Public Health Grand Rounds
Public Health Grand Rounds (PHGR) will continue to promote Preventive Medicine Grand Rounds (PMGR) while our monthly PHGR sessions are on hold. We welcome your questions. Please email us at grandrounds@cdc.gov.

Preventive Medicine – A Necessary Field of Medicine
What is a preventive medicine trained physician and why are they important or relevant for today’s physician population?
Ms. Grande, American College of Preventive Medicine (ACPM) CEO, will share data and insights on the field of preventive medicine—what the training requirements are, what differentiates a preventive medicine physician from other specialties of medicine, and why they are relevant and important for today’s public health workforce.
Presenters
Donna Grande, MGA
Chief Executive Officer
American College of Preventive Medicine
Washington, DC
Presentation Details
- June 7, 2023, 1:30 – 3:00 p.m. ET
- Remote participation only through Zoom
Passcode: PMGR_0607 (if asked) - The link will go live at time of the event. No registration is needed.
For More Information
Please contact the PMR/F program at prevmed@cdc.gov or visit the Preventive Medicine Grand Rounds web page.

Originally presented on Tuesday, March 19, 2019
Suicide is a leading cause of death in the US and suicide rates have increased more than 30 percent since 2000. Among American Indian and Alaska Native (AI and AN) communities, suicide rates are even higher than among the general population, and they are highest among youth and young adults, ages 15–34. Focusing on subgroups at risk, including youth among AI and AN communities, and implementing evidence-based prevention strategies is a key approach to reducing suicidal behaviors and may help reduce this health inequity.
Listen to our latest podcast on suicide prevention from someone who has lived experience and watch our encore presentation on Preventing Suicidal Behavior in American Indian and Alaska Native Communities.

Originally presented on Tuesday, November 14, 2017.
Women in the US are more likely to die from childbirth or pregnancy-related causes than other women in high-income countries. Research suggests that half of these deaths may be preventable but more evidence is needed. Learn how racial disparities persist and about CDC’s collaborations to prevent these deaths.

Acute flaccid myelitis (AFM) is an uncommon but serious neurologic condition. It affects the nervous system and causes the muscles and reflexes in the body to become weak. Most AFM cases have been in young children. Cases have been increasing every other year in the US since 2014.

The June session of Grand Rounds, “Smoking Cessation: Past, Present, and Future” was viewed in 7 foreign countries, 49 states, and the District of Columbia.
Special note: The surgeon general of the United States, Vice Admiral Jerome Adams, will introduce this special Grand Rounds via Zoom.
Public Health Grand Rounds will present key findings on the recently released US Surgeon General’s report on Smoking Cessation. Smoking remains the leading preventable cause of death and disease in the United States. Although the percentage of adults who smoke is at an all-time low in the US, 34 million adults still smoke and therefore continue to be at risk of developing smoking-related diseases.
The 2020 Surgeon General’s report is the first to focus solely on smoking cessation since 1990. Grand Rounds speakers will discuss progress on smoking cessation made over the past decades, such as clinical treatments and tools that increase the chances of success. Presenters will also give updates on the health benefits of quitting smoking and what strategies work best to help people quit smoking for good.
- Frequently Asked Questions
- Please contact us with any questions or comments at grandrounds@cdc.gov
Suicide is a leading cause of death in the US and suicide rates have increased more than 30 percent since 2000.
Social_round_govd
Registration is not required to watch the live webcast of Grand Rounds. The course code is PHGR10.
For more information regarding the following, please visit the Grand Rounds Continuing Education page.
- Continuing Education Accreditation statements
- Disclosure
- Instructions for receiving continuing education
For issues regarding obtaining continuing education credits, please email ce@cdc.gov.
See All Topics

The Advanced Molecular Detection (AMD) Program, established by Congress in 2013, has led the adaptation and deployment of novel laboratory technologies, namely next-generation sequencing and bioinformatics, in the US public health system. AMD technologies are now in use across the range of infectious diseases of public health importance, such as bacterial foodborne illness, tuberculosis, influenza, malaria and Legionnaires’ disease. This session of Public Health Grand Rounds addresses the rapid advances in AMD, how these technologies are being applied in public health, and their future uses.
CDC is leading a national genomics consortium to help coordinate SARS-CoV-2 sequencing in labs across the US. Large-scale, rapid genomic sequencing of the virus that causes COVID-19 will allow public health experts to:
- Monitor important changes in the virus as it continues to circulate.
- Gain important insights to support contact tracing.
- Provide crucial information to aid in identifying diagnostic and therapeutic targets.
- Advance public health research in the areas of transmission dynamics, host response, and evolution of the virus.
Listen to our new Beyond the Data podcast and find out how labs can monitor changes in the virus and provide diagnostic and potential treatment information.
A Glossary for Advanced Molecular Detection and Pathogen Genomics [DOC – 17 KB]

