Food Safety Differences Between Restaurants Linked and Not Linked to Outbreaks
EHS-Net Recommends
Restaurants should consider requiring kitchen manager food-safety certification from a high-quality training program.
More research is needed to find out how to reduce outbreaks caused by infected food handlers. In the meantime, restaurants should stress the importance of managing illness of food workers.

Why This Study Was Done
Each year, roughly 1 in 6 people in the United States gets sick from eating contaminated food. We need to know the causes of foodborne illness outbreaks so we can prevent future outbreaks. This study focused on restaurants because they are the most common place for outbreaks to occur.
What the Study Described
This study described how restaurant traits (for example, number of meals served), policies, and practices were linked to foodborne illness outbreaks and to infected food workers as the cause of outbreaks.
What the Study Found
EHS-Net found that restaurants with kitchen managers certified in food safety were less likely to have foodborne illness outbreaks.
Description of Outbreaks
- Outbreaks of norovirus were the most common (45%).
- The most common causes of outbreaks were infected food workers (65%) and workers touching food with their bare hands (35%).
Restaurant Traits Linked to Outbreaks
Outbreak and nonoutbreak restaurants were similar on these traits:
- Ownership (chain vs. independent).
- Number of meals served.
- Food-safety training.
- Language barriers.
- Sick leave pay.
- Policies to keep sick workers from working.
Outbreak restaurants were less likely to have
- A certified kitchen manager (CKM) on staff.
- Food-safety certification training provided by a state or local agency.
- Food-safety certification training provided by a restaurant corporation.
Outbreak restaurants were more likely to be
- Sit-down restaurants.
- Classified as ethnic restaurants.
Outbreak restaurants with CKMs were less likely than outbreak restaurants without CKMs to have had outbreaks
- Of norovirus and Clostridium perfringens.
- Caused by workers touching food with their bare hands.
Within outbreak restaurants, CKMs were more likely than other managers to be familiar with the Hazard Analysis Critical Control Point (HACCP) system. All CKMs were familiar with the HACCP food-safety system recommended by the U.S. Food and Drug Administration. Twenty percent of other managers were familiar with HACCP.
Restaurant Traits Linked to Infected Food Handlers
Kitchen manager certification, sick leave pay, and policies to keep sick workers from working did not lower rates of infected food handlers as a cause of outbreaks.
Restaurant Traits Linked to Outbreaks
Outbreak and nonoutbreak restaurants were similar on these traits:
- Ownership (chain vs. independent).
- Number of meals served.
- Food-safety training.
- Language barriers.
- Sick leave pay.
- Policies to keep sick workers from working.
Outbreak restaurants were less likely to have
- A certified kitchen manager (CKM) on staff.
- Food-safety certification training provided by a state or local agency.
- Food-safety certification training provided by a restaurant corporation.
Outbreak restaurants were more likely to be
- Sit-down restaurants.
- Classified as ethnic restaurants.
Outbreak restaurants with CKMs were less likely than outbreak restaurants without CKMs to have had outbreaks
- Of norovirus and Clostridium perfringens.
- Caused by workers touching food with their bare hands.
Within outbreak restaurants, CKMs were more likely than other managers to be familiar with the Hazard Analysis Critical Control Point (HACCP) system. All CKMs were familiar with the HACCP food-safety system recommended by the U.S. Food and Drug Administration. Twenty percent of other managers were familiar with HACCP.
Restaurant Traits Linked to Infected Food Handlers
Kitchen manager certification, sick leave pay, and policies to keep sick workers from working did not lower rates of infected food handlers as a cause of outbreaks.
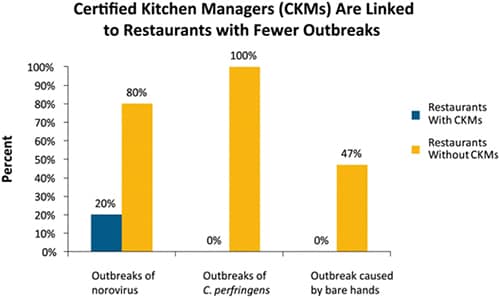
Norovirus: 20% of outbreaks occurred in restaurants with a CKM; 80% occurred in restaurants without a CKM. C. perfringens: No outbreaks occurred in restaurants with a CKM; 100% occurred in restaurants without a CKM. Bare-hand contact with food was not a contributing factor in any outbreaks in restaurants with a CKM. It was a contributing factor in 47% of outbreaks in restaurants without a CKM.
- Certified kitchen manager: manager who passed a test to show knowledge of food safety.
- HACCP: a seven-step approach to identify and manage food-safety hazards.
Scientific article this plain language summary is based on: Systematic Environmental Evaluations to Identify Food Safety Differences between Outbreak and Nonoutbreak Restaurants [PDF – 195 KB]
Other summaries related to certification:
- Kitchen Manager Certification Study and Food Safety
- Food Safety Certification and Knowledge
- Restaurant Traits Linked with Safer Ground Beef Preparation and Cooking Practices
Evaluation of Outbreak and Nonoutbreak Restaurants (study information)
More EHS-Net publications by Study Topic
This study was conducted by the Environmental Health Specialists Network (EHS-Net). EHS-Net is a federally funded collaboration of federal, state, and local environmental health specialists and epidemiologists working to better understand the environmental causes of foodborne illness.