
Onchocerciasis
[Onchocerca volvulus]
Causal Agent
Onchocerca volvulus causes onchocerciasis (river blindness).
Life Cycle

During a blood meal, an infected blackfly (genus Simulium) introduces third-stage filarial larvae onto the skin of the human host, where they penetrate into the bite wound  . In subcutaneous tissues the larvae
. In subcutaneous tissues the larvae  develop into adult filariae, which commonly reside in nodules in subcutaneous connective tissues
develop into adult filariae, which commonly reside in nodules in subcutaneous connective tissues  . Adults can live in the nodules for approximately 15 years. Some nodules may contain numerous male and female worms. Females measure 33 to 50 cm in length and 270 to 400 µm in diameter, while males measure 19 to 42 mm by 130 to 210 µm. In the subcutaneous nodules, the female worms are capable of producing microfilariae for approximately 9 years. The microfilariae, measuring 220 to 360 µm by 5 to 9 µm and unsheathed, have a life span that may reach 2 years. They are occasionally found in peripheral blood, urine, and sputum but are typically found in the skin and in the lymphatics of connective tissues
. Adults can live in the nodules for approximately 15 years. Some nodules may contain numerous male and female worms. Females measure 33 to 50 cm in length and 270 to 400 µm in diameter, while males measure 19 to 42 mm by 130 to 210 µm. In the subcutaneous nodules, the female worms are capable of producing microfilariae for approximately 9 years. The microfilariae, measuring 220 to 360 µm by 5 to 9 µm and unsheathed, have a life span that may reach 2 years. They are occasionally found in peripheral blood, urine, and sputum but are typically found in the skin and in the lymphatics of connective tissues  . A blackfly ingests the microfilariae during a blood meal
. A blackfly ingests the microfilariae during a blood meal  . After ingestion, the microfilariae migrate from the blackfly’s midgut through the hemocoel to the thoracic muscles
. After ingestion, the microfilariae migrate from the blackfly’s midgut through the hemocoel to the thoracic muscles  . There the microfilariae develop into first-stage larvae
. There the microfilariae develop into first-stage larvae  and subsequently into third-stage infective larvae
and subsequently into third-stage infective larvae  . The third-stage infective larvae migrate to the blackfly’s proboscis
. The third-stage infective larvae migrate to the blackfly’s proboscis  and can infect another human when the fly takes a blood meal
and can infect another human when the fly takes a blood meal  .
.
Geographic Distribution
The agent of river blindness, Onchocerca volvulus, occurs mainly in Africa, with additional foci in Latin America and the Middle East.
Clinical Presentation
Onchocerciasis can cause pruritus, dermatitis, onchocercomata (subcutaneous nodules), and lymphadenopathies. The most serious manifestation consists of ocular lesions that can progress to blindness.
Microfilariae of Onchocerca volvulus in tissue.
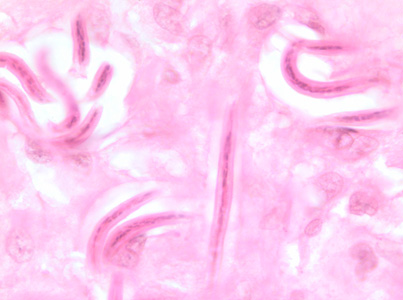


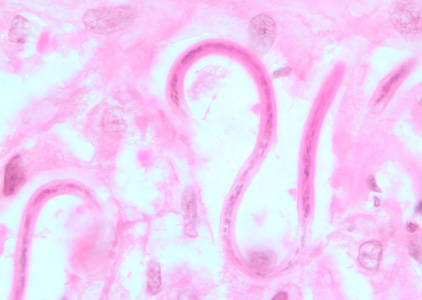

Adults of O. volvulus in tissue.





Diagnostic Findings
Microscopy
Onchocerciasis is usually diagnosed by the finding of microfilariae in skin snips or adults in biopsy specimens of skin nodules. Microfilariae of Onchocerca do not exhibit any form of periodicity and skin snips may be collected at any time.
Skin snips should be thin enough to include the outer part of the dermal palpillae but not so thick as to produce bleeding. Skin snips should be placed immediately in normal saline or distilled water, just enough to cover the specimen. Microfilariae tend to emerge more rapidly in saline, however in either medium the microfilariae typically emerge in 30-60 min and can be seen in wet mount preparations. For a definitive diagnosis, allow the wet mount to dry, fix in methanol, and stain with Giemsa or hematoxylin-and-eosin.
Treatment Information
Treatment information for onchocerciasis can be found at: https://www.cdc.gov/filarial-worms/treatment/onchocerciasis.html
DPDx is an educational resource designed for health professionals and laboratory scientists. For an overview including prevention, control, and treatment visit www.cdc.gov/parasites/.