Mental Health
Technical Instructions for Physical or Mental Disorders with Associated Harmful Behaviors and Substance-Use Disorders for Panel Physicians
Preface
The purpose of the immigration examination is to identify health-related conditions that render an applicant inadmissible. Medical screening for physical and mental disorders with associated harmful behaviors and substance-related disorders among persons overseas applying for US immigration or refugee status and non-immigrants who are required by law to have an overseas medical examination, hereafter referred to as applicants, is therefore an essential component of the immigration process. Because such conditions are challenging to diagnose and treat, these Technical Instructions provide a method for recording findings from the medical examination and additional guidance for the panel physician in classifying applicants. The Technical Instructions use uniform criteria for diagnosis consistent with current medical knowledge, and classification connected with legal definitions.
The required examination includes evaluation of physical and mental disorders with associated harmful behaviors and substance use disorders. Inadmissibility based on a physical or mental disorder is limited to applicants with associated harmful behavior or potentially harmful behavior.
The Immigration and Nationality Act (INA) provides three grounds of inadmissibility related to substance addiction or abuse, or physical or mental disorders that affect behavior. They are:
- Current physical or mental disorder with associated harmful behavior.
- Current physical or mental disorder with a history of associated harmful behavior if the harmful behavior is likely to recur or lead to other harmful behavior in the future.
- Drug (substance) abuse or addiction (medically identified as a “substance use disorder”) of any of the substances listed in Section 202 of the Controlled Substances Act (Appendix C).
These Instructions are to be followed when determining whether an individual applicant is afflicted with physical and mental disorders with associated harmful behaviors and substance use disorders for all examinations performed. They reflect the current medical knowledge and standards of the American Psychiatric Association’s Diagnostic and Statistical Manual of Mental Disorders (DSM).
The DSM diagnosis for substance use disorders is used in this examination to determine “drug abuse” and “drug addiction.”
The instructions in this document supersede all previous Technical Instructions, updates to the Technical Instructions, memoranda and letters to panel physicians, and memoranda and letters to international refugee resettlement organizations.
For any questions about these Technical Instructions, please contact the Immigrant, Refugee, and Migrant Health Branch of the Division of Global Migration Health (DGMH), Centers for Disease Control and Prevention (CDC), at cdcQAP@cdc.gov or 404-498-1600. These Technical Instructions and other information pertinent to them and the medical examination for applicants for US immigration can be found online.
Key Concepts
Physical Disorder
Physical disorders are clinically diagnosed medical conditions where the focus of attention is physical manifestations. Only physical conditions that are included in the current version of the World Health Organization’s Manual of the International Classification of Diseases (ICD) will be considered for the purpose of this examination.
Mental Disorder
Mental disorders are health conditions that are characterized by alterations in thinking, mood, or behavior (or some combination thereof). The current version of the DSM is an authoritative source on the classification of mental disorders and must be available and followed for the purpose of this examination.
“V” Coded Condition
“V” coded conditions listed in the DSM are not diagnoses but are used in clinical practice settings when the focus of clinical attention is on a behavior that is not due to a mental disorder. Because these “V” conditions are not mental disorders, they cannot be used in determining if a person has an inadmissible (Class A) health-related condition, regardless of whether there is an associated harmful behavior. However, behaviors associated with “V” coded conditions might require treatment.
Categorization of Substances
For purposes of this evaluation, substances are divided into two groups:
- Controlled substances – includes any substance listed in Schedules I through V of Section 202 of the Controlled Substances Act. (See Appendix C.)
- Non-controlled substances – includes alcohol and all other substances.
Substances used for clinical care in medical practice are not prohibited. Prescription drugs taken in accordance with a prescription do not amount to a substance use disorder. However, misuse of prescription drugs could indicate a substance use disorder. If that is suspected, further investigation would require a full evaluation by the examining physician with particular attention to whether illicit drugs are being used, because use of illicit drugs is a risk factor for the abuse of prescribed, controlled substances.
Substance Use Disorders
To establish any substance use disorder diagnosis, the examining physician must document the pattern of use and behavioral, physical, and psychological effects associated with the use or cessation of that substance. Diagnoses of substance use disorders are to be made in accordance with existing medical standards as determined by the current edition of the DSM.
The essential feature of a substance use disorder is a cluster of cognitive, behavioral, and physiological symptoms indicating that the individual continues using the substance despite significant substance-related problems.
The DSM criteria for substance use disorders fit within overall groupings of impaired control, social impairment, risky use, and pharmacological criteria. There are 11 total criteria listed in the DSM.
Drug (substance) abuse or addiction (medically identified as a “substance use disorder”) for a controlled substance is listed as a medical ground of inadmissibility by the INA. Therefore, an applicant will be barred from admission if he or she:
- Uses a controlled substance
AND - Meets DSM criteria for a substance use disorder for that controlled substance
The DSM uses the following criteria to determine the severity of a substance use disorder:
- The presence of 2-3 symptoms (this suggests a mild substance use disorder)
- The presence of 4-5 symptoms (this suggests a moderate substance use disorder)
- The presence of 6 or more symptoms (this suggests a severe substance use disorder)
If an applicant’s substance use meets criteria for a substance use disorder of any severity, and involves a controlled substance, the applicant is considered Class A for drug abuse/addiction.
