Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail.
Cryptosporidiosis Surveillance — United States, 2009–2010
Corresponding author: Jonathan S. Yoder, MPH, Division of Foodborne, Waterborne, and Environmental Diseases, National Center for Emerging and Zoonotic Infectious Diseases, CDC, 1600 Clifton Rd. NE, MS C-09, Atlanta, GA 30329; Telephone: 404-718-4696; Fax: 404-929-1932; E-mail: jyoder@cdc.gov.
Abstract
Problem/Condition: Cryptosporidiosis is a nationally notifiable gastrointestinal illness caused by extremely chlorine-tolerant protozoa of the genus Cryptosporidium.
Reporting Period: 2009–2010.
System Description: Fifty state and two metropolitan public health agencies voluntarily report cases of cryptosporidiosis through CDC's National Notifiable Diseases Surveillance System.
Results: For 2009, 7,656 confirmed and probable cases of cryptosporidiosis (2.5 per 100,000 population) were reported; for 2010, 8,951 confirmed and probable cases (2.9 per 100,000 population) were reported. All jurisdictions reported cryptosporidiosis cases for 2009–2010, and the number of jurisdictions reporting >3.5 cases per 100,000 population was 18 for 2009 and 20 for 2010. Cases were most frequently reported in children aged 1–9 years, followed by adults aged 25–29 years. This is the first reporting period in which more cases of cryptosporidiosis were reported in females than in males. Peak onset of illness occurred during early summer through early fall; the sympton onset of cases in children aged 5–9 years peaked earlier than that of cases reported in adults aged 25–34 years.
Interpretation: Transmission of Cryptosporidium occurs throughout the United States. Rate data from reporting jurisdictions should be compared with caution because individual jurisdictions have varying capacities to detect, investigate, and report cases. The symptom onset and age-specific peaks coincide with the summer recreational water season and might reflect increased use of communal swimming venues (e.g., swimming pools and interactive fountains) by young children who then transmit the parasite to other users and their caregivers.
Public Health Action: Local, state, and federal public health agencies can use cryptosporidiosis surveillance data to characterize the epidemiology of cryptosporidiosis in the United States, establish public health priorities (e.g., research) to improve cryptosporidiosis prevention and control, and design and evaluate efforts (e.g., health communication and policy) to prevent and control the transmission of Cryptosporidium.
Introduction
Cryptosporidiosis is a gastrointestinal illness caused by protozoa of the genus Cryptosporidium, whose taxonomy continues to evolve (1). Revised Cryptosporidium taxonomy based on recent advances in molecular testing methods has revealed that multiple species can infect humans. C. hominis (previously known as C. parvum genotype I) primarily exists in a human-to-human transmission cycle. C. parvum (previously known as C. parvum genotype II) can infect both humans and ruminants (e.g., preweaned calves), each with their own transmission cycles that intersect in zoonotic disease. Molecular techniques are needed to distinguish the morphologically indistinguishable oocysts of the two species. In addition, molecular studies have demonstrated that multiple subtypes of C. parvum and C. hominis can infect humans (2). To a lesser extent, human infections caused by C. felis, C. canis, C. meleagridis, C. suis, C. muris, C. andersoni, and Cryptosporidium cervine, horse, rabbit, skunk, and chipmunk I genotypes also have been documented. Illnesses caused by infection with the different Cryptosporidium species and subtypes within species can differ clinically (3,4).
In immunocompetent persons, cryptosporidiosis is characterized by weight loss, abdominal pain, diarrhea, which can be profuse, usually nonbloody, and watery, as well as anorexia, fatigue, joint pain, headache, fever, and vomiting (5). However, asymptomatic infection also can occur (6–9). Recurrence of symptoms after seeming resolution has been frequently reported; illness is self-limiting, and symptoms most frequently completely resolve within 2–3 weeks (5). Clinical presentation of cryptosporidiosis in HIV-infected patients varies with level of immunosuppression, ranging from no symptoms or transient disease to relapsing, chronic diarrhea or cholera-like diarrhea, which can lead to life-threatening wasting and malabsorption (10). Extraintestinal cryptosporidiosis (i.e., in the biliary or respiratory tract or rarely in the pancreas) has been documented among immunocompromised persons. The incidence of cryptosporidiosis among HIV-infected persons has decreased since the introduction of highly active antiretroviral therapy for HIV infection (11,12). The U.S. Food and Drug Administration approved nitazoxanide in 2004 for the treatment of cryptosporidiosis in immunocompetent children aged 1–11 years and in 2005 in immunocompetent persons aged ≥1 years (13,14). Nitazoxanide has not been demonstrated to be an efficacious treatment of cryptosporidiosis in immunocompromised persons (15,16).
Cryptosporidium oocysts are infectious immediately upon being excreted in feces. Cryptosporidium is transmitted by the fecal-oral route and results from the ingestion of oocysts through the consumption of fecally contaminated food or water or through contact with an infected person or animal. The infectious dose is low; studies have demonstrated that the ingestion of ≤10 C. hominis or C. parvum oocysts can cause infection in healthy persons (17,18). Infected persons have been reported to shed 107–108 oocysts in a single bowel movement (19) and can excrete infectious oocysts for up to 60 days after cessation of gastrointestinal symptoms (20).
Although cryptosporidiosis cases can occur sporadically, outbreaks have been well documented since the first reported U.S. drinking water-associated outbreak in 1984 (21) and the first reported U.S. recreational water–associated outbreak in 1988 (22,23). Cryptosporidium has since emerged as the most frequently recognized cause of recreational water–associated outbreaks, particularly in treated venues (e.g., pools and interactive fountains) (24). Cryptosporidium oocysts are extremely chlorine tolerant and can survive for 3.5–10.6 days in water where free chlorine levels are maintained at CDC-recommended levels of 1–3 mg/L (25). More recent outbreaks of cryptosporidiosis have been reported between various hosts. Foodborne outbreaks of cryptosporidiosis, most notably associated with food handlers who are ill or with ingestion of unpasteurized apple cider (26,27), with outbreaks resulting from person-to-person transmission (particularly in childcare settings (28), and from animal-to-person transmission, also have been reported (29,30).
In 1994, the Council of State and Territorial Epidemiologists (CSTE) called for the reporting of cryptosporidiosis as a nationally notifiable disease; 1995 marked the first full year of reporting. National surveillance data for 1995–2008 have been published elsewhere (31–35). This report summarizes national cryptosporidiosis surveillance data for 2009–2010 and analyzes cryptosporidiosis rates and the annual percentage change in national rates for the years 1995–2010.
