Kevin’s Story
For 6 years, Kevin served as the principal of Bozeman High School, the largest high school in Montana. His time there capped a 34-year career in education, beginning with his days as a social studies teacher. Kevin retired in 2019, after developing AFM. Today, he is focusing on his recovery, with the support of his wife Barb, three adult daughters, and two grandchildren.


In September of 2018, Kevin had cold-like symptoms he couldn’t shake. Kevin has large b-cell non-Hodgkin’s lymphoma, so when he started to feel weak and had trouble walking, he went to his cancer center to get hydration. He was there for 3 hours and started to feel worse. He was having trouble talking and told Barb, “I feel like I’m having a stroke.” He and Barb went straight to the ER.
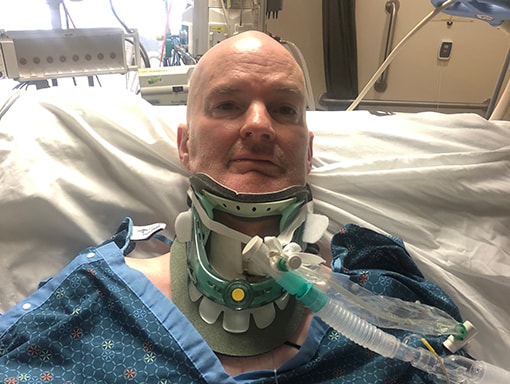
By the time they arrived at the ER, Kevin was having trouble breathing. Doctors admitted him to the intensive care unit (ICU), intubated him, and conducted a series of nerve tests. He quickly developed paralysis in his neck, diaphragm, and arms. Doctors diagnosed him with AFM and began treatment with steroids and intravenous immunoglobulin (IVIG). Doctors did not think plasmapheresis would be helpful, since Kevin had had a stem cell transplant 10 weeks earlier, as part of his lymphoma treatment.
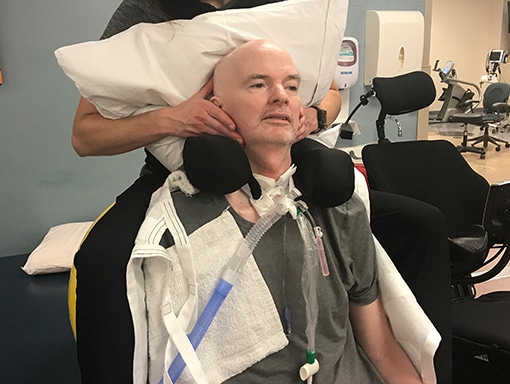
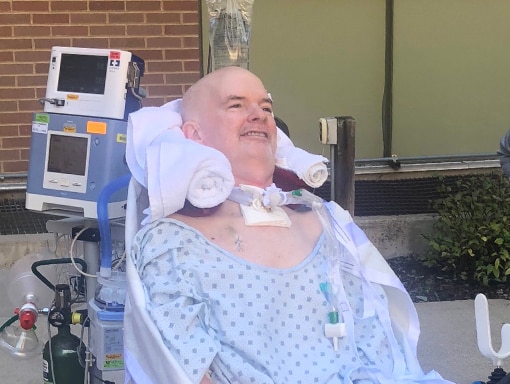
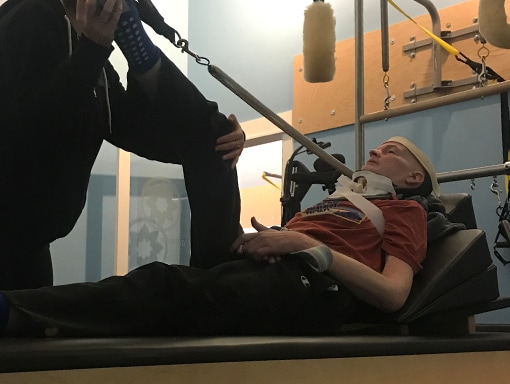
Kevin, Barb, and the medical team decided to transfer Kevin to a hospital in Salt Lake City, where he could receive treatment from specialists. Doctors in Salt Lake City did additional tests including an MRI and came to the same conclusion that Kevin had AFM. After 10 days in the ICU, Kevin moved to in-patient rehab. He spent 5 months there, doing intensive physical therapy, occupational therapy, and speech therapy every day, as well as talking to a counselor. He made steady progress, going from being unable to stand to being able to walk with assistance.
Kevin returned home and continued outpatient therapy at the hospital in Bozeman. Since the COVID-19 quarantine began, Kevin has been continuing therapy at home, with the help of Barb and his daughters. When the weather is nice, he enjoys going for walks in the neighborhood, using his walker. He is still on a ventilator at night but doesn’t need it during the day. He and Barb feel they’re getting closer and closer to removing the tracheostomy tube.
“Start the rehab therapy aggressively right from the beginning. It takes a long time, and it requires a lot of patience. It’s important to get assistance with mental health as soon as possible as well. The mental health challenges are as difficult, if not more so, than the physical challenges.”
“Reach out to other people who have gone through AFM to get their support. We’re part of a social media support group, which has been very helpful. That has been a great resource for learning as much as we can about the disease.”