CDC in Haiti

The U.S. Centers for Disease Control and Prevention (CDC) began working with Haiti’s Ministry of Public Health and Population (MSPP) in 2002 to address the growing HIV/AIDS epidemic. Initially focused on prevention and treatment services, CDC’s HIV work expanded to include laboratory systems strengthening, health information systems, workforce development and capacity building, and the integrated HIV and tuberculosis (TB) clinical services. CDC’s increased support to MSPP has resulted in substantial advances in health security and public health system strengthening in Haiti. CDC works with partners such as the Pan-American Health Organization and other non-governmental organizations to provide technical assistance and logistical support focused on rebuilding and strengthening Haiti’s laboratory systems.
HIV and Tuberculosis (TB)
As a key implementer of the U.S. President’s Emergency Plan for AIDS Relief (PEPFAR), CDC works with Haiti’s Ministry of Public Health and Population (MSPP) to build a sustainable, high-impact national HIV response program with the goal to achieve epidemic control of HIV. CDC works with partners and supports national efforts to:
- prevent the transmission of HIV
- increase the accessibility and quality of HIV clinical services and treatment
- increase patient adherence and treatment continuity
- strengthen surveillance, epidemiology, laboratory, and health information management systems
Haiti has the highest incidence of TB in the Western Hemisphere. CDC supports national efforts to expand the overall availability of treatment for multidrug-resistant TB. To increase TB case detection, CDC has worked closely with the MSPP to build TB-related laboratory and clinical capacity at high-volume sites throughout Haiti.
Laboratory diagnostic capacity for TB has expanded considerably since 2010, notably with the establishment of a national biosafety level 3 (BSL-3) laboratory to improve multi-drug resistant TB case detection and treatment capacities.
CDC increased access to strategic information by supporting the development and the expansion of integrated health management information systems. This also includes an electronic medical record (EMR) system and a case-based longitudinal surveillance system SALVH that is useful in providing fully deduplicated numbers which were used for the first time for both the process of calculating HIV estimates and for the COP23.
CDC is supporting trainings to improve quality of services and outcomes of beneficiaries. Trainings to departmental directorates’ staff, implementing partners, and the interagency USG PEPFAR Team include Continuous Quality Improvement (CQI) HealthQual Methodology for the National AIDS Control Program of MSPP.
CDC leveraged the national patient-tracing application, PLR. This application has been supported by CDC for several years, and supports the electronic Crisis Zone report to assist in tailoring actions for people living with HIV living in areas with heightened violence.
Global Health Security
CDC’s global health security efforts in Haiti help improve the country’s ability to prevent, detect, and respond to infectious disease outbreaks before they become global epidemics. These efforts are helping Haiti reach the targets outlined in the Global Health Security Agenda. CDC is supporting the government of Haiti to minimize disease threats by bolstering laboratory and disease surveillance capacity, improving emergency preparedness and response, facilitating immunization efforts, and addressing antimicrobial resistance.
Supported the establishment of a laboratory-enhanced surveillance system and Haiti’s National Epidemiological Surveillance Network, which monitors disease trends and detects potential outbreaks in real time, permitting timely case investigations. The network now covers over 60% of the health facilities across the country.
Increased laboratory testing capacity by supporting the establishment of a National Specimen Referral Network for the efficient transport of specimens to the National Public Health Laboratory.
Provides continuous technical support to the MSPP to revise the Integrated Disease Surveillance and Response tool. This effort improved multisector coordination of national and sub-national disease surveillance.
In 2023, CDC obtained engagement of the MSPP at the highest level to strengthen Emergency preparedness and response through a systematic approach to assess country capacity to establish a comprehensive plan.
Field Epidemiology Training Program (FETP)
CDC supports Haiti in strengthening the capacity of its workforce to investigate and respond to disease outbreaks through the establishment of a Field Epidemiology Training Program (FETP). FETP residents and graduates are a vital component of Haiti’s health workforce and promote health security throughout all levels of Haiti’s public health system. Graduates serve in leadership roles as departmental health directors, work in the field collecting and analyzing surveillance data, and provide crucial epidemiological expertise during emergencies.
Over 470 fellows have graduated from the program since it was established in 2011.
Since 2010, FETP graduates and trainees have responded to more than 4,000 outbreaks and emergencies, including COVID-19 and Cholera.
Most FETP graduates continue to work for the MSPP as doctors, nurses, computer scientists, lab technicians, and veterinarians throughout all ten geographical departments in Haiti.
Since 2010, CDC works closely with the MSPP to control the cholera epidemic and reduce the impact of the disease. CDC supports efforts to eliminate cholera transmission include:
- improving diarrheal disease surveillance
- enhancing laboratories capacity for diagnosis (culture and PCR)
- training rural potable water and sanitation technicians
- expanding water, sanitation, and hygiene (WASH) capacity, and
- supporting oral cholera vaccine campaigns
In 2022, after more than 3 years with no cholera cases reported, multiple factors facilitated a resurgence of cholera in the country. Although the current incidence of cholera is far lower than at the peak of the epidemic in 2011, the disease remains a persistent public health threat.
