The State of the HIV Epidemic in the U.S.

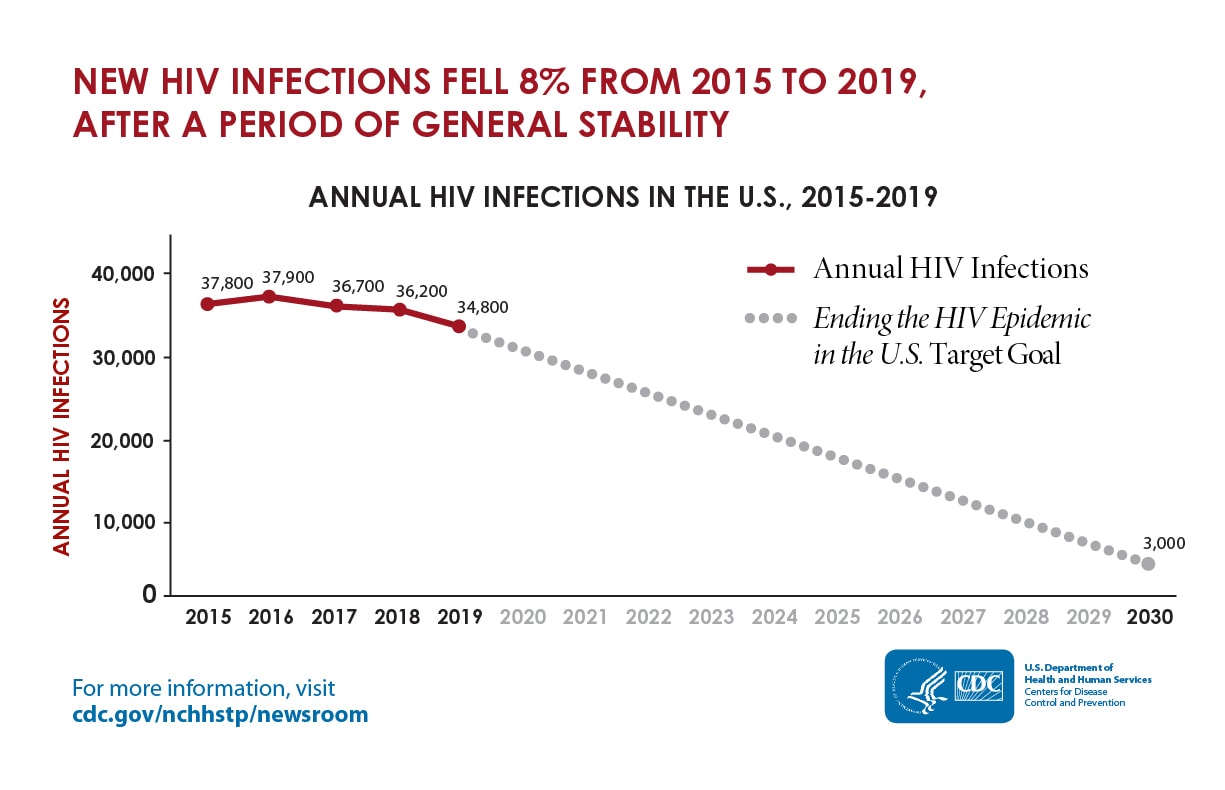
Annual HIV Infections in the U.S., 2015-2019
COVID-19 and HIV
The full impact of the COVID-19 pandemic on HIV in the U.S. will not be known for some time. However, CDC data have shown concerning setbacks to HIV prevention, including sharp declines in HIV testing and diagnosis from 2019 to 2020. These declines were due to high levels of disruptions to clinical care and community services, reductions in patients accessing the clinical services that were available, and reductions in partner services and testing as public health staff shifted to the COVID-19 response.
Prescriptions for pre-exposure prophylaxis (PrEP) also increased at slower rates than before COVID-19, and not at the rate needed to meet the federal Ending the HIV Epidemic in the U.S. The nation must accelerate efforts to protect health, expand access to proven HIV prevention tools, and meet rapidly approaching national goals to end the HIV epidemic.
Due to the disruptions in testing and clinical care services, CDC is not able to estimate new HIV infections (“HIV incidence”) for 2020 or to provide HIV trends through 2020. CDC is also unable to estimate the total number of diagnosed and undiagnosed HIV infections (“HIV prevalence”); or knowledge of HIV status.