Methods
Case Definition
Confirmed and probable cases of cryptosporidiosis are reported voluntarily to CDC. A confirmed case of cryptosporidiosis is defined as detection of Cryptosporidium
- organisms in stool, intestinal fluid, tissue samples, or biopsy specimens;
- antigens in stool or intestinal fluid; or
- nucleic acid by polymerase chain reaction (PCR)-based detection in stool, intestinal fluid, tissue samples, or biopsy specimens (36).
A probable case of cryptosporidiosis is a clinically compatible case that is linked epidemiologically to a confirmed case. This report includes both confirmed and probable cases as reported by jurisdictions.
Testing
If a patient experiences diarrhea lasting >3 days, health-care providers should consider cryptosporidiosis in the differential. To ensure appropriate diagnostic testing, health-care providers should specifically request Cryptosporidium testing, because routine examination of stool for ova and parasites is unlikely to include testing for Cryptosporidium. Oocyst excretion can be intermittent; therefore, the parasite might not be detected in a given stool specimen, so three stool specimens collected on separate days should be examined before considering test results to be negative (37). Commercially available immunoassay kits are available and might be more diagnostically sensitive and specific than routine microscopic examination (38). Direct fluorescent antibody (DFA) testing is an extremely diagnostically sensitive and specific detection method and is considered a benchmark for quality in testing (39). Other immunodiagnostic kits that do not require microscopy (e.g., enzyme immunoassay testing and rapid immunochromatographic cartridge assays) also are available; they do not take the place of routine ova and parasite examination. False-positive results might occur when using rapid immunochromatographic cartridge assays (40); therefore, confirmation by microscopy should be considered.
If PCR-based detection is needed to confirm cryptosporidiosis transmission, health-care providers should contact the state health department or CDC because this specialized testing for Cryptosporidium is not commercially available. PCR-based genotyping and subtyping tools are increasingly being used in outbreak investigations and infection- or contamination-source tracking to differentiate Cryptosporidium species and subtypes. If stool is preserved in formalin, Cryptosporidium isolates cannot be reliably genotyped or subtyped (41).
Reporting
Public health agencies in the 50 states, the District of Columbia (DC), and New York City (NYC) voluntarily report cases of cryptosporidiosis to CDC through the National Notifiable Diseases Surveillance System (NNDSS). Reports include the patient's place of residence (i.e., state and county), age, sex, race, ethnicity (i.e., Hispanic or non-Hispanic), and date of symptom onset, and indicate whether the case is associated with a detected outbreak. Because data on immune status are not collected as part of NNDSS cryptosporidiosis reporting, the number of cryptosporidiosis patients who are immunosuppressed is unknown. Because data in this report were finalized at a different time, the number of cases differs slightly from the number reported in CDC's annual summary of notifiable diseases.
Analysis
National cryptosporidiosis surveillance data for 2009–2010 were analyzed using SAS v.9.3 (SAS Institute Inc.; Cary, North Carolina). Population data from the U.S. Census Bureau using intercensal estimates for April 1, 2000 to July 1, 2010 were used to calculate rates by year, reporting jurisdiction, age, and sex.
Data were analyzed regionally on the basis of the U.S. Census Bureau-defined Northeast, Midwest, South, and West regions (42). To account for differences in the seasonal use of recreational water, the West region was further subdivided into Northwest and Southwest.
Results
The total number of reported cases of cryptosporidiosis increased 16.9% from 7,656 for 2009 to 8,951 for 2010 (Table 1). This followed a peak of 11,657 in 2007 (Figure 1). The rate of reported cases was 2.5 and 2.9 per 100,000 population in 2009 and 2010, respectively. The annual rate of reported cryptosporidiosis in the United States was relatively stable during 1995–2004, ranging from 0.4–1.3 per 100,000 population. Rates during 2005–2010 ranged from 2.3–3.9 per 100,000 population, peaking in 2007 (34).
Of cases reported for 2009 and 2010, 2.6% and 3.3%, respectively, were reported to be associated with a detected outbreak. All 50 states and two metropolitan jurisdictions reported cryptosporidiosis cases during the reporting period. By region, the rate of reported cryptosporidiosis cases per 100,000 population ranged from 1.5 in the Southwest to 4.3 in the Midwest in 2009 and 1.4 in the Southwest to 6.4 in the Midwest in 2010 (Table 1, Figure 2). By reporting jurisdiction, the rate of reported cryptosporidiosis cases per 100,000 population ranged from 0.1 in Hawaii to 17.1 in South Dakota in 2009 and 0.1 in Hawaii to 17.4 in Wisconsin in 2010. The number of jurisdictions reporting rates of >3.5 cases per 100,000 population was 18 in 2009 and 20 in 2010.
During 2009–2010, the date of symptom onset was reported nationally for 12,226 (73.6%) of the 16,607 cases reported. The number of cases by symptom onset peaked in mid-August (n = 1,077), which was 4.5 times larger than the lowest number of cases by symptom onset in late December (n = 237) (Figure 3). Increased reporting (>400 cases reported biweekly) was noted during June–September.
National surveillance data displayed a bimodal age distribution; cases were most frequently reported in children aged 1–9 years, followed by adults aged 25–29 years (Figure 4). In 2009, the rate of reported cryptosporidiosis was highest in children aged 1–4 years (5.3 per 100,000 population) and lowest in adults aged 50–54 years (1.5 per 100,000 population). The percentage of cases among males was 46.4% (3,464 of 7,656) and 48.3% (4,295 of 8,951) in 2009 and 2010, respectively (Table 2). The annual incidence rate by sex ranged from 2.3 to 2.9 per 100,000 population for males and females (Table 2, Figure 5). Cryptosporidiosis rates were higher among males aged 1–4 years than among females of the same age group. Conversely, females had a higher rate among persons aged 20–39 years. Symptom onset of cryptosporidiosis in children peaked earlier in the summer than among adults.
Of patients for whom race was reported, 85.4% (4,891 of 5,724) and 86.2% (5,977 of 6,933) were white in 2009 and 2010, respectively. Of patients for whom ethnicity was reported, 10.6% (512 of 4,811) and 9.5% (571 of 5,982) were Hispanic in 2009 and 2010, respectively (Table 2). Annually, data on race were missing for approximately one fourth of cases reported; data on ethnicity were missing for approximately one third of cases reported.
Discussion
National surveillance data are used to help characterize the epidemiology of cryptosporidiosis in the United States. In 2009 and 2010, the total number and rate of cases reported annually decreased from that of 2007, but represent a marked increase compared with annual statistics before 2005 (Figure 1). Whether the persistently elevated annual case counts and rates reflect changes in diagnostic testing practices, reporting patterns, or a change in infection and disease caused by Cryptosporidium remains unclear. The increased annual number of reported cases and rates during 2005–2010 might be the result of an increase in the number of communitywide and large (e.g., >1,000 cases) cryptosporidiosis outbreaks (24,43–51). Further, 2009 and 2010 had the lowest annual proportion of cases reported to be associated with detected cryptosporidiosis outbreaks since national reporting began in 1995 (32–35). This coincided with a decrease in the number of reported communitywide and large cryptosporidiosis outbreaks during 2009–2010.