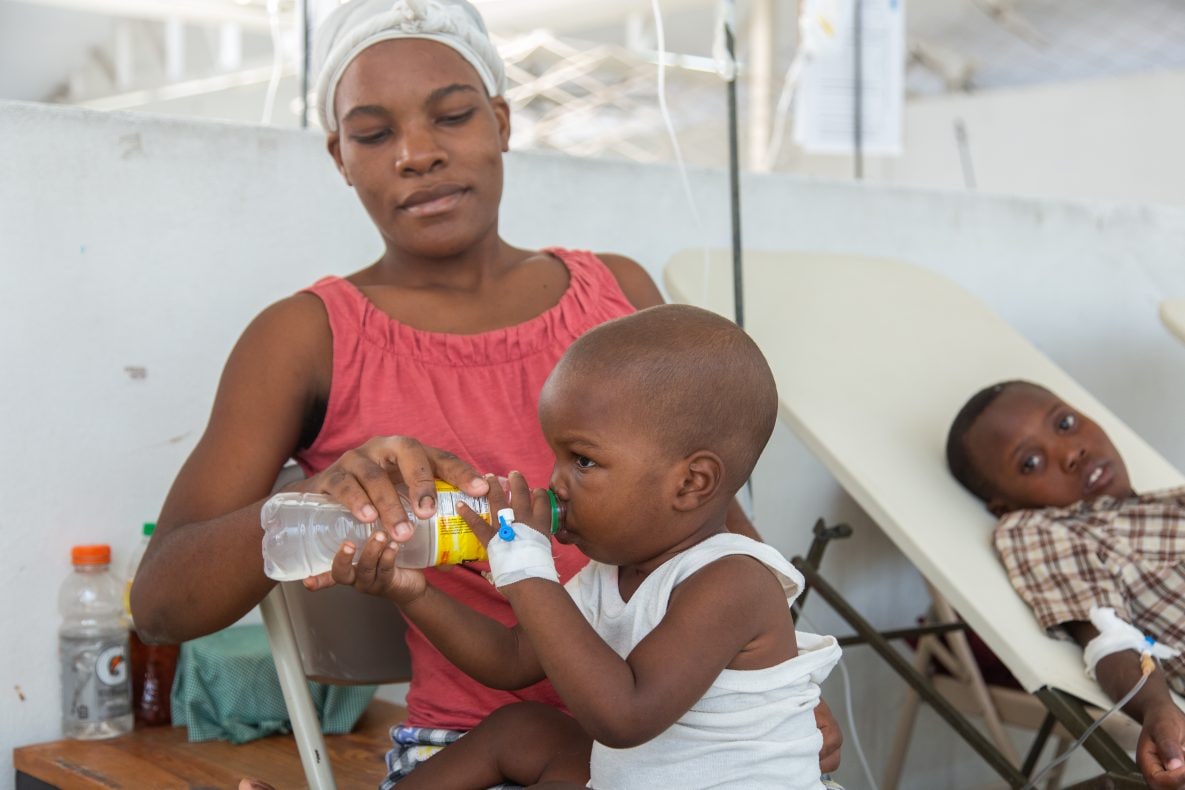
CREDIT: © UNICEF/U.S. CDC/Unique Identifier/Georges Harry Rouzier
During the 2022 outbreak response, CDC supported outbreak control by providing technical assistance and support in surveillance/laboratory capacity, vaccination, treatment and case management, risk communication and community engagement, and WASH.
Coordinated strategies with USAID to develop a comprehensive emergency response plan for maximum impact and targeted approach.
Malaria
Since 2010, CDC provides technical assistance on malaria control and elimination activities and interventions. Within the Caribbean region, Malaria remains endemic only on Hispaniola. CDC supports MSPP and other partners in adopting malaria rapid diagnostic tests, monitoring for anti-malaria drug resistance, and adopting the policy for community health workers to test and treat malaria.
Supports the National Malaria Control Program and other partners to strengthen the country’s control and elimination strategy.
Provided technical assistance as needed in the areas of vector control, molecular surveillance, and case management.
COVID-19
CDC played a critical role in the MSPP’s response to COVID-19. CDC leadership and technical staff participated as core members of the national incident management team, where they advised national policy and implementation decisions. Technical staff also heavily support the surveillance, laboratory, case management, and community engagement.
Technical and financial support to MSPP and National Lab for COVID-19 diagnostics–for both laboratory and surveillance activities.
Technical assistance on COVID-19 case management and infection prevention and control at the central level and departmental level through the Health Directorates and existing clinical partners.
Financial support for border surveillance and WASH activities within health facilities.
Technical assistance in emergency preparedness, training personnel for case investigation and contact tracing, and the general surveillance system and lab.
Technical assistance on vaccine preparedness activities including administration, waste management, adverse event monitoring and broader vaccine surveillance.
Additional CDC Activities
CDC experts work with partners on a broad range of public health issues, including activities related to:
- Neglected Tropical Diseases: CDC assists with strategic planning for lymphatic filariasis (LF) elimination including new strategies to deliver mass drug administration medicines to at-risk populations. In 2013, CDC began working with the Haitian government to initiate the Haiti Animal Rabies Surveillance Program— a cost effective intervention to reduce human rabies deaths using a multidisciplinary strategy.