CDC estimates that, as of 2019, about 1.2 million people in the U.S. have HIV. New HIV infections have declined in recent years, after a period of general stability. Overall, new infections fell 8% from 37,800 in 2015 to 34,800 in 2019.
Much of this progress was due to larger declines among young gay and bisexual men (ages 13-24) in recent years. From 2015 to 2019, new infections dropped 33% overall among this population.
There have been hopeful signs of progress in HIV prevention, but gains remain uneven, and HIV continues to affect some groups severely and disproportionately.
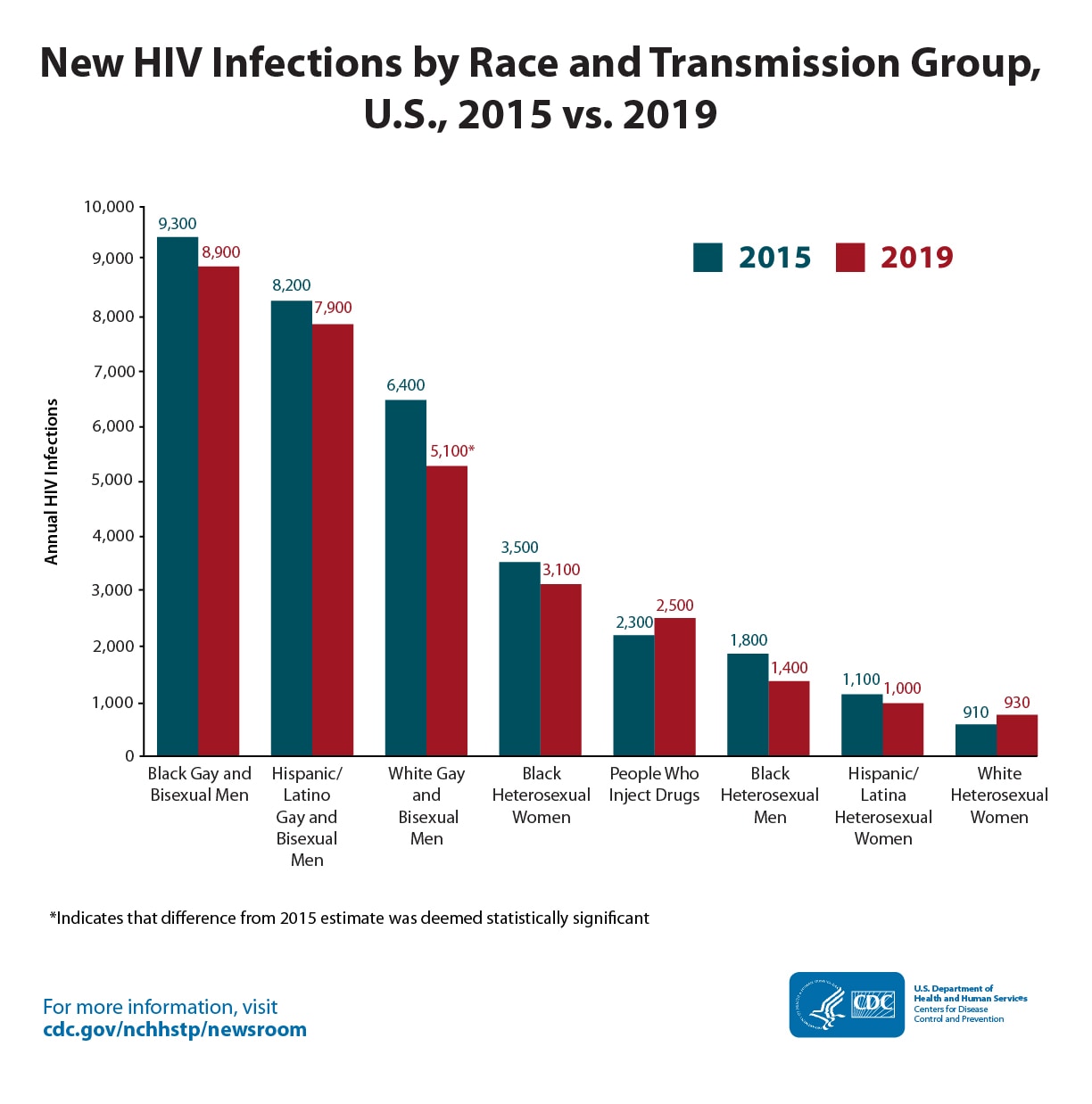
Annual HIV Infections in the U.S. by Race and Transmission Group, 2015 vs. 2019
Gay and bisexual men continue to account for most new HIV infections (66%), and disparities in HIV remain severe among some racial and ethnic minority groups. Black or African American people (hereafter referred to as Black people) face rates of infection that are eight times as high as White people, Hispanic and Latino people and face rates that are almost four times as high. Hispanic and Latino people can be of any race.
