
Case #298 – April, 2011
A 41-year-old woman presented to her health care provider with ulcerative lesions on her left ear and neck. Travel history included an excursion along the Amazon River in Brazil four months prior. She also reported numerous insect bites during her trip. The woman was referred to an infectious disease doctor who obtained a biopsy specimen from the largest lesion. The specimen was sent to Pathology where it was sectioned and stained with Giemsa. Figures A and B show what was observed at 1000x magnification. What is your diagnosis? Based on what criteria? What, if any, other testing would you recommend?
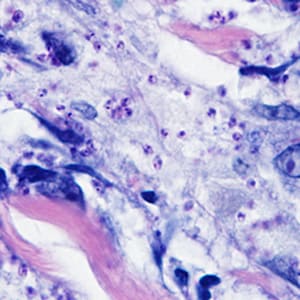
Figure A
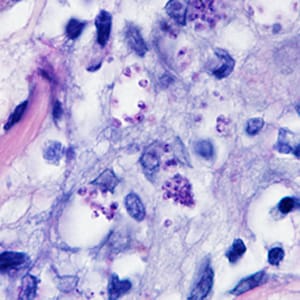
Figure B
Images presented in the DPDx case studies are from specimens submitted for diagnosis or archiving. On rare occasions, clinical histories given may be partly fictitious.
DPDx is an educational resource designed for health professionals and laboratory scientists. For an overview including prevention, control, and treatment visit www.cdc.gov/parasites/.