
Inequities in Physical Activity Environments and Leisure-Time Physical Activity in Rural Communities
ORIGINAL RESEARCH — Volume 19 — July 7, 2022
Michelle C. Kegler, DrPH, MPH1; Nicole Gauthreaux, MPH1; April Hermstad, MPH1; Kimberly Jacob Arriola, PhD, MPH1; Addison Mickens, DrPH, MPH, CHES2; Kelley Ditzel, PhD3; Clarisa Hernandez, MPH1; Regine Haardörfer, PhD1 (View author affiliations)
Suggested citation for this article: Kegler MC, Gauthreaux N, Hermstad A, Arriola KJ, Mickens A, Ditzel K, et al. Inequities in Physical Activity Environments and Leisure-Time Physical Activity in Rural Communities. Prev Chronic Dis 2022;19:210417. DOI: http://dx.doi.org/10.5888/pcd19.210417.
PEER REVIEWED
What is already known on this topic?
Disparities in physical activity exist by race, socioeconomic status, and rurality. Many rural areas have limited resources for leisure-time physical activity.
What is added by this report?
Access to physical activity resources, especially town center connectivity, was associated with leisure-time physical activity. Disparities in leisure-time physical activity were partially explained by perceptions of town center connectivity for lower-income residents and by perceptions of areas around the home/neighborhood for Black residents.
What are the implications for public health practice?
Investments in town center connectivity and racially diverse neighborhoods may aid in reducing inequities in leisure-time physical activity among rural residents.
Abstract
Introduction
Differential access to environments supportive of physical activity (PA) may help explain racial and socioeconomic disparities in leisure-time physical activity (LTPA) in rural communities.
Methods
We used baseline data from a mailed survey (N = 728) conducted in 2019 as part of an evaluation of The Two Georgias Initiative to examine the relationships among LTPA, sociodemographic characteristics, and perceived access to supportive PA environments (eg, areas around the home/neighborhood, indoor and outdoor exercise areas, town center connectivity) in 3 rural Georgia counties.
Results
More than half of respondents (53.5%) engaged in LTPA in the previous month. Perceptions of PA environments were generally neutral to somewhat negative. In multivariable models, overall PA environment was associated with LTPA (OR, 1.58; 95% CI, 1.06–2.35), as was annual household income >$50,000 relative to ≤$20,000 (OR, 2.72; 95% CI, 1.53–4.83) and race, with Black respondents less likely to engage in LTPA than White respondents (OR, 0.49; 95% CI, 0.29–0.85). Of the 5 PA environment domains examined, town center connectivity was significantly associated with LTPA (OR, 1.68, 95% CI, 1.20–2.36). Both the overall PA score (β = −0.014; 95% CI, −0.029 to −0.002) and town center connectivity (β = −0.020; 95% CI, −0.038 to −0.005) partially mediated associations between annual household income and LTPA. Areas supportive of PA around the home/neighborhood partially mediated the association by race (β = 0.016; 95% CI, 0.001–0.034).
Conclusion
Findings lend support for investing in town centers and racially diverse neighborhoods to increase walkability and PA infrastructure as potential strategies to reduce inequities in LTPA.
Introduction
Rural residents are less likely to meet federal physical activity (PA) guidelines than their urban counterparts, with the lowest rates among rural residents in the South (1–3). Although rural communities vary, they typically have lower levels of educational attainment, higher levels of poverty, less investment in infrastructure, and distance and/or terrain that decreases access to health-promoting resources (4,5). Scholars have urged the consideration of rurality in intersectionality approaches that examine how overlapping social categories produce inequalities based on disadvantaged social position (6–9). Knowledge about intersections of rurality, race, and socioeconomic status (SES) help to illuminate disparities in PA (1,2,10). According to the 2016–2017 National Health Interview Survey, 17.9% of rural Black adults met PA guidelines, compared with 27.8% of urban White adults, and a similar disparity was observed for rurality and education (ie, lowest rates of PA for rural residents with less education) (1).
Although PA is influenced by an array of determinants, studies generally show associations between features of the environment that support active living (eg, streetlights, paths, access to recreational facilities, aesthetics) and PA across the rural–urban continuum (11–14). Consistent with structural models that highlight the interplay among physical structures, social structures, and policies in producing inequities (15), using an equity lens necessitates a deeper examination of who has access to environments that support PA and whether differential access to health-promoting environments can explain differences in PA by race and SES in rural areas.
Given the possibility that unequal access to supportive environments may contribute to disparities in PA (7,13,16), the aims of this study were to examine 1) associations between the dimension of the PA environment and leisure-time PA (LTPA), 2) differential access to PA environments by race, SES, and neighborhood rurality, and 3) whether environments mediate relationships between race, SES, and LTPA in rural communities.
Methods
The Two Georgias Initiative is a place-based initiative designed to achieve greater health equity among rural Georgians. In 2017, the Healthcare Georgia Foundation funded 11 coalitions in rural Georgia (county population <35,000) to conduct a community assessment, develop a community health improvement plan, and implement strategies to address a range of community-identified priority areas, including efforts to improve PA environments. Throughout the 5-year initiative, coalitions received up to $100,000 per year and technical assistance and support from a community coach, external evaluators, and equity experts.
