PrEP for HIV Prevention in the U.S.
Pre-exposure prophylaxis (PrEP) is medicine that reduces a person’s chances of getting HIV from sex or injection drug use. It is safe and highly effective when taken as prescribed. The U.S. Food and Drug Administration approved the first PrEP for HIV prevention in 2012. Today, PrEP can be taken in the form of pills or shots. CDC estimates that 1.2 million people could benefit from PrEP in the United States.
- U.S. is making substantial progress in PrEP for HIV prevention.
- About 30% of people who could benefit from PrEP were prescribed it in 2021, compared to only about 13% in 2017.
- PrEP coverage remains drastically uneven.
- Most people who could benefit from PrEP are Black/African American (subsequently “Black”) or Hispanic/Latino, but CDC data suggest relatively few Black or Hispanic/Latino people have been prescribed it.
- PrEP coverage also varies widely by race/ethnicity and by sex.
- Major new investments are required to increase PrEP
- The cost of PrEP drugs and care is not the main obstacle to PrEP use for the vast majority of people who could benefit.
- However, additional strategies and resources are needed to address remaining gaps and address unmet needs to increase PrEP awareness and use.
- CDC works with partners to help make PrEP as accessible as possible.
Notable gains have been made in the use of PrEP as a key prevention strategy for ending the HIV epidemic in the United States. CDC data show that about 30% of the estimated 1.2 million people who could benefit from PrEP were prescribed it in 2021, compared to only about 13% in 2017.
The growth in PrEP use, along with improved testing and treatment, has played a part in recent decreases in new HIV infections, including a 12% overall decline—and a more substantial decline among 13- to 24-year-old gay and bisexual males—from 2017 to 2021.
Despite these positive trends, HIV prevention efforts must go further and faster for progress to reach all populations equitably and achieve a national goal for 50% of people who could benefit from PrEP to be using it by 2025. This effort is part of a broader federal initiative to end the U.S. HIV epidemic by 2030.
Many longstanding social and economic factors—including transphobia, stigma, experiencing homelessness or unemployment, and others—have made it more difficult for transgender women to access services and have put them at greatly increased chances of getting HIV. A recent CDC study found that 4 in 10 transgender women in seven major U.S. cities have HIV. Expanding PrEP use among transgender women is key to decreasing new HIV infections in this population.
The survey showed that just 32% of HIV-negative transgender women reported using PrEP, even though 92% were aware of the medication. Previous studies have also revealed high knowledge of PrEP and its benefits but very low uptake among transgender women.
Deeply entrenched social determinants of health continue to drive disparities in HIV treatment and prevention outcomes. Rates of new HIV infections are almost eight times higher among Black people—and almost four times higher among Hispanic/Latino people— than among White people.
Although most people who could benefit from PrEP are Black or Hispanic/Latino, CDC data suggest relatively few Black or Hispanic/Latino people have been prescribed it.