If an applicant’s substance use meets the criteria for a substance use disorder of any severity, but involves a non-controlled substance (e.g., alcohol), the panel physician should determine whether associated harmful behavior is present or if there is a history of associated harmful behavior that is judged likely to recur. If harmful behavior is present or is judged likely to recur, then the applicant is considered Class A for a physical or mental disorder. If the applicant does not have current harmful behavior or does not have a history of harmful behavior that is judged likely to recur, the applicant is considered Class B for a physical or mental disorder.
If an applicant’s substance use does not meet criteria for a substance use disorder, they are No Class.
Class A and Class B Medical Conditions
Class A medical conditions are inadmissible conditions and include the following:
- A current physical or mental disorder with associated harmful behavior
- A current physical or mental disorder with a history of associated harmful behavior, if the harmful behavior is likely to recur or to lead to other harmful behavior in the future
- Substance use disorder involving a controlled substance
- Substance use disorder involving a non-controlled substance with associated harmful behavior
- Substance use disorder involving a non-controlled substance with a history of associated harmful behavior, if the harmful behavior is likely to recur or to lead to other harmful behavior in the future
Class B medical conditions are not inadmissible medical conditions and include any physical or mental abnormality, disease, or disability serious in degree or nature amounting to a substantial departure from well-being. These include:
- A current physical or mental disorder without associated harmful behavior
- A current substance use disorder for a non-controlled substance without associated harmful behavior
- A physical or mental disorder with associated harmful behavior, that is now in sustained remission
- A substance use disorder for a controlled substance that is now in sustained remission
- A substance use disorder for a non-controlled substance with associated harmful behavior, that is now in sustained remission
Harmful Behavior
A harmful behavior is defined as an action associated with a mental or physical disorder that is causing or has caused any of the following:
- Serious psychological or physical injury to the applicant or to others (e.g., a suicide attempt or child abuse)
- A serious threat to health or safety (e.g., driving while intoxicated or verbally threatening to kill someone)
As part of the mental health evaluation, the panel physician is to identify any harmful behavior that is associated with an applicant’s physical or mental disorder.
Occasionally, there are cases where harmful behavior may primarily occur due to the applicant’s environment (e.g., an abusive household or the applicant lives in a region in which they are persecuted). These cases should be carefully evaluated on a case-by-case basis and an exception to the above definition of harmful behavior may be made, depending on the circumstances.
Another exception that may be considered is when individuals with significant intellectual disability may exhibit behaviors such as hitting, biting, and head-banging, as a means of expressing frustration. However, careful evaluation must be made to ensure that such repetitive behaviors are not done with intent to harm.
Once any associated harmful behavior has been identified, the panel physician must next make a determination regarding whether or not any harmful behavior associated with or caused by the disorder is current or in the past, and the likelihood of any past associated harmful behavior to recur, in order to provide basis for inadmissibility. Thus, for the purposes of these instructions, there are two categories of harmful behavior:
- Current harmful behavior and
- Prior harmful behavior
If the applicant presently is or in the past has engaged in harmful behavior associated with a physical or mental disorder, the panel physician must evaluate whether the harmful behavior is likely to recur. Many factors enter into this determination of classification, and the decision requires clinical judgment. In order to conclude that a past harmful behavior is unlikely to recur, at a minimum, the underlying physical or mental disorder must be either in remission or reliably controlled by medication or other effective treatment. As an additional guideline, when a mental or physical disorder has a favorable prognosis and is in remission or under control, but there was associated harmful behavior, if it has been 12 months since the harmful behavior occurred, the harmful behavior is considered less likely to recur. However, clinical judgement must be employed in determining if 12 months is enough time to make such a decision and it is possible that the panel physician may need longer than a 12-month period (See “Remission” section).
Disorders most commonly associated with harmful behavior include:
- Mood disorders that include major depression and bipolar disorders and can be associated with high rates of suicide and aggression.
- Anxiety disorders that include post-traumatic stress disorder, panic disorders, phobias, and anxiety disorders and can be associated with harmful behavior.
- Personality disorders that include antisocial, paranoid, and borderline personality disorders and can be associated with impulsive acts of violence.
- Sexual disorders that include paraphilia, which may lead to harmful behaviors like sexual assault, rape, etc.
- Schizophrenia and other psychotic disorders that can be associated with delusions, paranoia, suicide, and aggressive acts.
- Disorders usually first diagnosed in childhood that include intellectual disability and conduct disorder and are often associated with harmful behaviors. In addition, other cognitive disorders, such as dementia, can be associated with harmful behaviors. Cases such as these must be reviewed carefully, however, as some behaviors may be consistent with the actual disability or disorder and not intentionally harmful.
