
Scabies
[Sarcoptes scabiei]
Causal Agents
Sarcoptes scabiei var. hominis, the human itch mite, is in the arthropod class Arachnida, subclass Acari, family Sarcoptidae. The mites burrow into the upper layer of the skin but never below the stratum corneum. The burrows appear as tiny raised serpentine lines that are grayish or skin-colored and can be a centimeter or more in length. Other races of scabies mites may cause infestations in other mammals, such as domestic cats, dogs, pigs, and horses. It should be noted that races of mites found on other animals may cause a self-limited infestation in humans with temporary itching due to dermatitis; however they do not multiply on the human host.
Life Cycle
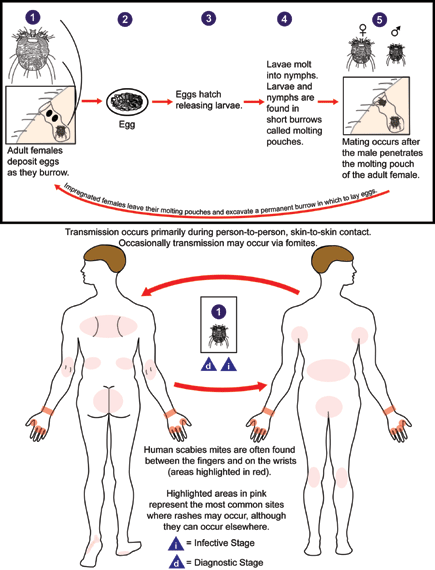
Sarcoptes scabiei undergoes four stages in its life cycle: egg, larva, nymph and adult. Females deposit 2-3 eggs per day as they burrow under the skin  . Eggs are oval and 0.10 to 0.15 mm in length
. Eggs are oval and 0.10 to 0.15 mm in length  and hatch in 3 to 4 days. After the eggs hatch, the larvae migrate to the skin surface and burrow into the intact stratum corneum to construct almost invisible, short burrows called molting pouches. The larval stage, which emerges from the eggs, has only 3 pairs of legs
and hatch in 3 to 4 days. After the eggs hatch, the larvae migrate to the skin surface and burrow into the intact stratum corneum to construct almost invisible, short burrows called molting pouches. The larval stage, which emerges from the eggs, has only 3 pairs of legs  and lasts about 3 to 4 days. After the larvae molt, the resulting nymphs have 4 pairs of legs
and lasts about 3 to 4 days. After the larvae molt, the resulting nymphs have 4 pairs of legs  . This form molts into slightly larger nymphs before molting into adults. Larvae and nymphs may often be found in molting pouches or in hair follicles and look similar to adults, only smaller. Adults are round, sac-like eyeless mites. Females are 0.30 to 0.45 mm long and 0.25 to 0.35 mm wide, and males are slightly more than half that size. Mating occurs after the active male penetrates the molting pouch of the adult female
. This form molts into slightly larger nymphs before molting into adults. Larvae and nymphs may often be found in molting pouches or in hair follicles and look similar to adults, only smaller. Adults are round, sac-like eyeless mites. Females are 0.30 to 0.45 mm long and 0.25 to 0.35 mm wide, and males are slightly more than half that size. Mating occurs after the active male penetrates the molting pouch of the adult female  . Mating takes place only once and leaves the female fertile for the rest of her life. Impregnated females leave their molting pouches and wander on the surface of the skin until they find a suitable site for a permanent burrow. While on the skin’s surface, mites hold onto the skin using sucker-like pulvilli attached to the two most anterior pairs of legs. When the impregnated female mite finds a suitable location, it begins to make its characteristic serpentine burrow, laying eggs in the process. After the impregnated female burrows into the skin, she remains there and continues to lengthen her burrow and lay eggs for the rest of her life (1-2 months). Under the most favorable of conditions, about 10% of her eggs eventually give rise to adult mites. Males are rarely seen; they make temporary shallow pits in the skin to feed until they locate a female’s burrow and mate.
. Mating takes place only once and leaves the female fertile for the rest of her life. Impregnated females leave their molting pouches and wander on the surface of the skin until they find a suitable site for a permanent burrow. While on the skin’s surface, mites hold onto the skin using sucker-like pulvilli attached to the two most anterior pairs of legs. When the impregnated female mite finds a suitable location, it begins to make its characteristic serpentine burrow, laying eggs in the process. After the impregnated female burrows into the skin, she remains there and continues to lengthen her burrow and lay eggs for the rest of her life (1-2 months). Under the most favorable of conditions, about 10% of her eggs eventually give rise to adult mites. Males are rarely seen; they make temporary shallow pits in the skin to feed until they locate a female’s burrow and mate.
Transmission occurs primarily by the transfer of the impregnated females during person-to-person, skin-to-skin contact. Occasionally transmission may occur via fomites (e.g., bedding or clothing). Human scabies mites often are found between the fingers and on the wrists.
Geographic Distribution
Scabies mites are distributed worldwide, affecting all races and socioeconomic classes in all climates.
Clinical Presentation
When a person is infested with scabies mites for the first time, symptoms may not appear for up to two months after becoming infested; however, an infested person can still transmit scabies during this time. If a person has had scabies before, they become sensitized to mites and symptoms generally occur much sooner, within 1 to 4 days. Mites burrowing under the skin cause a rash, which is most frequently found on the hands, particularly the webbing between the fingers; the folds of the wrist, elbow or knee; the penis; the breast; and/or the shoulder blades. Except in crusted (Norwegian) scabies, burrows and mites may be as few as 10-15 in number and can be difficult to find. A papular “scabies rash” may be seen in skin areas such as the buttocks, scapular region and abdomen, where female mites are absent; this may be a result of sensitization from a previous infection. Severe itching, especially at night and frequently over much of the body, including areas where mites are undetectable, is the most-common symptom of scabies. A more severe form of scabies that is more common among persons who are immunocompromised, elderly, or institutionalized is called crusted (Norwegian) scabies and is characterized by vesicles and formation of thick crusts over the skin, accompanied by abundant mites but only slight itching. Complications due to infestation are usually caused by secondary bacterial infections.
Sarcoptes scabiei mites.

