Diagnosing and Classifying AFM
Clinicians diagnose AFM. CDC classifies AFM.
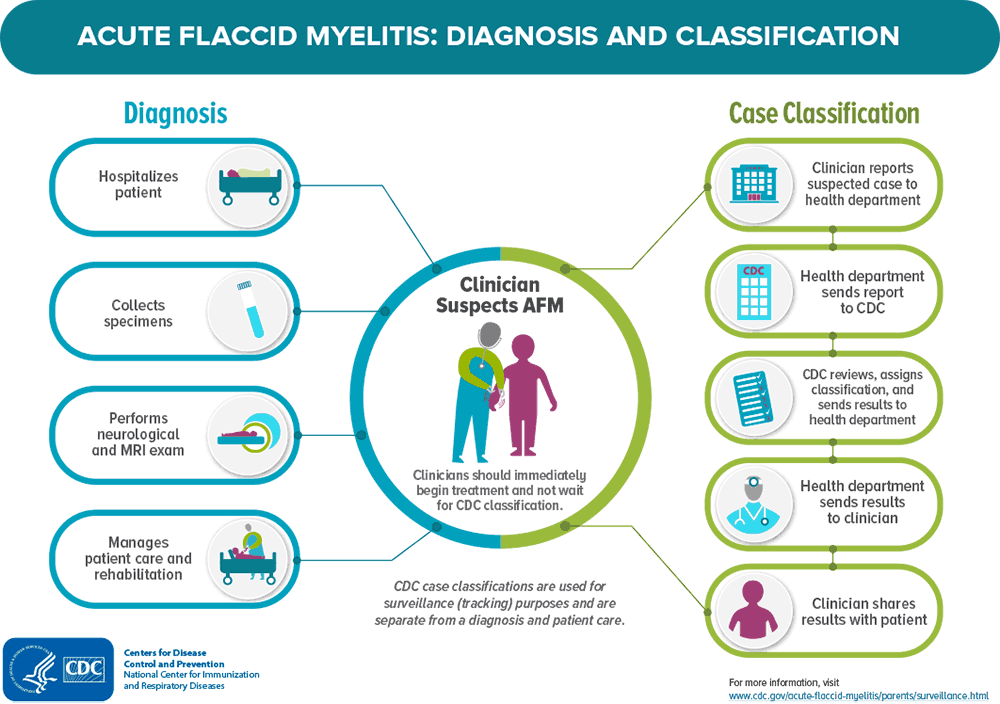
Clinicians diagnose AFM by taking a thorough medical history of the patient, doing a physical exam, and performing a magnetic resonance imaging (MRI) to review pictures of the spinal cord. If your child was diagnosed with AFM, consult with your child’s clinician about their treatment and rehabilitation plan.
When a clinician suspects or diagnoses AFM, they report the case to the state health department. The state health department sends CDC the medical records and specimens for the patient, with the patient’s personal information removed to protect privacy. We review these reports with a group of AFM experts and assign a case classification based on specific criteria. This is part of our national AFM surveillance process, and allows us to track cases of AFM over time. Using these consistent and specific criteria for case classifications helps us learn more about AFM by ensuring that the cases we are tracking are similar.
Some patients may have an AFM diagnosis from their clinician, but do not meet all the classification criteria for a confirmed or probable case. There are many reasons this can happen, for example if the MRI wasn’t done or if the results were unclear. Case classifications are meant for disease-tracking purposes only and have no effect on a clinical diagnosis given by the treating clinician. Your child’s clinician is the best person to talk to about your child’s illness and treatment options.
Clinicians should not wait for CDC’s case classification to diagnose AFM. If AFM is suspected, the clinician should hospitalize the patient immediately, refer to specialists, collect clinical specimens and order a brain and spinal MRI, monitor for signs of worsening symptoms, and begin treatment and rehabilitation.
Your child’s clinician will determine the best course of treatment. CDC case classifications do not change treatment or patient care.
AFM diagnosis is …
- Done by a clinician
- Done by examining the nervous system in combination with reviewing the MRI (pictures of the spinal cord)
- Meant to get the patient into medical treatment and care
- Independent from CDC’s case classification
AFM surveillance is …
- Done by CDC
- Done through reviewing patient medical records reported to CDC
- Meant to help track AFM, detect outbreaks, and inform research
- Independent from clinician’s diagnosis
Visit the Podcasts for Parents page to watch video podcasts, including episodes on surveillance and classification of AFM.