Sodium Intake Among U.S. Adults — 26 States, the District of Columbia, and Puerto Rico, 2013
1; , DrPH1; , PhD1; , PhD1; , PhD1 (Author affiliations at end of text)
Excess sodium intake is a major risk factor for hypertension, and subsequently, heart disease and stroke, the first and fifth leading causes of U.S. deaths, respectively (1). During 2011–2012, the average daily sodium intake among U.S. adults was estimated to be 3,592 mg (2), above the Healthy People 2020 target of 2,300 mg (3). To support strategies to reduce dietary sodium intake, 2013 Behavioral Risk Factor Surveillance System (BRFSS) data from states and territories that implemented the new sodium-related behavior module were assessed. Across 26 states, the District of Columbia (DC), and Puerto Rico, 39%–73% of adults reported taking action (i.e., watching or reducing sodium intake) (median = 51%), and 14%–41% reported receiving advice from a health professional to reduce sodium intake (median = 22%). Compared with adults without hypertension, a higher percentage of adults with self-reported hypertension reported taking action and receiving advice to reduce sodium intake. For states that implemented the module, these results can serve as a baseline to monitor the effects of programs designed to reduce sodium intake.
BRFSS is an annual, random-digit–dialed telephone survey representative of noninstitutionalized, civilian adults aged ≥18 years in each U.S. state and territory. Detailed information on the survey is available at http://www.cdc.gov/brfss. In 2013, 26 states, DC, and Puerto Rico implemented the new, optional sodium-related behavior module. The median American Association of Public Opinion Research location-specific response rate was 48.1% (range = 31.1%–60.3%) (4).
Taking action to reduce sodium intake was defined by a "yes" response to the question, "Are you currently watching or reducing your sodium or salt intake?" Receiving health professional advice to reduce sodium intake was defined by a "yes" response to the question, "Has a doctor or other health professional ever advised you to reduce sodium or salt intake?" Self-reported hypertension was defined by a "yes" response to the question, "Have you ever been told by a doctor, nurse, or other health professional that you have high blood pressure?" The percentage of respondents taking action or receiving advice to reduce sodium intake was estimated for each state overall and by self-reported hypertension status. All estimates were age-standardized using the 2000 U.S. standard projected population. States were categorized in quartiles based on age-standardized proportions of respondents reporting taking action to reduce sodium intake and on proportions reporting having received advice to reduce sodium intake.
A total of 185,463 participants answered questions from the optional sodium module. After excluding 5,396 participants with missing information on key variables, 180,067 participants were included. State sample sizes ranged from 3,332 (Massachusetts) to 12,363 (Minnesota). The proportion of respondents who reported taking action to reduce sodium intake ranged from 38.7% (Utah) to 73.4% (Puerto Rico), with a median of 50.6% (Table 1). Across all participating locations, a higher proportion of participants with hypertension reported taking action to reduce sodium intake compared with those without hypertension (p<0.001 for all comparisons) (Table 1).
The proportion of participants who reported receiving advice from a health professional to reduce sodium intake ranged from 13.5% (Minnesota) to 41.4% (Puerto Rico), with a median of 21.1%. Across all locations, a higher proportion of participants with hypertension reported receiving health professional advice to reduce sodium intake compared with those without hypertension (p<0.001 for all comparisons) (Table 2).
Although only 10 of the 28 survey areas were in the Southern U.S. Census Region,* most of the survey areas with the highest proportions of respondents reporting taking action to reduce sodium intake and most of those with the highest proportion of respondents reporting having received advice from a health professional to reduce sodium intake were in the South. Eight of 10 states in the South were in the top two quartiles for taking action; the two that were not in the top two quartiles were West Virginia and Kentucky (Figure 1). All 10 states in the South were in the top two quartiles for receiving advice. The other four survey areas in the top half were Connecticut, New Jersey, Hawaii, and Puerto Rico (Figure 2).
Discussion
In 2013, across 26 states, DC, and Puerto Rico, the proportion of respondents who reported both taking action and receiving advice to reduce sodium intake varied, with generally higher proportions in states in the Southern U.S. Census Region, Missouri, some states in the Northeastern U.S. Census Region, and Puerto Rico. Overall, approximately half of U.S. adults in participating states and territories reported taking action to reduce sodium intake, and about one in five reported receiving advice from a health professional to reduce sodium intake. Respondents with self-reported hypertension were more likely to take action and receive advice to reduce sodium intake than those without. However, among adults with self-reported hypertension, 20% (Puerto Rico) to 50% (Utah) did not report taking action to reduce sodium intake. In all but four locations (DC, Kentucky, New Jersey, and Puerto Rico), less than half of respondents reported receiving advice to reduce sodium intake. Among adults without hypertension, most did not report taking action to reduce sodium intake, and an even smaller proportion reported receiving professional advice to reduced sodium. These findings suggest an opportunity for promoting strategies to reduce sodium consumption among all adults, with and without hypertension.
