CDR Community Spotlights: Lawrence and Lowell, Massachusetts

In late summer 2016, Amy Bositis, director of clinical programs at the Greater Lawrence Family Health Clinic in Lawrence, Massachusetts, picked up her phone to learn that an acute HIV infection had just been diagnosed in a clinic client. “We provide comprehensive HIV services to our clients, but I had never been called in real time about a patient with a recent diagnosis, because it was relatively rare in Lawrence,” says Bositis. “I had definitely never experienced an acute infection1 being diagnosed among any of our patients.”
A few days later, processing a routine report, Bositis realized that two other clients had also recently received HIV diagnoses. Soon, the total of new HIV diagnoses at the clinic grew to five – all linked to use of injection drugs, a route of HIV transmission that over the years had become increasingly rare in Lawrence and nationwide.
Bositis quickly reported this unusual increase in new diagnoses to state health officials, including Dawn Fukuda, director of the Office of HIV/AIDS for the Massachusetts Department of Public Health (MDPH).
“We could tell that something urgent was happening,” says Fukuda. “Just before Amy called, I heard that HIV had been diagnosed at the county jail among six people who inject drugs. Altogether, it added up to a third of the total HIV diagnoses linked to use of injection drugs we normally see in a year statewide – but this was in one county, in one month.”
Beginning with these initial small groups of people with newly diagnosed HIV, investigators from the state health department, with support from CDC, launched a painstaking, months-long investigation to understand the true scope of the outbreak. The investigation included epidemiologic analysis of HIV data including viral sequences, and interviews with people who inject drugs.
The results were stunning: the investigation ultimately uncovered a network of interconnected clusters spanning 184 people with HIV – many of whom received a diagnosis during the course of the investigation itself. Most people affected by this large outbreak were in Lawrence and in nearby Lowell, though the networks extended across the state and even beyond state lines into neighboring New Hampshire.
“HIV is certainly not new to Lawrence, and we thought we had a pretty good idea of what works for prevention,” says Bositis. “We have a fantastic team that provides comprehensive HIV prevention and treatment services here at the clinic. But this outbreak made very real to us that HIV risks are evolving, and we needed to do even more to keep pace.”
The investigation revealed that many individuals in this network were experiencing homelessness or unstable housing. And nearly all had injected drugs – often fentanyl, which had been introduced into the area’s drug supply sometime in 2014. Fentanyl can increase risk for HIV transmission, in part because its effects wear off relatively quickly, inducing users to inject more frequently.
Because HIV was being transmitted primarily among people who inject drugs, MDPH began gathering information and insights on the outbreak from a variety of local sources, including clinics, hospitals, and boards of health as well as broader community sources like jails, advocates for people experiencing homelessness, local politicians, and first responders.
“We’ve always consulted with local communities, but this outbreak drove us to engage even more deeply with a wider range of stakeholders,” says Fukuda. “There was a real urgency to make sure we understood what was happening and could tailor our response accordingly, with support from across the community.”
Together, these stakeholders created profound policy and program changes. The Greater Lawrence Family Health Clinic, for example, completely reorganized the way it provides services in response to what they learned through the cluster investigation. While specialized medical needs and funding streams had typically encouraged the separation of services for HIV, substance use, tuberculosis, hepatitis C, and other health concerns, the clinic shifted to an integrated approach where all of these health issues are addressed together by a small team. Often this team works outside the clinic, bringing services directly to the people who need support most, including people living in homeless encampments.

While responding to an HIV cluster, a local health clinic was able to integrate its services to address HIV and syndemic health issues, such as substance use and hepatitis C. This enables clients to receive more comprehensive care and allows healthcare providers to have a more complete picture of each client’s health needs.
Within the encampments, law enforcement and other first responders learned as a result of the cluster investigation to adopt a public health approach to people who inject drugs or experience overdoses – referring them to medication assisted treatment for opioid use disorder, rather than taking them to jails for acute detox as they had often done previously. Similarly, homeless shelters began to relax policies against substance use that previously led staff to confiscate needles and syringes, which often caused people who inject drugs to remain on the street rather than using the shelters. Now, in some cases health workers are invited into the shelters to share prevention information, counsel clients, and conduct HIV tests.
