Facts about Upper and Lower Limb Reduction Defects
What are limb reduction defects?
Upper and lower limb reduction defects occur when a part of or the entire arm (upper limb) or leg (lower limb) of a fetus fails to form completely during pregnancy. The defect is referred to as a “limb reduction” because a limb is reduced from its normal size or is missing.
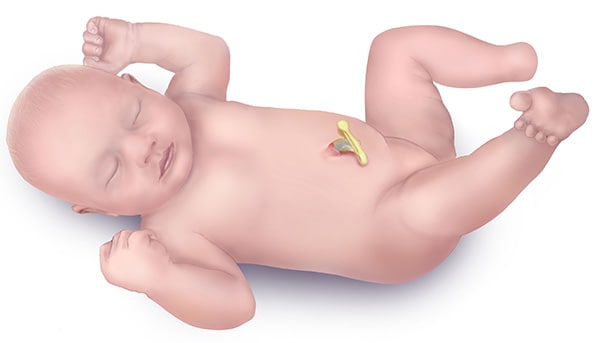
Congenital absence of foot and toes
Click here to view a larger image
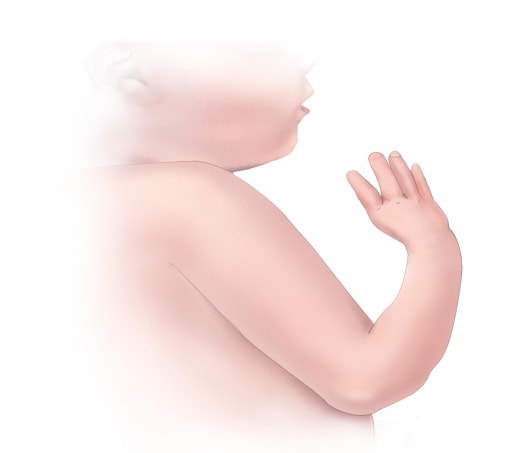
Longitudinal reduction defect of radius
Other Problems
Babies and children with limb reduction defects will face various issues and difficulties, but the extent of these will depend on the location and size of the reduction. Some potential difficulties and problems include:
- Difficulties with normal development such as motor skills
- Needing assistance with daily activities such as self-care
- Limitations with certain movements, sports, or activities
- Potential emotional and social issues because of physical appearance
How Many Babies are Born with Limb Reduction Defects?
Researchers estimate that about 1 in every 1,900 babies is born with a limb reduction defect in the United States. Some of these babies will have both upper and lower limb reduction defects.1
Causes and Risk Factors
The cause of limb reduction defects is unknown. However, research has shown that certain behaviors or exposures during pregnancy can increase the risk of having a baby with a limb reduction defect. These include:
- Exposure of the mother to certain chemicals or viruses while she is pregnant
- Exposure of the mother to certain medications
- Possible exposure of the mother to tobacco smoking (although more research is needed)
CDC works with many researchers to study risk factors that can increase the chance of having a baby with limb reduction defects, as well as outcomes of babies with the defect. Following are examples of what this research has found:
- A woman taking multivitamins before she gets pregnant might decrease her risk for having a baby with limb reduction defects, although more research is needed.2
- Certain sets of limb reduction defects might be associated with other birth defects, such as heart defects, omphalocele, and gastroschisis.3
Treatment
Specific treatment for limb reduction defects will be determined by the child’s doctor, based on things like the child’s age, the extent and type of defect, and the child’s tolerance for certain medications, procedures, and therapies.
The overall goal for treatment of limb reduction defects is to provide the child with a limb that has proper function and appearance. Treatment can vary for each child. Potential treatments include:
- Prosthetics (artificial limbs)
- Orthotics (splints or braces)
- Surgery
- Rehabilitation (physical or occupational therapy)
It is important to remember that some babies and children with limb reductions will have some difficulties and limitations throughout life, but with proper treatment and care they can live long, healthy, and productive lives.
References
- Mai CT, Isenburg JL, Canfield MA, Meyer RE, Correa A, Alverson CJ, Lupo PJ, Riehle‐Colarusso T, Cho SJ, Aggarwal D, Kirby RS. National population‐based estimates for major birth defects, 2010–2014. Birth Defects Research. 2019; 111(18): 1420-1435.
- Yang QH, Khoury MJ, Olney RS, & Mulinare J. Does periconceptional multivitamin use reduce the risk for limb deficiency in offspring? Epidemiology. 1997;8: 157-61.
- Rosano A, Botto LD, Olney RS, Khoury MJ, Ritvanen A, Goujard J, et al. Limb defects associated with major congenital anomalies: clinical and epidemiological study from the International Clearinghouse for birth defects monitoring systems. Am J Med Genet. 2000;93: 110-16.