
Free Living Amebic Infections
[Acanthamoeba spp.] [Balamuthia mandrillaris] [Naegleria fowleri] [Sappinia spp.]
Casual Agents
Free-living amebae belonging to the genera Acanthamoeba, Balamuthia, Naegleria and Sappinia are rare causes of disease in humans and animals.
Acanthamoeba spp. and Balamuthia mandrillaris are free-living amebae capable of causing granulomatous amebic encephalitis (GAE). Acanthamoeba is an important cause of severe keratitis among contact lens wearers and may also cause cutaneous lesions, particularly in immunocompromised individuals. Because species level identification is not typically performed on Acanthamoeba cases, the full range of pathogenic species within the genus is not known, but species known to infect humans include A. byersi, A. castellanii, A. culbertsoni, A. hatchetti, A. healyi, A. astroonyxix, A. divionensis and A. polyphaga. B. mandrillaris may also occur in association with skin lesions. Naegleria fowleri produces an acute, and usually lethal, central nervous system (CNS) disease called primary amebic meningoencephalitis (PAM). Sappinia pedata has been implicated in one human case of amebic encephalitis.
Life Cycle
Acanthamoeba spp.
Acanthamoeba spp. are ubiquitous in the environment and have been found in a variety of sites, including soil; fresh, brackish, and sea water; field-grown vegetables; sewage; swimming pools; contact lens supplies; medicinal pools; dental treatment units; dialysis machines; heating, ventilating, and air conditioning systems; and tap water; mammalian cell cultures; and vegetables. Acanthamoeba has two stages; cysts  and trophozoites
and trophozoites  in its life cycle and lacks a flagellate stage. The trophozoites replicate by mitosis (nuclear membrane does not remain intact)
in its life cycle and lacks a flagellate stage. The trophozoites replicate by mitosis (nuclear membrane does not remain intact)  . The trophozoites are the infective forms, although both cysts and trophozoites can enter the body
. The trophozoites are the infective forms, although both cysts and trophozoites can enter the body  through various means. Entry can occur through the eye
through various means. Entry can occur through the eye  , the nasal passages to the lower respiratory tract
, the nasal passages to the lower respiratory tract  , or ulcerated or broken skin
, or ulcerated or broken skin  . When Acanthamoeba spp. enters the eye it can cause severe keratitis in otherwise healthy individuals, particularly contact lens users
. When Acanthamoeba spp. enters the eye it can cause severe keratitis in otherwise healthy individuals, particularly contact lens users  . When it enters the respiratory system or through the skin, it can invade the central nervous system by hematogenous dissemination causing granulomatous amebic encephalitis (GAE)
. When it enters the respiratory system or through the skin, it can invade the central nervous system by hematogenous dissemination causing granulomatous amebic encephalitis (GAE)  or disseminated disease
or disseminated disease  , or skin lesions
, or skin lesions  in individuals with compromised immune systems. Both Acanthamoeba spp. cysts and trophozoites are found in tissue.
in individuals with compromised immune systems. Both Acanthamoeba spp. cysts and trophozoites are found in tissue.
Balamuthia mandrillaris
Balamuthia mandrillaris has been isolated from soil and dust, and also from autopsy specimens of infected humans and animals. B. mandrillaris has two stages, cysts  and trophozoites
and trophozoites  in its life cycle and lacks a flagellate stage. The trophozoites replicate by mitosis (nuclear membrane does not remain intact)
in its life cycle and lacks a flagellate stage. The trophozoites replicate by mitosis (nuclear membrane does not remain intact)  . The trophozoites are the infective forms, although both cysts and trophozoites gain entry into the body
. The trophozoites are the infective forms, although both cysts and trophozoites gain entry into the body  through various means. Entry can occur through the nasal passages to the lower respiratory tract
through various means. Entry can occur through the nasal passages to the lower respiratory tract  , or ulcerated or broken skin
, or ulcerated or broken skin  . When B. mandrillaris enters the respiratory system or through the skin, it can invade the central nervous system by hematogenous dissemination causing granulomatous amebic encephalitis (GAE)
. When B. mandrillaris enters the respiratory system or through the skin, it can invade the central nervous system by hematogenous dissemination causing granulomatous amebic encephalitis (GAE)  or disseminated disease
or disseminated disease  , or skin lesions
, or skin lesions  . B. mandrillaris cysts and trophozoites are found in tissue; a few cases have been associated with solid organ transplantation from an infected donor.
. B. mandrillaris cysts and trophozoites are found in tissue; a few cases have been associated with solid organ transplantation from an infected donor.
Naegleria fowleri
Naegleria fowleri has three stages in its life cycle: cysts  , trophozoites
, trophozoites  , and flagellated forms
, and flagellated forms  . The trophozoites replicate by promitosis (nuclear membrane remains intact)
