Justice, Equity, Diversity, and Inclusion in Climate Adaptation Planning
CDC has partnered with the American Public Health Association (APHA) to create the Climate Change and Health Playbook: Adaptation Planning for Justice, Equity, Diversity, and Inclusion. This comprehensive, step-by-step resource is designed to supplement the Building Resilience Against Climate Effects (BRACE) framework and support public health departments and adaptation planners as they blend JEDI into their climate and health efforts.
CDC has partnered with the American Public Health Association (APHA) to create the Climate Change and Health Playbook: Adaptation Planning for Justice, Equity, Diversity, and Inclusion. This comprehensive, step-by-step resource is designed to supplement the Building Resilience Against Climate Effects (BRACE) framework and support public health departments and adaptation planners as they blend JEDI into their climate and health efforts.


People throughout the United States face climate change-related health risks, but some of us will feel the effects earlier and more severely. This is because of differences in our exposures to climate hazards, our sensitivity to these hazards, and our ability to adapt. (1)
Groups at increased risk include those with low income, some communities of color, immigrant groups (including those with limited English proficiency), Indigenous peoples, children and pregnant women, older adults, vulnerable occupational groups, persons with disabilities, and persons with preexisting or chronic medical conditions. Characterizations of vulnerability should consider how populations of concern experience disproportionate, multiple, and complex risks to their health and well-being in response to climate change.
Climate vulnerability is influenced by three primary factors:

Contact between a person and one or more climate change-related hazards, such as heat waves, wildfires, or floods. For example, outdoor workers might face more frequent and longer exposure to extreme heat. Persons who live or work along the coast could be at risk from sea level rise, flooding, and storm surge.

The degree to which people are negatively affected by climate hazards if exposed. For example, people with pre-existing medical conditions such as asthma are more likely to have poor outcomes when exposed to poor air quality associated with climate change. Because of their developing airways, children who breath in wildfire smoke are more likely to be affected than are adults.

The ability of people to adjust to potential hazards, take advantage of opportunities, or respond to the consequences of climate hazards. This is often directly related to the material or social resources a person or community might draw upon to avoid or lessen risk. For example, older adults might have difficulty walking or lack transportation. This could make it hard for them to get to cooling centers.
Relationship between the factors that affect climate vulnerability and health outcomes
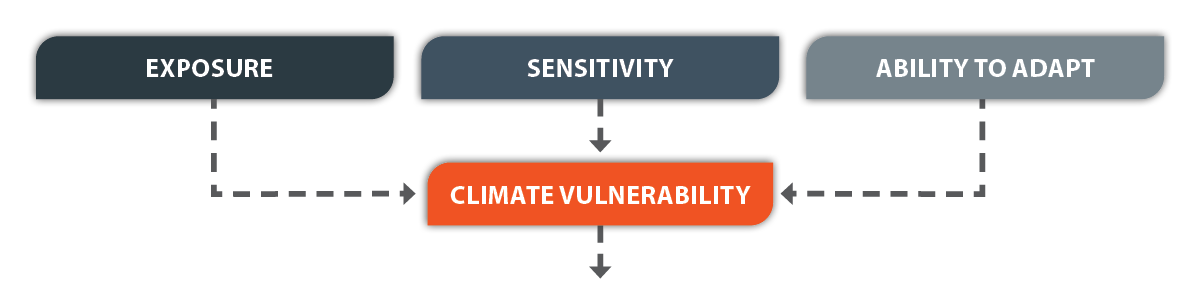