Geographically, the South is also disproportionately affected. The region accounted for more than half (53%) of new HIV infections in 2019, even though it only represented 38% of the U.S. population.
CDC has accelerated efforts to reduce health disparities among transgender women and other groups. Transgender women, Black people, and Hispanic and Latino people are key populations for CDC’s major HIV prevention funding programs, including funding to state and local health departments and community-based organizations. The ongoing Ending the HIV Epidemic in the U.S. (EHE) initiative also includes the use or expansion of innovative, community-tailored HIV testing and care strategies for these groups.
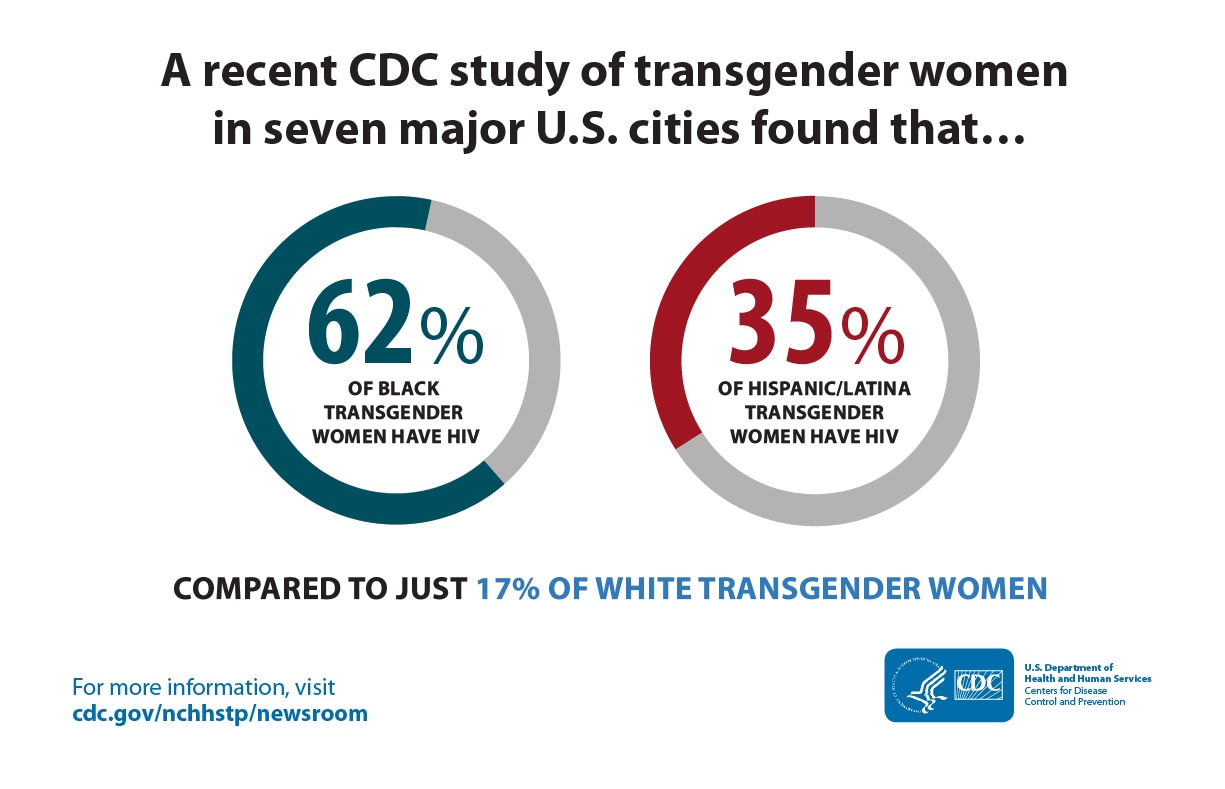
Proportion of Transgender Women with HIV in 7 U.S. cities by Race/Ethnicity, 2019-2020
HIV Among Transgender Women
Transgender women urgently need more HIV prevention and treatment services. A recent CDC study found that four in 10 transgender women in seven major U.S. cities have HIV. Among this group, there are stark racial and ethnic differences in HIV rates – nearly two-thirds of Black transgender women and over one-third of Hispanic and Latina transgender women have HIV.