The number of reported cases and cost of cryptosporidiosis in the United States continue to be substantial. Approximately 748,000 cryptosporidiosis cases occur annually (52). Each year, hospitalizations resulting from cryptosporidiosis cost an estimated $45.8 million; additionally, each ambulatory care visit for cryptosporidiosis costs $267–$757, depending on the patient's type of health-care insurance coverage (53). The high incidence and cost of cryptosporidiosis underscores the need for a better understanding of cryptosporidiosis epidemiology in the United States, particularly of risk factors, to optimize prevention and control. Prevention and control measures include 1) practicing good hygiene (e.g., not swimming when ill with diarrhea and washing hands appropriately); 2) avoiding contaminated water (e.g., not swallowing recreational water), using secondary or supplementary treatment systems (e.g., ultraviolet irradiation or ozonation) to inactivate Cryptosporidium in treated recreational water venues, and treating and filtering drinking water to inactivate or remove the parasite sufficiently; 3) exercising caution when traveling; and 4) avoiding fecal exposure during sexual activity (Box).
The geographic variation, age distribution, and early-summer through early-fall seasonality described here are consistent with findings of previous reports on U.S. national cryptosporidiosis surveillance data (32–35). Cryptosporidiosis is widespread geographically in the United States, with all 50 states and two metropolitan jurisdictions reporting cryptosporidiosis cases during 2009–2010. The cryptosporidiosis rate in the Midwest region was 1.3–2.9 times greater than that of the other regions in 2009 and 1.8–4.6 times greater than that of other regions in 2010. It is difficult to determine whether this disparity is the result of regional differences in the capacity to detect, investigate, or report cases, or if true regional differences exist in the transmission of Cryptosporidium. If the latter is correct, the increased cryptosporidiosis rate in the Midwest region might be linked to increased contact with preweaned calves (54,55).
Although cryptosporidiosis affects persons in all age groups, the number of reported cryptosporidiosis cases and rates were highest among children aged 1–4 years, followed by those aged 5–9 years and adults aged 25–29 years (Figure 4). Similar findings also have been noted in U.S. state, Canadian provincial, Australian state, and national Finnish and United Kingdom surveillance data (56–61). Among patients aged 1–4 years, the rate was higher in males; among those aged 20–39 years, the rate was higher in females. These data might reflect Cryptosporidium transmission from young children to their caregivers (e.g., childcare staff, family members, and other household contacts) (28).
Cryptosporidium can be transmitted by ingesting contaminated food and water or from contact with infected persons or animals. Several studies have characterized risk factors associated with cryptosporidiosis. Persons at increased risk for infection include those who have exposure to recreational water (73,74); have contact with livestock, particularly preweaned calves (73,75,76); have ingested untreated drinking water (75); are close contacts of infected persons (e.g., those in the same family or household or in childcare settings) (73,74,76); or who have traveled to areas where the disease is endemic (73,76). These risk factors vary by geographic setting (e.g., rural or urban) and by the Cryptosporidium species identified in the ill person (77).
The five-fold increase in cryptosporidiosis symptom onset during the summer, similarly observed in previous reports from the U.S. and other countries (56–59,61), is consistent with increased use of treated recreational water venues during the summer, particularly among younger children (24,43–51,62–64). Cryptosporidium has become the leading cause of reported treated recreational water–associated outbreaks of gastroenteritis (24). Transmission through recreational water is facilitated by the substantial number of Cryptosporidium oocysts that can be shed by a single person, the extended periods of time that oocysts can be shed (20,65), the low infectious dose (18,66), and the tolerance of Cryptosporidium oocysts to chlorine (25).
Recreational water can amplify smaller outbreaks into communitywide transmission when persons who are ill visit multiple recreational water venues or introduce the parasite to other settings (e.g., child care centers or schools) (67). To prevent communitywide outbreaks, CDC has collaborated with state health departments to develop guidelines for rapidly implementing communitywide control measures once an increase in case reporting exceeds a preoutbreak disease action threshold (e.g., an outbreak or a twofold to threefold increase in cases over baseline) rather than waiting for an outbreak investigation to implicate a specific source of transmission (62).
Reducing the transmission of this highly infectious, extremely chlorine-tolerant pathogen in treated recreational water venues (e.g., pools) requires a multipronged approach. Effective prevention requires that swimmers practice healthy swimming behaviors (e.g., keeping the parasite out of the water by not swimming while ill with diarrhea and, if diagnosed with cryptosporidiosis, at least 2 weeks following recovery). Once the parasite has been introduced into the water, engineering (e.g., secondary or supplemental disinfection systems or enhanced filtration) can minimize contamination and help control Cryptosporidium transmission.
Low infectious dose (18,19) and extreme chlorine tolerance (25) also make Cryptosporidium ideally suited for transmission through drinking water. To prevent Cryptosporidium transmission through drinking water, the U.S. Environmental Protection Agency (EPA) has implemented regulations designed to enhance the treatment of surface water supplies, including multiple regulatory changes enacted following a massive outbreak of cryptosporidiosis in 1993 in Milwaukee, Wisconsin (68). Subsequently, no cryptosporidiosis outbreaks associated with the use of community surface water supplies have been detected in the United States (44,46,47,49,69–72), highlighting the potential benefits of these regulations. To address the risk for outbreaks and illness associated with use of groundwater sources, EPA also is implementing the Groundwater Rule, which requires additional treatment and filtration of certain public ground water (e.g., well) systems (69).
In the United States, no federal agency regulates the design, construction, operation, and maintenance of treated recreational water venues. Pool codes are reviewed and approved by state or local public health officials. This lack of uniform national standards has been identified as a barrier to the prevention and control of outbreaks associated with treated recreational water venues. To provide support to state and local health departments, CDC is sponsoring development of the Model Aquatic Health Code (MAHC) (http://www.cdc.gov/healthywater/swimming/pools/mahc). MAHC is a collaborative effort between local, state, and federal public health and the aquatics sector to develop a data-driven, knowledge-based resource for state and local jurisdictions reviewing and updating their existing pool codes to optimally prevent and control recreational water–associated illness.
Limitations
The findings in this report are subject to at least three limitations. First, NNDSS data are incomplete on race, ethnicity, and symptom onset date, and do not include data on exposures and immune status of patients. Second, the cryptosporidiosis rate is likely to be underestimated by these national surveillance data because of underreporting (e.g., not all infected persons are symptomatic, persons who are symptomatic do not always seek medical care, health-care providers do not always include laboratory diagnostics in their evaluation of nonbloody diarrheal diseases, laboratories typically do not include Cryptosporidium testing in routine examination of stool for ova and parasites, case reports are not always completed for positive laboratory results or forwarded to public health officials). Third, confirmed cases of cryptosporidiosis based on false-positive results following the use of rapid cartridge assays might have been included.