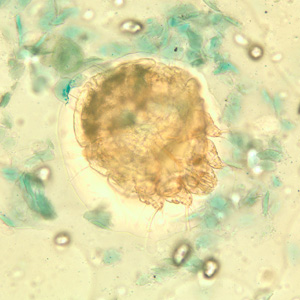
Sarcoptes scabiei mites in tissue specimens.


Follicle mites (Demodex spp.)



Laboratory Diagnosis
Most diagnoses of scabies infestation are made based upon the appearance and distribution of the rash and the presence of burrows. Whenever possible scabies should be confirmed by isolating the mites, ova or feces in a skin scraping. Scrapings should be made at the burrows, especially on the hands between the fingers and the folds of the wrist. Alternatively, mites can be extracted from a burrow by gently pricking open the burrow with a needle and working it toward the end where the mite is living. The extracted mite then can be identified by microscopy.
The following is a suggested method for collecting and examining skin scrapings:
Scrapings are best performed at the end of the burrows in non-excoriated and non-inflamed areas using a sterile scalpel blade containing a drop of mineral oil. The mineral oil enhances the adherence of the mites to the blade and can then be transferred to a glass slide. An additional 1-2 drops of mineral oil can be added to the slide, followed by a coverslip for microscopic examination. Skin scrapings should be screened at 40x or 100x magnification and then evaluated at 200 to 400x magnification for confirmation.
Treatment Information
Treatment information for scabies can be found at:
DPDx is an educational resource designed for health professionals and laboratory scientists. For an overview including prevention, control, and treatment visit www.cdc.gov/parasites/.