Data collection
This cross-sectional study used data from a baseline population-based survey that explored behaviors and environments related to common coalition priority areas. The survey was designed with different modules that mapped to local priorities: PA and access to active living environments, healthy eating and food access, health care access, social capital, and quality of life. Respondents were included in the study if they lived in 1 of the 3 counties in which the full PA module was administered (N = 728). In 2018, the population sizes in these counties ranged from 5,800 to 18,500, and Rural-Urban Continuum Codes were 7 and 8 (17).
We used commercial lists of randomly selected residential mailing addresses to identify the sampling frame, which varied by county size. One adult per household was eligible to participate. Baseline surveys were mailed in waves from January through March 2019. Each mailing included an introductory letter describing the study and information on the incentive (a $15 gift card), the survey, and a stamped return envelope. Each household received a postcard reminder and, if necessary, a second survey. A total of 2,671 surveys were sent, and 728 were completed (27.2% response rate); the county-specific response rate ranged from 25.6% to 31.7%. The Emory University Institutional Review Board determined that this study was a nonresearch program evaluation that did not require institutional review board approval.
Measures
Leisure-time physical activity
We used a measure from the Centers for Disease Control and Prevention’s Behavioral Risk Factor Surveillance System (BRFSS) to measure LTPA (18). Respondents were asked, “During the past month, other than your regular job, did you participate in any physical activities or exercises such as running, calisthenics, golf, gardening, or walking for exercise?” Response options were yes, no, or don’t know/not sure. We excluded responses of don’t know/not sure from analyses that used this variable.
Walking and biking for transport
We assessed walking and biking for transport by asking, “How often do you use each of the following to get from place to place?” and then listing walk, bike, personal vehicle (car/truck/sport utility vehicle), golf cart, ride from family/friend/neighbor, taxi service or rideshare such as Uber/Lyft, and public transportation (bus/van). Response options ranged from 0 (never) to 4 (daily) (19).
Perceived PA environments
Questions on overall PA environment and 5 domains were adapted from the Rural Active Living Perceived Environmental Support Scale, or RALPESS (20). We chose 22 items from the original measure. We computed a mean score for each of 5 domains by averaging the scores obtained from a 5-point Likert scale, where 0 indicated strongly disagree; 1, disagree; 2, neutral; 3, agree; and 4, strongly agree. We computed an overall score by averaging all 22 items, with selected items reverse coded as necessary. Cronbach α was 0.85.
Area around your home/neighborhood contained 6 items: 1) the roads around my home have a place to walk or ride a bike next to the road, 2) the roads around my home have good lighting, 3) it is safe to walk or ride a bike on the roads around my home, 4) there is fast traffic on the roads around my home, 5) there are busy roads to cross around my home, and 6) loose dogs in the area around my home make it unsafe to take walks. Cronbach α was 0.67.
Indoor exercise areas contained 3 items: 1) my town has private indoor exercise areas (pay to use), 2) my town offers indoor exercise activities (eg, programs, sports teams, classes, lessons, etc), and 3) there are choices of activities for PA or exercise at the indoor exercise areas in my town. Cronbach α was 0.87.
Outdoor exercise areas contained 4 items: 1) outdoor exercise areas in my town have available restrooms, 2) outdoor exercise areas in my town have water fountains, 3) outdoor exercise areas are nice to use, and 4) police officers or sheriffs regularly patrol the outdoor areas in my town where people could be physically active or exercise. Cronbach α was 0.88.
Town center connectivity contained 5 items: 1) there are shopping areas and places to eat in the town center, 2) there are sidewalks in the town center, 3) the sidewalks are nice to use in the town center (eg, they are shaded, there are pleasant things to look at, no trash, well kept), 4) the streets are marked where I should cross in the town center or there are crosswalks, and 5) the area around the town center has working streetlights. Internal consistency was good for this domain (Cronbach α = 0.88)
Lastly, school and church facilities were combined to create an organizational facilities domain of 4 items: 1) at least 1 school allows community members to use indoor facilities during nonschool hours, 2) at least 1 school allows community members to use outdoor facilities during nonschool hours, 3) my community has churches with indoor recreational areas for exercise open to the public, and 4) my community has churches with outdoor recreational areas for exercise open to the public. Cronbach α was 0.69.
Sociodemographic characteristics
The 3 primary sociodemographic variables of interest were race, annual household income, and neighborhood rurality. Race and ethnicity were assessed by asking, “What is your race or ethnicity?” Response options were White, not of Hispanic origin; African American or Black, not of Hispanic origin; Hispanic; more than 1 race; and other. We dichotomized into White or Black, with other races and ethnicities excluded in multivariable models and bivariate analyses examining racial differences because of small numbers. Annual household income was assessed by asking, “What is your total yearly household or family income from all sources?” Response options included 3 categories, which we combined according to distribution: $20,000 or less, $20,001 to $50,000, and more than $50,000. Neighborhood rurality was assessed with the question, “Which of the following best describes the neighborhood where you live? By neighborhood, we mean the area within a 20-minute walk from your home.” This item was created by our team to capture qualitative differences based on where one lived in a rural county. We combined responses into 2 categories: in town or rural area. The survey also assessed age, sex, education, employment, marital status, and height and weight, which were used to calculate body mass index (BMI).
