Multistate Outbreak of Salmonella Typhimurium Infections Linked to Peanut Butter, 2008–2009
Posted January 21, 2009
Click here to go to the Final Update
This outbreak appears to be over. However, Salmonella is an important cause of human illness in the United States. More information about Salmonella, and steps people can take to reduce their risk of infection, can be found on the CDC Salmonella Web Page.
On this Page
Outbreak Highlights
- Case count is 488 in 43 states with latest reported illness beginning on January 8, 2009.
- Questions and Answers Related to the Salmonella Typhimurium Outbreak and Pets
- CDC Podcast - Salmonella Serotype Typhimurium Outbreak in Peanut Butter and Peanut Butter-Containing Products
- CDC’s Role in Food Safety
- Advice to Consumers
- Signs and Symptoms
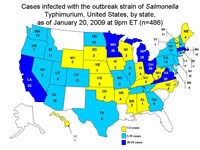
Persons Infected with the Outbreak Strain of Salmonella Typhimurium, United States, by State
Epidemic Curve
CDC is collaborating with public health officials in many states and the United States Food and Drug Administration (FDA) to investigate a multistate outbreak of human infections due to Salmonella serotype Typhimurium.
As of 9PM EDT, Tuesday, January 20, 2009, 486 persons infected with the outbreak strain of Salmonella Typhimurium have been reported from 43 states. The number of ill persons identified in each state is as follows: Alabama (1), Arizona (10), Arkansas (4), California (62), Colorado (12), Connecticut (9), Georgia (6), Hawaii (3), Idaho (11), Illinois (5), Indiana (4), Iowa (2), Kansas (2), Kentucky (3), Maine (4), Maryland (8), Massachusetts (42), Michigan (25), Minnesota (35), Missouri (9), Mississippi (3), Nebraska (1), New Hampshire (11), New Jersey (s19), New York (18), Nevada (5), North Carolina (4), North Dakota (10), Ohio (65), Oklahoma (2), Oregon (7), Pennsylvania (14), Rhode Island (4), South Dakota (2), Tennessee (9), Texas (6), Utah (5), Vermont (4), Virginia (20), Washington (13), West Virginia (2), Wisconsin (3), and Wyoming (2). Additionally, one ill person was reported from Canada.
Among the persons with confirmed, reported dates available, illnesses began between September 8, 2008 and January 8, 2009. Patients range in age from < 1 to 98 years; 48% are female. Among persons with available information, 22% reported being hospitalized. Infection may have contributed to six deaths.
The outbreak can be visually described with a chart showing the number of persons who became ill each day. This chart is called an epidemic curve or epi curve. The epi curve and information about interpreting it may be found here. It shows that most illnesses began after October 1, 2008. Illnesses that occurred after December 21, 2008 may not yet be reported due to the time it takes between when a person becomes ill and when the illness is reported. This takes an average of 2 to 3 weeks. Please see the Salmonella Outbreak Investigations: Timeline for Reporting Cases for more details.
Outbreak Investigation
The investigation is ongoing, and exposures to peanut butter and other peanut butter-containing products are being examined.
Peanut Butter
Preliminary analysis of the first national case-control study conducted by CDC and public health officials in multiple states on January 3 and 4, 2009, comparing foods eaten by ill and well persons indicates that peanut butter is a likely source of the bacteria causing the infections.
An investigation by the Minnesota Department of Health suggested King Nut brand creamy peanut butter as a likely source of Salmonella infections among many ill persons in Minnesota. The Minnesota Department of Agriculture Laboratory isolated the outbreak strain of Salmonella Typhimurium from an open 5-pound container of King Nut brand creamy peanut butter. King Nut creamy peanut butter is distributed in many states to establishments such as long-term care facilities, hospitals, schools, universities, restaurants, delis, cafeterias, and bakeries. It is not sold directly to consumers and is not known to be distributed for retail sale in grocery stores.
The Connecticut Department of Public Health Laboratory and the Georgia Department of Agriculture independently isolated Salmonella from unopened 5-pound containers of King Nut brand peanut butter. Officials in Connecticut have identified the Salmonella found in their container as the outbreak strain. Further tests are pending in Georgia to determine if the Salmonella in their container is also the outbreak strain.
To date, 15 clusters of infections in five states have been reported in schools and other institutions, such as long-term care facilities and hospitals. Among 14 clusters for which we have detailed information, King Nut is the only brand of peanut butter used in those facilities.
King Nut is produced by Peanut Corporation of America (PCA) in Blakely, Georgia. This facility, which is no longer producing any products, has expanded its recall to include all peanut butter and peanut paste produced at this plant since July 1, 2008. Peanut butter and peanut butter paste was not sold directly to consumers but was distributed to institutions, food service providers, food manufacturers and distributors in many states, Canada, Korea, and Haiti. Peanut butter and peanut paste is commonly used as an ingredient in many products, including cookies, crackers, cereal, candy, ice cream and other foods.
