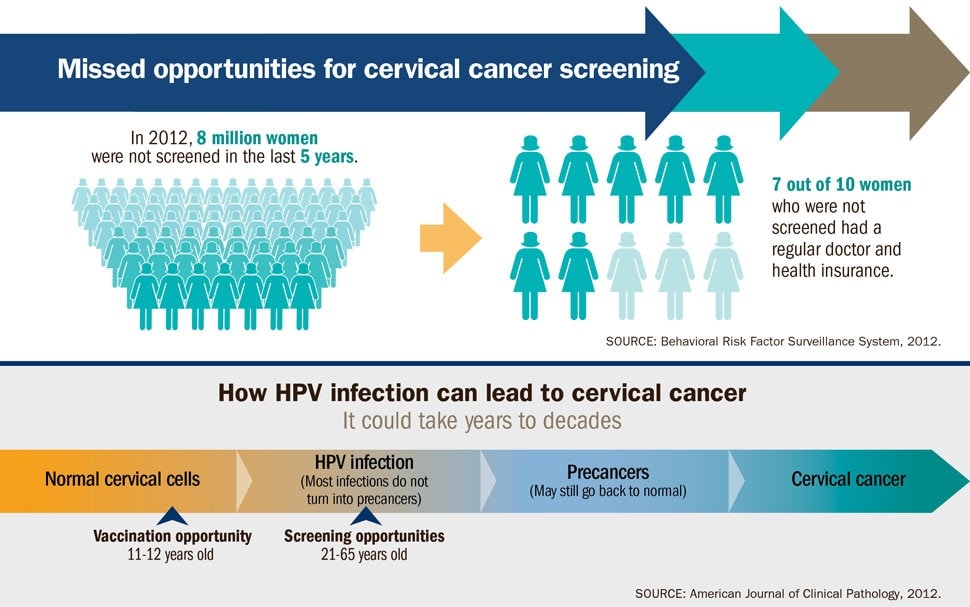
The good news is there is a vaccine! Vaccines protect you before you are exposed to an infection. That’s why the HPV vaccine is recommended earlier rather than later: to protect you long before you are ever exposed to the virus. Two doses of HPV vaccine are recommended at ages 11–12 (the vaccine can be given starting at age 9 years). If you have not gotten your HPV vaccine yet, talk to your doctor because the HPV vaccine is also recommended for everyone through age 26 years (if they were not adequately vaccinated already).
January is Cervical Cancer Awareness Month, a great time to talk about how HPV vaccines can help prevent cancer. This newsletter will focus on HPV, the vaccine for HPV, and cervical cancer caused by HPV.
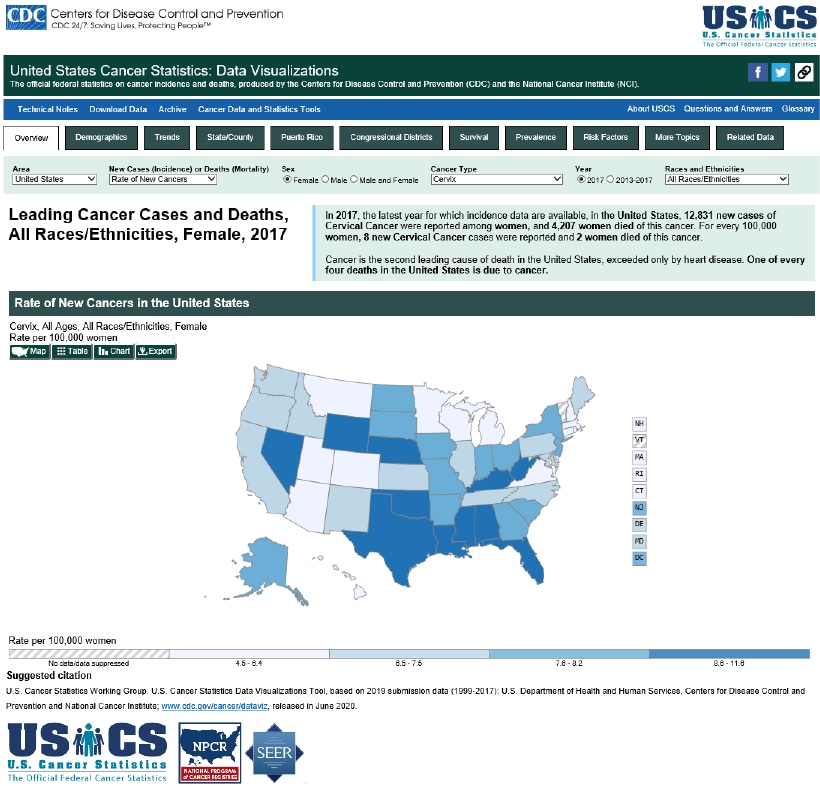
Every year, nearly 12,000 females living in the U.S. will be diagnosed with cervical cancer, and more than 4,000 females die from cervical cancer—even with screening and treatment.