Before the COVID-19 pandemic, CDC data suggest that declines in HIV infections were likely due to increased uptake of HIV prevention strategies, such as PrEP and rapid and effective HIV treatment. Recent data suggest that community-driven innovations in the delivery of health care services may have helped people with HIV continue to get treatment and care during the onset of the COVID-19 pandemic. In 2020:
- 25% of people eligible for PrEP were prescribed it (23% in 2019).
- 68% of people with diagnosed HIV were virally suppressed (66% in 2019), and 82% were rapidly linked to care within one month of diagnosis (81% in 2019) in 46 jurisdictions.
However, the nation must accelerate progress in HIV prevention. PrEP prescriptions are increasing at slower rates than before COVID-19 and the same level of people with HIV were virally suppressed in 2020 than 2019. The Ending the HIV Epidemic in the U.S. initiative goals call for 50% of people who could benefit from PrEP to be prescribed it and 95% of people with diagnosed HIV being virally suppressed by 2025.
Additionally, approximately 13% of people with HIV in the U.S. still do not know their status, and few are receiving adequate HIV care and treatment that will help them get and keep viral suppression and live longer, healthier lives. HIV testing is critical to ending the epidemic because it is the bridge to all HIV treatment and prevention.
Addressing disparities will be crucial
Data show that HIV prevention and treatment services are not reaching many who could benefit the most.
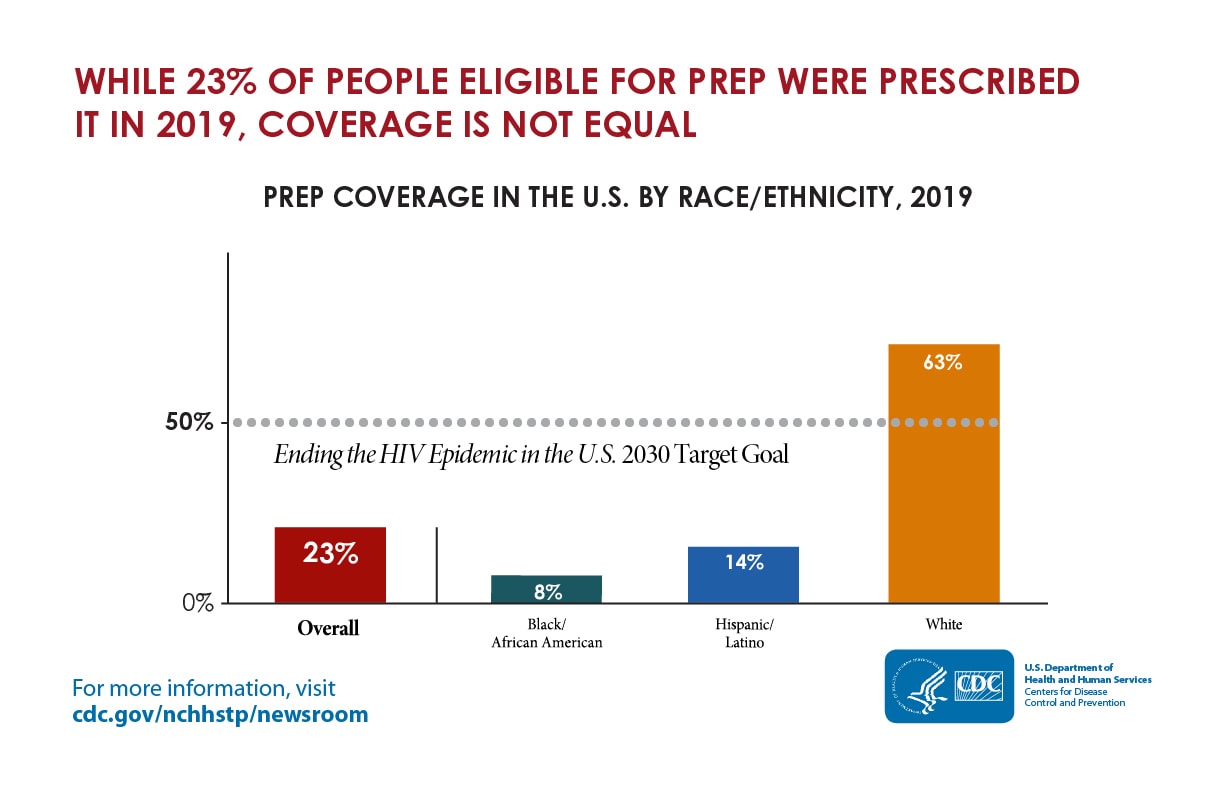
PrEP Coverage in the U.S. by Race/Ethnicity, 2020
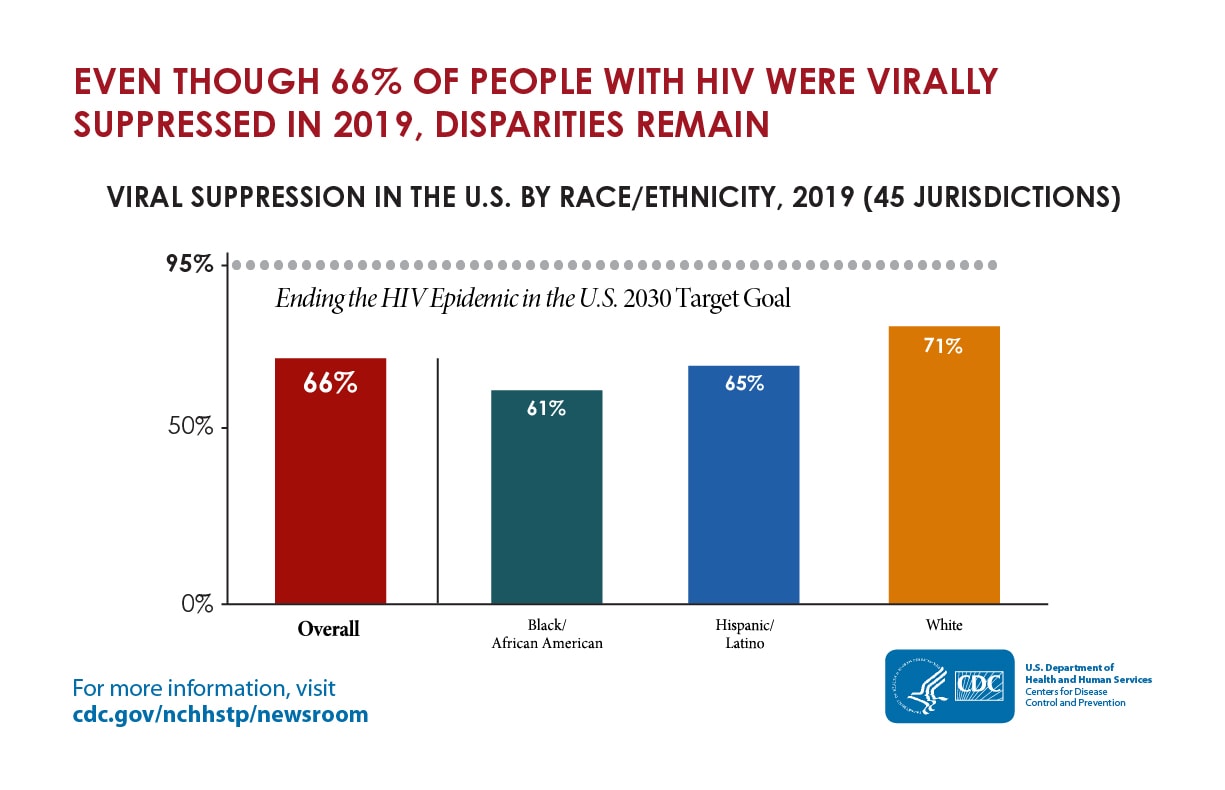
Viral Suppression Rates in the U.S. by Race/Ethnicity, 2020
To end the HIV epidemic in the U.S., the nation must ensure that people eligible for PrEP use it, and that people with HIV are equitably aware of their status, rapidly linked to and retained in care, and get and keep viral suppression.
As the nation continues to respond to COVID-19, increasing access to HIV prevention and treatment through Ending the HIV Epidemic in the U.S. (EHE) initiative remains an urgent priority – as far too many have not yet been reached with the strategies that work. Getting back on track will require expanding all EHE strategies. A significant increase in resources is required to deliver many innovations and programmatic activities at the level needed to meet the initiative’s 2025 goals. Without the resources needed to intensify these efforts, we will fall short of these rapidly approaching national goals.
Visit HIV.gov for more about this federal initiative, and CDC.gov/endHIV for more about CDC’s role in this effort.
If you are a member of the news media and need more information, please visit www.cdc.gov/nchhstp/newsroom or contact CDC’s Media Office at 404-639-3286 or media@cdc.gov.