Data analysis
We used SPSS version 26.0 (IBM Corp) and SAS version 9.4 (SAS Institute, Inc) to conduct descriptive and multivariable analyses. Sociodemographic differences between those engaged in LTPA and those who were not were assessed by using t tests, analysis of variance, and χ2 tests, as appropriate for each variable type. Differences in PA environments by group (eg, race) were tested by using 1-way analysis of variance and t tests, with the Tukey honestly significant difference test used to identify posthoc differences between groups. We used multivariable logistic regressions to assess associations between LTPA and the PA environment. The first model included the overall PA environment score and the second included the individual domain scores; both models included race, annual household income, and neighborhood rurality as independent variables, while controlling for sex, age, and county. We excluded records with data missing on any of these variables (ie, we used listwise deletion).
To explore whether PA environments may at least partly explain racial differences in LTPA, we used structural equation modeling through variable-measured path models with 1 mediator, which is equivalent to a simple mediation model that accommodates noncontinuously distributed variables and allows for clustering (21). At the bivariate level, we conducted simple linear regression models between the independent variables and each of the 5 PA environment domains and overall score. We used MPlus version 8.4 (Muthen & Muthen) to conduct mediation analyses to assess whether the PA environment (ie, overall and specific domains) mediates the effects of race or income on PA. Models accounted for clustering in counties, and 95% CIs for the indirect effects were determined by using bootstrapping (n = 1,000).
Results
Overall, the sample was 68.9% female and 32.4% Black, with a mean age of 60.5 (SD, 15.4) years (Table 1). Respondents were well distributed across annual household income categories: 30.0% lived on $20,000 or less, 38.4% on $20,001 to $50,000, and 31.7% on more than $50,000. Similarly, we found a broad range of education levels and employment: 41.1% were retired and 34.8% worked full-time. More than half (58.1%) were married or living with a partner. Most described themselves as living in rural areas of the county (81.1%) as opposed to in town (18.9%).
LTPA by sociodemographic characteristics
Overall, slightly more than half (53.5%; 348 of 651) of respondents had engaged in LTPA at least once in the previous month. We found significant differences in LTPA for every variable we examined except sex and county (Table 1). LTPA was most common among White respondents (59.1%), those with annual household income of more than $50,000 (70.9%), those with a college degree (69.6%), and those who worked full-time (62.4%). Respondents engaging in LTPA were younger on average, more frequently walked or biked for transport, and were normal weight (62.7%) or overweight (61.6%). Those living in rural areas (57.0%) were more likely to engage in LTPA than those living in town (41.7%).
Physical activity environments by LTPA
The composite PA environment score was associated with LTPA for respondents who engaged in LTPA (mean, 2.0; SD, 0.03) versus those who did not (mean, 1.8; SD, 0.03) (Table 1). Only 1 domain, town center connectivity, was associated with LTPA (mean, 2.6; SD, 0.7 vs mean, 2.4; SD, 0.8). Although significant, differences were small for both the overall composite score and the town center connectivity domain. Indoor exercise areas, outdoor exercise areas, and school and church facilities were not associated with LTPA.
Physical activity environments by selected demographic and neighborhood variables
Ratings of the PA environments generally ranged from neutral to slightly negative (range, 1.4–2.6) (Table 2). On the basis of the overall composite score, respondents with higher annual household incomes perceived their PA environments slightly more positively than respondents with middle and low household incomes. Black respondents viewed their PA environments slightly more negatively than White respondents, and we found no significant difference based on neighborhood rurality.
Three of the 5 PA environment domains differed by annual household income: indoor exercise areas, outdoor exercise areas, and town center connectivity (Table 2). For 2 domains (indoor and outdoor exercise areas), respondents with an annual household income of more than $50,000 had more positive perceptions than respondents in the 2 lower income categories. For town center connectivity, respondents with annual household incomes of more than $50,000 had more positive perceptions than those with annual household incomes of $20,000 or less.
All 5 PA environment domains differed by race (Table 2). White respondents had more positive perceptions than Black respondents about indoor exercise areas, outdoor exercise areas, town center connectivity, and school and church facilities. Black respondents, in contrast, had more positive perceptions about the area around their homes. Only 1 PA environment domain differed by neighborhood rurality: respondents living in town viewed the area around their home more positively than did those who lived in more rural areas.
Multivariable associations between sociodemographic characteristics, PA environments, and LTPA
In the first model, the overall composite PA environments score was significantly associated with engaging in any LTPA (OR, 1.58; 95% CI, 1.06–2.35) (Table 3). Annual household income of more than $50,000 was also associated with increased odds of LTPA (OR, 2.72; 95% CI, 1.53–4.83). Black respondents were less likely than White respondents to engage in LTPA (OR, 0.49; 95% CI, 0.29–0.85).
In the second model, of the 5 dimensions examined, only perceptions of town center connectivity was significantly associated with LTPA (OR, 1.68; 95% CI, 1.20–2.36). Race and annual household income were also significant, with Black respondents less likely than White respondents (OR, 0.51; 95% CI, 0.29–0.88) and respondents with an annual household income of more than $50,000 more likely to engage in LTPA (OR, 2.83; 95% CI, 1.57–5.07).
