International Health Regulations (IHR)
The International Health Regulations (IHR) 2005 are a legally binding agreement of 196 countries to build the capability to detect and report potential public health emergencies worldwide. IHR require that all countries have the ability to detect, assess, report, and respond to public health events.
CDC works with countries around the globe to comply with the IHR (2005). CDC’s global programs address more than 400 diseases, health threats, and conditions that are major causes of death, disease, and disability. Our global programs are run by world leaders in epidemiology, surveillance, informatics, laboratory systems, and other essential disciplines. Through partnerships with other countries’ ministries of health, CDC is improving the quality of critical public health services.
About IHR
With trade and travel expanding on a global level, the opportunity for greater disease spread also increases. The public health and economic impact due to infectious diseases can cause great harm to humans and severely damage a country’s economy. The World Health Assembly first adopted IHR in 1969 to cover six diseases. Over the years, the IHR were revised multiple times. The IHR (2005) is legally binding; all WHO member states must report events of international public health importance. Countries reference IHR (2005) to determine how to prevent and control global health threats while keeping international travel and trade as open as possible.
IHR (2005) requires that all countries have the ability to do the following:
- Detect: Make sure surveillance systems and laboratories can detect potential threats
- Assess: Work together with other countries to make decisions in public health emergencies
- Report: Report specific diseases, plus any potential international public health emergencies, through participation in a network of National Focal Points
- Respond: Respond to public health events
IHR (2005) also includes specific measures countries can take at ports, airports and ground crossings to limit the spread of health risks to neighboring countries, and to prevent unwarranted travel and trade restrictions.
In today’s tightly connected world, a disease can spread from any remote village to any major city on all continents in as little as 36 hours. Recent disease outbreaks, including the COVID-19 pandemic, have demonstrated that a disease threat anywhere is a disease threat everywhere. All countries have a responsibility to one another to build healthcare systems that are strong and that work to identify and contain public health events before they spread.
IHR (2005) is more flexible and future-oriented than previous regulations, requiring countries to consider the possible impact of all hazards, whether they occur naturally, accidentally, or intentionally.1 In spite of broader global agreement to the importance of IHR (2005), only about 1/3 of the countries in the world currently have the ability to assess, detect, and respond to public health emergencies. These gaps in global preparedness leave Americans and the rest of the world vulnerable.
Global health security is not just a health issue; a crisis such Ebola, Zika, or COVID-19 can devastate economies and keep countries from developing. The International Monetary Fund estimates that the COVID-19 pandemic will cost the global economy about $13.8 trillion U.S. dollars through 2024. The impact of this kind of economic devastation reaches farther and wider than ever.2
One of the most important aspects of IHR (2005) is the requirement that countries detect and report events that may constitute a potential public health emergency of international concern (PHEIC).
Under IHR (2005), a PHEIC is declared by the World Health Organization if the situation meets 2 of 4 criteria:
- Is the public health impact of the event serious?
- Is the event unusual or unexpected?
- Is there a significant risk of international spread?
- Is there a significant risk of international travel or trade restrictions?
Once a WHO member country identifies an event of concern, the country must assess the public health risks of the event within 48 hours. If the event is determined to be notifiable under the IHR, the country must report the information to WHO within 24 hours. Some diseases always require reporting under the IHR, no matter when or where they occur, while others become notifiable when they represent an unusual risk or situation.
Always Notifiable:
- Smallpox
- Poliomyelitis due to wild-type poliovirus
- Human influenza caused by a new subtype
- Severe acute respiratory syndrome (SARS)
Other Potentially Notifiable Events:
- May include cholera, pneumonic plague, yellow fever, viral hemorrhagic fever, and West Nile fever, as well as any others that meet the criteria laid out by the IHR.
- Other biological, radiological, or chemical events that meet IHR criteria
Since IHR (2005) was put into place, WHO has declared the following PHEICs:
- H1N1 influenza (2019–2010)
- Polio (2014–Present)
- Ebola (2014–2016) & (2019–2020)
- Zika virus (2016)
- COVID-19 (2020–Present)
- Monkeypox (2022–Present)
When a PHEIC is declared, WHO helps coordinate an immediate response with the affected country and with other countries around the world.
IHR represents an agreement among 196 countries, including all WHO Member States, to work together for global health security.
In the U.S., CDC works with state and local reporting and response networks to receive information at the federal level and then respond to events of concern at the local and federal levels. The Department of Health and Human Services (DHHS) has assumed the lead role in carrying out the reporting requirements for IHR (2005). The Health and Human Services’ Secretary’s Operations Center (SOC) is the National Focal Point responsible for reporting events to WHO. CDC works with other federal agencies to support IHR (2005) implementation.