. The trophozoites replicate by promitosis (nuclear membrane remains intact)  . N. fowleri is found in fresh water, soil, thermal discharges of power plants, geothermal wells, and poorly-chlorinated recreational and tap water. Trophozoites can turn into temporary non-feeding flagellated forms which usually revert back to the trophozoite stage. Trophozoites infect humans or animals by penetrating the nasal mucosa, usually during swimming or sinus irrigation
. N. fowleri is found in fresh water, soil, thermal discharges of power plants, geothermal wells, and poorly-chlorinated recreational and tap water. Trophozoites can turn into temporary non-feeding flagellated forms which usually revert back to the trophozoite stage. Trophozoites infect humans or animals by penetrating the nasal mucosa, usually during swimming or sinus irrigation  , and migrating to the brain
, and migrating to the brain  via the olfactory nerves causing primary amebic meningoencephalitis (PAM). Naegleria fowleri trophozoites are found in cerebrospinal fluid (CSF) and tissue, while flagellated forms are occasionally found in CSF. Cysts are not seen in brain tissue.
via the olfactory nerves causing primary amebic meningoencephalitis (PAM). Naegleria fowleri trophozoites are found in cerebrospinal fluid (CSF) and tissue, while flagellated forms are occasionally found in CSF. Cysts are not seen in brain tissue.
Hosts
There is no major reservoir host as these ameba species are free-living in the environment and are only opportunistically parasitic. However, such infections have been documented in a variety of animal species.
Geographic Distribution
These amebae occur worldwide in water and soil; below is a summary of the locations where human infections are known to have occurred:
Acanthamoeba spp.: Acanthamoeba-associated keratitis occurs worldwide predominantly among contact lens users. Cases of Acanthamoeba-associated GAE have been reported broadly as well.
Balamuthia mandrillaris: Reports of B. mandrillaris infections primarily originate from the Americas, particularly Latin America, with limited cases reported from Asia, Australia, and Europe. In the United States, many cases have been reported from southwestern states. Many cases reported from Peru have involved the development of facial skin lesions.
Naegleria fowleri: Cases have been reported on all inhabited continents. Most cases in the United States have been associated with warm freshwater exposure in southern states. However, there have been cases reported from northern states in summer months.
The single reported case of infection with Sappinia pedata in a human was identified in Texas.
Clinical Presentation
Acanthamoeba spp.: Disseminated infection typically shows up as inflammation of the lungs or sinuses, and/or skin infections but has the potential to spread to the brain. GAE has a chronic onset that progressively worsens over a span of weeks to months. Signs and symptoms are typical of meningoencephalitis and encephalitis, and involve varying degrees of neurological impairment. There are very few known survivors of GAE.
Acanthamoeba keratitis is most commonly unilateral and individual ocular symptoms are variable. A characteristic circular stromal infiltrate may become apparent in the iris. Corneal ulceration and scarring can occur if not treated. Although highly associated with contact lens use, cases occurring in the absence of contact lenses have occurred.
Cutaneous acanthamebiasis presents as a single or disseminated chronic skin lesions, which are most commonly crusted or ulcerated, they may be indurated or have an eschar. Skin infections caused by Acanthamoeba can appear as reddish nodules, skin ulcers, or abscesses in the skin. The lesions may be mistaken for fungal or mycobacterial skin infection, cutaneous amebiasis caused by Entamoeba histolytica or cutaneous leishmaniasis. These may occur with or without concurrent central nervous system disease.
Balamuthia mandrillaris: Infection with B. mandrillaris involves a similar course to Acanthamoeba-associated GAE. The disease might appear mild at first but can become more severe over weeks to several months. Often the disease is fatal with a case fatality rate of more than 89%. Plaque-like skin lesions, most often on the face, particularly in the cheek or nose area, but sometimes on the torso or limbs may precede the development of neurological symptoms by weeks or months.
Naegleria fowleri: PAM is characterized by severe CNS dysfunction with rapid degeneration caused by hemorrhagic-necrotizing meningoencephalitis. Unlike GAE, the onset of PAM symptoms occurs quickly following infection (1-9 days; median 5 days after swimming or other nasal exposure to Naegleria-containing water). Symptoms are similar to bacterial meningitis, for which it is often mistaken, with deteriorating neurological function and complications. The case fatality rate is extremely high.
Acanthamoeba spp. cysts.
The cysts of Acanthamoeba spp. are typically 10—25 µm in diameter. The cysts have a two-layered wall with pores: a wrinkled fibrous outer wall (exocyst) and an inner wall (endocyst) that may be hexagonal, spherical, star-shaped or polygonal. Cysts contain only one nucleus with a large karyosome. Cysts may be found in the brain, eyes, skin, lungs and other organs.