The effects of the Lawrence and Lowell investigations rippled statewide. Massachusetts moved quickly to fill the gaps in services identified in the course of the investigation, investing an additional $1.7 million in state funding for HIV prevention. These funds have been used to provide a wide range of services, including expanding testing for HIV and hepatitis C, linking people receiving HIV diagnoses in hospital emergency departments to care, and even providing medication storage for people experiencing homelessness who might need a safe place to keep their HIV medication.
Detection of the outbreak also lent urgency to take advantage of a 2016 change in state law shifting the authority to approve syringe services programs (SSPs) from elected officials to local boards of health. SSPs typically provide comprehensive services, including sterile needles and syringes, Narcan to prevent fatal drug overdoses, and referrals to substance use disorder treatment. In part because of the outbreak, Lawrence, Lowell, and other local boards of health approved these programs, and the number of publicly supported SSPs in Massachusetts grew from just 5 in 2016 to 33 by 2019.
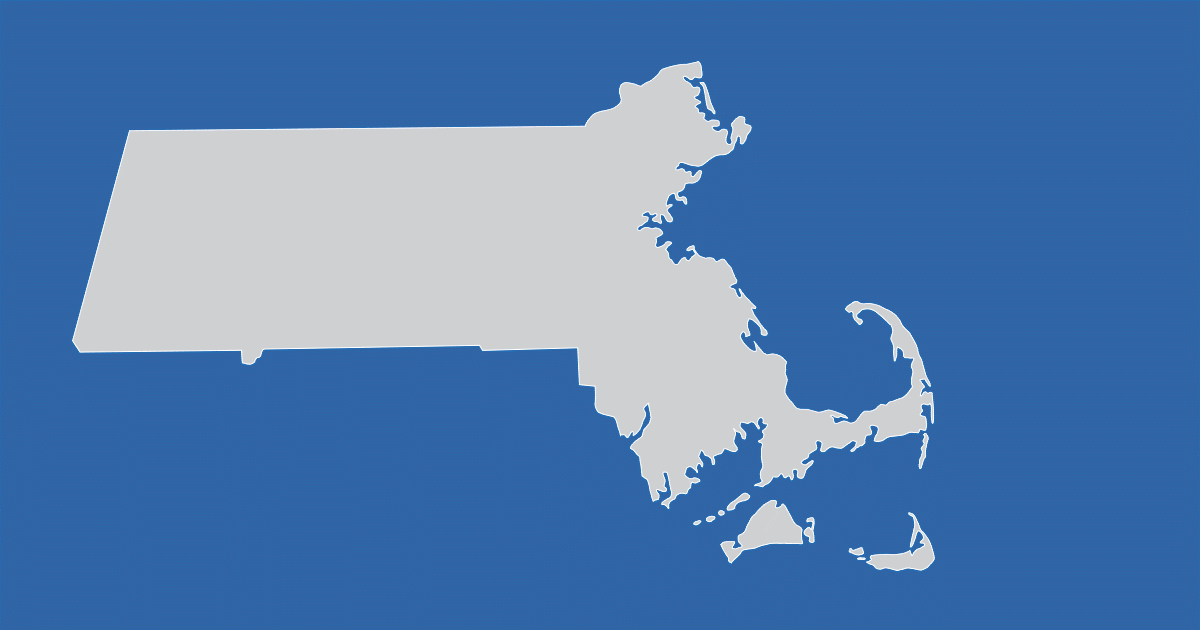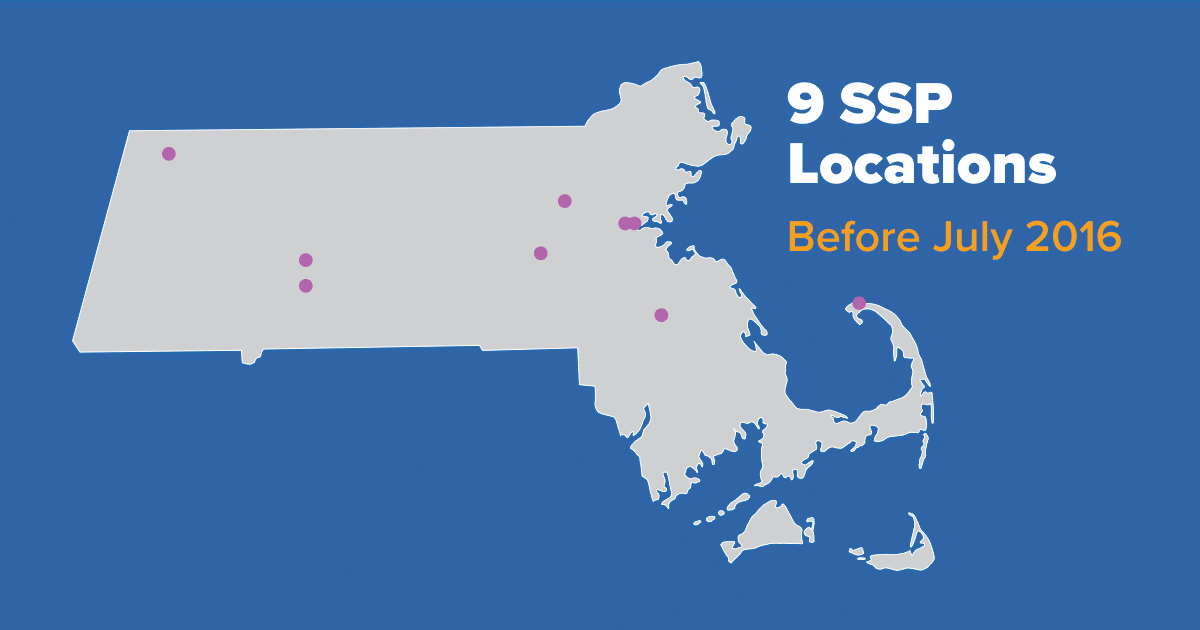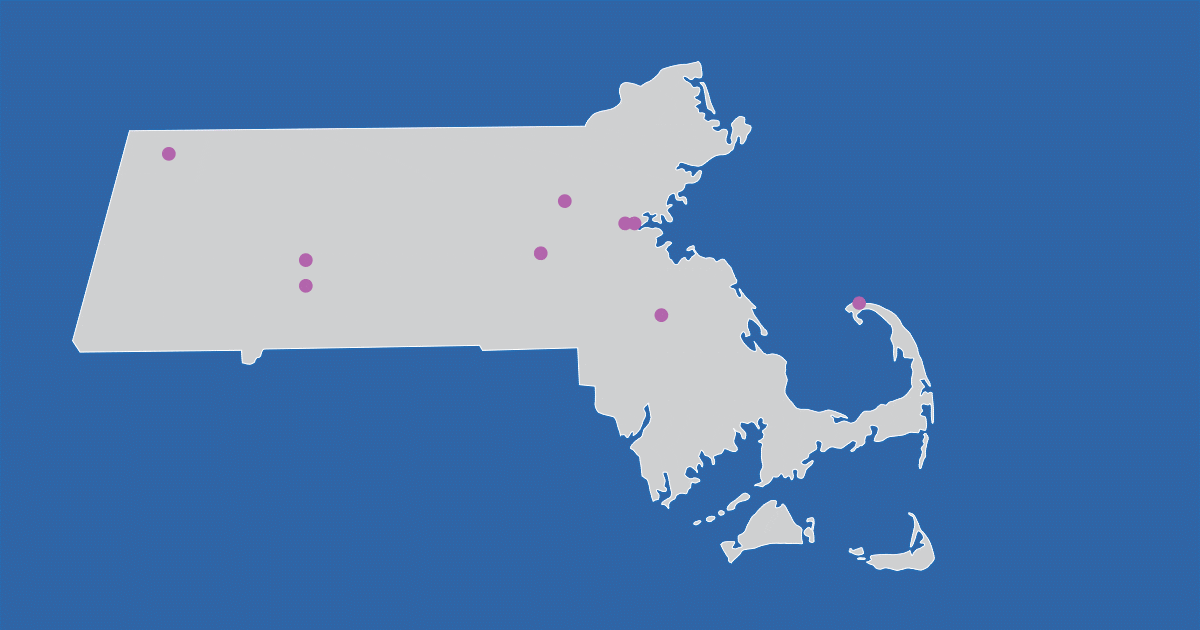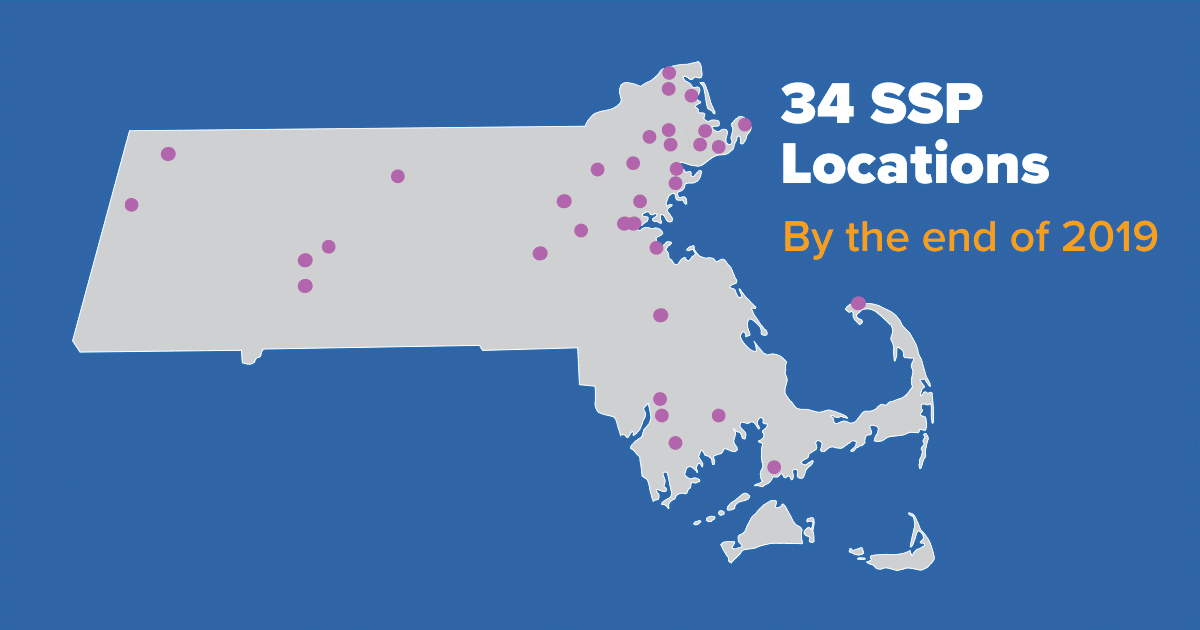
Due to a state-wide policy shift in Massachusetts in 2016, and in part because of an HIV outbreak, public support for SSPs increased and local boards of health across the state approved additional SSPs. These program provide a range of services, such as linking to substance use disorder treatment, access to and disposal of sterile syringes and injection equipment, and testing and linkage to care for infectious diseases, including HIV.
“The cluster detection and response effort was important because data drive policy,” says Kevin Cranston, assistant commissioner of MDPH. “Seeing this outbreak, and being able to document its scope and impact, catalyzed tremendous change to provide more and better services to vulnerable communities in Lawrence and Lowell and across Massachusetts.”
1 Acute infection is the first stage of HIV infection and indicates a recent transmission. Learn more about the stages of HIV infection.