Case #319 – March, 2012
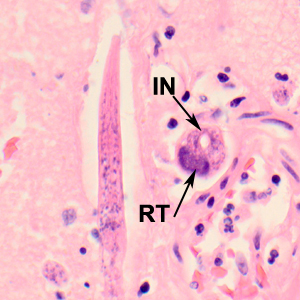
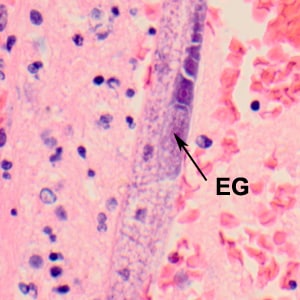
A 65-year-old patient was admitted to the hospital with fever, nausea, and vomiting after recently being treated as an outpatient for a urinary tract infection. Her past medical history included being diagnosed with bipolar disorder, hypertension, osteoarthritis, and compression fractures. She was a smoker and the only known animal contacts were her pet dogs. During hospitalization, her mental health continued to decline and she was pronounced brain-dead after one month’s stay at the hospital. CT and MRI scans of her brain prior to death did not show any focal lesions. An autopsy was performed and cultures of brain tissue were negative for bacterial and viral agents. Sections of brain tissue were processed by Pathology and stained with hematoxylin and eosin (H&E). Figures A–B show what was observed by the attending pathologist. Images were captured and sent to the DPDx Team for diagnostic assistance. What is your diagnosis? Based on what criteria?
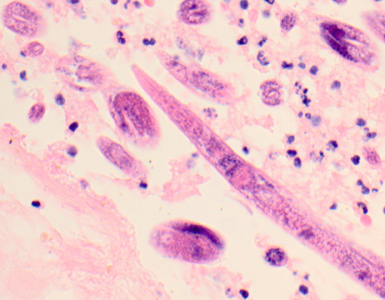
Figure A
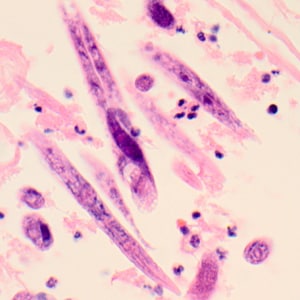
Figure B
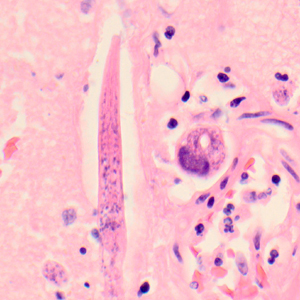
Figure C
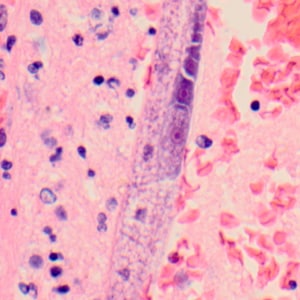
Figure D
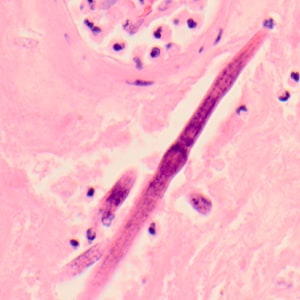
Figure E
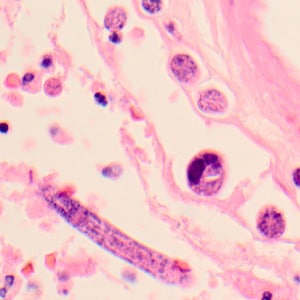
Figure F
This case and images were kindly provided by the University of South Alabama Medical Center, Mobile, AL.
Images presented in the DPDx case studies are from specimens submitted for diagnosis or archiving. On rare occasions, clinical histories given may be partly fictitious.
DPDx is an educational resource designed for health professionals and laboratory scientists. For an overview including prevention, control, and treatment visit www.cdc.gov/parasites/.