This is the first report with state-level estimates of sodium intake behavior among the general population. The geographic pattern of the prevalence of taking action or receiving advice to reduce sodium intake appears to roughly correspond with the pattern of the prevalence of self-reported hypertension (5). BRFSS 2009 data indicate the prevalence of self-reported hypertension is generally higher in the Southern U.S. Census Region, plus Indiana, Michigan, Missouri, Ohio, Pennsylvania, and Rhode Island. A possible explanation for the higher prevalence of taking action and receiving health professional advice to reduce sodium intake in Connecticut and New Jersey could be proximity to New York City's (NYC) media campaign promoting sodium reduction and other NYC and state programs aimed at reducing sodium intake. For example, in April 2013, NYC launched a communication campaign for consumers to purchase lower-sodium foods.†
The finding that Puerto Rico had the highest percentage of respondents both taking action and receiving advice for sodium reduction is new. The high percentages might be related to high hypertension prevalence. Based on 2013 BRFSS data, the prevalence of self-reported hypertension in Puerto Rico was 42.3%, whereas the national prevalence was 31.4% (6).
The findings in this report are subject to at least four limitations. First, BRFSS data are self-reported and subject to recall and social desirability bias, which might overestimate or underestimate prevalence. Second, the methods used by participants to watch or reduce sodium intake were not assessed. Third, these results are not generalizable to the entire United States. Although CDC encouraged states to use the module to assess the sodium-related behavior, the reasons individual states chose to use the module is unknown. Finally, response bias is possible because BRFSS response rates were <50%. Despite these limitations, this report is the first to provide multistate data on sodium-reduction behavior among all BRFSS respondents.
The data in this report highlight the opportunity to increase the proportion of health care professionals who advise their patients to reduce sodium intake and the proportion of U.S. adults who take action to reduce sodium intake. During 2011–2012, approximately 48% of hypertension among U.S. adults was uncontrolled (7). From 2010 to 2030, total direct medical costs of cardiovascular disease are projected to triple, increasing from $273 billion to $818 billion (in 2008 U.S. dollars) (8). Reducing sodium intake by 1,200 mg daily is projected to save $18 billion in health care costs yearly (9). Health care professionals can make a difference by recommending healthy dietary patterns, such as the Dietary Approaches to Stop Hypertension (10). By expanding the use of the sodium-related behavior module, states can enhance the ability to evaluate the effects of sodium-reduction campaigns.
1Division for Heart Disease and Stroke Prevention, National Center for Chronic Disease Prevention and Health Promotion, CDC.
Corresponding author: Jing Fang, jfang@cdc.gov, 770-488-0259.
References
- Kochanek KD, Murphy SL, Xu J, Arias E. Mortality in the United States, 2013. NCHS Data Brief, no. 178. Hyattsville, MD: US Department of Health and Human Services, CDC; 2014. Available at http://www.cdc.gov/nchs/data/databriefs/db178.htm.
- US Department of Agriculture. What we eat in America. NHANES 2011–2012, individuals 2 years and over (excluding breast-fed children), day 1. Available at http://www.ars.usda.gov/SP2UserFiles/Place/80400530/pdf/1112/Table_1_NIN_GEN_11.pdf.
- US Department of Health and Human Services. Healthy People 2020. Nutrition and weight status. Available at http://www.healthypeople.gov/2020/topics-objectives/topic/nutrition-and-weight-status/objectives.
- CDC. Behavioral Risk Factor Surveillance System. 2013 summary data quality report, August 15, 2014. Available at http://www.cdc.gov/brfss/annual_data/2013/pdf/2013_DQR.pdf.
- CDC. Self-reported hypertension and use of antihypertensive medication among adults—United States, 2005–2009. MMWR Morb Mortal Wkly Rep 2013;62:237–44.
- CDC. BRFSS prevalence and trends data. Available at http://www.cdc.gov/brfss/brfssprevalence.
- Ritchey MD, Wall HK, Gillespie C, George MG, Jamal A. Million Hearts: prevalence of leading cardiovascular disease risk factors—United States, 2005–2012. MMWR Morb Mortal Wkly Rep 2014;63:462–7.
