Jack’s Story
In June of 2016, Jack, was a rambunctious, high-energy 3-year-old living in Jacksonville, Florida.
He was constantly on the move, he loved riding his bike, and he had just become a big brother, when his parents Jennifer and Dan welcomed baby Matthew to the family.


Jack was having trouble walking on his way into preschool one morning. He was getting over a cold, so Dan brought him home to rest. Jack slept through much of the day. In the evening, Jack shook his arms oddly, like they were asleep. He had not improved by the next morning, and he hadn’t gone to the bathroom all night. Jack’s pediatrician advised Dan and Jennifer to take him to the emergency room.
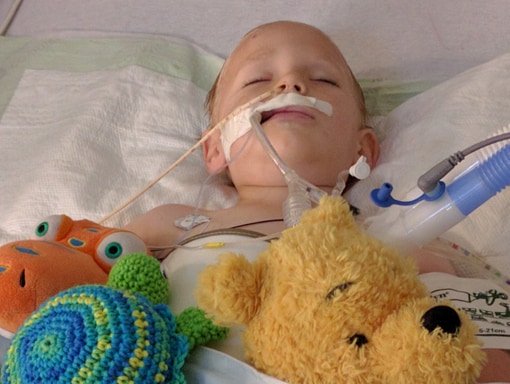
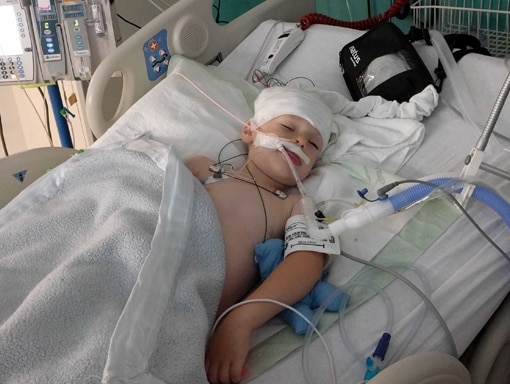
After conducting a series of tests, doctors at the ER suspected there was an issue with Jack’s appendix. Then Jack’s legs got weaker, he started to struggle to hold up his head, and he stopped moving his arms completely. Jennifer and Dan then went with Jack by ambulance to another hospital, where more doctors performed additional tests, including an MRI and an EEG. Early in the morning after a couple of days in the hospital, Jack stopped breathing on his own and had to be intubated. Jennifer remembers AFM moving rapidly through Jack’s body.
Doctors initially suspected transverse myelitis or Guillain-Barré syndrome. They began treatment with steroids, plasmapheresis, and intravenous immunoglobulin (IVIG). After 30 days, his doctors diagnosed Jack with AFM and recommended moving him to an intensive rehabilitation facility.
Jack and his mom took a medical flight to a facility in Baltimore, Maryland. Every day, he had 2 hours of occupational therapy, 2 hours of physical therapy, an hour of speech, and an hour of teaching. Slowly, Jack started to swallow a bit, talk a bit, and begin to kick his legs. After nearly 4 months of inpatient care, Jack was ready to come home.
Back at home, Jennifer and Dan moved Jack’s bedroom into the dining room, to allow space for his medical equipment. Jack started physical therapy, occupational therapy, and speech therapy at a local rehabilitation center. Jack made steady progress. In August of 2017, Jack had a diaphragmatic pacer placed to reduce the need for ventilator support.
Today, Jack is doing well in elementary school. He is still on a ventilator, but he continues to make progress, with the help of a medical team. He can now sit up and hold his head up by himself, and he’s starting to gain movement in his fingers and his shoulder. His parents say he talks a mile a minute and he’s an expert at controlling a TV, tablet, and video game console with his toes. “He’s going to do something spectacular in his life,” Jennifer says. “I don’t know what it is yet, and he doesn’t either. God has a plan, and we’re going to be okay.”
“Don’t be afraid to ask questions. Don’t be intimidated. You have to be your child’s advocate, and sometimes that means you have to ask doctors really hard questions. Be vigilant and know that there’s a community of other parents who are very willing to help. Don’t stop trying and don’t give up. Know that you’re not alone.”