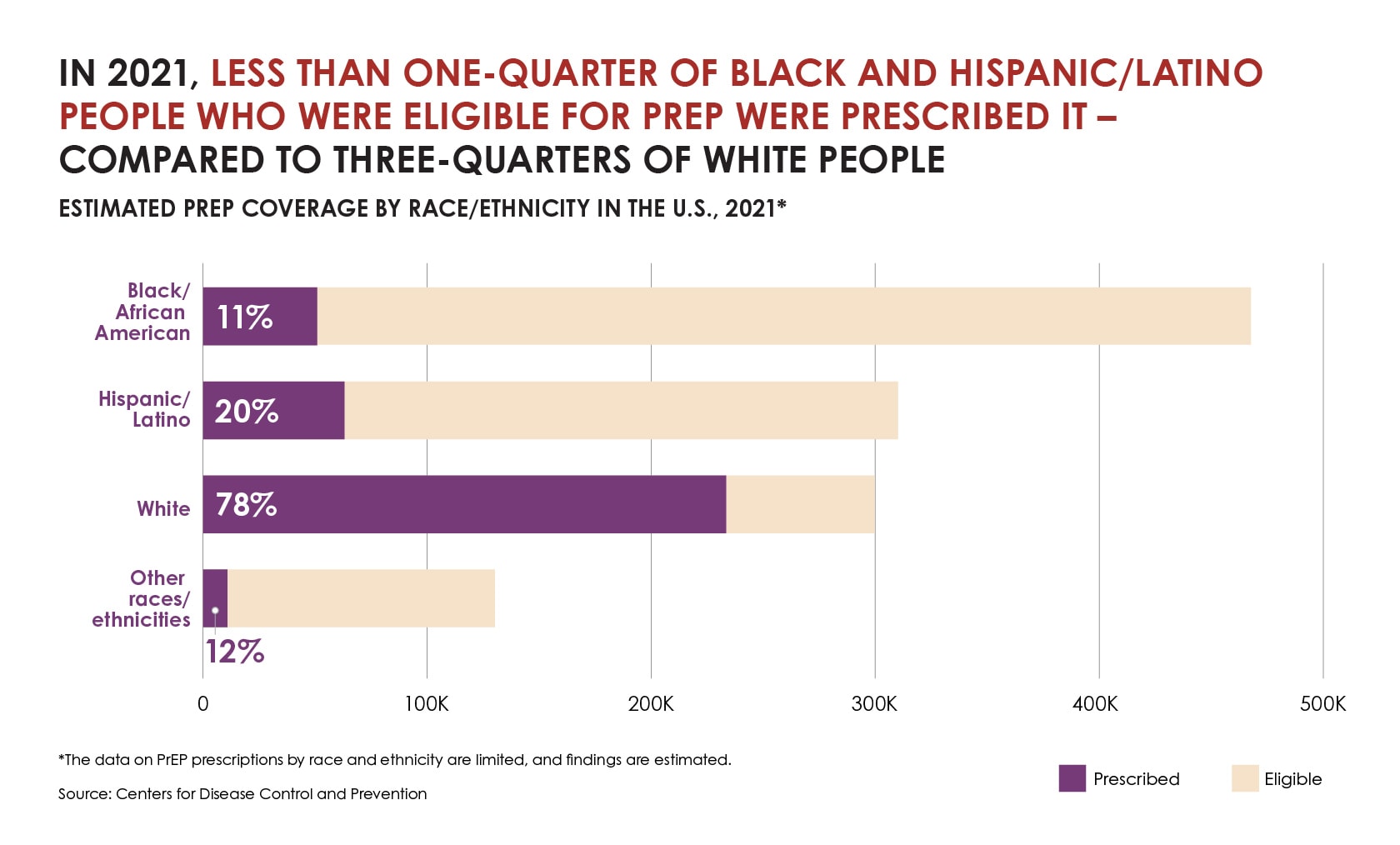
In 2021, less than on-quarter of black and Hispanic/Latino people who were eligible for prep were prescribed it-compared to three-quarters of white people.
PrEP coverage is also unevenly distributed among people based on sex, with coverage almost three times as high among males (34%) as among females (12%). Addressing this imbalance is critical. About one-fifth of new HIV infections in 2021 were among women,1 and over half of those were among Black women.
To end the HIV epidemic, we must ensure equitable access to HIV treatment and prevention, including PrEP. This will require increased investments in outreach, education, and services, as well as efforts to address the root causes and social determinants that contribute to HIV disparities. These include poverty, housing instability, unequal access to health care, lack of education, stigma, and systemic racism.
Additional CDC data on PrEP uptake are available here.
Major New Investments Required to Increase PrEP Uptake
Since the first studies documenting its effectiveness, CDC has worked with partners to increase use of PrEP and is continuing work to accelerate those efforts with available resources.
However, substantial barriers remain, and HIV prevention resources have not kept pace with prevention needs. For example, allocated funding has consistently fallen short of Presidents’ requests for the federal Ending the HIV Epidemic in the U.S. (EHE) initiative. EHE strives for 50% of people who could benefit from PrEP to be prescribed it by 2025, in part by accelerating PrEP use in geographic areas severely affected by HIV.