- Substance-related disorders that include substance dependence or abuse. For specific substances listed in Schedule I-V of Section 202 of the Controlled Substances Act (see Appendix C), no associated harmful behavior is required for the applicant to have a medically inadmissible condition based on substance abuse/dependence (please see above for the determination of substance abuse/dependence). The panel physician is reminded that for substances not listed in Schedule I-V such as alcohol, that abuse or dependence is evaluated as a mental disorder and determination of associated harmful behavior is required for applicant to have a medically inadmissible condition. With alcohol dependence or abuse there is often associated harmful behavior during periods of intoxication and withdrawal.
Physical disorders are rarely associated with harmful behavior. However, it may happen in delirious or confused states due to metabolic disturbances, hypoglycemia, some psychomotor epilepsies and in the aftermath of generalized seizure disorders.
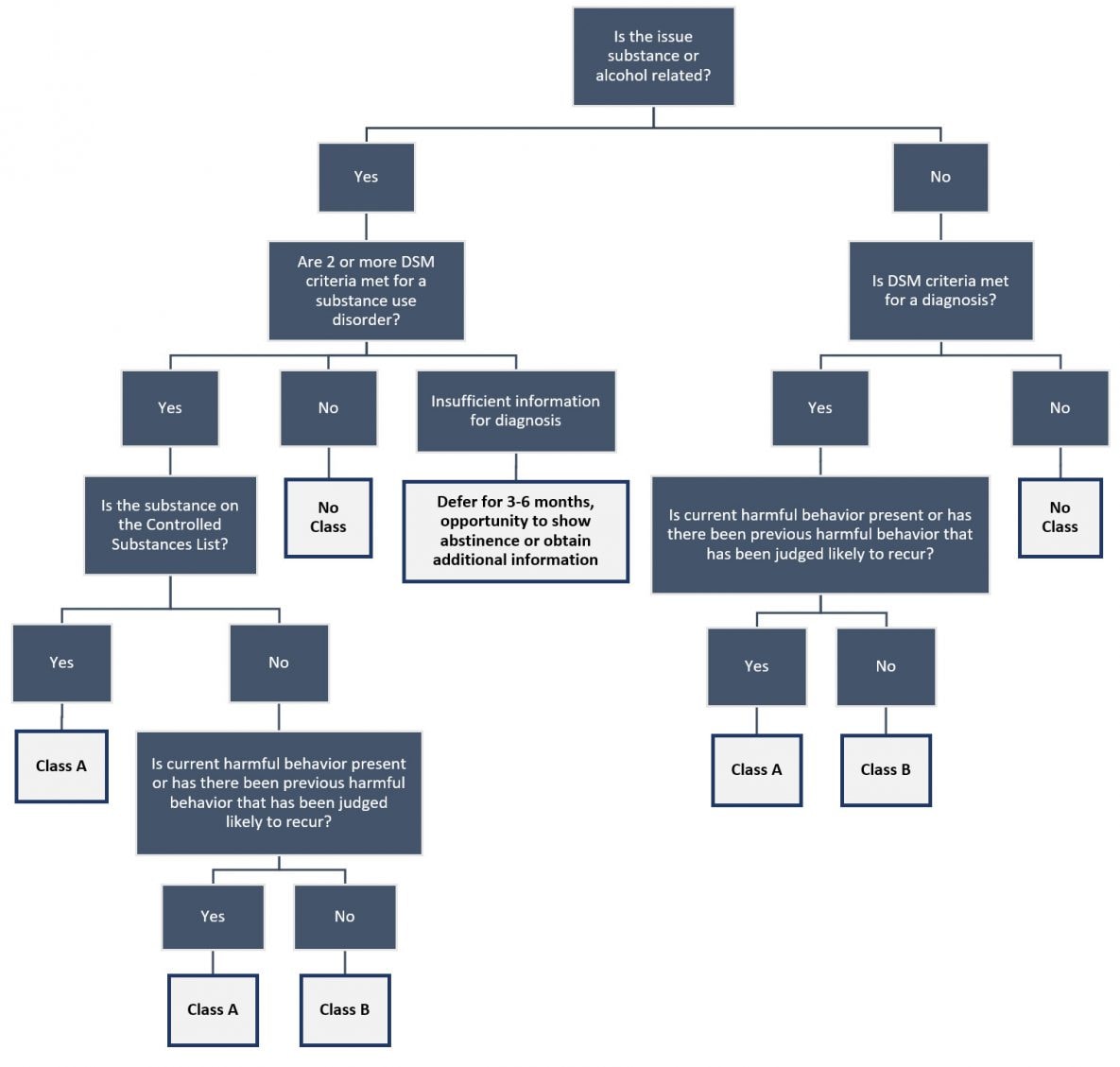
Because there are mental disorders that are commonly associated with harmful behavior, it may be helpful to first look for the harmful behavior when assessing an applicant for a possible mental disorder (See Figure 1). Due to the inherent complexity of this issue, the panel physician might feel that a more specialized psychiatric examination is indicated (Table 3).
Finally, it is important to note that people can have multiple harmful behaviors that are not associated with a physical or mental disorder, but that may render them inadmissible under criminal grounds as determined by DHS/USCIS. However, only harmful behavior that is associated with a physical or mental disorder is relevant for the classification of US medical eligibility; neither harmful behavior nor the physical or mental disorder by itself makes an applicant medically inadmissible.
