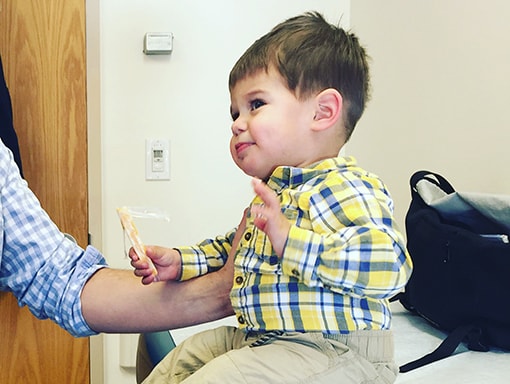
Noah’s Story
When he was 6 months old, Noah developed AFM and paralysis spread quickly through his body. Through treatment and therapy, Noah has made great progress. Today, he’s a happy, active 6-year-old, living in Amesbury Massachusetts, with his parents Elisa and Mitch.


In September 2014, Noah kept catching colds, but his symptoms weren’t out of the ordinary so his pediatrician wasn’t concerned. Then on the morning of Friday, October 3, Elisa set Noah down on the bed after nursing, and he fell backwards on the bed. She sat him up again, and he fell right back down. She remembers Noah’s legs looked floppy, like butterflies. Elisa pinched his toes, and Noah had no reaction. She called Noah’s pediatrician, who told her to take him to a nearby hospital.
At the ER, the doctor couldn’t identify what was causing the problem and recommended transferring Noah to a children’s hospital in Boston immediately, so he could be treated by specialists. Elisa believes that decision saved Noah’s life. An ambulance brought Noah and his parents to Boston, where doctors took some blood, ordered an MRI, and performed a spinal tap. They could see Noah’s shoulders, arms, and fingers were also getting weak. Looking at test results, they suspected Noah either had some type of myelitis or Guillain-Barre syndrome. They started treatment with steroids and intravenous immunoglobulin (IVIG).
The next day, doctors did another MRI, which confirmed Noah had AFM. Noah had an allergic reaction to the first IVIG, so they tried a different immunoglobulin product that worked well. Doctors continued with steroid treatments. At this point Noah’s face had started to droop, and he couldn’t hold his head up. Doctors performed a nasogastric (NG) intubation, so they could feed him through a tube running from his nose to his stomach.
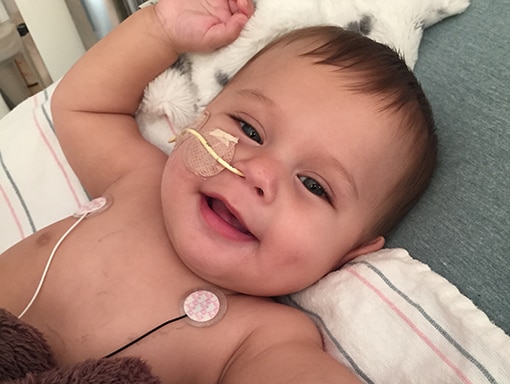
After 8 days in the hospital, doctors had stabilized Noah and were able to remove the NG tube. He was also able to twitch his toes and wiggle his arms. With this progress, the doctors decided it was time for Noah to go home. They didn’t recommend bringing him to a rehab facility, because there wasn’t anything therapists could do there that couldn’t be done at in outpatient therapy and at home.
A physical therapist started working with Noah, initially once a week, then twice a week, and then 3 times a week. Noah also began occupational therapy, pool therapy, hippotherapy, and music therapy. Elisa and Mitch learned about an AFM specialist in Dallas, Texas, and started making annual trips to see him. The specialist reviews Noah’s progress and recommends specific protocols for his therapy team.
Physical therapy was initially all about play—like encouraging Noah to move to get a toy. He moved on to a mobile stander and a small treadmill, and today he completes simple obstacle courses. Noah enjoys army crawling the most and says the hardest part of therapy is “mostly listening.” Elisa and Mitch say one of the biggest struggles has been getting the insurance company to cover Noah’s therapy.

Since being diagnosed with AFM, Noah’s symptoms have gotten worse twice. Both times happened while he was fighting off viral infections. He was able to get back to his baseline in a few weeks each time, but his entire AFM experience has caused Noah a lot of anxiety. “Some days I get anxious and some days not,” Noah says. “I’ve been really good about keep keeping my anxiety down. Sometimes I do colors of the rainbow (a relaxation exercise). Sometimes TV helps, too, but not all the time. When we’re not near the TV, I just do colors or breathing.”
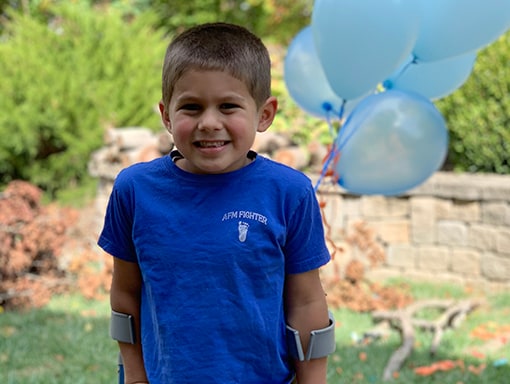
Today, Noah can walk with the help of forearm crutches and uses a wheelchair for longer distances. He loves baseball and plays on a team called the Red Sox. He enjoys going to the beach and likes to write and illustrate stories. These days, he’s excited about becoming a big brother. “Around Thanksgiving, that’s when Mr. Luke comes,” he says. “He’ll be a teeny, tiny baby.” In the meantime, he’s working on training his dog George. “We’re training him to help me,” Noah says. “He’s a very good dog, and he’s very cute. He’s almost as tall as the Eiffel Tower!”
“Have an open mind. Don’t put a limit on your child or the diagnosis, because doctors are still learning about this. Every kid is so individualized. It’s not a one-size-fits-all diagnosis. And you have to network. If you’re not a good networker or advocate, find a family liaison or someone who can help. You have to figure out what works for you and your family, but you also have to find the people who believe what you believe. Because not every doctor might believe what you believe, and that’s okay. That’s their prerogative. But you want to find people who are on the same page as you and have the same goals.”
“Mostly my advice is to be calm and don’t get mad if you’re frustrated. It’s okay, because life is frustrating sometimes. I know there can be some challenges in life, but you can’t stay stuck in the challenges. If you say you can’t do it, you can’t do it. But if you say you can do it, you can do it.”