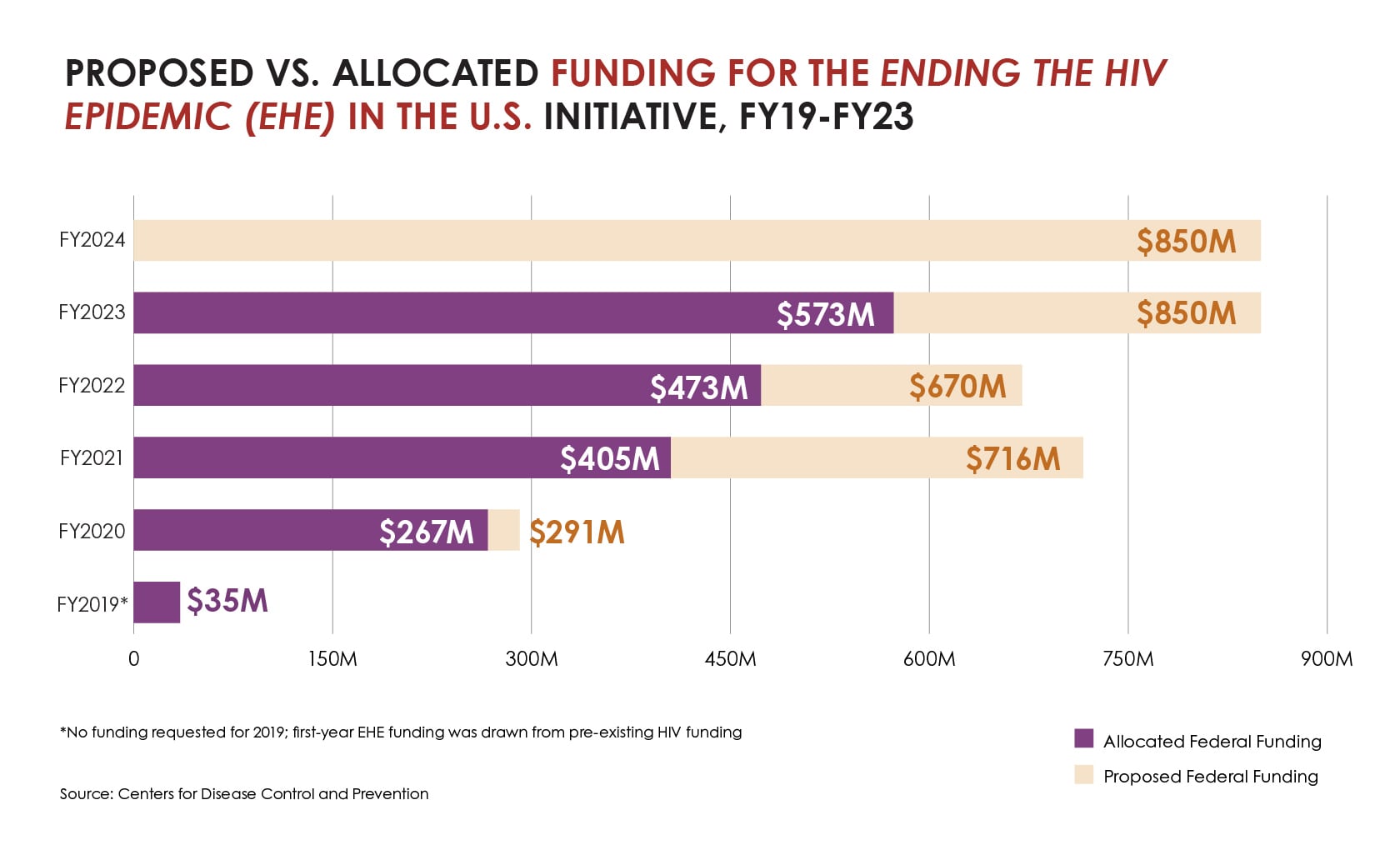
Proposed vs. allocated funding for the ending the HIV epidemic (EHE) in THE U.S. initiative, FY19-FY23
And while the President has requested $237 million to begin a national PrEP program since 2022, Congress has not yet provided any resources for this additional effort.