Mental Health Examination
Overview
As part of the medical evaluation and physical examination of the applicant, the panel physician will carry out or obtain a mental health evaluation for the following purposes:
- To identify and diagnose any physical or mental disorder, including alcohol-related disorders
- To identify any harmful behavior associated with a disorder.
- To determine the likelihood of recurrence of prior harmful behaviors associated with a physical or mental disorder.
- To identify substance use disorders.
- To determine the remission status of any disorder previously diagnosed.
For most applicants, the panel physician’s examination will require only one appointment. However, for some applicants multiple appointments or consultations with a mental health specialist may be required to make an accurate diagnosis of whether the applicant is afflicted with a Class A or Class B condition as it relates to physical or mental disorders with associated harmful behavior or substance use disorders.
The panel physician can recognize that an applicant with a physical or mental disorder might have an associated harmful behavior during any point of the examination, including:
- While taking the medical history of a mental disorder
- While taking history of harmful behavior
- While observing for current abnormal behavior during the physical examination
Medical History
Observation alone is not sufficient to fully assess an applicant. Additionally, random screening for drugs is not part of the routine medical evaluation of applicants for U.S. and must not be performed without reason (see section on Laboratory Testing below for more information). Therefore, to fully investigate the applicant’s past medical history, the panel physician, when possible, should first do the following:
- Review the applicant’s Medical History and Physical Examination Worksheet (DS-3026) and available medical records.
- Obtain other relevant records, such as police, military, school, and employment, that might provide a history of harmful behavior associated with physical or mental disorders.
- Ask accompanying family members for information about the applicant regarding any social dysfunction, as well as any school, occupational or law enforcement problems.
- Ask about the applicant’s history of diagnosed mental or physical disorders.
- Ask about applicant’s use of drugs and medicines, both currently and in the past.
- Ask about harmful behaviors.
Psychiatric Evaluation
For applicants whose answers or history (in the Medical History section above) indicate the need to investigate further, the panel physician should conduct an activities assessment and mental status examination that assess, at a minimum:
- Orientation
- Mood and affect
- Speech and language
- Thought processes and content
- Behavior
The panel physician may estimate the degree of cognitive impairment in dementia or intellectual disability by assessing the applicant’s (1) level of knowledge and (2) ability to carry out functions of daily living (e.g., learning, communication, and routine activities).
Any available reports of cognitive, development, or intelligence testing, or neuropsychological testing in the medical record are welcome and should be included with the panel physician’s report. However, the panel physician is not asked to routinely send applicants for additional psychological tests.
Under most circumstances, the panel physician or mental health specialist will not need to provide additional psychological or neuropsychological testing. Use of projective instruments, such as Rorschach test, may not be useful given the added administrative and time burden involved. No psychological or neuropsychological testing is a substitute for the panel physician’s or a mental health specialist’s history and examination of the applicant. However, for certain cases, particularly when harmful behavior is present, these tests may aid in making a diagnosis.
Laboratory Testing
Random screening for drugs is not part of the routine medical examination for applicants for U.S. admission. The panel physician needs to evaluate the applicant’s history, behavior and physical appearance when determining if drug screening should be performed.
Whole populations of applicants must not be routinely subjected to random laboratory screening. The panel physician should make an individual decision based on the indications for drug screening. (See Table 1)
Laboratory testing to identify underlying medical conditions that might be causing psychiatric manifestations may be necessary before making any mental disorder diagnoses. However, specialized laboratory testing, such as dexamethasone suppression tests or challenge administration of various pharmaceuticals, is usually not indicated in the diagnosis of applicants.
Other possible uses of laboratory support depend on the availability of such laboratory services and the clinical judgment of the panel physician as to their usefulness in classification of the individual applicant. For example, therapeutic levels of prescribed anticonvulsant medications, antipsychotic medications, or other medicines used in psychiatry (such as lithium levels) might be of value to the panel physician in:
- Determining the applicant’s adherence to a prescribed course of treatment.
- Possibly changing or adjusting the applicant’s medications, and therefore contributing to remission of illness and reduction of associated harmful behavior.
Random screening for drugs on short notice to the applicant can provide additional evidence to aid in diagnosis and classification. For example, the panel physician might request that three random screenings for drugs within a 3- to 6-month period be done with only 24 to 48 hour notification to the applicant. The period of advance notification should be the minimum practical time for the applicant to arrive at the screening facility, preferably 24 or 48 hours after notification.
It is the panel physician’s responsibility to know the reliability and validity of the laboratory tests and laboratory methods used during the medical evaluation. All drug testing is to be done by using materials licensed by the US Food and Drug Administration or by the equivalent licensing office in other countries. Rapid testing or semi-quantitative testing may be used for the screening test; however, gas chromatography/mass spectrometry (GC/MS), performed at a reference laboratory, needs to be used as the confirmatory test. Positive and negative controls must be used with any testing and only test kits that are for medical diagnosis and treatment must be used. Forensic testing is minimally regulated and will be labeled “not for medical diagnosis and treatment” and, therefore, should not be used because it is not sensitive enough for medical purposes.