Mediation analyses
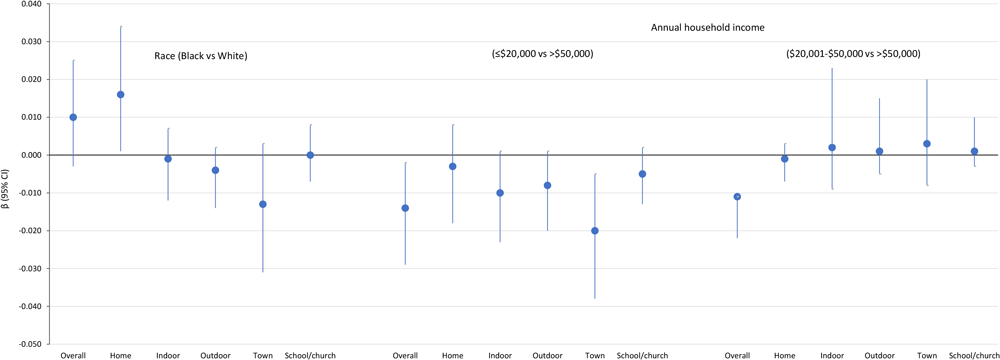
In models assessing whether perceptions of the PA environment mediate the relationship between annual household income and PA, we found that the composite PA environment score mediated this relationship for respondents in the lowest income category (β = −0.014; 95% CI, −0.029 to −0.002) and middle income category (β = −0.011; 95% CI, −0.022 to −0.011) compared with respondents in the highest income category (Figure 1). Of the 5 domains (Figure 1), only town center connectivity significantly mediated the relationship between low annual household income and PA (β = −0.020; 95% CI, −0.038 to −0.005).
![]()
Figure 1.
Standardized mediation effect sizes estimating the indirect effect for the overall score on the physical activity environment and component scores as mediators between race or annual household income and physical activity in 3 rural counties in Georgia, 2019. [A tabular version of this figure is available.]
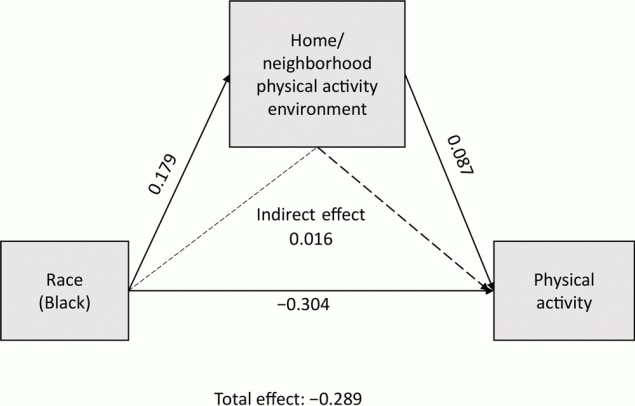
In our assessment of whether perceptions of the PA environment mediate the relationship between race and LTPA, we found that the overall score did not (Figure 1), but the home/neighborhood environment partially mediated the relationship between race and LTPA (β = 0.016; 95% CI, 0.001–0.034) (Figure 1 and Figure 2).
![]()
Figure 2.
Home/neighborhood physical activity environment as a mediator of the relationship between race and leisure-time physical activity in 3 rural counties in Georgia, 2019. [A text version of this figure is available.]
Discussion
We examined whether perceived access to environments supportive of PA was associated with increased LTPA. We also examined access to these environments by race, SES (annual household income), and neighborhood rurality, and whether differential access to supportive environments may explain racial and SES differences in LTPA in a rural population. In multivariable analyses, we found that residents in these rural counties who reported a more favorable PA environment were more likely to engage in LTPA. Although most studies of the environment and PA have focused on urban and suburban environments, several studies have documented associations in rural populations, albeit with varied dimensions emerging as salient (12,13,22–24). Of the 5 PA environment domains we examined, town center connectivity was significantly associated with LTPA in multivariable models. Other domains, including one’s home/neighborhood, indoor and outdoor exercise areas, and school and church facilities were not significantly associated with LTPA. This finding may have resulted partly from a measurement issue for the home/neighborhood domain. Previous qualitative research in the same region found that much PA around the home occurred through yard work, which would not have been captured in the home/neighborhood measure because of its focus on walkability (25). Notably, perceptions of the various domains were mainly neutral to negative across the board. This limited variability may have reduced our ability to detect associations with LTPA. Previous research on these domains in the RALPESS instrument focused on validity and reliability of the measure, excluding predictive validity (20,26).
We also examined perceptions of access to various PA domains. Our findings generally support past research that documents that supportive PA environments are less available in rural areas than in nonrural areas (24,27,28). Only the area around one’s home varied by neighborhood rurality; however, all domains varied by race and most also varied by annual household income. In general, White respondents reported better access than Black respondents in all domains except around one’s home. Overall PA environment and 3 domains varied by annual household income, including indoor and outdoor recreation areas and town center connectivity.
Our study also examined whether differential access to environments supportive of PA might explain racial and SES differences in PA during leisure time. Results showed that the overall PA environment partially mediated the association between annual household income and LTPA. This finding lends support to investing in PA environments as a strategy to promote PA and reduce income-related inequities. To our knowledge, ours is one of the first studies to examine how PA environments may mediate associations between race and LTPA in rural communities (15). In an examination of which domains may mediate this association, town center connectivity was significant. These findings, even though the effect was small, lend support to main street investment that increases walkability (eg, sidewalks, lighting, aesthetics, destinations) and other efforts to improve access to PA opportunities given their potential to increase LTPA in rural communities, especially for lower-income households. Several community coalitions in The Two Georgias Initiative are working to improve PA infrastructure (eg, playgrounds, walking trails) and stimulate new destinations in the town center (eg, walking tour of historic sites, flea markets).