Cervical cancer is the fourth most common cancer in females worldwide, with more than 500,000 new cases estimated each year.
HPV infects epithelial tissue, the tissue that covers organs. Most people who become infected with HPV do not know they have it, and the body’s immune system gets rid of the HPV infection naturally within a year or two—even oncogenic types. However, when the body’s immune system cannot get rid of an infection with oncogenic HPV types, it can linger over time and turn normal cells into abnormal cells and then cancer.
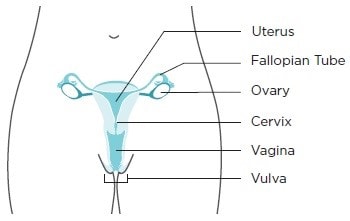
Cancer is always named for the part of the body where it starts, even if it spreads to other body parts later. When cancer starts in the cervix, it is called cervical cancer. The cervix connects the vagina (birth canal) to the upper part of the uterus. The uterus (or womb) is where a baby grows when a female is pregnant.
Among the cancer-related outcomes of HPV infection, invasive cervical cancer has been considered the most important worldwide, with about 570,000 new cases and over 300,000 attributable deaths in 2018. Cervical cancer occurs most often in females over age 30.
Infection with a high-risk HPV type is considered necessary for the development of cervical cancer but, by itself, is not sufficient to cause cancer. Most females with HPV infection, even those with high-risk HPV types, do not develop cancer.
Screening tests and the HPV vaccine can help prevent cervical cancer. When cervical cancer is found early, it is highly treatable and associated with long survival and good quality of life.
At CDC, three different centers work together on HPV and cervical cancer:
- National Center for HIV, Viral Hepatitis, STD, and TB Prevention (NCHHSTP)
- National Center for Immunization and Respiratory Diseases (NCIRD)
- National Center for Chronic Disease Prevention and Health Promotion (NCCDPHP)
Under NCHHSTP, the Division of STD Prevention (DSTDP), provides national leadership, research, policy development, and scientific information to help people live safer, healthier lives by the prevention of STDs (i.e., HPV) and their complications (i.e., cervical cancer).
Under NCIRD, the Immunization Services Division (ISD), protects individuals and communities from vaccine-preventable diseases (i.e., HPV) through provision of federal funds and contracts to purchase vaccine, the provision of technical and financial support of immunization programs, provider and public education, and evaluation and research. There is also the Division of Viral Diseases (DVD), that prevents disease, disability, and death from viral diseases (i.e., HPV) through immunization and other prevention measures.
Under NCCDPHP, the Division of Cancer Prevention and Control (DCPC), works to reduce cancer (i.e., cervical cancer) risk factors and promote cancer screenings, especially for groups affected by disparities, which are differences in health across different geographic, racial, ethnic, and socioeconomic groups. DCPC works to:
Public health problems are diverse and can include infectious diseases, chronic diseases, emergencies, injuries, environmental health problems, as well as other health threats. Regardless of the topic, we take the same systematic, science-based approach to a public health problem by following four general steps.
1. Surveillance (What is the problem?)
In public health, we identify the problem by using surveillance systems to monitor health events and behaviors occurring among a population.
HPV infections are not nationally notifiable. This is because (1) most sexually active individuals will acquire at least 1 type of HPV infection at some point in their lives and infections usually clear or become undetectable, and (2) most infections will not have any associated clinical disease. However, special studies to monitor HPV infection and HPV-associated diseases (i.e., genital warts and cancers) can help determine the impact of HPV vaccine programs. Existing and new systems are in place to monitor coverage and impact of HPV vaccine outcomes in the United States.
Surveillance data on HPV-associated cancers, including cervical cancer, are collected in two population-based central cancer registries in the United States:
- CDC’s National Program of Cancer Registries (NPCR)
- Surveillance Epidemiology and End Results (SEER) program
NPCR and SEE together collect data on cancers diagnosed in 100% of the US population.
