Adverse Childhood Experiences, Overdose, and Suicide
Injury Center Priorities Are Urgent and Preventable

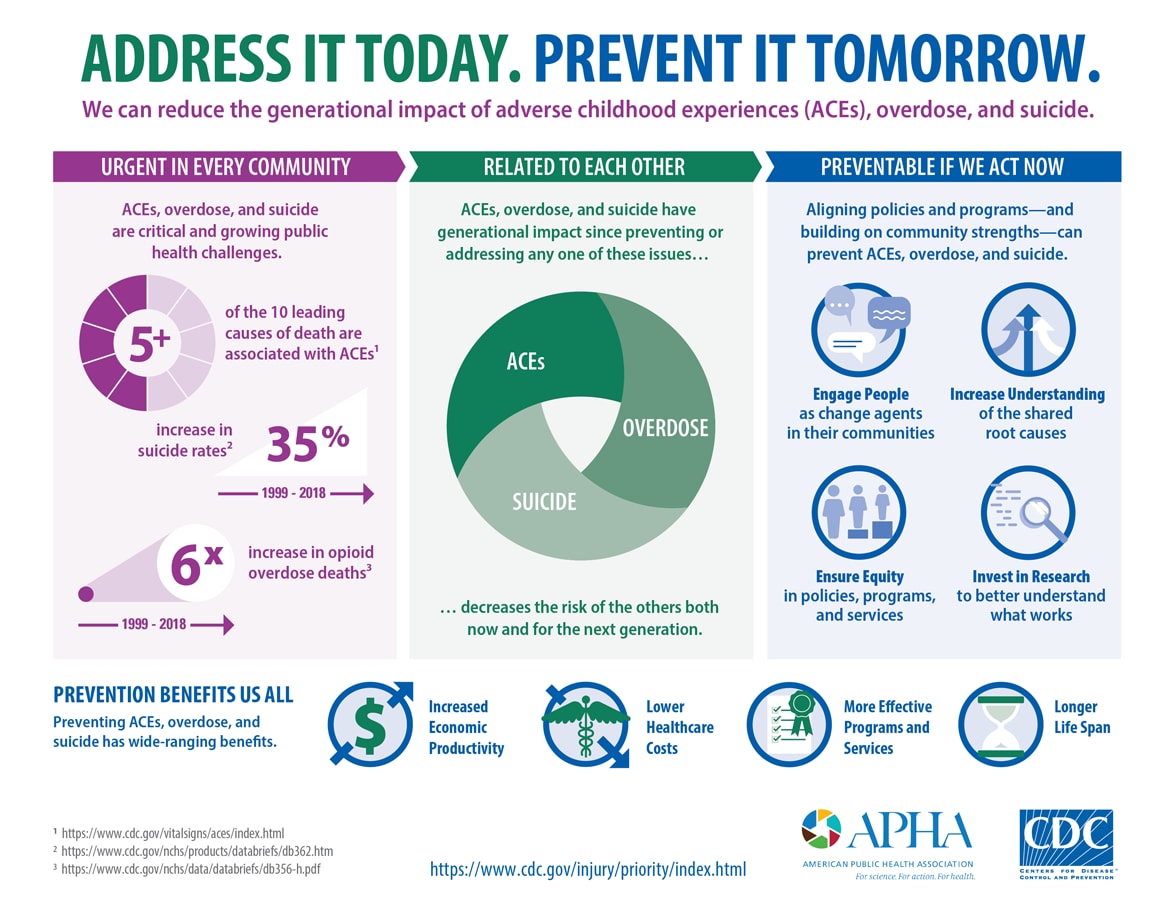
Adverse childhood experiences (ACEs), overdose, and suicide are urgent and related public health challenges that have consequences for all of us. But these challenges are preventable if we adopt a coordinated approach that focuses on addressing today’s crises while preventing tomorrow’s.

Experiencing adversity in childhood can change the way the brain develops and functions, contributing to increased risk of chronic diseases, such as diabetes, cancer, and stroke; substance use; suicide; and other injury and violence-related outcomes.

More than 92,000 drug overdose deaths occurred in the United States in 2020 alone. The adverse childhood experience of having a parent with substance use disorder or die from an overdose has profound impacts on the next generation.