The increased resources that the President has requested for HIV prevention are vital to overcome the barriers that hinder PrEP uptake, including lack of knowledge; lack of trusted or easily accessible PrEP providers; and—for some—continued financial barriers to PrEP medications and clinical services.
Fortunately, a recent CDC analysis found the number of people who face financial barriers to PrEP drugs and services has been cut in half in recent years. The decline is due in large part to Medicaid expansion and requirements that PrEP medications and clinical services be covered with no cost-sharing under the Affordable Care Act (ACA). A separate recent analysis prepared for the HIV+Hepatitis Policy Institute by researchers at RTI International indicates the most substantial unmet resource need is for community and provider outreach and patient navigation services needed to increase PrEP awareness and use.
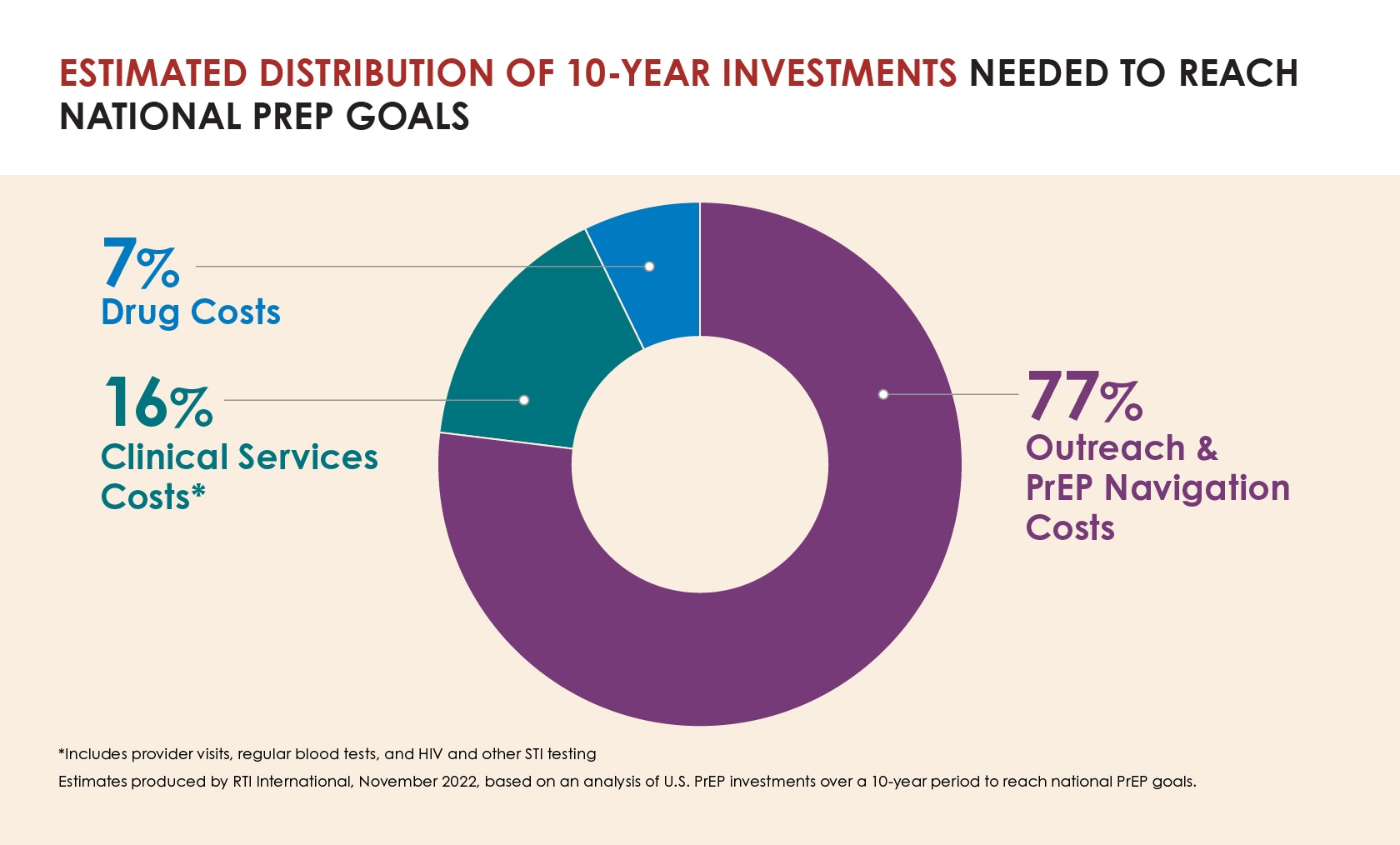
Estimated distribution of 10-year investments needed to reach national prep goals.