We found that the area around one’s home partially mediated the association between race and LTPA. Specifically, Black respondents reported slightly more positive walkability around their homes (eg, safe to walk/ride bike on roads), and this factor reduced the association between race and LTPA. Although the effect was small and based on cross-sectional data, this finding suggests that efforts to increase neighborhood walkability, especially in majority-Black neighborhoods, deserve attention as a potential strategy to increase LTPA. A review of the built environment and PA among African Americans noted some evidence for sidewalks, light traffic, and safety from crime as associated with PA (29). Not having time or transportation to gain access to spaces for PA has also been identified as a barrier for African Americans (30) and provides further justification for a neighborhood focus. Moreover, given the history of redlining, residential segregation, and disinvestment in Black neighborhoods that has resulted in neighborhoods with fewer health-promoting amenities (16,31,32), this approach would be an appropriate step toward health equity.
Limitations
This study has several limitations. First, it was cross-sectional, which negates our ability to infer causality. It may be that people who engage in LTPA view their environments as more conducive to PA based on their direct experience in these environments. Second, our measures, including PA, were self-reported and may have been subject to social desirability bias. Additionally, it would have been useful to have complementary objective measures of the environment. Third, although the sample was randomly selected, the response rate was low and respondents tended to be older, more educated, and White relative to the overall population in the US census. Despite this, our response rate and methods are consistent with recent recommendations (and response rates) for surveillance in rural communities (33). Fourth, even though we adjusted for clustering at the county level, clustering within smaller geographic units may have occurred. Fifth, we modified the RALPESS instrument to align with evaluation objectives, which may have decreased its reliability. Finally, we focused on LTPA. Thus, our findings do not apply to all forms of PA, including occupational and transport-related activity.
Conclusion
These findings, even though the effect was small and data were cross-sectional, lend support to downtown improvement projects that increase walkability (eg, sidewalks, crosswalks, lighting, aesthetics, destinations) and other efforts to improve access to PA opportunities given their potential to increase LTPA in rural communities, especially for lower-income households. Our study also suggests that investing in Black neighborhoods to make them more supportive of PA (eg, improved sidewalks, lighting, nice aesthetics, destinations) may pay dividends in terms of public health outcomes such as increased PA. Overall, this study adds to the limited research on PA in rural areas and provides insight into whether and how the environment may contribute to racial and SES differences in LTPA.
Acknowledgments
This study was funded by Healthcare Georgia Foundation Grant 3342 Evaluation of The Two Georgias Initiative. No copyrighted materials were used in this article.
Author Information
Corresponding Author: Michelle C. Kegler, DrPH, MPH, Department of Behavioral, Social and Health Education Sciences, Emory Prevention Research Center, Rollins School of Public Health, Emory University, 1518 Clifton Rd NE, Atlanta, GA 30322. Telephone: 404-712-9957. Email: mkegler@emory.edu.
Author Affiliations: 1Department of Behavioral, Social and Health Education Sciences, Emory Prevention Research Center, Rollins School of Public Health, Emory University, Atlanta, Georgia. 2Share Health Southeast Georgia, Waycross, Georgia. 3Public Administration, Georgia College & State University, Milledgeville, Georgia.
References
- Whitfield GP, Carlson SA, Ussery EN, Fulton JE, Galuska DA, Petersen R. Trends in meeting physical activity guidelines among urban and rural dwelling adults — United States, 2008–2017. MMWR Morb Mortal Wkly Rep 2019;68(23):513–8. CrossRef PubMed
- Matthews KA, Croft JB, Liu Y, Lu H, Kanny D, Wheaton AG, et al. Health-related behaviors by urban–rural county classification — United States, 2013. MMWR Surveill Summ 2017;66(5):1–8. CrossRef PubMed
- Trivedi T, Liu J, Probst J, Merchant A, Jhones S, Martin AB. Obesity and obesity-related behaviors among rural and urban adults in the USA. Rural Remote Health 2015;15(4):3267. CrossRef PubMed
- Crosby RA, Wendel ML, Vanderpool RC, Casey BR. Rural populations and health: determinants, disparities, and solutions. New York (NY): John Wiley & Sons; 2012.
- Leider JP, Meit M, McCullough JM, Resnick B, Dekker D, Alfonso YN, et al. The state of rural public health: enduring needs in a new decade. Am J Public Health 2020;110(9):1283–90. CrossRef PubMed
- Abshire DA, Wippold GM, Wilson DK, Pinto BM, Probst JC, Hardin JW. Rurality, gender, and obesity: an intersectionality perspective on rural men’s health. Am J Public Health 2021;111(10):1761–3. CrossRef PubMed
- Mwangi EW, Constance-Huggins M. Intersectionality and Black women’s health: making room for rurality. J Prog Hum Serv 2019;30(1):11–24. CrossRef
- Afifi RA, Parker EA, Dino G, Hall DM, Ulin B. Reimagining rural: shifting paradigms about health and well-being in the rural United States. Annu Rev Public Health 2022;43(1):135–54. CrossRef PubMed
- Crenshaw K. Demarginalizing the intersection of race and sex: a Black feminist critique of antidiscrimination doctrine, feminist theory and antiracist politics. Univ Chi Leg F 1989:139(1).
