Continue to check our website for further updates on when we will reopen. When the museum reopens, all visitors will need to make reservations at least a week in advance. Walk-in visits are no longer permitted.
Teen Newsletter: Histoplasmosis
February 2023
The David J. Sencer CDC Museum (CDCM) Public Health Academy Teen Newsletter was created to introduce teens to public health topics. Each newsletter focuses on a different public health topic that CDC studies. Newsletter sections include: Introduction, CDC’s Work, The Public Health Approach, Out of the CDC Museum Collection, and Teen Talk.
CDC’s Mycotic Diseases Branch (MDB) works with partners to prevent illness and death from fungal diseases such as histoplasmosis. They are one of few public health groups in the world devoted to the prevention and control of fungal diseases. They investigate outbreaks, develop prevention interventions, and work to increase access to lifesaving antifungal medications. MDB is broken into teams that focus on different areas of work.

MDB’s Epidemiology Team:
- Determines the number of people who get sick from fungal diseases
- Tracks trends and patterns in how fungal diseases affect people
- Promotes education and awareness about fungal diseases
- Develops and evaluates ways to prevent fungal diseases
- Helps prepare healthcare facilities and laboratories in other countries to better detect and treat fungal diseases

MDB’s Laboratory Team:
- Finds and identifies disease-causing fungi in patient and environmental specimens
- Performs tests on certain specimens to see if they are resistant to antifungal medicines
- Researches and develops new detection, diagnostic, and subtyping methods
- Uses whole genome sequencing to study how and why certain fungi spread and make people sick
- Conducts a yearly mold identification training course in collaboration with the Association of Public Health Laboratories
- Helps other laboratories improve their abilities to test for certain fungi
CDC and partners organize Fungal Disease Awareness Week to highlight the importance of recognizing serious fungal diseases early enough in the course of a patient’s illness to provide life-saving treatment.
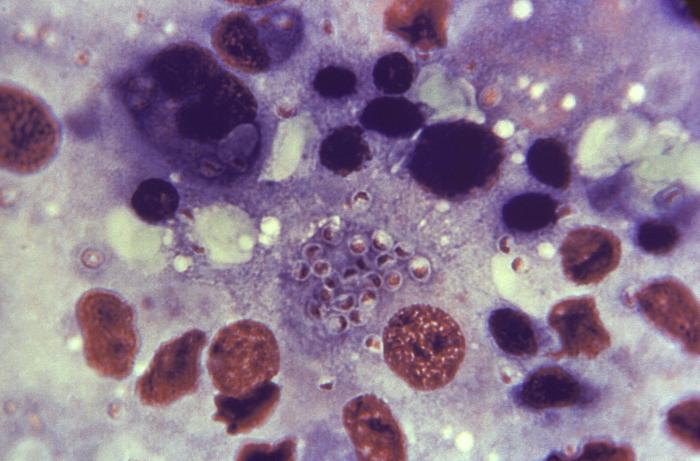
Histoplasmosis is an infection caused by a fungus called Histoplasma capsulatum. The fungus lives in the environment, particularly in soil that contains large amounts of bird or bat droppings where conditions are ideal for the fungus to grow. In the United States, Histoplasma capsulatum mainly lives in the central and eastern states, especially areas around the Ohio and Mississippi River valleys. The fungus also lives in parts of Central and South America, Africa, Asia, and Australia.
Histoplasma capsulatum spores circulate in the air after contaminated soil is disturbed, such as with activities like spelunking, cleaning chicken coops, or construction. The spores are too small to see without a microscope and people can breathe them in without knowing it. In the lungs, a person’s body temperature allows the spores to transform into yeast. These yeast can then travel to lymph nodes and can spread to other parts of the body through the bloodstream.
Although most people who breathe in the spores don’t get sick, those who do may have a fever, cough, and fatigue. Symptoms of histoplasmosis may appear between 3 and 17 days after a person breathes in the fungal spores. Many people who get histoplasmosis will get better on their own without medication. However, histoplasmosis can develop into a long-term lung infection. It can spread from the lungs to other parts of the body, such as the central nervous system (the brain and spinal cord).

Some people are at higher risk for developing the severe forms of histoplasmosis:
- People who have weakened immune systems, such as people who have HIV/AIDS, organ transplant recipients, or those who are taking certain medications
- Infants
- Adults aged 55 and older
Prescription antifungal medication, such as itraconazole, is needed to treat severe histoplasmosis in the lungs, chronic histoplasmosis, and infections that have spread from the lungs to other parts of the body.
Click the image below to read the personal stories of Ken and Mauricio, two people affected by histoplasmosis.
Public health problems are diverse and can include infectious diseases, chronic diseases, emergencies, injuries, environmental health problems, as well as other health threats. Regardless of the topic, we take the same systematic, science-based approach to a public health problem by following four general steps.
- Surveillance (What is the problem?). In public health, we identify the problem by using surveillance systems to monitor health events and behaviors occurring among a population.
Histoplasmosis has been described as the most common endemic mycosis (fungal disease) in the United States. However, histoplasmosis is not nationally notifiable,
meaning that not all doctors are to report confirmed or suspected cases to CDC. It is reportable in certain states, dependent upon state and local laws.
This map shows the average rate of reported histoplasmosis cases per 100,000 people by county for 12 states with available surveillance data during 2011–2014. Note that many of the states are blank not because there were no cases of histoplasmosis, but because they were not reported to CDC. On this map, cases are classified according to people’s county of residence, which might not be where they acquired the infection. These rates cannot be directly compared across states because different histoplasmosis case definitions were used in each state.