Up-to-date incidence and mortality statistics on HPV-associated cancers can be visualized through a web-based tool – United States Cancer Statistics: Data Visualizations
The National Health and Examination Survey (NHANES) is also used to monitor the impact of vaccination on HPV prevalence (i.e., type-specific HPV prevalence in genital and oral specimens in males and females, cervical lesions among females undergoing cervical cancer screening).
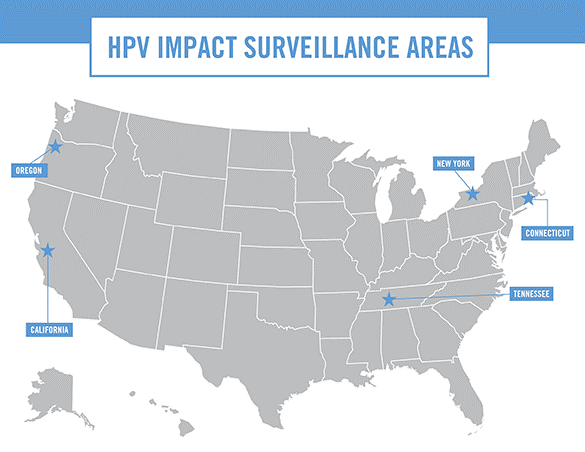
Another program, the Human Papillomavirus (HPV) Vaccine Impact Monitoring Project (HPV-IMPACT), monitors rates of high-grade cervical lesions (CIN2+) in females in the United States. Scientists use data from the project to determine the impact of the U.S. HPV vaccination program on cervical precancers caused by HPV. HPV-IMPACT includes defined areas in five states covering 1.5 million women.
For ease of explaining and understanding the public health approach for this public health problem (HPV and cervical cancer) let’s focus on cervical cancer as the problem for step 1.
2. Risk Factor Identification (What is the cause?)
After we’ve identified the problem, the next question is, “What is the cause of the problem?” For example, are there factors that might make certain populations more susceptible to disease, such as something in the environment or certain behaviors that people are practicing?
More than 9 of every 10 cases of cervical cancer are caused by HPV. Long-lasting infection with certain types of HPV is the main cause of cervical cancer. High-risk HPV types (including types 16, 18, and others) act as carcinogens in the development of cervical cancer and other anogenital cancers. High-risk HPV types are detected in 99% of cervical precancers.
Type 16 is the cause of approximately 50% of cervical cancers worldwide, and types 16 and 18 together account for about 66% of cervical cancers. An additional five high-risk types, 31, 33, 45, 52, and 58, are responsible for another 15% of cervical cancers.
About 10% of females with HPV infection on their cervix will develop long-lasting HPV infections that put them at risk for cervical cancer.
A small proportion of infected persons become persistently infected; persistent infection is the most important risk factor for the development of cervical cancer. In females, squamous intraepithelial lesions (SIL) of the cervix can be detected through screening. High-grade squamous intraepithelial lesions (HSIL) are considered cancer precursors. If left undetected and untreated, such cancer precursors can progress to cervical cancer years or decades later.
A female is at increased risk of HPV-induced cervical cancer if she has HIV (the virus that causes AIDS, learn more about HIV/AIDS from the December 2020 Teen Newsletter) or another condition that makes it hard for the body to fight off health problems. Smoking, using birth control pills for a long time (five or more years), having given birth to three or more children, or having several sexual partners are other risk factors.
3. Intervention Evaluation (What works?)
Once we’ve identified the risk factors related to the problem, we ask, “What intervention works to address the problem?” We look at what has worked in the past in addressing this same problem and if a proposed intervention makes sense with our affected population.
Screening tests and the HPV vaccine can help prevent cervical cancer.
Two screening tests can help prevent cervical cancer or find it early—
- The Papanicolaou (Pap) test looks for precancers, cell changes on the cervix that might become cervical cancer if they are not treated appropriately (females should start getting Pap tests at age 21)
- The HPV test looks for the virus (human papillomavirus) that can cause these cell changes.
The HPV vaccine is cancer prevention. HPV is estimated to cause nearly 36,000 cases of cancer in men and women every year in the United States. HPV vaccination can prevent more than 32,000 of these cancers from ever developing by preventing the infections that cause those cancers.