Conclusion
The quality and completeness of national cryptosporidiosis data can be improved by enhancing the capacity of state and local jurisdictions to detect, investigate, and voluntarily report cases (78). Existing state and local public health infrastructure supported through CDC (e.g., FoodNet and Environmental Health Specialists Network [EHS-Net] Water Program) could facilitate enhancement of surveillance efforts. Although many jurisdictions investigate cryptosporidiosis cases, risk-factor data are not available for all jurisdictions via NNDSS. Collaborating with reporting jurisdictions to improve CDC's ability to access jurisdictional risk factor data would enhance national collection efforts while simplifying analysis of these data as well as their comparison with data from other sources (e.g., FoodNet) (73). The systematic collection and molecular characterization of Cryptosporidium isolates would further the understanding of U.S. cryptosporidiosis epidemiology by revealing transmission patterns and potential risk factors (79). Such an effort would require phasing out the practice of preserving stool specimens with formalin, which decreases the ability to perform molecular amplification methods. CDC is preparing to pilot Crypto Net, the first U.S. molecular surveillance system for parasites, to better understand the transmission of cryptosporidiosis in the United States.
CDC can further optimize the quality of national surveillance data by investigating reports of and factors associated with false-positive cryptosporidiosis results (e.g., testing for Cryptosporidium when the testing method is not indicated, user error, or problems with test validity) when using rapid cartridge assays (40) (e.g., conducting a head-to-head comparison of rapid cartridge assays to DFA), and responding accordingly. Establishing standards for how diagnostic methods are integrated into the case definition will improve the stability of NNDSS data and allow for the interpretation of national reporting trends.* Additionally, advocating for the incorporation of Cryptosporidium testing in standard ova and parasite testing, and educating health-care providers to specifically name request testing for Cryptosporidium, might also improve data quality.
Improving the completeness and quality of national surveillance data will better direct the design and evaluation of health communication and policy efforts to prevent and control cryptosporidiosis. In response to the increased case counts and rates of cryptosporidiosis and treated recreational water–associated outbreaks of cryptosporidiosis, CDC has developed two websites: Cryptosporidiosis (available at http://www.cdc.gov/parasites/crypto) and Healthy Swimming (available at http://www.cdc.gov/healthywater/swimming/index.html). The websites target multiple audiences (e.g., state and local public health partners, the aquatics sector, and the public) and provide resources (e.g., for responding to cryptosporidiosis outbreaks) and recommendations (e.g., on inactivation of Cryptosporidium in treated recreational water or preventing and controlling Cryptosporidium transmission in child care settings). National surveillance data can be used to guide the revision, updating, and expansion of health communication efforts and other public health interventions (e.g., MAHC) to prevent and control cryptosporidiosis.
Acknowledgments
This report is based, in part, on contributions by jurisdiction surveillance coordinators Ruth Ann Jajosky, DMD, and Willie Anderson, Office of Surveillance, Epidemiology, and Laboratory Services, CDC.
References
- Xiao L, Fayer R, Ryan U, Upton SJ. Cryptosporidium taxonomy: recent advances and implications for public health. Clin Microbiol Rev 2004;17:72–97.
- Xiao L. Molecular epidemiology of cryptosporidiosis: an update. Exp Parasitol 2010;124:80–9.
- Cama VA, Bern C, Roberts J, et al. Cryptosporidium species and subtypes and clinical manifestations in children, Peru. Emerg Infect Dis 2008;14:1567–74.
- Cama VA, Ross JM, Crawford S, et al. Differences in clinical manifestations among Cryptosporidium species and subtypes in HIV-infected persons. J Infect Dis 2007;196:684-91.
- Hunter PR, Hughes S, Woodhouse S, et al. Sporadic cryptosporidiosis case-control study with genotyping. EID 2004;10:1241–9.
- Hellard ME, Sinclair MI, Hogg GG, Fairley CK. Prevalence of enteric pathogens among community based asymptomatic individuals. J Gastroenterol Hepatol 2000;15:290–3.
- Pettoello-Mantovani M, Di Martino L, Dettori G, et al. Asymptomatic carriage of intestinal Cryptosporidium in immunocompetent and immunodeficient children: a prospective study. Pediatr Infect Dis J 1995;14:1042–7.
- Davies AP, Campbell B, Evans MR, Bone A, Roche A, Chalmers RM. Asymptomatic carriage of protozoan parasites in children in day care centers in the United Kingdom. Pediatr Infect Dis J 2009;28:838–40.
- Horman A, Korpela H, Sutinen J, Wedel H, Hanninen ML. Meta-analysis in assessment of the prevalence and annual incidence of Giardia spp. and Cryptosporidium spp. infections in humans in the Nordic countries. Int J Parasitol 2004;34:1337–46.
- Hunter PR, Nichols G. Epidemiology and clinical features of Cryptosporidium infection in immunocompromised patients. Clin Microbiol Rev 2002;15:145–54.
- Brady MT, Oleske JM, Williams PL, et al. Declines in mortality rates and changes in causes of death in HIV-1–infected children during the HAART era. J Acquir Immune Defic Syndr 2010;53:86–94.
- Kaplan JE, Hanson D, Dworkin MS, et al. Epidemiology of human immunodeficiency virus-associated opportunistic infections in the United States in the era of highly active antiretroviral therapy. Clin Infect Dis 2000;30 (Suppl) 1:S5–14.
- U.S. Food and Drug Administration. Alinia (nitazoxanide) label. Approved July 21, 2004.
- U.S. Food and Drug Administration. Alinia (nitazoxanide) label. Approved June 16, 2005.
- Abubakar I, Aliyu SH, Arumugam C, Usman NK, Hunter PR. Treatment of cryptosporidiosis in immunocompromised individuals: systematic review and meta-analysis. Br J Clin Pharmacol 2007;63:387–93.
- Amadi B, Mwiya M, Sianongo S, et al. High dose prolonged treatment with nitazoxanide is not effective for cryptosporidiosis in HIV positive Zambian children: a randomised controlled trial. BMC Infect Dis 2009;9:195.
- Chappell CL, Okhuysen PC, Langer-Curry R, et al. Cryptosporidium hominis: experimental challenge of healthy adults. Am J Trop Med Hyg 2006;75:851–7.
- Okhuysen PC, Chappell CL, Crabb JH, Sterling CR, DuPont HL. Virulence of three distinct Cryptosporidium parvum isolates for healthy adults. J Infect Dis 1999;180:1275–81.
