Cluster Investigation and Response
Health departments should investigate and respond to prioritized clusters to prevent ongoing rapid HIV transmission. Investigation involves gathering additional information to understand affected people’s needs. Effective response measures should be tailored to address these needs.
Because clusters are part of larger networks and result from gaps in prevention and care, health departments should implement response activities at individual, network, and systems levels.
Role of CDR LCG in review, prioritization, investigation, and response
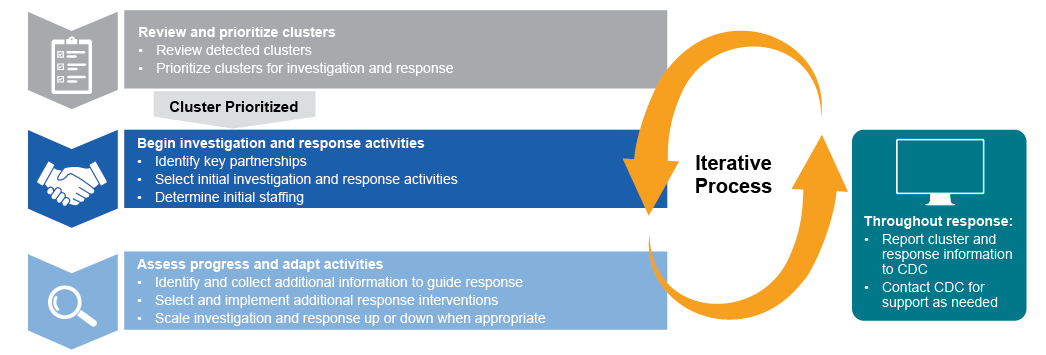
Begin investigation and response
Once the CDR LCG has reviewed and prioritized clusters, they should begin investigation and response activities. They should guide the following steps, which may be done at the same time:
- Review available information. Revisit data sources to learn how transmission may be occurring, and which communities may be affected.
- Identify partners for response. Work with affected community members, providers, community-based organizations, local health departments, and local planning groups on response activities.
- Share cluster-level information with partners. Summary information will help partners better understand what services are currently available and where gaps are occurring.
- Select and implement response strategies. Tailor strategies at individual, network, and systems levels to improve response effectiveness.
Three initial activities health departments can tailor or expand while developing more specific cluster response activities:
- Provide linkage or relinkage to care for people in the cluster.
- Link network members identified through partner services to HIV testing, PrEP/PEP, syringe programs, sexual health, or other appropriate services.
- Develop and share tailored and non-stigmatizing communications with the affected community, providers, and community-based organizations (link to Communications section).
- Set specific goals for each cluster. Health departments should set specific, measurable targets to guide response and future scaling up or down of response activities. For example:
- Linking a specific number of people to care
- Testing a certain percentage of the known network
- Increasing the number of pre-exposure prophylaxis/post-exposure prophylaxis (PrEP/PEP) providers
- Discuss staffing and funding needs. Consult your CDR plan to fill necessary roles for investigation and response activities. In addition, determine the need for specific skills or expertise (for example, language skills or knowledge of specific populations).
- Report the cluster. Report cluster investigation and response activities to CDC through regular submission of CRFs.
Considerations for multijurisdictional clusters
A multijurisdictional cluster includes people in more than one state, local, or territorial health department jurisdiction. The primary jurisdiction, where the most cases in a cluster are located, will generally take the lead once a cluster is detected. However, all jurisdictions involved should be included in ongoing efforts to address a cluster. Where multijurisdictional response is required, health departments may need to develop a plan for secure data sharing with one another. CDC may be able to help with coordination of multijurisdictional cluster response.
Assess progress and adapt response
The CDR LCG should meet regularly to:
- Assess progress toward goals for cluster response.
- Identify what additional information is needed and how to gather that information.
- Build upon response efforts by selecting and tailoring additional response strategies at individual, network, and systems levels.
Collect additional information
The CDR LCG should consider what additional information they need to guide response activities. This may include exploring social factors (for example, drug use patterns) or structural factors (for example, access to drug treatment). Activities to collect this information can include:
- Examining clinical data.
- Holding focus groups with community partners.
- Conducting expanded partner services interviews or provider surveys.
- Implementing expanded partner services or social network strategies to identify more network members and assess their needs.
- Reviewing existing policies to identify areas for improvement.
- Assessing access to HIV prevention, care, and essential support services for affected populations through phone calls or web searches.
Additional response activities
The CDR LCG should select response activities at individual, network, and systems levels tailored to the cluster.
Systems-level changes are particularly important, and often require significant investment because they have broad impact and lead to lasting change.
Many of these activities affect more than one level. For example, a systems-level policy change should improve services to a network and for individual cluster members.
Partnerships and collaboration with community members, providers, and local organizations are essential for activities to succeed.