- WASH: CDC provided support to conduct essential repairs on drinking water networks ensuring reliable access to clean water for numerous communities. CDC also worked to improve water quality to reduce the incidence of waterborne diseases.
- Vaccine-preventable diseases: CDC provide technical support to the vaccination program in areas of governance, vaccine strategy and for surveillance and diagnosis of vaccine-preventable diseases.
- Infection prevention and control: Developing infection prevention and control (IPC) measures and updating standard operation procedures (SOP) for healthcare facilities. These SOPs allowed for rapidly detecting and containing emerging threats to healthcare settings before spreading to patients and communities. As such, protecting healthcare workers and patients from infection in healthcare settings.
- Dengue: CDC provides technical assistance to the National Public Health Laboratory in the investigation and testing protocols of dengue cases in Haiti.
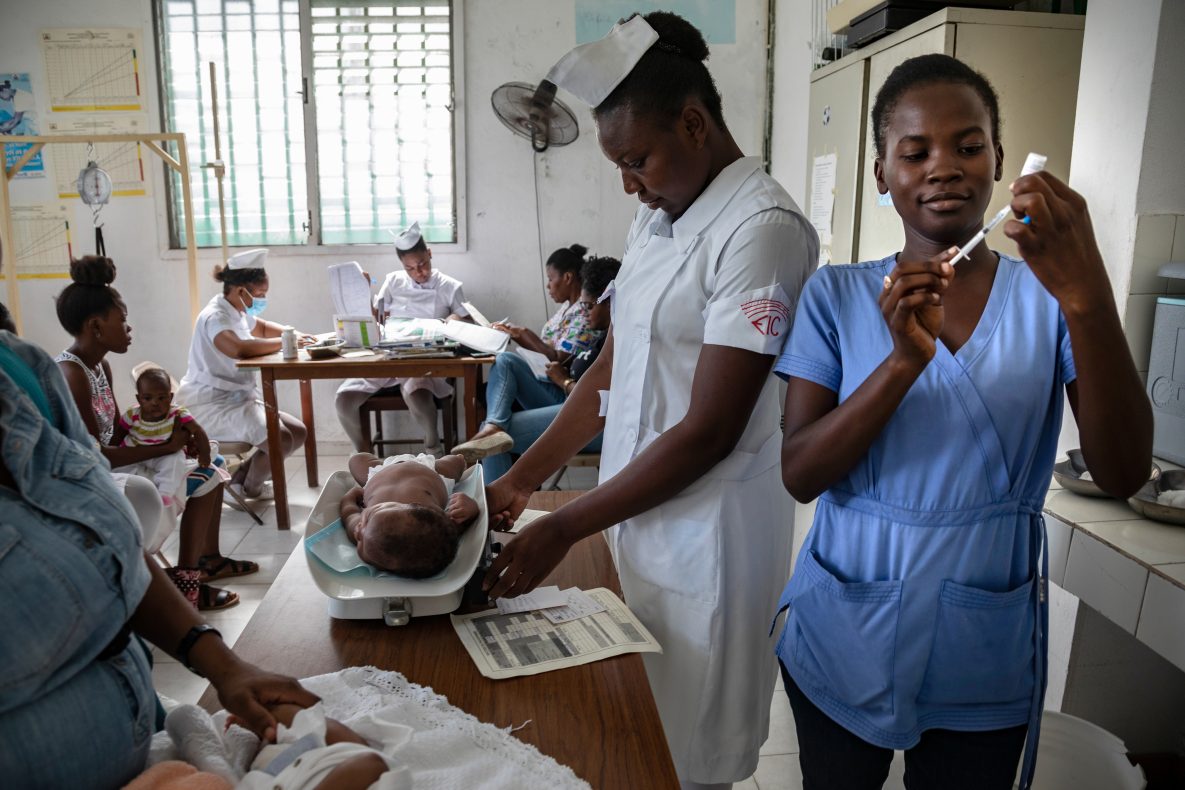
©UNICEF/U.S.CDC/UN#/Rouzier
- Relationships Nurtured by CDC Over Decades Bring Indoor Toilets to Thousands in Northern Haiti During COVID-19 Pandemic
- Training Epidemiologists in Guinea to Respond to Infectious Disease Outbreaks, from Ebola to COVID-19: A First- Person Account by Dr. Salomon Corvil
- Photo Essay: Cholera Response Work in Haiti
- Cholera in Haiti
- Improving Water, Sanitation and Hygiene in Haiti: Past, Present, and Future
- S. Embassy in Haiti (usembassy.gov)
- Haiti | Travelers’ Health | CDC
- Haiti Yellow Book 2024
- Global HIV & TB Haiti country profile | CDC
- Publications: Haiti Articles All Issues | Emerging Infectious Diseases journal | CDC
- Cholera Outbreak — Haiti, September 2022–January 2023 | MMWR (cdc.gov)
- Surveillance in Haiti
- Rabies in Haiti