- Goodgame RW, Genta RM, White AC, Chappell CL. Intensity of infection in AIDS-associated cryptosporidiosis. J Infect Dis 1993;167:704–9.
- Jokipii L, Jokipii AM. Timing of symptoms and oocyst excretion in human cryptosporidiosis. New Engl J Med 1986;315:1643–7.
- D'Antonio RG, Winn RE, Taylor JP, et al. A waterborne outbreak of cryptosporidiosis in normal hosts. Ann Intern Med 1985;103:886–8.
- CDC. Swimming-associated cryptosporidiosis—Los Angeles County. MMWR 1990;39:343–5.
- Sorvillo FJ, Fujioka K, Nahlen B, et al. Swimming-associated cryptosporidiosis. Am J Public Health 1992;82:742–4.
- Hlavsa MC, Roberts VA, Anderson AR, et al. Surveillance for waterborne disease outbreaks and other health events associated with recreational water—United States, 2007–2008. MMWR 2011;60(No. SS-12).
- Shields JM, Hill VR, Arrowood MJ, Beach MJ. Inactivation of Cryptosporidium parvum under chlorinated recreational water conditions. J Water Health 2008;6:513–20.
- Smith HV, Caccio SM, Cook N, Nichols RA, Tait A. Cryptosporidium and Giardia as foodborne zoonoses. Vet Parasitol 2007;149:29–40.
- Blackburn BG, Mazurek JM, Hlavsa M, et al. Cryptosporidiosis associated with ozonated apple cider. Emerg Infect Dis 2006;12:684–6.
- Cordell RL, Addiss DG. Cryptosporidiosis in child care settings: a review of the literature and recommendations for prevention and control. Pediatr Infect Dis J 1994;13:310–7.
- CDC. Cryptosporidiosis outbreak at a summer camp—North Carolina, 2009. MMWR 2011;60:918–22.
- Chalmers RM, Giles M. Zoonotic cryptosporidiosis in the UK: challenges for control. J Appl Microbiol 2010;109:1487–97.
- Dietz VJ, Roberts JM. National surveillance for infection with Cryptosporidium parvum, 1995–1998: what have we learned? Public Health Rep 2000;115:358–63.
- Hlavsa MC, Watson JC, Beach MJ. Cryptosporidiosis surveillance—United States 1999–2002. MMWR 2005;54(No. SS-1).
- Yoder JS, Beach MJ; CDC. Cryptosporidiosis surveillance—United States, 2003–2005. MMWR 2007;56(No. SS-7).
- Yoder JS, Beach MJ. Cryptosporidium surveillance and risk factors in the United States. Exp Parasitol 2010;124:31–9.
- Yoder JS, Harral C, Beach MJ. Cryptosporidiosis surveillance—United States, 2006–2008. MMWR 2010;59:1–14.
- CDC. Cryptosporidiosis (Cryptosporidium) 2009 case definition. Available at http://www.cdc.gov/osels/ph_surveillance/nndss/casedef/cryptosporidiosis_2009.htm. Accessed March 13, 2012.
- van Gool T, Weijts R, Lommerse E, Mank TG. Triple Faeces Test: an effective tool for detection of intestinal parasites in routine clinical practice. Eur J Clin Microbiol Infect Dis 2003;22:284–90.
- Johnston SP, Ballard MM, Beach MJ, Causer L, Wilkins PP. Evaluation of three commercial assays for detection of Giardia and Cryptosporidium organisms in fecal specimens. J Clin Microbiol 2003;41:623–6.
- Arrowood MJ, Sterling CR. Comparison of conventional staining methods and monoclonal antibody-based methods for Cryptosporidium oocyst detection. J Clin Microbiol 1989;27:1490–5.
- Robinson TJ, Cebelinski EA, Taylor C, Smith KE. Evaluation of the positive predictive value of rapid assays used by clinical laboratories in Minnesota for the diagnosis of cryptosporidiosis. Clin Infect Dis 2010;50:53–5.
- Lalonde LF, Gajadhar AA. Effect of storage media, temperature, and time on preservation of Cryptosporidium parvum oocysts for PCR analysis. Vet Parasitol 2009;160:185–9.
- U.S. Census Bureau. Census regions and divisions of the United States. Available at http://www.census.gov/geo/www/us_regdiv.pdf. Accessed June 12, 2012.
- Yoder JS, Hlavsa MC, Craun GF, et al. Surveillance for waterborne disease and outbreaks associated with recreational water use and other aquatic facility-associated health events—United States, 2005–2006. MMWR 2008;57(No. SS-9).
- Barwick RS, Levy DA, Craun GF, Beach MJ, Calderon RL. Surveillance for waterborne-disease outbreaks—United States, 1997–1998. MMWR 2000;49(No. SS-4).
- Herwaldt BL, Craun GF, Stokes SL, Juranek DD. Waterborne-disease outbreaks, 1989–1990. MMWR 1991;40(No. SS-3).
- Kramer MH, Herwaldt BL, Craun GF, Calderon RL, Juranek DD. Surveillance for waterborne-disease outbreaks—United States, 1993–1994. MMWR 1996;45(No. SS-1).
- Lee SH, Levy DA, Craun GF, Beach MJ, Calderon RL. Surveillance for waterborne-disease outbreaks—United States, 1999–2000. MMWR 2002;51(No. SS-8).
- Levine WC, Stephenson WT, Craun GF. Waterborne disease outbreaks, 1986–1988. MMWR 1990;39(No. SS-1).
- Levy DA, Bens MS, Craun GF, Calderon RL, Herwaldt BL. Surveillance for waterborne-disease outbreaks—United States, 1995–1996. MMWR 1998;47:1–34.
- Moore AC, Herwaldt BL, Craun GF, Calderon RL, Highsmith AK, Juranek DD. Surveillance for waterborne disease outbreaks—United States, 1991–1992. MMWR 1993;42(No. SS-5).
- Yoder JS, Blackburn BG, Craun GF, et al. Surveillance for waterborne-disease outbreaks associated with recreational water—United States, 2001–2002. MMWR 2004;53(No. SS-8).
- Scallan E, Hoekstra RM, Angulo FJ, et al. Foodborne illness acquired in the United States—major pathogens. Emerg Infect Dis 2011;17:7–15.
- Collier SA, Stockman LJ, Hicks LA, et al. Direct healthcare costs of selected diseases primarily or partially transmitted by water. Epidemiol Infect 2012;11:1–11.
- Santin M, Trout JM, Xiao L, et al. Prevalence and age-related variation of Cryptosporidium species and genotypes in dairy calves. Vet Parasitol 2004;122:103–17.