Acanthamoeba spp. trophozoites.
Trophozoites of Acanthamoeba spp. are pleomorphic and measure approximately 15—45 µm. They often have multiple spine-like processes called acanthapodia. Trophozoites contain a large nucleus with a large, centrally-located karyosome but no peripheral chromatin. There is no flagellated trophozoite stage in Acanthamoeba spp.


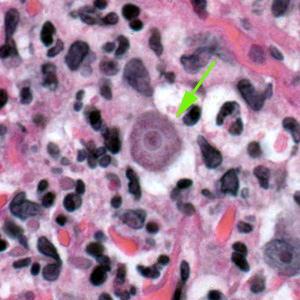

Balamuthia mandrillaris cysts.
The cysts of Balamuthia mandrillaris are highly similar morphologically to those of Acanthamoeba spp. and are also typically 10—25 µm (mean 15 µm) in diameter. Generally these cannot be reliably distinguished from Acanthamoeba spp. without either molecular confirmation or electron microscopy. The cysts have two walls apparent in light microscopy, and do not have pores: a wrinkled fibrous outer wall (exocyst) and an inner wall (endocyst) that may be variable in shape. A third layer (mesocyst) is only visible via electron microscopy. Cysts contain only one nucleus with a large karyosome. Cysts may be found in the brain, skin, lungs and other organs.









Balamuthia mandrillaris trophozoites.
Trophozoites of Balamuthia mandrillaris are pleomorphic and measure approximately 15—60 µm. They often produce long pseudopodia (broader than those of Acanthamoeba spp.). Trophozoites contain a large nucleus with a large, centrally-located karyosome but no peripheral chromatin. Binucleate forms are rare. There is no flagellated trophozoite stage in B. mandrillaris.







Naegleria fowleri cysts.
Naegleria fowleri does not form cysts in human tissue. Cysts in the environment and culture are spherical, 7-15 µm in diameter and have a smooth, single-layered wall. Cysts have a single nucleus.

Naegleria fowleri trophozoites.
There are two forms of trophozoites in Naegleria fowleri: ameboid and ameboflagellate, the latter of which is only rarely found in humans (within CSF). The ameboid trophozoites measure 10-35 µm but when rounded are usually 10—15 µm in diameter. In culture, trophozoites may grow to over 40 µm. The cytoplasm is granular and contains many vacuoles. The single nucleus is large and has a large, dense karyosome and lacks peripheral chromatin.





Sappinia spp. cysts and trophozoites.
Sappinia is a genus of free-living amebae rarely isolated from human specimens. The genus is found worldwide and has been isolated in the feces of many animals, including mammals and reptiles. Cysts and trophozoites both possess two nuclei.






Indirect immunofluorescence (IIF) assay for free-living amebic infections.





Gross pathology images in free-living amebic infections.