Examples of response activities and level of impact
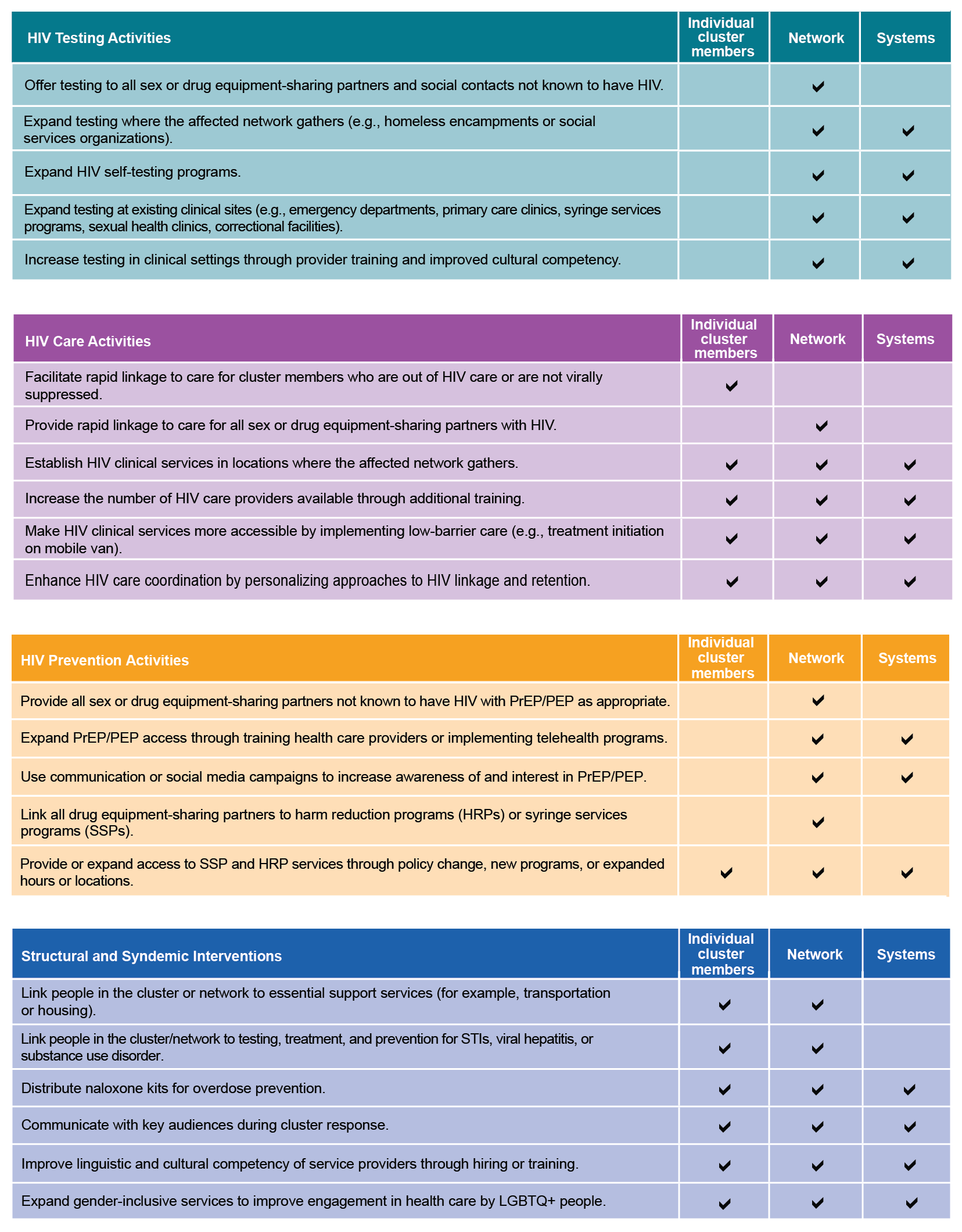
The HIV CDR Science Brief provides detailed examples of the above activities in past cluster responses.
Scaling up investigation and response
Different aspects of cluster investigation and response can be scaled up depending on the needs of the affected network.
Assess needs. Reasons why a health department may scale up response activities:
- The cluster meets pre-determined criteria (for example, high number of recent diagnoses or recent transmission among a specific population).
- Response activities exceed the capacity of staff initially assigned to support the response.
Determine activities to increase response capacity. Some examples include:
Activating surge staff or partnerships (for example, adding a public information officer for communications support).
- Increasing community collaboration and partnerships.
- Identifying supplemental funding or redirecting existing funds.
- Activating an Incident Management or Incident Command System within the HIV program, agency, or state-wide.
Communicate with staff and community partners during scaled up response. CDR staff should provide regular updates to local and state leadership, response staff, community partners, and CDC and other federal agencies. These staff and partners can also provide feedback on escalated response activities.
Scaling down or ending response
When cluster data indicate significant progress toward goals, consider scaling down some or all response activities.
Factors to consider:
- Evidence that transmission has declined, and HIV prevention and care have improved. This can include:
- A reduced number of new diagnoses over time, particularly in the setting of strong HIV testing coverage.
- High rates of people being in care and virally suppressed.
- A large percentage of people in the network have received partner services interviews. Reported contacts have been tested and referred to services as needed.
- Cluster no longer meets priority criteria.
- Community partners express support for scaling down response activities.
Activities when scaling down or ending a response should include:
- Determining a threshold for again scaling up the response.
- Planning for key response activities that should continue as routine practice.
- Communicating to partners that the scale down is occurring and discussing which activities should be ongoing.
Report response activities to CDC. CDR activities should be reported to CDC. CDC Detection and Response Branch epidemiologists can also provide advice and support for investigation and response activities.
Evaluate response activities
Consider evaluation during and after response to gather lessons learned and opportunities for improving future responses. Evaluation can show whether the response addressed prevention and treatment gaps. Metrics to examine can include:
- New HIV diagnoses identified mainly through active investigation and intervention activities, such as partner services and testing.
- Implementation or expansion of additional services.
- Effective policy changes that address barriers and strengthen services for affected communities.
Monitor cluster after response ends. After investigation and response activities have ended, continue to monitor for any changes. New cluster growth might indicate a need to reopen a cluster response.
Contact CDC for support
CDC may be able to assist health departments with the planning and implementation of investigation and response activities. Health departments should reach out to their assigned CDC Detection and Response Branch epidemiologist to discuss their needs and interests.