- Xiao L, Zhou L, Santin M, Yang W, Fayer R. Distribution of Cryptosporidium parvum subtypes in calves in eastern United States. Parasitol Res 2007;100:701–6.
- Chalmers RM, Smith R, Elwin K, Clifton-Hadley FA, Giles M. Epidemiology of anthroponotic and zoonotic human cryptosporidiosis in England and Wales, 2004–2006. Epidemiol Infect 2011;139:700–12.
- Laupland KB, Church DL. Population-based laboratory surveillance for Giardia sp. and Cryptosporidium sp. infections in a large Canadian health region. BMC Infect Dis 2005;5:72.
- Majowicz SE, Michel P, Aramini JJ, McEwen SA, Wilson JB. Descriptive analysis of endemic cryptosporidiosis cases reported in Ontario, 1996–1997. Can J Public Health 2001;92:62–6.
- Naumova EN, Chen JT, Griffiths JK, et al. Use of passive surveillance data to study temporal and spatial variation in the incidence of giardiasis and cryptosporidiosis. Public Health Rep 2000;115:436–47.
- Rimhanen-Finne R, Sakari Jokiranta T, Virtanen MJ, Kuusi M. Giardia and Cryptosporidium infection in Finland: a registry-based study of their demographic determinants. APMIS 2011;119:735–40.
- Waldron LS, Dimeski B, Beggs PJ, Ferrari BC, Power ML. Molecular epidemiology, spatiotemporal analysis, and ecology of sporadic human cryptosporidiosis in Australia. Appl Environ Microbiol 2011;77:7757–65.
- CDC. Communitywide cryptosporidiosis outbreak—Utah, 2007. MMWR 2008;57:989–93.
- Dziuban EJ, Liang JL, Craun GF, et al. Surveillance for waterborne disease and outbreaks associated with recreational water—United States, 2003–2004. MMWR 2006;55(No. SS-12).
- St Louis ME. Water-related disease outbreaks, 1985. MMWR 1988;37(No. SS-2).
- Chappell CL, Okhuysen PC, Sterling CR, DuPont HL. Cryptosporidium parvum: intensity of infection and oocyst excretion patterns in healthy volunteers. J Infect Dis 1996;173:232–6.
- DuPont HL, Chappell CL, Sterling CR, et al. The infectivity of Cryptosporidium parvum in healthy volunteers. New Engl J Med 1995;332:855–9.
- Turabelidze G, Lin M, Weiser T, Zhu BP. Communitywide outbreak of cryptosporidiosis in rural Missouri associated with attendance at child care centers. Arch Pediatr Adolesc Med 2007;161:878–83.
- Mac Kenzie WR, Hoxie NJ, Proctor ME, et al. A massive outbreak in Milwaukee of Cryptosporidium infection transmitted through the public water supply. New Engl J Med 1994;331:161–7.
- Brunkard JM, Ailes E, Roberts VA, et al. Surveillance for waterborne disease outbreaks associated with drinking water—United States, 2007–2008. MMWR 2011;60(No. SS-12).
- Yoder J, Roberts V, Craun GF, et al. Surveillance for waterborne disease and outbreaks associated with drinking water and water not intended for drinking—United States, 2005–2006. MMWR 2008;57:39–62.
- Liang JL, Dziuban EJ, Craun GF, et al. Surveillance for waterborne disease and outbreaks associated with drinking water and water not intended for drinking—United States, 2003–2004. MMWR 2006;55:31–65.
- Blackburn BG, Craun GF, Yoder JS, et al. Surveillance for waterborne-disease outbreaks associated with drinking water—United States, 2001–2002. MMWR 2004;53(No. SS-8).
- Roy SL, DeLong SM, Stenzel SA, et al. Risk factors for sporadic cryptosporidiosis among immunocompetent persons in the United States from 1999 to 2001. J Clin Microbiol 2004;42:2944–51.
- Robertson B, Sinclair MI, Forbes AB, et al. Case-control studies of sporadic cryptosporidiosis in Melbourne and Adelaide, Australia. Epidemiol Infect 2002;128:419–31.
- Goh S, Reacher M, Casemore DP, et al. Sporadic cryptosporidiosis, North Cumbria, England, 1996-2000. Emerg Infect Dis 2004;10:1007–15.
- Hunter PR, Hughes S, Woodhouse S, et al. Sporadic cryptosporidiosis case-control study with genotyping. Emerg Infect Dis 2004;10:1241–9.
- Chalmers RM, Smith R, Elwin K, Clifton-Hadley FA, Giles M Epidemiology of anthroponotic and zoonotic human cryptosporidiosis in England and Wales, 2004-2006. Epidemiol Infect. 2011;139:700–12
- National Association of County and City Health Officials. Local health department job losses and program cuts: findings from the July 2011 survey.
- Chalmers RM, Elwin K, Thomas AL, Guy EC, Mason B. Long-term Cryptosporidium typing reveals the aetiology and species-specific epidemiology of human cryptosporidiosis in England and Wales, 2000 to 2003. Euro Surveill 2009;14:2.
* In 2011, the CDC/CSTE national cryptosporidiosis case definition changed, reflecting that cases diagnosed by rapid cartridge assays are classified as probable cases.