- James CV, Moonesinghe R, Wilson-Frederick SM, Hall JE, Penman-Aguilar A, Bouye K. Racial/ethnic health disparities among rural adults — United States, 2012–2015. MMWR Surveill Summ 2017;66(23):1–9. CrossRef PubMed
- Cohen DA, Scribner RA, Farley TA. A structural model of health behavior: a pragmatic approach to explain and influence health behaviors at the population level. Prev Med 2000;30(2):146–54. CrossRef PubMed
- Frost SS, Goins RT, Hunter RH, Hooker SP, Bryant LL, Kruger J, et al. Effects of the built environment on physical activity of adults living in rural settings. Am J Health Promot 2010;24(4):267–83. CrossRef PubMed
- Whitfield GP, Carlson SA, Ussery EN, Watson KB, Berrigan D, Fulton JE. National-level environmental perceptions and walking among urban and rural residents: informing surveillance of walkability. Prev Med 2019;123:101–8. CrossRef PubMed
- Lee KH, Dvorak RG, Schuett MA, van Riper CJ. Understanding spatial variation of physical inactivity across the continental United States. Landsc Urban Plan 2017;168:61–71. CrossRef
- Smith M, Hosking J, Woodward A, Witten K, MacMillan A, Field A, et al. Systematic literature review of built environment effects on physical activity and active transport — an update and new findings on health equity. Int J Behav Nutr Phys Act 2017;14(1):158. CrossRef PubMed
- Lovasi GS, Hutson MA, Guerra M, Neckerman KM. Built environments and obesity in disadvantaged populations. Epidemiol Rev 2009;31(1):7–20. CrossRef PubMed
- US Census Bureau. Quickfacts. Accessed June 15, 2019. https://www.census.gov/quickfacts/fact/table/US/PST045219.
- Centers for Disease Control and Prevention. Behavioral Risk Factor Surveillance System survey questionnaire. Atlanta (GA): US Department of Health and Human Services, Centers for Disease Control and Prevention; 2017.
- Quinn TD, Jakicic JM, Fertman CI, Barone Gibbs B. Demographic factors, workplace factors and active transportation use in the USA: a secondary analysis of 2009 NHTS data. J Epidemiol Community Health 2017;71(5):480–6. CrossRef PubMed
- Umstattd MR, Baller SL, Hennessy E, Hartley D, Economos CD, Hyatt RR, et al. Development of the Rural Active Living Perceived Environmental Support Scale (RALPESS). J Phys Act Health 2012;9(5):724–30. CrossRef PubMed
- Kline R. Principles and practice of structural equation modeling. New York (NY): Guilford Publications; 2015.
- Abildso CG, Daily SM, Meyer MRU, Edwards MB, Jacobs L, McClendon M, et al. Environmental factors associated with physical activity in rural U.S. counties. Int J Environ Res Public Health 2021;18(14):7688. CrossRef PubMed
- Nykiforuk CIJ, Atkey K, Brown S, Caldwell W, Galloway T, Gilliland J, et al. Promotion of physical activity in rural, remote and northern settings: a Canadian call to action. Health Promot Chronic Dis Prev Can 2018;38(11):419–35. CrossRef PubMed
- Hill JL, Waters CN, Kolivras KN, Estabrooks PA, Zoellner JM. Do the features, amenities, and quality of physical activity resources differ between city and county areas of a large rural region? Fam Community Health 2016;39(4):273–82. CrossRef PubMed
- Kegler MC, Escoffery C, Alcantara I, Ballard D, Glanz K. A qualitative examination of home and neighborhood environments for obesity prevention in rural adults. Int J Behav Nutr Phys Act 2008;5(1):65. CrossRef PubMed
- Nolan R, Agley J, Umstattd Meyer MR, Spicer PG, Hallam JS. Continued development of the Rural Active Living Perceived Environmental Support Scale (RALPESS): preliminary evidence for validity among American Indians. Rural Remote Health 2019;19(2):5200–5200. CrossRef PubMed
- Umstattd Meyer MR, Moore JB, Abildso C, Edwards MB, Gamble A, Baskin ML. Rural active living: a call to action. J Public Health Manag Pract 2016;22(5):E11–20. CrossRef PubMed
- Robinson JC, Carson TL, Johnson ER, Hardy CM, Shikany JM, Green E, et al. Assessing environmental support for better health: active living opportunity audits in rural communities in the southern United States. Prev Med 2014;66:28–33. CrossRef PubMed
- Casagrande SS, Whitt-Glover MC, Lancaster KJ, Odoms-Young AM, Gary TL. Built environment and health behaviors among African Americans: a systematic review. Am J Prev Med 2009;36(2):174–81. CrossRef PubMed
- Sa J, Heimdal J, Sbrocco T, Seo D-C, Nelson B. Overweight and physical inactivity among African American students at a historically black university. J Natl Med Assoc 2016;108(1):77–85. CrossRef PubMed