Diabetes is a serious public health problem. About 34 million Americans have diabetes, and more than 88 million American adults have prediabetes. People with prediabetes have blood sugar levels that are higher than normal, but not high enough to be diagnosed with type 2 diabetes. They are at risk for type 2 diabetes, heart attack and stroke, but lifestyle changes, such as losing weight and increasing physical activity, can reduce their risk and may even prevent the onset of type 2 diabetes.
Learn how participating in the CDC-led National Diabetes Prevention Program lifestyle change program can help prevent or delay type 2 diabetes in those at high risk.
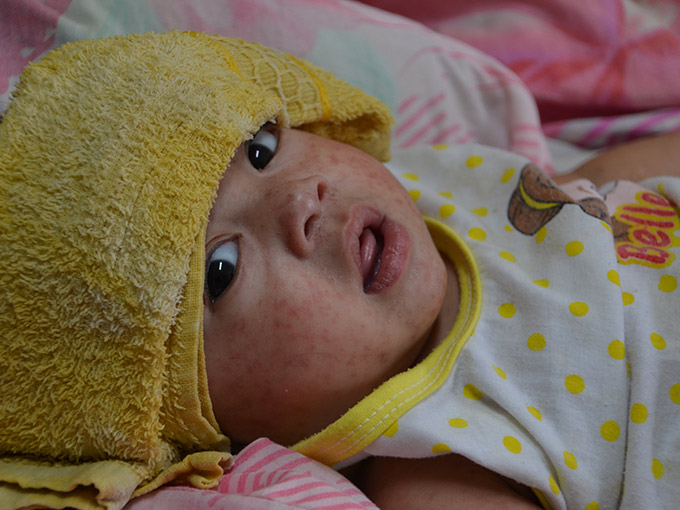
Last year marked the highest number of measles cases in a single year in the United States since 1992, with a total of 1,282 confirmed cases. More than 73% of these cases were linked to outbreaks in New York, affecting under-vaccinated communities. Measles was declared eliminated in the United States in 2000; however, the sustained transmission of almost 12 months nearly led to the loss of our elimination status.

Dr. John Iskander recaps our excellent 2019 Grand Rounds season and announces our new “Beyond the Data” podcast debuting in January 2020. Watch any of these sessions to earn free CE credit.
There is no live session for December.

The November session of Grand Rounds, “PFAS and Protecting Your Health,” was viewed in 3 foreign countries and 41 states, the District of Columbia, and the US Virgin Islands
Human exposure to PFAS (per- and polyfluoroalkyl substances) is a growing public health concern. PFAS are a large group of human-made chemicals that have been used in industry and consumer products worldwide since the 1950s. These chemicals are in food packaging and many other household products, and have been found in the air, soil, and water.

Approximately 6.5 million people in the United States have an intellectual disability (ID). It is the most common developmental disability. Yet, people with intellectual disabilities report difficulty finding appropriately trained and willing healthcare providers.

Pregnant women should routinely receive the Tdap (pertussis) vaccine and the influenza (flu) vaccine, as recommended by the Centers for Disease Control and Prevention (CDC). These vaccines have been shown to provide significant benefits to mother and baby.
CDC Public Health Grand Rounds is a monthly scientific presentation featuring the important work that CDC is doing in the United States and around the world to protect people and save lives. Experts discuss major public health issues, key challenges, cutting-edge scientific evidence, potential solutions, and recent developments. Each session is the result of a rigorous process which takes months to prepare. This attention to detail ensures that our audiences receive up-to-date, scientifically accurate, and usable information. Grand Rounds welcomes clinicians, researchers, students of public health, medicine and nursing, and the public that we serve to attend in person or watch the live webcast. Did you miss the live session? No worries! We invite you to watch Grand Rounds on our “On Demand” page where we archive each session for your convenience. Free Continuing Education is available for most topics.





