Celebrating 20 Years of Restaurant Food Safety Research!
CDC’s Environmental Health Specialists Network (EHS-Net), established in 2000, brings together state and local environmental health programs, the United States Department of Agriculture (USDA), and the Food and Drug Administration (FDA). EHS-Net researches food safety policies and practices and investigates foodborne illness outbreaks in restaurants. EHS-Net has conducted 15 collaborative research studies; state and local EHS-Net programs also conduct their own individual research projects.

In 2006, EHS-Net found that restaurants with foodborne outbreaks were less likely to have a kitchen manager certified in food safety than restaurants without outbreaks.
- FDA used these findings to recommend a provision requiring restaurants to have a certified kitchen manager in their 2013 Food Code.
- FDA used additional EHS-Net studies to further strengthen the provision in the 2017 Food Code, which now requires restaurants to have a certified manager on site during all hours of operation.

FDA’s Food Codeexternal icon contains science-based guidance to improve food safety in restaurants, delis, caterers, and others. Jurisdictions can use it as a model for their own food safety rules for these establishments.

Nearly 1 in 10 foodborne outbreaks are linked with ground beef each year.
- EHS-Net found that only about 1 in 5 retail establishments kept beef grinding records. These records help trace food implicated in an outbreak back to the facility that produced it. USDA used these and other findings to require establishments to keep beef grinding logs.
- Rhode Island, an EHS-Net site, was the only northeastern state that prohibited selling undercooked ground meat to children. Their research found they had lower E. coli illness rates than other northeastern states. This finding supported FDA’s update to the 2009 Food Code to prohibit undercooked ground meat in children’s menu items.

The bacteria Listeria monocytogenes causes the third highest number of foodborne illness deaths in the United States each year. Contamination of deli meats is an important cause of outbreaks.
- EHS-Net found many delis were not following guidance to control bacteria like Listeria monocytogenes. For example, about half of delis did not fully clean their slicers every 4 hours, and 1 in 6 delis had a refrigerator that was too warm.
- EHS-Net’s findings were used by CDC, FDA, and USDA in a joint effort to assess the impact of deli practices on risk of disease from Listeria. This assessment was then included in USDA’s 2016 guidelines on best practices for controlling these harmful bacteria in delis.

Norovirus is the leading cause of foodborne outbreaks in the United States. Infected food workers cause about 70% of norovirus outbreaks related to contaminated food.
- EHS-Net found 1 in 5 food workers reported working while sick with vomiting and diarrhea. Fear of losing their job or leaving coworkers short staffed were important factors in their decision.
- EHS-Net also found that food workers washed their hands only 1 of every 4 times they should have.
- These findings informed CDC’s Vital Signs on preventing norovirus outbreaks. This guidance stressed that restaurants should ensure food workers wash their hands and require sick food workers to stay home, including paying them sick leave or using other practices to support sick workers staying home.
California’s assessment of mobile food trucks found that 95% of them had at least one critical food safety risk factor. Their finding underscored that mobile food trucks are similar to restaurants in their food safety risks and would benefit from similar inspection practices.
Minnesota’s research on restaurant food cooling practices found that foods cooled in containers less than 3 inches deep were significantly more likely to cool in time to avoid dangerous germ growth. Restaurants can prevent outbreaks caused by food cooling too slowly by adopting this best practice.

New York City’s evaluation of their restaurant grading program showed that the program improved food safety. The proportion of restaurants scoring an “A” on their inspections increased by 35%. This positive result supported a later initiative to expand grading to the city’s mobile food vending units.
New York helped local health department investigators develop an enhanced sampling plan and training to detect Listeria in two food establishments with long-lasting outbreaks. Sampling found the same strain of Listeria in the establishments making people ill with listeriosis. Investigators used these results to recommend focused interventions for the establishments. The results also showed the value of environmental sampling in investigating and stopping outbreaks.
Rhode Island reviewed its foodborne illness complaint system and found it identified most outbreaks investigated in the state and quickly detected illnesses, likely helping prevent more illness. These findings highlight the vital role complaint systems play in detecting and preventing outbreaks.
Tennessee’s assessment of food safety in grocery stores found almost half of grocery stores prepared food in complex ways, such as cooking raw animal products and then cooling them. In addition, more than 1 in 10 grocery stores engaged in high-risk practices, such as smoking and curing. These findings highlight the need to assess the food safety risk of grocery store practices and adjust inspection frequencies accordingly.
EHS-Net’s goal to improve foodborne outbreak investigations and the data obtained from them led them to create NEARS in 2014. This surveillance system captures environmental assessment data from outbreak investigations that were not regularly collected before. NEARS complements CDC’s Foodborne Disease Outbreak Surveillance System, which collects epidemiologic and laboratory data from investigations. Since it was created,
- 51 state and local health departments registered for NEARS and reported 1,200 outbreaks to the system.
- CDC provided environmental assessment training to all NEARS participants.
- 4 articles were published sharing NEARS findings.
This finding suggests restaurants can reduce the impact of outbreaks through the following actions:
- Providing food safety training for managers and food workers
- Having managers certified in food safety
- Having cleaning policies for surfaces where food is prepared
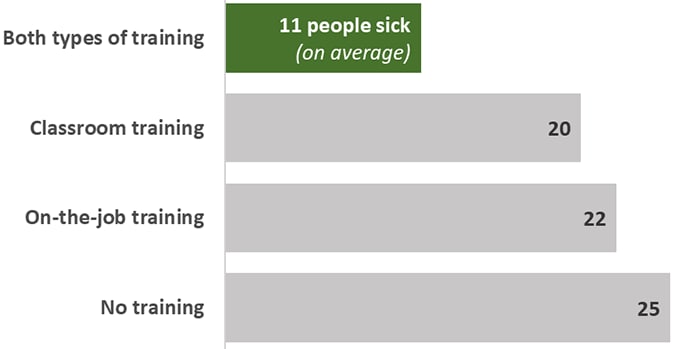
NEARS found norovirus outbreaks had fewer sick people when restaurants provided training on food safety.
Since 2000, findings from EHS-Net’s research have been distributed in the following:
- 52 articles
- 25 plain language summaries
- 4 infographics
CDC and EHS-Net sites have also given about 130 presentations on their work at local, regional, and national conferences and meetings over the past 5 years alone.
- Read our column summarizing key findings from EHS-Net’s 20 years of restaurant food safety research.external icon
- Explore our EHS-Net Findings in Plain Language for more research results.
- Read our EHS-Net Partner Success Stories for more details on individual research projects and explore our Tools from EHS-Net programs.
- See our complete list of EHS-Net Publications.
- Learn more about the National Environmental Assessment Reporting System.
- Find out more about E. coli, Listeria, and norovirus.