HPV vaccination works. HPV infections, genital warts, and cervical precancers (abnormal cells on the cervix that can lead to cancer) have dropped significantly since the vaccine has been in use in the United States.
- Among teen girls, infections with HPV types that cause most HPV cancers and genital warts have dropped 86 percent.
- Among young adult females, infections with HPV types that cause most HPV cancers and genital warts have dropped 71 percent.
- Among vaccinated females, the percentage of cervical precancers caused by the HPV types most often linked to cervical cancer has dropped by 40 percent.
Over 12 years of monitoring and research have shown that HPV vaccination is very safe. Each HPV vaccine—Gardasil® 9, Gardasil®, and Cervarix®—went through years of extensive safety testing before they were licensed by the U.S. Food and Drug Administration (FDA). Each vaccine was found to be safe and effective in clinical trials.
Currently, Gardasil® 9 (human papillomavirus 9-valent vaccine, recombinant; 9vHPV) is the only HPV vaccine available for use in the U.S. The safety of Gardasil 9 was studied in clinical trials with more than 15,000 participants before it was licensed and continues to be monitored. Gardasil 9 protects against 9 types of HPV (6, 11, 16, 18, 31, 33, 45, 52, and 58). HPV types 16 and 18 cause most cervical and other cancers attributable to HPV. HPV types 6 and 11 cause anogenital warts.
During 2012–2016, an average of 43,999 HPV-associated cancers (12.2 per 100,000 persons) were reported annually, and an estimated 79% (34,800) of these cancers were attributable to HPV. Of these cancers, an estimated 32,100 (92%) were attributable to the types targeted by the HPV vaccine – 9vHPV (Gardasil® 9). Cervical cancer screening and HPV vaccination can prevent many of these cancers.
One of the largest problems in reducing cervical cancer is that many do not receive the HPV vaccine or are not screened for cervical cancer.
A catch-up HPV vaccination is now recommended for all persons through age 26 years.
4. Implementation (How did we do it?)
In the last step, we ask, “How can we implement the intervention? Given the resources we have and what we know about the affected population, will this work?”
With over 120 million doses distributed in the United States, HPV vaccine has a reassuring safety record that’s backed by more than 12 years of monitoring and research to show its efficacy.
Under the Affordable Care Act (ACA), the Gardasil® 9 vaccine should be provided without cost for everyone in the recommended age groups by all covered private health insurance plans and the insurance obtained through the health exchanges as of 2017.
What if you don’t have health insurance or can’t afford the HPV vaccine?
The Vaccines for Children (VFC) program helps families of eligible children who might not otherwise have access to vaccines. The program provides vaccines at no cost to children ages 18 years and younger who are uninsured, Medicaid-eligible, or American Indian/Alaska Native. To learn more, see VFC program.
Merck, the manufacturer of the vaccine, also has a patient assistance program and offers the vaccine at no cost for adults of ages 19 to 26 who do not have health insurance and cannot afford to pay for the vaccine.
What about screening? CDC recommends:
- If you are 21 to 29 years old: You should start getting Pap tests at age 21. If your Pap test result is normal, your doctor may tell you that you can wait three years until your next Pap test.
- If you are 30 to 65 years old: Talk to your doctor about which testing option is right for you—
- A Pap test only. If your result is normal, your doctor may tell you that you can wait three years until your next Pap test.
- An HPV test only. This is called primary HPV testing. If your result is normal, your doctor may tell you that you can wait five years until your next screening test.
- An HPV test along with the Pap test. This is called co-testing. If both of your results are normal, your doctor may tell you that you can wait five years until your next screening test.
- If you are older than 65: Your doctor may tell you that you don’t need to be screened anymore if—
- You have had normal screening test results for several years, or
- You have had your cervix removed as part of a total hysterectomy for non-cancerous conditions, like fibroids.
To improve accessibility for screening, the CDC National Breast and Cervical Cancer Early Detection Program (NBCCEDP) provides low-income, uninsured, and underserved females access to timely cervical cancer screening and diagnostic services. Currently, the NBCCEDP funds 70 awardees: all 50 states, the District of Columbia, 6 U.S. territories, and 13 tribal organizations. Since 1991, NBCCEDP-funded programs have provided more than 15 million cervical cancer screening tests to nearly 6 million females.
As you can see, using The Public Health Approach helps public health professionals identify a problem, find out what is causing it, and determine what solutions/interventions work.