Laboratory Diagnosis
Acanthamoeba spp.: Acanthamoeba infection can be diagnosed by detection of trophozoites and cysts on microscopic examination of stained smears of biopsy specimens (brain tissue, skin, cornea) or of corneal scrapings. Lactophenol blue, acridine orange, silver, and calcofluor white stains have been used in the diagnosis of acanthamoebiasis on histologic sections and environmental samples (i.e. pelleted contact lens case contents). In granulomatous amebic encephalitis cases, trophozoites and cysts are only rarely found in the CSF. Acanthamoeba can be cultured from clinical and environmental samples in the laboratory on non-nutrient agar with a Page’s saline and Escherichia coli overlay.
Confocal microscopy or cultivation of the causal organism, and its identification by direct immunofluorescent antibody, may also prove useful. When there are large numbers of cysts and/or trophozoites, as in very severe cases, diagnosis may be possible through direct microscopy on corneal scrapings or contaminated surfaces (i.e. contact lens cases). An increasing number of PCR-based techniques (conventional and real-time PCR) have been described for detection and identification of free-living amebic infections in the clinical samples listed above. Such techniques may be available in selected reference diagnostic laboratories.
Balamuthia mandrillaris infection is generally diagnosed post-mortem. Outside of molecular detection via PCR and recently, metagenomic deep sequencing, B. mandrillaris is most reliably detected via immunofluorescence or immunoperoxidase staining of tissue samples.
For Naegleria fowleri infections, the diagnosis can be made by microscopic examination of cerebrospinal fluid (CSF). It may be possible to detect motile trophozoites on a wet mount, and a Giemsa-stained smear will show trophozoites with typical morphology. PCR may be used to detect evidence of N. fowleri in CSF and brain tissue. Amebic culture on non-nutrient agar plates overlaid with a fine lawn of Escherichia coli enhances the likelihood of detection by microscopic methods. (More on diagnosis of N. fowleri infections).
Real-Time PCR
A real-time PCR was developed at CDC for identification of Acanthamoeba spp., Naegleria fowleri, and Balamuthia mandrillaris in clinical samples.* This assay targets 18S small subunit ribosomal RNA gene sequences, and uses distinct primers and TaqMan probes for the simultaneous identification and differentiation of these three parasites.
Reference:
* Qvarnstrom Y, Visvesvara GS, Sriram R, da Silva AJ. Multiplex real-time PCR assay for simultaneous detection of Acanthamoeba spp., Balamuthia mandrillaris, and Naegleria fowleri. J Clin Microbiol 2006;44(10):3589-3595.
Laboratory Safety
Free living amebae could pose a potential safety risk to laboratory staff, particularly when large numbers are present in culture. Personal protective equipment (laboratory gown and gloves with eye protection) should be worn at all times, and other appropriate BSL-2 precautions should be taken. Individuals with immunosuppressive illnesses or open wounds in exposed areas of skin may be at greater risk of infection when working with cultures of free living amebae.
Suggested Reading
Naegleria fowleri: Siddiqui, R., Ali, I.K.M., Cope, J.R. and Khan, N.A., 2016. Biology and pathogenesis of Naegleria fowleri. Acta Tropica, 164, pp.375-394.
Further information and FAQ on Naegleria fowleri
Acanthamoeba spp.: Lorenzo-Morales, J., Khan, N.A. and Walochnik, J., 2015. An update on Acanthamoeba keratitis: diagnosis, pathogenesis and treatment. Parasite, 22.
Further information and FAQ on Acanthamoeba spp.
Balamuthia mandrillaris: Lorenzo-Morales, J., Cabello-Vílchez, A.M., Martín-Navarro, C.M., Martínez-Carretero, E., Piñero, J.E. and Valladares, B., 2013. Is Balamuthia mandrillaris a public health concern worldwide?. Trends in Parasitology, 29(10), pp.483-488.
Further information and FAQ on Balamuthia mandrillaris
Sappinia spp.: Walochnik, J., Wylezich, C. and Michel, R., 2010. The genus Sappinia: History, phylogeny and medical relevance. Experimental Parasitology, 126(1), pp.4-13.
Culture methodologies: Schuster, F.L., 2002. Cultivation of pathogenic and opportunistic free-living amebas. Clinical Microbiology Reviews, 15(3), pp.342-354.
DPDx is an educational resource designed for health professionals and laboratory scientists. For an overview including prevention, control, and treatment visit www.cdc.gov/parasites/.