At the individual, community, and national levels, these aspects of vulnerability affect all people to some degree. However, past and present political, economic, social, and environmental factors in our society affect all three of these drivers and lead to some groups having more vulnerability than others. Drivers of climate vulnerability rarely occur alone. For example, extremely hot days can lead to heat-related illnesses such as heat exhaustion or heat stroke. Heat can also increase air pollution levels and health problems related to poor air quality, such as respiratory issues, heart disease, and lung disease. People living in economically or socially marginalized neighborhoods are more likely to experience adverse effects of extreme heat and air pollution than those living in other parts of the same city.
CDC defines climate justice as:
All people — regardless of race, color, national origin, or income — are entitled to equal protection from environmental and health hazards caused by climate change and equal access to the development, implementation, and enforcement of environmental laws, regulations, and policies.
Climate justice recognizes the following:
Climate-related risks are not distributed equally. Many differences in climate vulnerability factors stem from systemic and structural racism, discriminatory policies, stigma, and longstanding marginalization and disenfranchisement. These obstacles particularly affect communities of color, people with disabilities, members of the LGBTQ+ community, women, people who are incarcerated or without homes, and those who live in rural or frontier settings. (2)
Climate change will worsen existing disparities in social conditions and health. Social determinants of health are conditions in the places where people live, learn, work, and play that affect a wide range of health risks and outcomes. Climate change is expected to greatly affect those conditions and to intensify inequities. For example, people with limited income are more likely to live in subsidized housing, which is more likely to be in an area that floods. (3) Their housing options also might have mold problems and inadequate insulation and air conditioning to effectively cope with severe heat or strong storms. People with lower incomes also might be unable to afford flood or fire insurance, rebuild damaged homes, or pay high medical bills after catastrophe strikes, fueling a continuous cycle of increasing vulnerability for those who are already disadvantaged.
Harms associated with climate change are burdening groups that have contributed the least to cause it. Just 20 countries produce more than 80% of greenhouse gas emissions. Most of that (about 25%) has been from the United States. (4) People living in countries that emit less greenhouse gasses are facing serious harm to their health and well-being from gases released by those 20 countries. This disparity in responsibility and harm is also seen between different communities within the United States. (5) Inequities are expected to increase in the future with additional climate change, further marginalizing those who are disproportionately affected. (6)

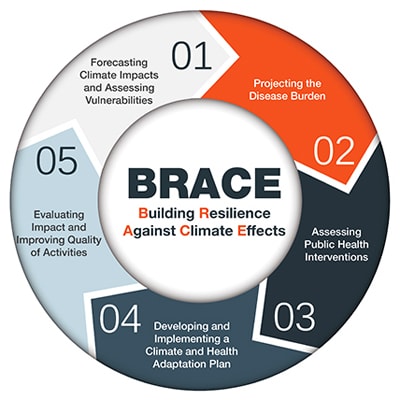
The Building Resilience Against Climate Effects (BRACE) framework is a five-step process that allows health officials to develop strategies and programs to help communities prepare for the health effects of climate change.
CDC partnered with the American Public Health Association (APHA) to create the Climate Change and Health Playbook: Adaptation Planning for Justice, Equity, Diversity, and Inclusion. This comprehensive, yet practical, step-by-step resource is a supplement to BRACE. Understanding JEDI’s role in public health is a critical step to identifying and engaging populations most affected by climate change.
Below are a few activities and key considerations that health departments can use to include JEDI in each step of BRACE.

Forecasting climate Impacts and assessing vulnerabilities
- Define what “vulnerability” means for your jurisdiction
- Build and maintain meaningful community engagement
- Reflect on how JEDI affects the community

Projecting the disease burden
- Anticipate limitations of an entirely quantitative data approach
- Diversify your data to tell a more complete story
- Consider indirect and emerging health consequences of climate change for groups at a higher risk

Assessing public health interventions
- Conduct a racial equity impact assessment
- Work with community members to understand what adaptation efforts are already in place and identify resource gaps
- Offer public health resources in a variety of languages and with options for persons with hearing and visual impairments

Developing and implementing a climate and health adaptation plan
- Develop a logic model to visualize how the adaptation plan will reduce health disparities
- Engage non-health governmental partners
- Delegate adaptation planning and implementation leadership roles to local public leaders

Evaluating impact and improving quality of activities
- Engage community partners in evaluation planning
- Incorporate equity into evaluation questions
- Track populations experiencing inequities
Explore the Climate Change and Health Playbook: Adaptation Planning for Justice, Equity, Diversity, and Inclusion for more details on how to apply JEDI principles to your climate resilience initiatives.
Here are some other governmental strategies intended to move the country toward climate justice.

References
- https://health2016.globalchange.gov/climate-change-and-human-health
- https://www.cdc.gov/healthequity/core/index.html
- https://furmancenter.org/research/publication/housing-in-the-us-floodplains
- https://www.ucsusa.org/resources/each-countrys-share-co2-emissions
- https://www.sciencedirect.com/science/article/pii/S2214629621004552?via%3Dihub
- https://www.sciencedirect.com/science/article/abs/pii/S0140673619325966?via%3Dihub