Deferring a Diagnosis/Classification
If the panel physician is unable to determine whether an applicant has a diagnosis of a physical or mental disorder, or substance use disorder for a substance listed in Section 202 of the Controlled Substances Act, the panel physician may defer diagnosis and classification in order to obtain additional medical evidence.
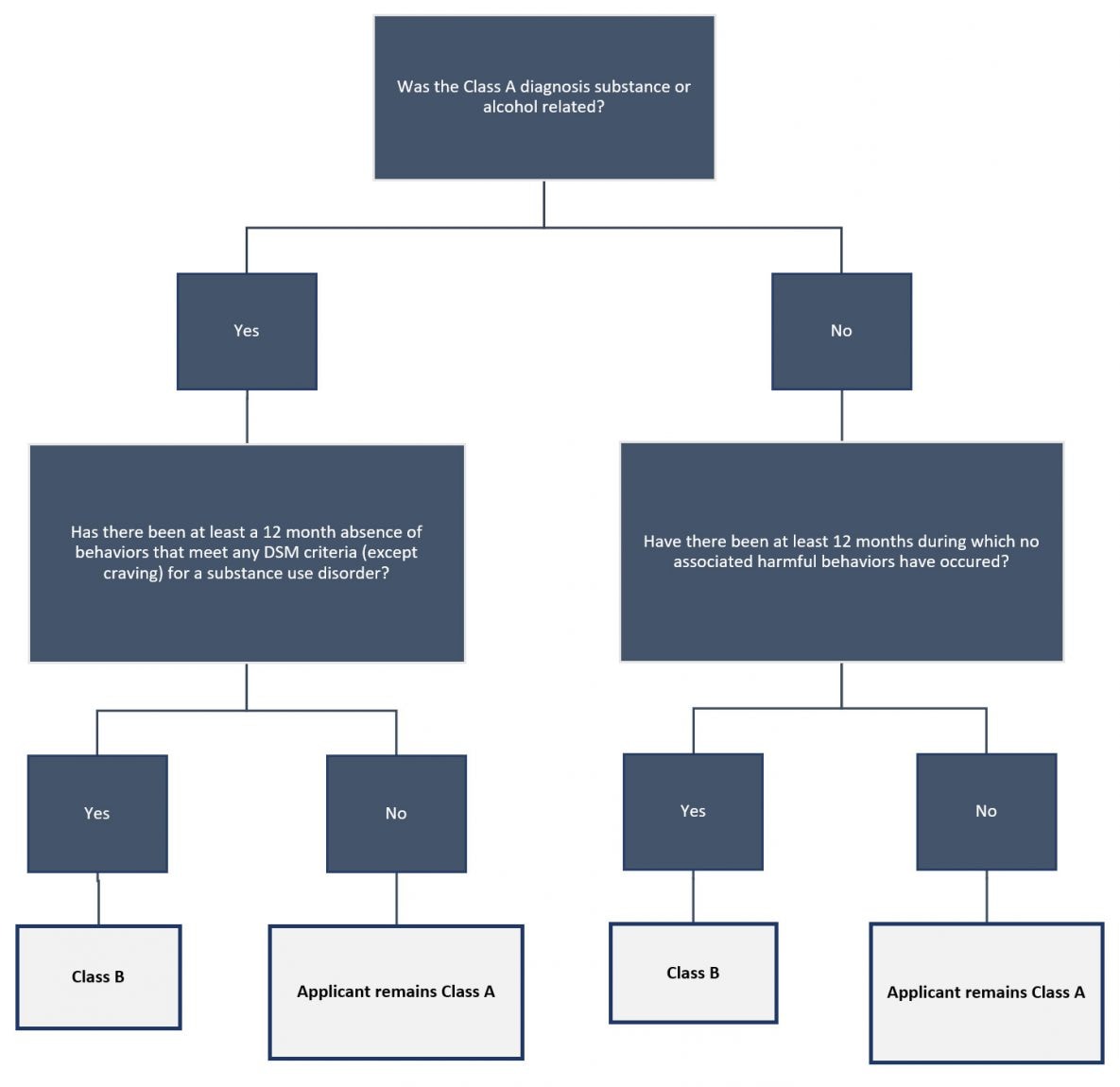
For applicants with deferred diagnosis and classification, the panel physician must have medical rationale for the deferral and must explain to the applicant what is required during the next 3 to 6 months (see Figure 2) in order for the panel physician to be able to diagnose and classify. Additionally, the panel physician should consider documenting in a statement signed by the applicant the information he or she is providing to the applicant.
Referring the Applicant to a Specialist for Psychiatric Examination
Referral to a mental health specialist is not a requirement for this examination. However, after reviewing the applicant’s medical history and other available records (such as medical, psychiatric, police, military, school, and employment) and performing mental status and physical examinations (including an activities assessment and mental status assessment), the panel physician might feel that a more specialized psychiatric examination is indicated (See Table 3). In these cases, the panel physician should have a mental health specialist previously identified who can carry out a full psychiatric evaluation upon request by the panel physician.