People with lived experience (personally having attempted suicide or having had suicidal thoughts) may suffer long-term mental and physical health consequences including anger, guilt, and physical impairment. Similarly, survivors of a loved one’s suicide may experience ongoing pain and suffering, including grief, stigma, depression, anxiety, posttraumatic stress disorder, and increased risk of suicide or suicidal thoughts.
ACEs are associated with at least five of the 10 leading causes of death.
Drug overdoses have increased more than 500% between 1999 and 2020. Drug overdose remains a leading cause of injury-related death in the United States.
From 1999-2018, suicide rates rose 35 percent and declined in 2019- 2020. Suicide was the 9th leading cause of death in the United States in 2020.
Adverse childhood experiences increase the risk of opioid misuse and overdose and suicide later in life. ACEs are associated with younger age of opioid initiation, injection drug use, and likelihood of experiencing overdose.1
- A recent CDC study examined the association between experiencing ACEs and recent opioid misuse. Study findings showed that the odds of opioid misuse increased as the number of adverse childhood experiences increased. Students experiencing five or more ACEs were 15 times more likely to report opioid misuse than those experiencing no ACEs.2
- Losing a loved one to overdose or suicide during childhood is an ACE that can increase the risk of overdose or suicide.3
- ACEs are associated with lower educational attainment, unemployment, and poverty. These are risk factors for ACEs, suicide, and substance use that can impact future generations as well.4
- Experiencing trauma before age 18 is associated with increased odds of opioid misuse; the odds of opioid misuse are approximately three times higher among adults with four or more different experiences of trauma.5
- Having any ACE is associated with an increased risk for suicide. The odds of ever attempting suicide are 30 times higher for adults with four or more ACEs compared to adults with no ACEs. 6
CDC is working with partners to reduce the impact of ACEs, suicide, and overdose by:
- Generating understanding of the connection between ACEs, overdose, and suicide to inform more holistic, comprehensive, and effective policy and programs. Use shared, evidence-based, and easy-to-understand messages that create urgency.
- Engaging people as champions for prevention and agents for change in their own communities, including those with personal experience with these issues, decision-makers, champions across sectors, and others.
- Employing a comprehensive public health approach to prevent harm in the first place
- Identify people in need early and ensure equitable access to the programs and services they need.
- Provide long-term social and economic supports (e.g., income support for working families, paid family and sick leave, high quality childcare, and multi-generational substance use treatment that increase safe, stable, nurturing relationships and environments).
- To be effective, focus policies, funding and programs first where the need is greatest.
- Investing in research and evaluation to develop, test, implement, and translate evidence-based strategies to prevent ACEs, opioid overdose, and suicide and to address the connection between them.
Additional strategies for preventing ACEs and suicide can be found in CDC’s Technical Packages for Violence Prevention.
- Stein MD, Conti MT, Kenney S, et al. Adverse childhood experience effects on opioid use initiation, injection drug use, and overdose among persons with opioid use disorder. Drug Alcohol Depend. 2017;179:325-329. doi:10.1016/j.drugalcdep.2017.07.007
- Swedo, E. A., Sumner, S. A., de Fijter, S., Werhan, L., Norris, K., Beauregard, J. L., Montgomery, M. P., Rose, E. B., Hillis, S. D., & Massetti, G. M. (2020). Adolescent Opioid Misuse Attributable to Adverse Childhood Experiences. The Journal of Pediatrics, 224, 102-109.e3. https://doi.org/10.1016/j.jpeds.2020.05.001
- https://www.cdc.gov/violenceprevention/pdf/preventingACES.pdf [PDF – 3.66 MB]
- Metzler M, Merrick MT, Klevens J, Ports KA, Ford DC. Adverse childhood experiences and life opportunities: Shifting the narrative. Children and Youth Services Review. 2017;72:141-149. and Maguire-Jack, K. Pathways from childhood abuse and other adversities to adult health risks: The role of adult socioeconomic conditions. Child Abuse Negl. 2016;51:390-399.
- Quinn K, Boone L, Scheidell JD, Mateu-Gelabert P, McGorray SP, Beharie N, et al. The relationships of childhood trauma and adulthood prescription pain reliever misuse and injection drug use. Drug and Alcohol Dependence. 2016;169:190-8.
- Hughes K, Bellis MA, Hardcastle KA, Sethi D, Butchart A, Mikton C, Jones L., Dunne MP. The effect of multiple adverse childhood experiences on health: a systematic review and meta-analysis. The Lancet; 2017;2:e356-66.