Being adequately prepared to manage these infectious disease outbreaks is a challenge for many countries. IHR (2005) Monitoring and Evaluation (MEF) provides a roadmap for assessing a country’s health security capacity, enabling them to identify areas for improvement.
IHR MEF is composed of four processes:
- States Parties Self-Assessment Annual Reporting(SPAR),
- Joint External Evaluations, (JEE),
- After Action Reviews(AAR), and
- Simulation Exercises(SimEx).
The SPAR is a mandatory process under IHR (2005); the JEE, AAR, and SimEx are voluntary. Together, these provide a comprehensive approach to assessing a country’s health security capacity and to developing recommendations for how to address associated gaps.
Additionally, results of the JEE and other country-based assessments can be used to guide the development of National Action Plans for Health Security. The NAPHS aims to address gaps in a country’s health security capacity through a system that aligns to the JEE’s recommendations.
When used together, these processes can help governments improve their preparedness against infectious disease threats, gain domestic support for health security work, and direct partners to the areas where more support is needed. To support IHR MEF activities within countries, CDC serves as a major contributor to global public health efforts to prevent, detect, and respond to public health risks.
The Joint External Evaluation (JEE) is a voluntary and comprehensive process to evaluate country capacity across 19 technical areas, to address infectious disease risks through a coordinated response.
The JEE process brings together experts from around the world to help a country assess its strengths and weaknesses and identify recommendations to improve its health security capacity. Multisectoral collaboration, through processes like the JEE, is key to strengthening health systems—this means engaging not just health partners, but other government sectors, such as environmental, agricultural, defense, and finance.
Through the JEE, countries are able to:
- Identify the most critical gaps within their health systems
- Prioritize opportunities for enhanced preparedness and response
- Engage with current and prospective donors and partners to effectively target resources
CDC has collaborated with WHO on developing and refining the JEE process and tools since its inception in 2016. As of April 2022, 115 JEEs have been completed including every country in Africa, representing over half of the UN member states that committed to achieving the goals of the IHR 2005. CDC has provided assistance in over 60% of the JEEs conducted throughout the world and helps countries who have completed this process translate JEE findings and recommendations into action.
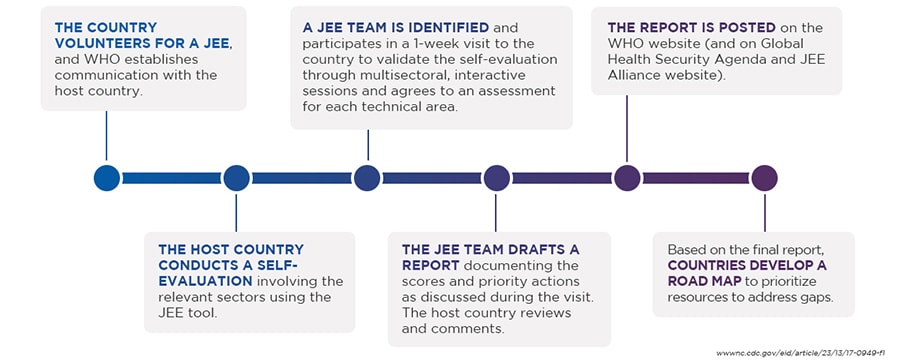
After a JEE is completed, the external experts work with their country counterparts to produce a written report, which includes the scores and all-important priority actions. This report serves as a guide for the country on how to build health security capacity within each technical area. The associated priority actions can feed directly into a National Action Plan for Health Security (NAPHS) and other post-JEE planning processes. JEE results are also published online so that partners can work with countries in a more coordinated fashion to address health security gaps.
CDC supports countries as they develop and strengthen their National Action Plan for Health Security (NAPHS) following a Joint External Evaluation (JEE). Through an all-of-government approach, the NAPHS is developed collectively, with input from different government sectors, and support from international partners. Developing the NAPHS helps countries identify activities that align to the 19 JEE Technical Areas and prioritize them for implementation. The resulting plan details the activities necessary to address gaps within a country’s health security capacity. These activities are then monitored to determine what is working, what needs to be changed, and what to focus on next to continue to build country capacity.
CDC works with partners to generate a NAPHS that is realistic and actionable by providing technical expertise across all stages of development. Specifically, CDC works with partners to facilitate:
- Communication, coordination, and collaboration
- Prioritization, resource mapping, and mobilization
- Implementation and monitoring
- Gostin, Lawrence, The International Health Regulations and beyond; The Lancet, Vol. 4, Issue 10, 606–607.
- Heymann, David L et al., Global health security: the wider lessons from the west African Ebola virus disease epidemic; The Lancet, Vol. 385, Issue 9980, 1884 – 1901.