- Powell LM, Slater S, Chaloupka FJ, Harper D. Availability of physical activity-related facilities and neighborhood demographic and socioeconomic characteristics: a national study. Am J Public Health 2006;96(9):1676–80. CrossRef PubMed
- Duncan DT, Aldstadt J, Whalen J, White K, Castro MC, Williams DR. Space, race, and poverty: spatial inequalities in walkable neighborhood amenities? Demogr Res 2012;26(17):409–48. CrossRef PubMed
- Lee DC, McGraw NA, Doran KM, Mengotto AK, Wiener SL, Vinson AJ, et al. Comparing methods of performing geographically targeted rural health surveillance. Emerg Themes Epidemiol 2020;17(1):3. CrossRef PubMed
Tables
| Characteristic | Full sample (N = 728)b | Engaged in leisure-time PA in past month (n = 348)b | Did not engage in leisure-time PA in past month (n = 303)b | P valuec |
|---|---|---|---|---|
| Age, mean (SD), y | 60.5 (15.4) | 57.9 (15.1) | 63.4 (15.0) | <.001 |
| Sex | ||||
| Male | 217 (31.1) | 115 (58.1) | 83 (41.9) | .17 |
| Female | 480 (68.9) | 228 (52.2) | 209 (47.8) | |
| Raced | ||||
| White | 456 (67.6) | 250 (59.1) | 173 (40.9) | <.001 |
| Black | 219 (32.4) | 82 (42.5) | 111 (57.5) | |
| Annual household income, $ | ||||
| ≤20,000 | 175 (30.0) | 58 (38.4) | 93 (61.6) | <.001 |
| 20,001–50,000 | 224 (38.4) | 109 (53.2) | 96 (46.8) | |
| >50,000 | 185 (31.7) | 122 (70.9) | 50 (29.1) | |
| Education | ||||
| Some high school or less | 81 (11.5) | 27 (38.6) | 43 (61.4) | <.001 |
| High school diploma/GED | 207 (29.3) | 80 (42.6) | 108 (57.4) | |
| Some college or technical school | 221 (31.1) | 111 (55.8) | 88 (44.2) | |
| College and above | 197 (27.9) | 126 (69.6) | 55 (30.4) | |
| Employment | ||||
| Working full-time | 237 (34.8) | 138 (62.4) | 83 (37.6) | <.001 |
| Working part-time | 45 (6.6) | 22 (53.7) | 19 (46.3) | |
| Retired | 280 (41.1) | 133 (53.4) | 116 (46.6) | |
| Not employed/homemaker/student/on disability | 120 (17.6) | 39 (35.8) | 70 (64.2) | |
| Marital status | ||||
| Married/living with partner | 423 (58.1) | 224 (58.8) | 157 (41.2) | .002 |
| Separated/divorced/widowed | 201 (27.6) | 102 (42.7) | 76 (57.3) | |
| Single | 104 (14.3) | 48 (52.1) | 44 (47.8) | |
| Neighborhood rurality | ||||
| In town | 120 (18.9) | 50 (41.7) | 70 (58.3) | .002 |
| Rural | 514 (81.1) | 293 (57.0) | 221 (43.0) | |
| County of residence | ||||
| County A | 276 (37.9) | 131 (52.8) | 117 (47.2) | .19 |
| County B | 242 (33.2) | 121 (58.2) | 87 (41.8) | |
| County C | 210 (28.8) | 96 (49.2) | 99 (50.8) | |
| Active transportation modes, mean (SD)e | ||||
| Walking | 1.4 (1.5) | 1.7 (1.5) | 1.1 (1.4) | <.001 |
| Biking | 0.3 (0.8) | 0.4 (0.8) | 0.2 (0.8) | .04 |
| Body mass index, kg/m2 | ||||
| Normal weight (18.5–24.9) | 158 (23.4) | 89 (62.7) | 53 (37.3) | <.001 |
| Overweight (25.0–29.9) | 226 (33.5) | 125 (61.6) | 78 (38.4) | |
| Obese (≥30.0) | 291 (43.1) | 115 (43.7) | 148 (56.3) | |
| Physical activity environment domains, mean (SD)f | ||||
| Around home/neighborhood | 1.6 (0.8) | 1.7 (0.9) | 1.6 (0.8) | .17 |
| Indoor exercise areas | 2.0 (1.2) | 2.1 (1.2) | 1.9 (1.2) | .11 |
| Outdoor exercise areas | 1.7 (1.0) | 1.7 (1.0) | 1.7 (1.0) | .32 |
| Town center connectivity | 2.5 (0.8) | 2.6 (0.7) | 2.4 (0.8) | .001 |
| School and church facilities | 1.7 (0.8) | 1.7 (0.7) | 1.6 (0.8) | .24 |
| Overall composite score | 1.9 (0.6) | 2.0 (0.03) | 1.8 (0.03) | .02 |
Abbreviations: GED, General Educational Development.
a The authors developed and administered a baseline population-based survey that explored behaviors and environments related to physical activity. All values are number (percentage) unless otherwise indicated; percentages may not add to 100 because of rounding.
b Numbers in categories may not add to numbers in column headers because not all respondents answered all questions; percentages are based on the number of respondents who answered the question. Responses of don’t know/not sure were excluded.
c For continuous variables (mean [SD]), t test was used. For categorical variables, χ2 test was used.
d Assessed by asking, “What is your race or ethnicity?” Response options were White, not of Hispanic origin; African American or Black, not of Hispanic origin; Hispanic; more than 1 race; and other. Responses were dichotomized into White or Black, with other races and ethnicities excluded in multivariable models and bivariate analyses examining racial differences because of small numbers.