|
TABLE 1. (Continued) Number, percentage,* and rate† of cryptosporidiosis, by region/state — National Notifiable Diseases Surveillance System, United States, 2009–2010 |
||||||||
|---|---|---|---|---|---|---|---|---|
|
Region/State |
2009 |
2010 |
||||||
|
No. |
(%) |
Rate |
No. outbreak cases§ |
No. |
(%) |
Rate |
No. outbreak cases |
|
|
Northwest |
491 |
(6.4) |
3.4 |
14 |
513 |
(5.7) |
3.6 |
27 |
|
Alaska |
8 |
(0.1) |
1.1 |
6 |
(0.1) |
0.8 |
||
|
Idaho |
98 |
(1.3) |
6.3 |
110 |
(1.2) |
7.0 |
||
|
Montana |
57 |
(0.7) |
5.8 |
49 |
(0.5) |
4.9 |
||
|
Oregon |
199 |
(2.6) |
5.2 |
14 |
218 |
(2.4) |
5.7 |
27 |
|
Washington |
102 |
(1.3) |
1.5 |
102 |
(1.1) |
1.5 |
||
|
Wyoming |
27 |
(0.4)) |
4.8 |
28 |
(0.3) |
5.0 |
||
|
Southwest |
845 |
(11.0) |
1.5 |
0 |
806 |
(9.0) |
1.4 |
3 |
|
Arizona |
34 |
(0.4) |
0.5 |
40 |
(0.4) |
0.6 |
||
|
California |
459 |
(6.0) |
1.2 |
384 |
(4.3) |
1.0 |
||
|
Colorado |
138 |
(1.8) |
2.8 |
134 |
(1.5) |
2.7 |
||
|
Hawaii |
1 |
(0.0) |
0.1 |
1 |
(0.0) |
0.1 |
||
|
Nevada |
25 |
(0.3) |
0.9 |
38 |
(0.4) |
1.4 |
3 |
|
|
New Mexico |
149 |
(1.9) |
7.3 |
137 |
(1.5) |
6.6 |
||
|
Utah |
39 |
(0.5) |
1.4 |
72 |
(0.8) |
2.6 |
||
|
Total |
7,656 |
(100.0) |
2.5 |
201 |
8,951 |
(100.0) |
2.9 |
298 |
|
Sources: Population estimates are from the U.S. Census Bureau. Intercensal estimates of the resident population for the United States, regions, states, and Puerto Rico: April 1, 2000 to July 1, 2010. Available at http://www.census.gov/popest/data/index.html. Estimates of the New York City population are from Intercensal estimates of the resident population for counties: April 1, 2000 to July 1, 2010 (summing populations of Bronx, Kings, New York, Richmond, and Queens counties). Available at http://www.census.gov/popest/data/intercensal/county/county2010.html. * Percentages might not total 100% because of rounding. † Incidence per 100,000 population on the basis of U.S. Census Bureau population estimates. § Number of cases linked to a suspected outbreak. ¶ New York State case reports include New York City. |
||||||||
FIGURE 1. Incidence* of cryptosporidiosis, by year — National Notifiable Diseases Surveillance System, United States, 1995–2010†
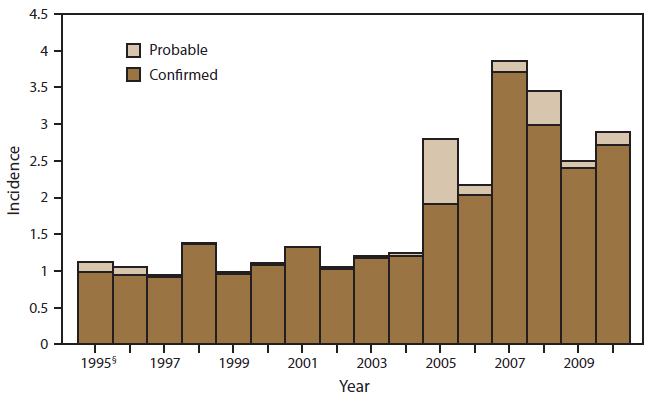
* Per 100,000 population.
† N = 85,514.
§ First full year of national reporting.
Alternate Text: This figure is a bar graph that reflects the incidence (per 100,000 population) of cryptosporidiosis, by year, during 1995-2009, as reported to the National Notifiable Diseases Surveillance System, United States. Incidence is classified using one of three descriptions: probable, confirmed, and non-outbreak. The number of cases reported during 2009-2010 decreased from the previous reporting periods but remain historically elevated. The rate of reported cryptosporidiosis in the United States was stable during 1995-2003, with annual rates ranging 0.4-1.3/100,000 population and an annual increase of 1.4%. During 2003-2007, the annual rate of reported cryptosporidiosis cases increased by 32.5% each year. Incidence rates peaked in 2007 at 3.9 per 100,000 population. During 2007-2010, incidence rates declined 10.5% per year.
FIGURE 2. Incidence* of cryptosporidiosis, by reporting jurisdiction — National Notifiable Diseases Surveillance System, United States, 2010
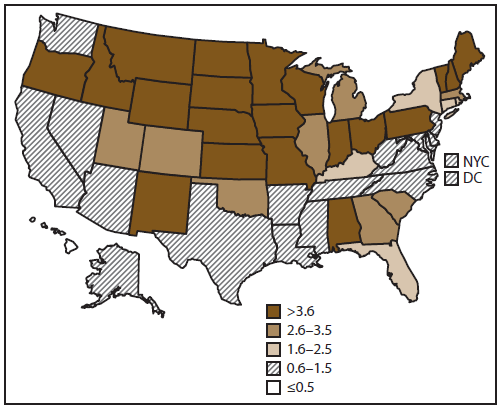
Abbreviations: NYC = New York City, DC = District of Columbia.
* Per 100,000 population.
Alternate Text: This figure is a U.S. map that shows the number and rate (per 100,000 population) of cryptosporidiosis reported in each state, by reporting jurisdiction, for 2010, as reported to the National Notifiable Diseases Surveillance System, United States. By region, the rate of reported cryptosporidiosis cases per 100,000 population ranged from 1.5 in the Southwest to 4.3 in the Midwest in 2009 and 1.4 in the Southwest to 6.4 in the Midwest in 2010.
FIGURE 3. Number* of cryptosporidiosis case reports, by date of symptom onset — National Notifiable Diseases Surveillance System, United States, 2009–2010
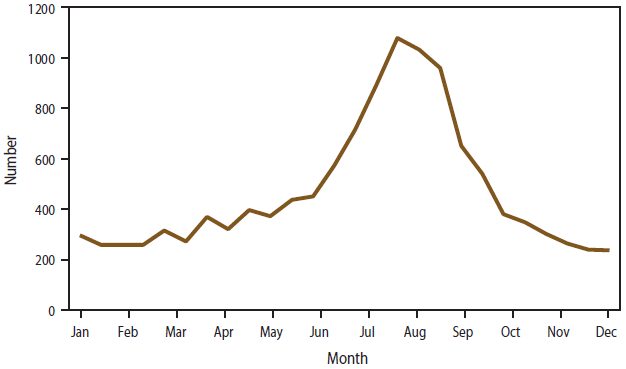
* N = 16,607; date of onset for 4,381 patients was unknown.
Alternate Text: This figure is a line graph that reflects the number of cryptosporidiosis case reports, by month of symptom onset, as reported to the National Notifiable Diseases Surveillance System, United States. During 2009-2010, the date of symptom onset was reported for 12,226 (73.6%) of the 16,607 cases reported. The number of cases by symptom onset peaked in mid-August (n = 1,077), which was 4.5 times larger than the lowest number of cases by symptom onset in late December (n = 237).
