Current Critical Congenital Heart Defects Screening Activities
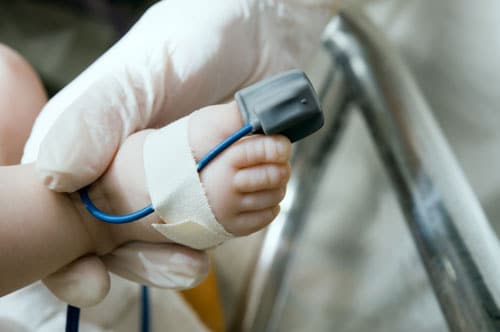
Since 2011, when screening for critical congenital heart defects (CCHDs) was added to the Recommended Uniform Screening Panel for newborn screening,1 CDC has worked to understand how well newborn CCHD screening identifies babies with CCHD, the concerns of state and local governments involved in carrying out screening, and the health outcomes of babies with CCHD. By 2018, all U.S. states and the District of Columbia had implemented CCHD screening policies2.
CDC remains dedicated to learning more about CCHD screening. In 2021, CDC funded eight states to conduct the following activities:
- Ascertaining timing and method of CCHD detection, including CCHD screening
- Linking CCHD screening and birth defects tracking data to evaluate current screening methods
- Monitoring CCHD screening among certain populations (e.g., racial/ethnic groups)
- Using data from screening in practice to examine how well the set of rules for CCHD screening identifies babies with CCHD
- Assessing the impact of CCHD screening and early identification on infant outcomes
These activities can provide important information to assess the impact of CCHD screening across the United States.
Other CDC Activities
CDC’s other tracking and research activities for CCHD screening include:
- Looking at how different states started screening for CCHDs in their hospitals, how many babies with CCHDs have been found, and problems that might impact the success of CCHD screening [Read summary]
- Studying if CCHD screening is good value for the money, or cost-effective, as more states began to screen babies for CCHDs [Read summary]
- Evaluating how much CCHD screening costs for each baby screened [Abstract]
- Learning what factors might impact whether a baby is diagnosed with a CCHD before being sent home from the hospital [Read summary]
- Exploring how birth defects tracking programs and newborn screening programs can work together [Read issue brief [510 KB / 11 pages]]
- Estimating the number of babies with late diagnosed CCHDs that could potentially be detected through screening [Read summary]
- Estimating the number of babies detected and missed with CCHD screening [Read summary]
CHD Projects Across the Lifespan
The Centers for Disease Control and Prevention (CDC) works to identify causes of CHDs and ways to prevent them. We do this through:
- Surveillance or disease tracking:
- CDC funds and coordinates the Metropolitan Atlanta Congenital Defects Program (MACDP). CDC also funds population-based state tracking programs. Birth defects tracking systems are vital to help us find out where and when birth defects occur and whom they affect.
- CDC funds projects to track CHDs across the lifespan to learn about health issues and needs among all age groups.
- CDC, in partnership with March of Dimes, surveyed adults with CHDs to assess their health, social and educational status, and quality of life. The survey is called CH STRONG, Congenital Heart Survey To Recognize Outcomes, Needs, and well-beinG. Read project updates from CH STRONG.
- CDC, along with two funded sites, will survey parents and caregivers of children with CHDs about their child’s healthcare utilization, barriers to care, quality of life, social and educational outcomes, and transition of care from childhood to adulthood as well as needs and experiences of the caregivers.
- Research: CDC funds the Centers for Birth Defects Research and Prevention, which collaborate on large studies such as the National Birth Defects Prevention Study (NBDPS) (births 1997-2011) and the Birth Defects Study To Evaluate Pregnancy exposureS (BD-STEPS) (2014-present). These studies work to identify factors that put babies at risk for birth defects, including heart defects.
- Collaboration:
- CDC promotes collaboration between birth defects tracking programs and newborn screening programs to improve understanding of the effectiveness of CCHD screening.
- CDC provides technical assistance to the Congenital Heart Public Health Consortium (CHPHC). The CHPHC is a group of organizations uniting resources and efforts in public health activities to prevent CHDs and improve outcomes for affected children and adults. Their website provides resources for families and providers on CHDs.
References
2 Glidewell J, Grosse SD, Riehle-Colarusso T, et al. Actions in Support of Newborn Screening for Critical Congenital Heart Disease — United States, 2011–2018. MMWR Morb Mortal Wkly Rep 2019; 68:107–111. DOI: http://dx.doi.org/10.15585/mmwr.mm6805a3