Most cases of histoplasmosis are not part of a larger outbreak. However, histoplasmosis outbreaks linked to a common source occur occasionally. This map shows the locations of 105 histoplasmosis outbreaks that happened during 1938–2013 and the number of outbreak-related cases by state or territory. Some of these outbreaks happened in places where scientists did not expect Histoplasma capsulatum to live. Investigating histoplasmosis outbreaks helps public health officials understand who is most at risk for developing histoplasmosis.

For ease of explaining and understanding the public health approach for this public health problem, let’s focus on a specific outbreak of histoplasmosis at a campsite in Louisiana in 2018 and learn how CDC partners with the state health department to respond.
- Risk Factor Identification (What is the cause?). After we’ve identified the problem, the next question is, “What is the cause of the problem?” For example, are there factors that might make certain populations more susceptible to diseases, such as something in the environment or certain behaviors that people are practicing?
When two patients were hospitalized in Louisiana with histoplasmosis, the health department began investigating their recent activities. They found that both had just returned from a camping trip with a large group of people, about half of whom were now feeling sick. The health department learned that the campers participated in many activities, including hiking, collecting firewood, digging soil, and geocaching. Geocaching is a digital scavenger hunt wherein players locate objects and sites using a smartphone or GPS device. When they toured the geocaching sites, they found that one of the objects had been hidden in the soil at the bottom of a hollow tree. When the team looked inside with a flashlight, little eyes stared back at them. Bats!

This hollowed-out tree was the source of Histoplasma in the Louisiana campsite outbreak.
Because the fungus that causes histoplasmosis can grow in soil with a high concentration of bat droppings, investigators tested the soil in the tree. The samples came back positive for Histoplasma capsulatum.
“Fungal disease outbreaks are relatively rare— this investigation confirmed that people can get histoplasmosis in Louisiana, and that disruption of soil is still a significant health risk for both sick and healthy individuals,” said Jose Serrano, MPH, epidemiologist at the Louisiana Department of Health and lead investigator of the histoplasmosis outbreak.
- Intervention Evaluation (What works?). Once we’ve identified the risk factors related to the problem, we ask, “What intervention works to address the problem?” We look at what has worked in the past in addressing this same problem and if a proposed intervention makes sense with our affected population.
The investigation team recommended the following actions to help prevent similar histoplasmosis outbreaks:
- Campers should avoid disrupting soil in areas with bird or bat poop.
- Camp staff should help educate campers about the risk and symptoms of histoplasmosis.
- Public health officials and health care providers should help increase awareness about histoplasmosis throughout Louisiana.
- Implementation (How did we do it?). In the last step, we ask, “How can we implement the intervention? Given the resources we have and what we know about the affected population, will this work?”

After finding the fungus, the Louisiana Department of Health worked to identify any potential high-risk areas to prevent others from becoming exposed. Officials told campers to avoid activities that disturb soil. Additionally, health department staff provided a document that camp officials can share with all future visitors. It tells campers how to reduce their risk of being exposed to the fungus.
Still, improved efforts are needed to educate the community in endemic areas about histoplasmosis to prevent the occurrence of such outbreaks in the future. In addition, increased awareness among health care providers of this disease would facilitate appropriate diagnosis and treatment as the two original cases were initially misdiagnosed with pneumonia.
Using The Public Health Approach helps public health professionals identify a problem, find out what is causing it, and determine what solutions/interventions work.
This month’s Out of the CDC Museum Collection includes pictures of bats, an organism related to histoplasmosis. The droppings of bats and birds contain large amounts of nitrogen, an element that encourages the growth of fungi such as Histoplasma capsulatum. Contact with soil in areas of concentrated bat or bird droppings is a major risk factor for developing histoplasmosis.
Although these images were taken from a study of rabies in the 1960s, they show how CDC has conducted research for decades to learn more about how animals are connected to diseases that can make us sick. These images were added to the museum’s collection in 2020.

Check out the ears on this little bat! Bats rely on echolocation to visualize the world using reflected sound waves, so these large ears are important adaptations.

Look closely! Those aren’t just rocks. They’re thousands of bats roosting on the ceiling of a cave.

Bats are trapped in the field using very large string nets that trap them as they fly. Surveying bats in an area can help us learn more about their population and any diseases they might carry, such as rabies or Ebola.