If an applicant has been referred to a mental health specialist for psychiatric evaluation and the panel physician still needs guidance and assistance in determining the diagnosis and classification of a Class A or Class B or No Class A or Class B condition, DGMH may be consulted to provide additional assistance.
Please note that the panel physician should only consult DGMH in situations where, after their own examination and/or evaluation by a mental health specialist, they are still unable to make a final determination on diagnosis or classification. DGMH should not be consulted to make routine determinations on diagnoses or classifications that are straight forward and easily finalized by the panel physician.
To submit a case to DGMH for review, a copy of the all pertinent medical information may be sent via secure files to cdcQAP@cdc.gov.
Remission
The current version of the DSM defines sustained remission as a period of at least 12 months during which no substance use or mental disorder-associated behaviors have occurred, with the exception of craving in the case of substance use disorders. The panel physician and his or her mental health specialist must use their clinical judgment in determining if 12 months is an acceptable period of time for the applicant to demonstrate sustained remission. This time period must be based on the reliability of the evidence provided, such as clinical reports or participation in a program.
Remission must also be considered in two contexts:
- General mental disorders
- Substance use disorders
For general mental disorders, the determination of remission must be made based on the assessment of associated harmful behavior, either current or prior that is judged likely to recur, and DSM criteria. The disorder must be under control either by medication or natural history of the disorder, and the recurrence of specific life events or circumstances that precipitated the episode(s) must be unlikely to recur (see Table 2).
For substance use disorders – including those for non-controlled substances, such as alcohol – the determination of remission must be made based on applicant’s substance use and DSM criteria. There must be no use of the substance in question other than indicated medical treatment, and at least 12 months during which the applicant does not meet any of the criteria for a substance use disorder, with the exception of craving. It is important to note that while a substance use disorder for a non-controlled substance (e.g., alcohol) does not itself render an applicant inadmissible, achieving sustained remission from the disorder is necessary in order for there to be clinical confidence that a prior associated harmful behavior is not likely to recur.
When an applicant is diagnosed with a Class A condition, panel physicians must explain clearly what is expected in order for them to meet criteria for remission. If treatment is indicated, panel physicians should also provide information regarding recommended treatment options.
Applicants who are or who have been determined to be Class A for a substance use disorder for a controlled substance are not eligible for a waiver (see “Waivers” section below for more information) and therefore, must complete the required time period for sustained remission before reapplying for admission.
Additional Concepts to Consider
Alcohol
Alcohol is not a controlled substance and, therefore, for classification purposes, an alcohol use disorder is treated like a physical or mental disorder. This means that an alcohol-use disorder must have associated harmful behavior present in order to be a Class A condition. However, in regards to remission, alcohol use disorders are treated the same as all other substance use disorders, meaning an applicant must meet the specific criteria for remission as defined in the DSM in order to overcome a Class A designation. Specifically, the determination of remission from an alcohol use disorder should not be based on the likelihood of recurrence of past harmful behaviors, but rather a 12-month absence of behaviors that meet any DSM criteria (except craving) for a substance use disorder.
Sexually Dangerous People
Not all sexually dangerous people have behaviors attributable to a psychiatric or general medical disorder. For instance, rapist is not a psychiatric diagnosis. However, people diagnosed with paraphilias might commit rape when their intense sexual fantasy, urge, or fetish is enacted with a child or other non-consenting person. People who have harmful behaviors associated with sexual acts, whether reported as a criminal act or psychiatric disorder, have been shown not to benefit reliably from treatment programs. Documented or acknowledged episodes of paraphilia might represent only a fraction of the sexually dangerous person’s history of related harmful behaviors. Harmful behaviors also include the viewing of child pornography because a child (children) is at least indirectly harmed during the making of such imagery, or directly harmed at worst. Given the pattern of recurring harmful behaviors in paraphilia and the high relapse rate of sexual offenders, applicants with a history of harmful behavior associated with sexual acts are almost always likely to have a recurrence of harmful behavior and therefore remain medically classifiable as a Class A mental disorder with associated harmful behavior for the remainder of their lives.
Cannabis and CBD
According to Appendix C — Section 202 of the United States Controlled Substances Act, marijuana and all of its components and derivatives, including delta-9-tetrahydrocannabinol (THC) and cannabidiol (CBD) > 0.3%, are considered Schedule I controlled substances. Schedule I controlled substances are considered by the United States Drug Enforcement Agency (DEA) to be drugs or substances with high potential for abuse and having no currently accepted medical use in the United States.
Because several state governments have legalized marijuana or some of its derivatives, including derivatives with > 0.3% THC, there has been great confusion as to the legality of the use of such products. Local or online advertisements for CBD and/or other cannabis derivatives may be prominent at times, but the US Food and Drug Administration states it is currently illegal to market CBD by adding it to a food or labeling it as a dietary supplement.
Therefore, at this time, applicants who meet criteria for cannabis use disorder with the use of cannabis and/or any of its derivatives, including CBD or THC, are inadmissible and must be in sustained remission in order to be classified as Class B for travel clearance purposes.
