Congenital Zika Syndrome & Other Birth Defects
Zika virus infection during pregnancy can lead to congenital Zika syndrome and other birth defects. This webpage describes these outcomes and how healthcare providers can monitor infants for these findings.
Congenital Zika Syndrome
A distinct pattern of birth defects and disabilities, called congenital Zika syndromeexternal icon, has been found with Zika virus infection during pregnancy. Although many of the features seen as part of congenital Zika syndrome can be caused by other infections during pregnancy, the five features listed below are rarely seen with other infections or are unique to congenital Zika syndrome:
- Severe microcephaly in which the skull has partially collapsed
- Decreased brain tissue with a specific pattern of brain damage, including subcortical calcifications
- Damage to the back of the eye, including macular scarring and focal retinal pigmentary mottling
- Congenital contractures, such as clubfoot or arthrogryposis
- Hypertonia restricting body movement soon after birth
Congenital Zika virus infection has also been associated with other abnormalities, including but not limited to brain atrophy and asymmetry, abnormally formed or absent brain structures, hydrocephalus, and neuronal migration disorders. Other anomalies include excessive and redundant scalp skin. Reported neurologic findings include hyperreflexia, irritability, tremors, seizures, brainstem dysfunction, and dysphagia. Reported eye abnormalities include, but are not limited to, focal pigmentary mottling and chorioretinal atrophy in the macula, optic nerve hypoplasia or atrophy, other retinal lesions, iris colobomas, congenital glaucoma, microphthalmia, lens subluxation, cataracts, and intraocular calcifications.
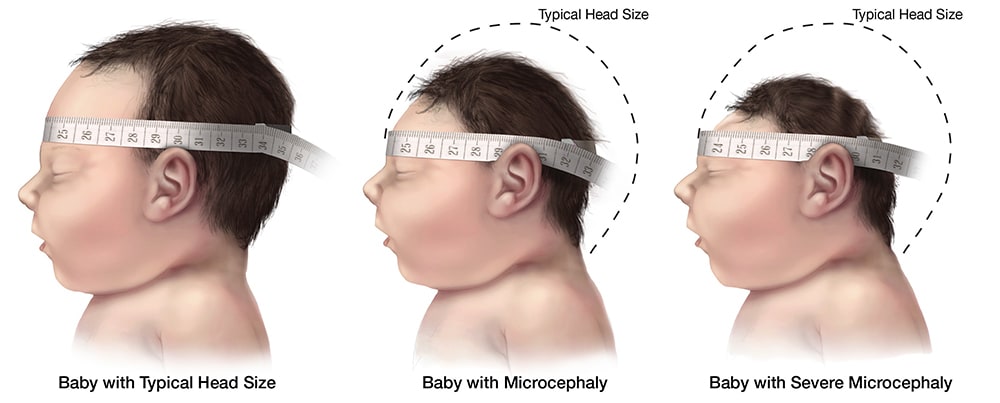
Microcephaly
Microcephaly is a congenital malformation resulting in smaller than normal head size for age and sex. It has also been associated with other birth defects and neurologic conditions in children and adults. For infants diagnosed with microcephaly, head size correlates with underlying brain size. However, these measurements do not consistently predict long term sequelae. Neurologic sequelae may include seizures, vision or hearing problems, and developmental disabilities. Symptoms vary with the extent of brain disruption.
There is now scientific consensus that Zika virus infection during pregnancy is a cause of microcephaly. We do not know if a newborn who gets Zika virus infection around the time of birth will develop microcephaly after birth. Babies can develop microcephaly after birth if their head growth slows or if the brain fails to develop. There have been no reports of Zika virus infection around the time of birth leading to microcephaly in infants.
Diagnosis of Microcephaly
Microcephaly is diagnosed when an infant’s head is smaller than expected as compared to infants of the same age (or gestational age) and sex. For the purpose of evaluating an infant for possible congenital Zika virus infection, microcephaly is defined as occipitofrontal circumference less than the third percentile, based on standard growth charts for sex, age, and gestational age at birth. For a diagnosis of microcephaly to be made, the occipitofrontal circumference should be disproportionately small and not explained by other etiologies (e.g., other congenital disorders).
Diagnosing Microcephaly
| Diagnosis | Pregnancy Outcome |
|---|---|
| Definite Congenital Microcephaly | For Live Births: Head circumference (HC) at birth less than the 3rd percentile for gestational age and sex OR if HC at birth is not available, HC less than the 3rd percentile for age and sex within the first 2 weeks of life For Stillbirths and Elective Terminations: HC at delivery less than the 3rd percentile for gestational age and sex |
| Possible Congenital Microcephaly | For Live Births: If earlier HC is not available, HC less than the 3rd percentile for age and sex beyond 6 weeks of life For All Pregnancy Outcomes: Microcephaly diagnosed or suspected on prenatal ultrasound in the absence of available postnatal HC measurements |
Charts for Head Circumference at Birth
| Gestational Age | INTERGROWTH-21st Fetal Growth Standard for Head Circumference at Birth |
|---|---|
| 33–43 Weeks | Newborn Size at Birth Chartexternal icon and tool for calculating centiles for head circumference for infants 33–42 weeksexternal icon |
| 24–32 Weeks | Very Preterm Size at Birth Referencesexternal icon and tool for calculating centiles for head circumference for infants 24–32 weeksexternal icon |
| <24 Weeks | Fetal Growth Standardsexternal icon |
INTERGROWTH-21st Fetal Growth Standards are based on measurements in utero only. International standards for birth measurements in infants less than 24 weeks gestation are not available. For most elective pregnancy terminations and many stillbirths, accurate postnatal head circumference measurements are not possible.