e Assessed by asking, “How often do you use each of the following to get from place to place?” and then listing walk, bike, personal vehicle (car/truck/sport utility vehicle), golf cart, ride from family/friend/neighbor, taxi service or rideshare such as Uber/Lyft, and public transportation (bus/van). Response options ranged from 0 (never) to 4 (daily).
f Overall physical activity environment and specific domains were adapted from the Rural Active Living Perceived Environmental Support Scale, or RALPESS (20); 22 items were chosen from the original measure. A mean score for each domain was computed by averaging the scores obtained from a 5-point Likert scale, where 0 indicated strongly disagree; 1, disagree; 2, neutral; 3, agree; and 4, strongly agree. An overall score was computed by averaging all 22 items, with selected items reverse coded as necessary.
| Characteristic | Around home or neighborhood | Indoor exercise areas | Outdoor exercise areas | Town center connectivity | School and church facilities | Overall composite score |
|---|---|---|---|---|---|---|
| Rating by neighborhood rurality, mean (SD) | ||||||
| In town | 1.8 (0.8) | 2.1 (1.2) | 1.8 (1.0) | 2.5 (0.7) | 1.7 (0.8) | 2.0 (0.5) |
| Rural | 1.6 (0.8) | 2.0 (1.7) | 1.7 (1.0) | 2.5 (0.8) | 1.7 (0.8) | 1.9 (0.6) |
| P valueb | .009 | .35 | .34 | .64 | .41 | .07 |
| Rating by annual household income, mean (SD), $ | ||||||
| ≤20,000 | 1.7 (0.7) | 1.8 (1.2) | 1.6 (1.0) | 2.3 (0.8) | 1.6 (0.8) | 1.8 (0.6) |
| 20,001–50,000 | 1.6 (0.8) | 1.8 (1.2) | 1.6 (1.0) | 2.5 (0.8) | 1.6 (0.8) | 1.8 (0.6) |
| >50,000 | 1.7 (0.9) | 2.3 (1.2)c | 1.9 (0.9)c | 2.6 (0.7)d | 1.8 (0.7) | 2.0 (0.6)c |
| P valuee | .76 | <.001 | .005 | .004 | .05 | .003 |
| Rating by race, mean (SD) | ||||||
| Black | 1.9 (0.8) | 1.7 (1.2) | 1.4 (1.0) | 2.3 (0.8) | 1.5 (0.9) | 1.8 (0.6) |
| White | 1.6 (0.8) | 2.1 (1.2) | 1.9 (0.9) | 2.6 (0.7) | 1.7 (0.7) | 2.0 (0.6) |
| P valueb | <.001 | <.001 | <.001 | <.001 | .001 | .003 |
a The authors developed and administered a baseline population-based survey that explored behaviors and environments related to physical activity. Questions on overall physical activity environment and 5 domains were adapted from the Rural Active Living Perceived Environmental Support Scale, or RALPESS (20). The survey asked respondents to respond to such statements as “The roads around my home have good lighting” and “Outdoor exercise areas in my town have water fountains.” Response options were 0, strongly disagree; 1, disagree; 2, neutral; 3, agree; and 4, strongly agree; missing data were excluded from denominators.
b Determined by t test.
c Households with >$50,000 in annual household income had significantly more positive perceptions than respondents in middle- and low-income groups.
d Households with >$50,000 in annual household income had significantly more positive perceptions than respondents in the lowest income groups.
e Determined by analysis of variance, with Tukey honestly significant difference test.
| Model | Odds Ratio (95% CI) |
|---|---|
| Model 1a: overall physical activity environment | |
| Composite physical activity environment score | 1.58 (1.06–2.35) |
| Rural (vs in town) | 1.33 (0.79–2.44) |
| Black (vs White) | 0.49 (0.29–0.85) |
| Annual household income $20,001 to $50,000 (vs ≤$20,000) | 1.66 (1.00–2.76) |
| Annual household income >$50,000 (vs ≤$20,000) | 2.72 (1.53–4.83) |
| Model 2a: physical activity environment components | |
| Town center | 1.68 (1.20–2.36) |
| Around home | 1.10 (0.84–1.44) |
| Indoor areas in town | 0.88 (0.70–1.11) |
| Outdoor areas in town | 0.99 (0.74–1.33) |
| School and church facilities | 1.09 (0.80–1.48) |
| Rural (vs in town) | 1.28 (0.75–2.17) |
| Black (vs White) | 0.51 (0.29–0.88) |
| Annual household income $20,001 to $50,000 (vs ≤$20,000) | 1.60 (0.95–2.68) |
| Annual household income >$50,000 (vs ≤$20,000) | 2.83 (1.57–5.07) |
a The authors developed and administered a baseline population-based survey that explored behaviors and environments related to physical activity. Questions on overall physical activity environment and 5 domains were adapted from the Rural Active Living Perceived Environmental Support Scale, or RALPESS (20). The survey asked respondents to respond to such statements as “the roads around my home have good lighting” and “outdoor exercise areas in my town have water fountains.” N = 439 (analysis did not include respondents with missing values); adjusted for covariates (county, sex, and age). The 3 primary sociodemographic variables of interest were race, annual household income, and neighborhood rurality.
Error processing SSI fileThe opinions expressed by authors contributing to this journal do not necessarily reflect the opinions of the U.S. Department of Health and Human Services, the Public Health Service, the Centers for Disease Control and Prevention, or the authors’ affiliated institutions.