FIGURE 4. Number* and average annual rate† of cryptosporidiosis case reports, by age group and year—National Notifiable Diseases Surveillance System, United States, 2009–2010
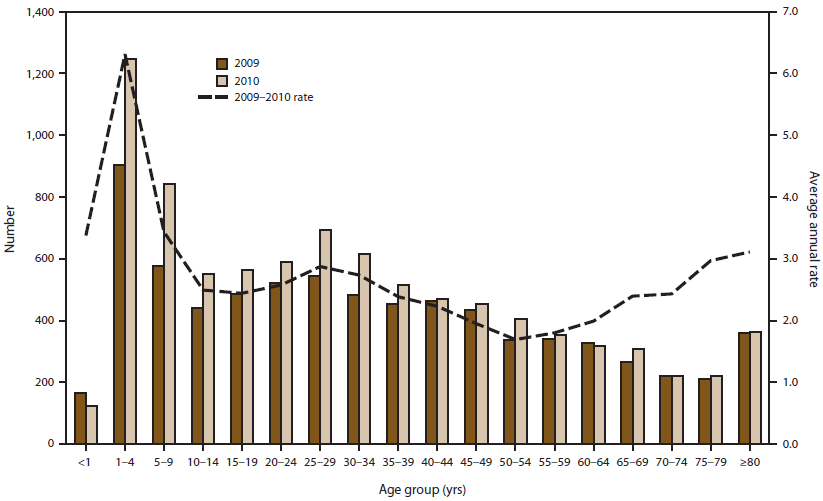
* N = 16,607; age for 214 patients was unknown.
† Incidence per 100,000 population.
Alternate Text: This figure is a bar graph with a trend line that presents the number and rate (per 100,000 population) of cryptosporidiosis case reports, by age group and year, for 2009-2010, as reported to the National Notifiable Diseases Surveillance System, United States. The graph shows that the number of reported cryptosporidiosis cases and rates were highest among children aged 1-4 years, followed by those aged 5-9 years, and then adults aged 25-29 years.
|
TABLE 2. Number, percentage*, and rate† of cryptosporidiosis, by selected patient demographic characteristics — National Notifiable Diseases Surveillance System, United States, 2009–2010 |
||||||
|---|---|---|---|---|---|---|
|
Characteristic |
2009 |
2010 |
||||
|
No. |
(%) |
Rate |
No. |
(%) |
Rate |
|
|
Sex |
||||||
|
Male |
3,464 |
(45.2) |
2.3 |
4,295 |
(48.0) |
2.8 |
|
Female |
3,998 |
(52.2) |
2.6 |
4,605 |
(51.4) |
2.9 |
|
Missing |
194 |
(2.5) |
— |
51 |
(0.6) |
— |
|
Race§ |
||||||
|
Alaska Native/American Native |
32 |
(0.4) |
— |
56 |
(0.6) |
— |
|
Asian Pacific Islander |
60 |
(0.8) |
— |
67 |
(0.7) |
— |
|
Black |
544 |
(7.1) |
— |
617 |
(6.9) |
— |
|
White |
4,891 |
(63.9) |
— |
5,977 |
(66.8) |
— |
|
Other |
197 |
(2.6) |
— |
216 |
(2.4) |
— |
|
Missing |
1,932 |
(25.2) |
— |
2,018 |
(22.5) |
— |
|
Ethnicity§ |
||||||
|
Hispanic |
512 |
(6.7) |
— |
571 |
(6.4) |
— |
|
Non-Hispanic |
4,299 |
(56.2) |
— |
5,411 |
(60.5) |
— |
|
Missing |
2,845 |
(37.2) |
— |
2,969 |
(33.2) |
— |
|
Total |
7,656 |
(100.0) |
2.5 |
8,951 |
(100.0) |
2.9 |
|
Source: Population estimates are from the U.S. Census Bureau. Intercensal estimates of the resident population by sex and age for the United States: April 1, 2000 to July 1, 2010. Available at http://www.census.gov/popest/data/intercensal/national/nat2010.html. * Percentages might not total 100% because of rounding. † Incidence per 100,000 population on the basis of U.S. Census Bureau population estimates. § Rates by race and ethnicity are not reported because of the high percentage of unreported race and ethnicity. |
||||||
FIGURE 5. Incidence* of cryptosporidiosis, by sex and age group — National Notifiable Diseases Surveillance System, United States, 2009–2010
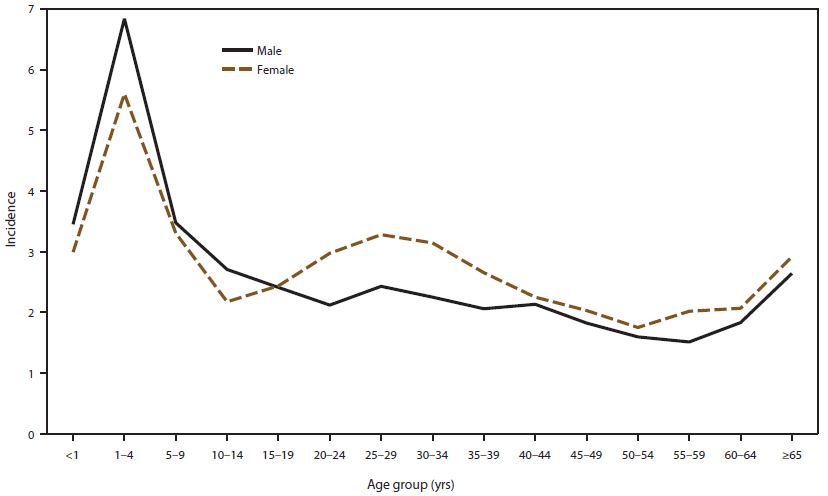
* Per 100,000 population.
Alternate Text: This figure is a line graph that reflects the incidence of cryptosporidiosis, by sex and age group (persons aged <1 year->65 years), for 2009-2010, as reported to the National Notifiable Diseases Surveillance System, United States. The graph shows that the annual incidence rate by sex ranged from 2.3 to 2.9 per 100,000 population for males and females.
|
BOX. CDC recommendations to prevent and control cryptosporidiosis |
|---|
|
Practice good hygiene.
Information about hand hygiene is available from CDC at http://www.cdc.gov/healthywater/hygiene/hand/handwashing.html. Note: Cryptosporidium oocysts are not effectively inactivated by alcohol-based hand sanitizers.
Information about recreational water illnesses and how to stop them from spreading is available from CDC at http://www.cdc.gov/healthywater/swimming.
Avoid water (drinking and recreational) that might be contaminated.
Information about water filters is available from CDC at http://www.cdc.gov/parasites/crypto/gen_info/filters.html. Avoid eating food that might be contaminated.
Practice extra caution when traveling. Information about how to prevent illnesses while traveling is available from CDC at http://wwwnc.cdc.gov/travel/content/safe-food-water.aspx. Prevent contact and contamination with feces during sex.
__________________________ Information about cryptosporidiosis prevention and control is available from CDC at http://www.cdc.gov/parasites/crypto/prevention.html. |
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of Health and Human Services. |
All MMWR HTML versions of articles are electronic conversions from typeset documents. This conversion might result in character translation or format errors in the HTML version. Users are referred to the electronic PDF version (http://www.cdc.gov/mmwr) and/or the original MMWR paper copy for printable versions of official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices.
**Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.


