Key points
- CDC tracks invasive group A Streptococcus (group A strep) disease using 2 surveillance systems.
- Invasive disease refers to when bacteria invade parts of the body, like blood, that are normally free from germs.
- Rates of serious group A strep disease have been increasing since 2014.
- Preliminary 2023 data indicate the number of serious infections caused by group A strep reached a 20-year high.
- Learn about trends in group A strep disease.

Recent trends
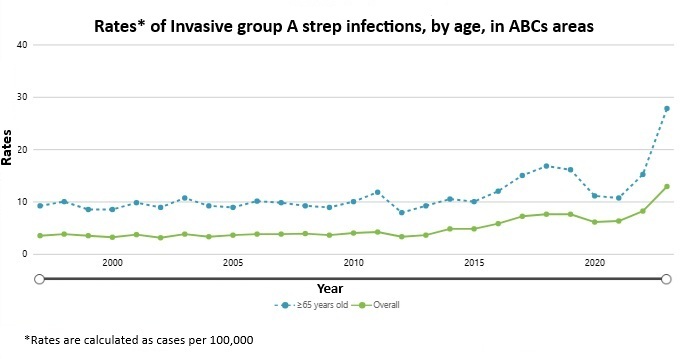
Overall, the number of serious group A strep infections has been increasing in the United States over the past decade.1 The increase has been seen primarily in adults.
While group A strep bacteria circulate year-round, they're more common in December through April ("high season"). Rates of group A strep disease were notably low throughout the year during the COVID-19 pandemic.
Since 2022
Seasonal pattern: The seasonal pattern of group A strep disease activity has returned.
High season: The number of minor and serious group A strep infections during the high season has exceeded what was seen pre-pandemic.
Low season: Low season rates are similar to pre-pandemic rates.
Data systems
National Notifiable Diseases Surveillance System
Streptococcal toxic shock syndrome (STSS) is the only nationally notifiable disease caused by group A strep bacteria.
CDC collects national information about STSS through the National Notifiable Diseases Surveillance System (NNDSS). CDC receives NNDSS data each week.
Active Bacterial Core surveillance
CDC collaborates with some state health departments and academic institutions to conduct group A strep surveillance for invasive disease including:
- Cellulitis with bacteremia (bloodstream infection)
- Necrotizing fasciitis
- Pneumonia with bacteremia
- STSS
Information is collected through Active Bacterial Core surveillance (ABCs), which is part of CDC's Emerging Infections Program.
How the data are interpreted
Invasive disease burden
Looking at U.S. invasive group A strep disease data for the last five years, CDC estimates there were between
- 20,000 to 27,000 cases each year
- 1,800 and 2,400 deaths each year
Invasive disease trends
Adults
The U.S. rates of invasive group A strep disease began increasing in 2014.
The increase was largest among adults aged 18 through 64 years old, but the rate also increased among older adults. Substantial increases in cases among two groups appear to account for much of the change:
- People experiencing homelessness
- People with injection drug use
Children
Rates among children have been stable. However, there was a decrease seen during the COVID-19 pandemic and a subsequent rebound following the pandemic. During the pandemic, measures to reduce the spread of respiratory disease were widely implemented.
Antibiotic resistance
Through ABCs, CDC tracks data on group A strep isolate resistance to certain antibiotics.
Group A strep bacteria aren't resistant to the first-line antibiotics for strep throat: penicillin and amoxicillin.
Estimating non-invasive infections
In the United States
Experts estimate that several million cases of non-invasive group A strep infections occur in the United States each year. Non-invasive group A strep infections include:
For example, strep throat causes an estimated 5.2 million outpatient visits each year among people younger than 65 years old2. These visits result in 2.8 million antibiotic prescriptions each year.
Globally
Globally, the burden from non-invasive group A strep infections is even greater. For example, the World Health Organization estimates that each year3
- Over 100 million children worldwide have impetigo
- Over 600 million have pharyngitis due to group A strep
Trends in seasonality
Group A strep infections can occur any time during the year. However, some infections are more common in the United States in certain seasons:
- Strep throat and scarlet fever: Winter and spring
- Impetigo and other skin infections: Summer
Estimating complications
Complications from group A strep infections include:
In the United States
Acute rheumatic fever incidence is significantly less common in the United States and developed countries compared to less developed countries. However, there's likely significant regional variation as seen in the annual incidence rates shown below:
- American Samoa and Hawaii: 1.1 to 1.5 cases per 1,000 population45
- Tennessee: 0.6 cases per 100,000 population6
- Utah: 3.7 cases per 100,000 population7
Asian and Pacific Islander people are more likely to be hospitalized for acute rheumatic fever compared to White people8:
Globally
Worldwide, rheumatic heart disease remains a significant cause of cardiovascular disease and death. The World Health Organization estimates3:
- 470,000 new cases of acute rheumatic fever occur each year
- 282,000 new cases of rheumatic heart disease occur each year
In 2015, there was an estimated 33.4 million cases of rheumatic heart disease9.
In addition, over 300,000 people die each year from rheumatic heart disease or its complications10.
An estimated 470,000 cases of PSGN occur each year globally3.
Data definitions
The Council of State and Territorial Epidemiologists (CSTE) released the most recent case definition for STSS in 2010.
- Gregory, CJ, Okaro, JO, Reingold, A, et al. Invasive Group A Streptococcal Infections in 10 US States. JAMA. 2025;333(17):1498–1507.
- Lewnard JA, King LM, Fleming-Dutra KE, Link-Gelles R, Van Beneden CA. Incidence of pharyngitis, sinusitis, acute otitis media, and outpatient antibiotic prescribing preventable by vaccination against group A Streptococcus in the United States. Clin Infect Dis. 2021;73(1):e47–e58.
- Carapetis JR, Steer AC, Mulholland EK, Weber M. The global burden of group A streptococcal diseases. Lancet Infect Dis. 2005;5(11):685–94.
- Erdem G, Mizumoto C, Esaki D, et al. Group A streptococcal isolates temporally associated with acute rheumatic fever in Hawaii: Differences from the continental United States. Clin Infect Dis. 2007;45:e20–4.
- Beaudoin A, Edison L, Introcaso CE, Goh L, Marrone J, Mejia A, Van Beneden C. Acute rheumatic fever and rheumatic heart disease among children—American Samoa, 2011–2012. MMWR Morb Mortal Wkly Rep. 2015; 64(20);555–8.
- Land MA, Bisno AL. Acute rheumatic fever: A vanishing disease in suburbia. JAMA. 1983;249(7):895–98.
- Stockmann C, Ampofo K, Hersh AL, et al. Evolving epidemiologic characteristics of invasive group A streptococcal disease in Utah, 2002–2010. Clin Infect Dis. 2012;55(4):479–87.
- Bradley-Hewitt T, Longenecker CT, Nkomo V, et al. Trends and presentation patterns of acute rheumatic fever hospitalisations in the United States. Cardiol Young. 2019;29(11):1387–90.
- Watkins DA, Johnson CO, Colquhoun SM, et al. Global, regional, and national burden of rheumatic heart disease, 1990-2015. N Engl J Med. 2017;377(8):713-722.
- Global Burden of Disease Collaborative Network. Global Burden of Disease Study 2016 (GBD 2016) Results. Seattle, United States: Institute for Health Metrics and Evaluation (IHME), 2017, available at https://vizhub.healthdata.org/gbd-results/ (accessed 20 March 2018).