The CDC Inside Knowledge campaign raises awareness of the five main types of gynecologic cancer, including cervical cancer. It encourages females to pay attention to their bodies, so they can recognize any warning signs and seek medical care.
Campaign resources include television, radio, and print public service announcements (PSAs). Click for resources (videos, podcasts, shareable graphics, fact sheets, and posters ) specific to cervical cancer.
Below is a short (30 sec) video of a cervical cancer survivor sharing her personal experience that makes her dedicated to protecting her own children from HPV-related cancers.
Recognize the female in the poster below? It’s Cote De Pablo! She is an actress best known for her role in the show NCIS (Fun fact: Heather & Trudi both like the show. Not sure who Heather and Trudi are? Join the live Zoom on 01/26/2021 at 8pm EST).
CDC works 24/7 to provide information that helps protect the health of individuals and communities. One way to get the information to the public is through posters. Posters are some of the most used formats for communicating information in public health. Posters can increase knowledge, change attitudes and alter behaviors. Many public health campaigns use posters (i.e., the CDC Inside Knowledge campaign has the “I was lucky” poster with Cote De Pablo, above).
Below is a poster we have in the CDC Museum Collection that CDC created to provide information about the prevalence of HPV and health problems associated with HPV. To the right is a digital version of that poster in Spanish.

Another way the CDC gets information out is through guidelines/guidebooks for healthcare providers. Below are a couple of pages from the 2007 HPV guidebook for clinicians.

Click here to see current HPV information for healthcare providers.
You might be thinking that the items above don’t look that old. That is because the HPV vaccine is a newer vaccine. If you recall from the public health approach section above, the HPV vaccine has only been in use for 12 years. Items in the CDC Museum Collection do not have to be old to be a part of public health history. In fact, collecting history is an on-going effort. The CDC Museum is currently collecting for the COVID-19 collection.
You might have noticed that more recently, posters and other previously printed materials have been used digitally on websites and social media. Complete the social media challenge below, where you can help promote the HPV vaccine by posting a digital CDC poster on your social media.
All January 2021 Teen Newsletter winners will be announced 01/26/21 during the Zoom – see individual deadlines below, as applicable.
**NEW** The CDC Museum Public Health Academy Teen Newsletter is excited to announce a new newsletter activity prize category: Future CDCer
To qualify for Future CDCer, you must participate in all newsletter activities (scavenger hunt—Goosechase, Zoom, social media challenge, Ask a CDCer, and pre-Zoom game—Kahoot). All that qualify will be entered into a prize drawing for a CDC Museum Public Health Academy t-shirt.
*The following newsletter activities: Scavenger Hunt, Zoom, and Social Media Challenge are available for your participation anytime – even after deadlines. To be eligible for prizes you must complete activities by the deadline.
Want to do a fun digital scavenger hunt?
Time: ~20 min to complete
Complete all missions by 01/25/21 11pm EST, for prize drawing.
See below for more details.
Want to learn more from CDCers who work on HPV?
Join us for an exclusive Zoom on 01/26/21 at 8pm EST.
Advance registration required. All who register by or on 01/25/21 11pm will be entered into a prize drawing.
Watch the human papillomavirus (HPV) Teen Talk.
Help CDC promote HPV vaccination!
Pick your favorite HPV vaccine poster and post it on your social media using #CDCTeenNewsletter
Submit a screenshot of your post by 01/25/21 11pm EST to be entered into a prize drawing.
Do you have a question for a CDCer who works on HPV?
Submit your question for the HPV experts who will be joining the Zoom on 01/26/21 at 8pm EST.
If your question is selected, you will get a shout out on the live Zoom and a prize.
Please do not submit questions that are answered by reading this newsletter.
Submit your question(s)external icon by 01/25/21 11pm EST.
CDCM PHA Teen Newsletter Scavenger Hunt
January 2021
Step 1: Download the GooseChase iOS or Android app
Step 2: Choose to play as a guest
Step 3: Enter game code – 5DQKZW
Step 4: Enter password – CDC
Step 5: Enter your email as your player name (this is how we will contact you if you are the prize winner)
Step 6: Go to Sexually Transmitted Infections (STIs) to complete your missions
Tips for Winning:
- All answers are found on the website, see Step 6.
- Open-ended answers and photo submissions are evaluated for accuracy.
- Complete all the missions by 01/25/21 11pm EST, to be entered into a drawing for a prize.
- Make sure to make your player name is your email.
Have fun!