Though cost of drugs and care is not the main obstacle to PrEP use for the vast majority of people who need it, CDC estimates 4% of people who could benefit from PrEP continue to face these barriers. Additional strategies are needed to address these remaining gaps and support PrEP uptake for this group.
1 Based on assigned sex at birth. Data for gender are not provided because the estimates for transgender people and people of additional gender identity are too small to report.
Even with substantial funding gaps, CDC and its state, local, and federal partners are continuing to maximize all available resources and innovations to reach as many people with PrEP as possible.
While CDC received less than a quarter of the new resources the President requested for the agency to accelerate its areas of the federal EHE initiative in 2023, CDC plans to invest the majority of the increase in projects specifically designed to increase knowledge about, demand for, access to, and persistent use of PrEP among populations that are disproportionately affected by HIV. Key projects funded include:
- Expanding campaigns to address disparities in awareness and use of PrEP: CDC is launching a new social marketing campaign to increase PrEP awareness and use among Black and Hispanic/Latino gay and bisexual men and will be expanding its “She’s Well” campaign to reach more Black women.
- Furthering innovation and outreach in EHE jurisdictions: Through EHE, CDC has provided increased funds to strengthen key HIV prevention strategies, including PrEP uptake, in 57 priority areas. Funds may be used for community outreach, education, peer support to navigate care, as well as mobile units, pop-up sites, telehealth, and other novel engagement strategies to increase PrEP uptake. Funds may also be used for laboratory costs for screening or monitoring PrEP where needed. To further expand these efforts, CDC is providing additional resources in 2023 to allow jurisdictions to partner with new community-based organizations or clinics.
Expanding PrEP provision in STI clinics: STI clinics can play a vital role in reaching groups at risk for HIV who may not otherwise have access to healthcare services. CDC has increased funding for HIV prevention services, including PrEP delivery, in STI specialty clinics in EHE jurisdictions from $3 million in 2020 to $14 million in 2023.
- Studying ways to increase PrEP use through multiple PrEP options: CDC’s “PrEP Choice” study has been funded to implement and evaluate provider education and support tools designed to help increase PrEP counseling, initiation, adherence, and persistence among gay and bisexual men using daily, intermittent, or injectable PrEP. The project will also collect data on the factors leading to the selection of a particular PrEP regimen and patterns of use to help guide future programs.
These expanded efforts build upon longstanding CDC programs to increase the use of PrEP and other proven prevention strategies:
- CDC requires state and local health departments that receive any of the agency’s approximately $400 million annual HIV prevention and surveillance funding to incorporate PrEP into their local strategies. Activities focus on education, training, communication, and linking people who would benefit to providers.
- CDC is also providing up to $282 million in funding to more than 135 community-based organizations to increase use of PrEP and other key prevention strategies among populations most severely affected by HIV, including Black and Hispanic/Latino people, gay and bisexual men, transgender women, Black cisgender women, and people who inject drugs.