- Heidenreich PA, Trogdon JG, Khavjou OA, et al. Forecasting the future of cardiovascular disease in the United States: a policy statement from the American Heart Association. Circulation 2011;123:933–44.
- Bibbins-Domingo K, Chertow GM, Coxson PG, et al. Projected effect of dietary salt reductions on future cardiovascular disease. N Engl J Med 2010;362:590–9.
- Sacks FM, Svetkey LP, Vollmer WM, et al. Effects on blood pressure of reduced dietary sodium and the Dietary Approaches to Stop Hypertension (DASH) diet. N Engl J Med 2001;344:3–10.
* South Census region includes Alabama, Arkansas, Delaware, District of Columbia, Florida, Georgia, Kentucky, Louisiana, Maryland, Mississippi, North Carolina, Oklahoma, South Carolina, Tennessee, Texas, Virginia, and West Virginia.
† Available at http://www.nyc.gov/html/doh/html/pr2013/pr008-13.shtml.
Summary
What is already known on this topic?
National surveillance data show that current sodium intake in the United States is substantially higher than recommended. Excess sodium intake is an important risk factor for hypertension.
What is added by this report?
In 2013, among 26 states, the District of Columbia, and Puerto Rico, the median prevalence of taking action to reduce sodium intake was 51%, ranging from 39% to 73%. The median prevalence of receiving health professional advice to reduce sodium intake was 22%, ranging from 14% to 41%. Although action and advice were higher among hypertensive participants across locations, 20%–50% did not report taking action, and 38%–68% reported not receiving advice to reduce sodium intake.
What are the implications for public health practice?
These data highlight the opportunity to increase the proportion of health professionals who advise their patients to reduce sodium intake and the proportion of U.S. adults who take action to reduce sodium intake.
FIGURE 1. Age-adjusted percentage of adults aged ≥18 years who reported taking action to reduce their dietary sodium intake — 26 states, the District of Columbia, and Puerto Rico, Behavioral Risk Factor Surveillance System, 2013
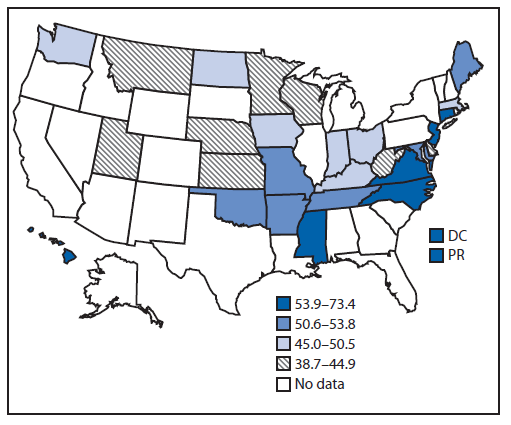
Alternate Text: The figure above is a map showing the age-adjusted percentage of adults aged ≥18 years who reported taking action to reduce their dietary sodium intake in 26 states, the District of Columbia, and Puerto Rico during 2013.
FIGURE 2. Age-adjusted percentage of adults aged ≥18 years who reported being advised by a health professional to reduce dietary sodium intake — 26 states, the District of Columbia, and Puerto Rico, Behavioral Risk Factor Surveillance System, 2013
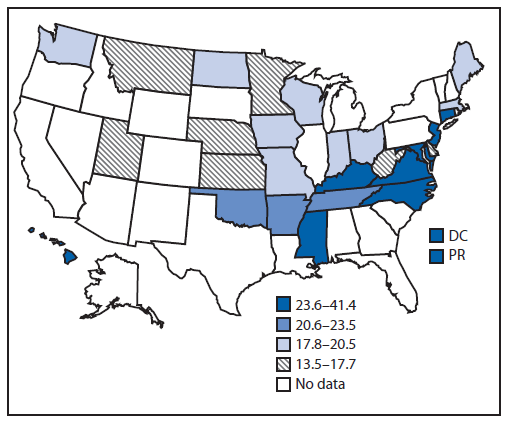
Alternate Text: The figure above is a map showing age-adjusted percentage of adults aged ≥18 years who reported being advised by a health professional to reduce dietary sodium intake in 26 states, the District of Columbia, and Puerto Rico during 2013.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All MMWR HTML versions of articles are electronic conversions from typeset documents.
This conversion might result in character translation or format errors in the HTML version.
Users are referred to the electronic PDF version (http://www.cdc.gov/mmwr)
and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S.
Government Printing Office (GPO), Washington, DC 20402-9371;
telephone: (202) 512-1800. Contact GPO for current prices.
**Questions or messages regarding errors in formatting should be addressed to
mmwrq@cdc.gov.