Other Peanut-Containing Products
To clarify whether other peanut-butter containing foods are associated with the outbreak, CDC along with state partners conducted a second national case-control study. On January 17-19 2009, telephone interviews were conducted with 54 persons who became ill with the outbreak strain and 399 well persons. Preliminary analysis of data received as of 9PM, Sunday, January 18, reveals an association between illness and consumption of pre-packaged peanut butter crackers, specifically with Austin and Keebler brands.
Austin and Keebler brand peanut butter crackers are produced by the Kellogg Company in North Carolina, using peanut paste from the Peanut Corporation of America. On January 14, 2009, The Kellogg Company put a precautionary hold on these peanut butter crackers, and on January 16 recalled these products. Other peanut butter containing products produced by a variety of companies may have been made with the ingredients recalled by PCA. CDC and state health departments continue to investigate the association of other brands and foods that contain peanut butter with illness.
The list of peanut butter and other peanut containing products that may be affected in this outbreak is still being determined and is incomplete at this time. However, the list of currently recalled products can be found on the FDA website. FDA and the product manufacturers are working to determine the list of affected products, which may be extensive. Many companies have already announced whether their products include ingredients being recalled by Peanut Corporation of America, Georgia, and more companies are expected to make similar announcements. The list of recall announcements from companies can be found at FDA website.
Recommendations
Based on available information, CDC and FDA recommendations include:
For consumers
- Do not eat products that have been recalled and throw them away in a manner that prevents others from eating them. These products include Austin and Keebler brand peanut butter crackers and King Nut brand peanut butter produced since July 1, 2008. (FDA's web site has recalled lot numbers).
- Postpone eating other peanut butter containing products (such as cookies, crackers, cereal, candy and ice cream) until more information becomes available about which brands may be affected.
- Use FDA’s online database to check if foods you’re concerned about are on the recall list.
- Call the consumer hotline phone number that may be on any product packaging you have to get information directly from the product manufacturer.
- Persons who think they may have become ill from eating peanut butter are advised to consult their health care providers.
For retailers
- Stop selling recalled products.
For directors of institutions and food service establishments
- Ensure that they are not serving recalled products.
For manufacturers
- Inform consumers about whether their products could contain peanut butter or other peanut-containing products from Peanut Corporation of America. If a manufacturer knows their products do not contain peanut-containing products from PCA, they should inform consumers of that.
To date, no association has been found with major national brand name jars of peanut butter sold in grocery stores.
For more information
- For the latest information about the epidemiological investigation, go to the CDC Salmonella Typhimurium Outbreak Investigation Update website.
- For the latest information about recalled products, go to FDA Salmonella Typhimurium Outbreak site.
- More general information about Salmonella can be found on the CDC Salmonella website.
Public health officials will advise the public if more products are identified as being associated with the outbreak.
Clinical Features/Signs and Symptoms
Most persons infected with Salmonella develop diarrhea, fever, and abdominal cramps 12–72 hours after infection. Infection is usually diagnosed by culture of a stool sample. The illness usually lasts 4 to 7 days. Although most people recover without treatment, severe infections may occur. Infants, elderly persons, and those with impaired immune systems are more likely than others to develop severe illness. When severe infection occurs, Salmonella may spread from the intestines to the bloodstream and then to other body sites and can cause death unless the person is treated promptly with antibiotics.
More information on this investigation can be found below.
- Connecticut Department of Consumer Protection press release
- Georgia Department of Agriculture
- Minnesota Department of Health and Minnesota Department of Agriculture press release
- FDA – Salmonella Typhimurium Outbreak
- More information on Salmonella
- More general information about Salmonella can be found here under Salmonella FAQs.
CDC's Role in Food Safety
As an agency within the U.S. Department of Health and Human Services (HHS), CDC leads federal efforts to gather data on foodborne illnesses, investigate foodborne illnesses and outbreaks, and monitor the effectiveness of prevention and control efforts. CDC is not a food safety regulatory agency but works closely with the food safety regulatory agencies, in particular with HHS’s U.S. Food and Drug Administration (FDA) and the Food Safety and Inspection Service within the United States Department of Agriculture (USDA). CDC also plays a key role in building state and local health department epidemiology, laboratory, and environmental health capacity to support foodborne disease surveillance and outbreak response. Notably, CDC data can be used to help document the effectiveness of regulatory interventions.
Get email updates
To receive email updates about this page, enter your email address:
Contact Us:
- Centers for Disease Control and Prevention
1600 Clifton Rd
Atlanta, GA 30333 - 800-CDC-INFO
(800-232-4636)
TTY: (888) 232-6348 - Contact CDC–INFO
 ShareCompartir
ShareCompartir