For a study comparing head circumference measurements in utero to those obtained after birth, see: Melamed N, Yogev Y, Danon D, et al. Sonographic estimation of fetal head circumference: how accurate are we? Ultrasound Obstet Gynecol 2011;37:65-71.
In the setting of Zika virus infection, the head circumference might be disproportionately small in comparison with the length of the infant. The small head size should not be explained by other etiologies.
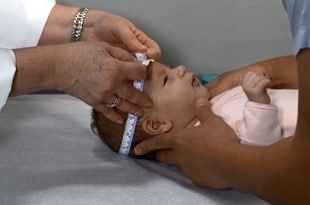
Measuring Head Circumference
Head circumference (occipitofrontal circumference) measurements should be taken using a tape measure that cannot be stretched. The tape is securely wrapped around the widest possible circumference of the head, 1–2 finger widths above the eyebrow on the forehead and at the most prominent part of the back of the head. Ideally, the measurement should be taken three times, with the largest measurement recorded to the nearest 0.1 cm. It may be helpful to have the parent or nurse hold the infant’s arms.
Although head circumference measurements may be influenced by molding and other factors related to delivery, the measurements should be taken on the first day of life because commonly-used birth head circumference reference charts by age and sex are based on measurements taken before 24 hours of age. The most important factor is that the head circumference is carefully measured and documented. If measurement within the first 24 hours of life is not done, the head circumference should be measured as soon as possible after birth.
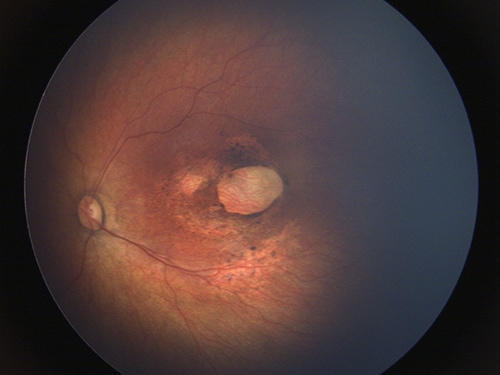
Ocular Findings in Babies with Congenital Zika Virus Infection
Ocular abnormalities have been reported in infants with congenital Zika virus infection with and without microcephaly or other central nervous system anomalies. Ocular findings have been reported involving both the anterior and posterior parts of the eye. Among infants with presumed congenital Zika virus infection, the most commonly reported structural ocular abnormalities involve the macula and the optic nerve.
Learn more about ocular findings in babies with congenital Zika virus infection. More >external icon
The most commonly reported macular findings include
- Focal pigmentary mottling
- Chorioretinal atrophy
Commonly reported optic nerve findings include
- Optic nerve hypoplasia or atrophy
Other ocular findings that have been reported in infants with congenital Zika virus infection include, but are not limited to
- Other retinal lesions: subretinal hemorrhage, hypopigmentation, vascular tortuosity, abnormal termination of the vessels, focal vascular dilation
- Congenital glaucoma
- Iris colobomas
- Microphthalmia
- Cataracts
- Subluxation of the lens
- Intraocular calcification
Although most ocular abnormalities have been reported in infants with microcephaly, ocular abnormalities have been found in infants without microcephaly or other central nervous system findings. Therefore, it is critical that all infants with possible congenital Zika virus infection receive recommended screening and follow-up care.
CDC Interim Guidance for the Evaluation and Management of Infants with Possible Congenital Zika Virus infection recommends a comprehensive ophthalmologic exam within one month of birth for (1) all infants born to people with laboratory evidence of Zika virus infection during pregnancy and (2) infants who have physical exam findings consistent with congenital Zika syndrome, regardless of mother’s Zika test results.
- Measurement of Head Circumference: Implications for Microcephaly Surveillance in Zika-Affected Areasexternal icon (Tropical Medicine and Infectious Disease, 2021)
- Vital Signs: Zika-Associated Birth Defects and Neurodevelopmental Abnormalities Possibly Associated with Congenital Zika Virus Infection – U.S. Territories and Freely Associated States, 2018 (MMWR, 2018)
- Health and Development at Age 19–24 Months of 19 Children Who Were Born with Microcephaly and Laboratory Evidence of Congenital Zika Virus Infection During the 2015 Zika Virus Outbreak — Brazil, 2017
- Vital Signs: Update on Zika Virus–Associated Birth Defects and Evaluation of All U.S. Infants with Congenital Zika Virus Exposure — U.S. Zika Pregnancy Registry, 2016 (MMWR, 2017)
- Baseline Prevalence of Birth Defects Associated with Congenital Zika Virus Infection — Massachusetts, North Carolina, and Atlanta, Georgia, 2013–2014 (MMWR, 2017)
- Characterizing the Pattern of Anomalies in Congenital Zika Syndrome for Pediatric Cliniciansexternal icon (JAMA Network, 2017)
- Facts about Microcephaly
- Zika virus and birth defects – Reviewing the evidence for causalityexternal icon (NEJM, 2016)