Mental Health Screening Results and Travel Clearance
The mental health screening is complete when all required aspects of the medical examination have been finalized, including the report of the specialist and laboratory test results, if indicated. At this time, the panel physician should be able to assign to the applicant a classification regarding a physical or mental disorder or substance related disorder.
Travel clearances for the evaluation regarding physical or mental disorders or substance use disorders are valid for the same length of time as the overall examination validity. Applicants who do not travel within the examination validity period will need to restart the mental health screening process at the same time that they restart the rest of the examination.
Applicants may have more than one classification. However, applicants cannot be classified as both Class A and Class B for the same physical or mental disorder, or substance related disorder.
Mental Health and Substance Abuse/Addiction Classifications and Descriptions
No Class A or Class B Classification
- Applicants with no diagnosis of physical or mental disorder.
- Applicants with incidental use of a substance, but who do not meet criteria for substance use disorder.
- Applicants with harmful behavior that is not associated with any diagnosable physical or mental disorder, or substance use disorder.
Class A Physical or Mental Disorder with Associated Harmful Behavior
- Applicants diagnosed with current physical or mental disorder based on current DSM criteria with associated harmful behavior.
- Applicants diagnosed with current physical or mental disorder based on current DSM criteria with history of associated harmful behavior judged likely to recur.
- Applicants diagnosed with a substance use disorder for a substance NOT provided in Schedule I-V of Section 202 of the Controlled Substances Act, based on current DSM criteria with associated harmful behavior.
- Applicants diagnosed with a substance use disorder for a substance NOT provided in Schedule I-V of Section 202 of the Controlled Substances Act, based on current DSM criteria with history of associated harmful behavior judged likely to recur.
Class A Substance Abuse or Dependence for Specific Substances provided in Schedule I-V of Section 202 of the Controlled Substances Act
- Applicants diagnosed with a substance use disorder for a substance provided in Schedule I-V of Section 202 of the Controlled Substances Act, based on current DSM criteria.
Class B Physical or Mental Disorder with No Associated Harmful Behavior
- Applicants diagnosed with current physical or mental disorder based on current DSM criteria with no associated harmful behavior.
Class B Physical or Mental Disorder with History of Associated Harmful Behavior Unlikely to Recur
- Applicants diagnosed with physical or mental disorder (including substance use disorders for non-controlled substances, such as alcohol) based on current DSM criteria with history of associated harmful behavior judged unlikely to recur.
Class B Substance Abuse or Dependence in Full Remission
- Applicants diagnosed with substance use disorder for a controlled substance based on current DSM criteria who now meet criteria for sustained remission.
DSM Diagnoses and Classifications
| DSM Diagnosis | Involving Controlled Substance? | Associated Harmful Behavior (Current, or Likely to Recur)? | Meets Criteria for Sustained Remission? | Classification for Immigration Purposes |
|---|---|---|---|---|
| No Diagnosis (does not meet DSM criteria) | Yes or No | N/A – does not apply | N/A – does not apply | No Class |
| Substance Use Disorder (mild, moderate, or severe) |
Yes | N/A – does not apply | No | Class A, Addiction or abuse of a specific substance on the CSA |
| Yes | Class B, Sustained, full remission of addiction or abuse of specific substance on the CSA | |||
| No | Yes | No | Class A, Any physical or mental disorder (including other substance-related disorder) with harmful behavior or history of such behavior likely to recur | |
| Yes | Class B, Any physical or mental disorder (excluding addiction or abuse of specific substance on the CSA but including other substance-related disorder) without harmful behavior or history of such behavior unlikely to recur | |||
| No | N/A – does not apply | Class B, Any physical or mental disorder (excluding addiction or abuse of specific substance on the CSA but including other substance-related disorder) without harmful behavior or history of such behavior unlikely to recur | ||
| Mental or Physical Disorder
|
N/A – does not apply | Yes | No | Class A, Any physical or mental disorder (including other substance-related disorder) with harmful behavior or history of such behavior likely to recur |
| Yes | Class B, Any physical or mental disorder (excluding addiction or abuse of specific substance on the CSA but including other substance-related disorder) without harmful behavior or history of such behavior unlikely to recur | |||
| No | N/A – does not apply | Class B, Any physical or mental disorder (excluding addiction or abuse of specific substance on the CSA but including other substance-related disorder) without harmful behavior or history of such behavior unlikely to recur |
Waivers
A provision allows applicants with a Class A physical disorder or mental disorder with associated harmful behavior to petition for a Class A waiver. Form I-601 or I-602 (for immigrants or refugees, respectively) must be completed. These waivers are submitted to the Department of Homeland Security (DHS), U.S. Citizenship and Immigration Services (USCIS) on an individual basis. After submission, DGMH reviews the waivers and supporting medical examination upon request by USCIS to provide an opinion regarding the case. DGMH’s review of the waiver and supporting medical examination documentation is to ensure that the applicant has been classified properly and that an appropriate U.S. health care provider is identified for the applicant for continued treatment post arrival. However, USCIS has the final authority to adjudicate the waiver request.
Immigrant visa applicants diagnosed with substance use disorders for controlled substances are not eligible for a waiver. However, under section 207 of the INA, the DHS may waive this provision if the applicant is seeking admission to the U.S. as a refugee.
Documentation
Pertinent information relating to physical or mental disorders, and substance related disorders should be indicated on the DS-3026 or in the 106 Mental Health Report in eMedical.
Department of State forms DS-2054, DS-3025, DS-3026, and DS-3030 or the 106 Mental Health Report in eMedical must be completed in their entirety and included in the applicant’s travel packet. This includes assigning a classification on the DS-2054 if an applicant is Class A or Class B for a physical or mental disorder or substance related disorder. Incomplete documentation may result in refusal to grant a visa or designation of medical hold status at arrival to ports of entry.
For applicants that are referred to a mental health specialist for further evaluation, the panel physician is required to attach the original specialist’s report to the DS forms or upload to eMedical.
For applicants that are referred for psychological or laboratory testing, the panel physician is required to attach the original of all testing results to the DS forms or upload to eMedical.
The report of the specialist and all testing results must be provided in English.
Any other documents provided for review regarding the diagnosis or classification of a physical or mental disorder, or substance related disorder for an applicant should be attached to the DS forms or uploaded to the eMedical record by the panel physician. All applicants with Class A conditions for physical or mental disorders, and substance related disorders should be reported to the US Embassy upon detection.
APPENDICES:
APPENDIX A: GLOSSARY OF ABBREVIATIONS
| Acronym | Full Phrase |
|---|---|
| CDC | Centers for Disease Control and Prevention, United States |
| DGMH | Division of Global Migration Health |
| DHS | Department of Homeland Security |
| DOS | Department of State |
| DSM | Diagnostic and Statistical Manual of Mental Disorders |
| FDA | Food and Drug Administration |
| ICD | Manual of the International Classification of Diseases |
| WHO | World Health Organization |
APPENDIX B: USEFUL RESOURCES
American Psychiatric Association: Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition. World Health Organization: Manual of the International Classification of Diseases.
APPENDIX C: CONTROLLED SUBSTANCES
Schedules I through V of Section 202 of the Controlled Substances Act. Found in Part 1308 of Title 21 Code of Federal Regulations.
FIGURES:
Figure 1. Classification Algorithm for Suspected Substance Use Disorder, or Physical or Mental Disorder
alternative text for web accessible infographic
Figure 2. Classification Algorithm for Evaluating Remission after a Class A Determination:
Include (but are not limited to) –
- History of any substance abuse or dependence with a specific substance listed in Schedules I through V of Section 202 of the Controlled Substances Act. (See Appendix C)
- Applicant-provided information that appears to contradict information provided by family members or from other records such as police military school and employment
- Unexplained gaps of time in the applicant’s past schooling or employment.
- Evidence of unreliable or false information given during the interview or examination.
- Any demeanor, presentation, or findings that the examining physician associates with substance abuse or dependence, such as motor ability and interpersonal skills; deepened skin coloring, needle scarring, or skin ulcers along the veins in the arms or legs; or a hard, bumpy, or shrunken liver.
- Evidence or appearance of intoxication with any substance during the examination. Disturbed behavior that might be associated with a substance-related disorder.
- Follow-up of an initial positive drug screen or a history of a positive drug-screening test.
Include (but are not limited to) –
- The availability of effective treatments.
- The applicant’s faithfulness with previous treatment, willingness to remain on treatment, and his or her insight into disorder. He or she stating in writing a willingness to continue medication or other effective treatment to control the disorder can help demonstrate this.
- The natural history of the disorder (for instance, bipolar mood disorders without ongoing treatment are characterized by multiple episodes of illness and remission).
- The number of and interval between previous episodes of illness (for instance, episodes of schizophrenia with prominent psychotic symptoms were 3 years apart at the beginning of the illness but are now happening every year).
- Any trend towards increasing severity of episodes of illness or emergence of treatment-resistant symptoms.
- The likelihood of recurrence of specific life events that precipitated previous episodes of illness or likelihood of severe life stresses that might precipitate further episodes of illness (for instance, postpartum depression in a young woman).
- Unusual circumstances that precipitated a single episode of illness judged unlikely to recur.
The Panel Physician may refer the applicant to a mental health specialist if after interview, review of records, and examination, he or she is unable to –
- Arrive at a probable psychiatric diagnosis for purposes of the determination of a mental disorder with associated harmful behavior (past or present)
- Arrive at a probable diagnosis of substance-related disorder according to DSM criteria.
- Arrive at a probable diagnosis for past episodes of mental disorder according to current DSM criteria, or determine that previous difficulties in functioning were the result of a mental disorder.
- Rule out the presence of a mental disorder that may be associated with harmful behavior.
- Determine if harmful behavior has been associated with a physical or mental disorder.
- Determine if any prior associated harmful behavior is likely to recur.
- Determine if any diagnosed physical or mental disorders that affect behavior are in remission or under control.
- Determine the likelihood of maintaining remission or effective control of diagnosed physical or mental disorders that affect behavior.