Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail.
Three Sudden Cardiac Deaths Associated with Lyme Carditis — United States, November 2012–July 2013
Lyme disease* is a multisystem illness caused by Borrelia burgdorferi, a spirochete transmitted by certain species of Ixodes ticks. Approximately 30,000 confirmed and probable cases of Lyme disease were reported in the United States in 2012, primarily from high-incidence states in the Northeast (Connecticut, Delaware, Maine, Maryland, Massachusetts, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, and Vermont) and upper Midwest (Minnesota and Wisconsin) (1,2).† Common manifestations include cutaneous, neurologic, and rheumatologic signs and symptoms. Symptomatic infection of the heart is rare in recognized Lyme disease cases and usually resolves promptly with appropriate antibiotic therapy. Nonetheless, cardiac involvement occasionally can cause life-threatening cardiac conduction abnormalities. During November 2012–July 2013, one woman and two men (ranging in age from 26 to 38 years) from high-incidence Lyme disease states experienced sudden cardiac death and, on postmortem examination, were found to have evidence of Lyme carditis. The three deaths were investigated by the Connecticut Department of Public Health, Massachusetts Department of Public Health, New Hampshire Department of Public Health, New York State Department of Health, and CDC. Donated corneas from two decedents had been transplanted to three recipients before the diagnosis of Lyme disease was established, but no evidence of disease transmission was found. Although death from Lyme carditis is rare, it should be considered in cases of sudden cardiac death in patients from high-incidence Lyme disease regions. Reducing exposure to ticks is the best method for preventing Lyme disease and other tickborne infections.§
Case Reports and Public Health Investigation
Patient 1. In November 2012, a Massachusetts resident was found unresponsive in an automobile after it veered off the road. No evidence of traumatic injury was found. An electrocardiogram (EKG) performed by emergency responders showed no cardiac activity, and the patient was pronounced dead at a nearby hospital. The patient had no serious preexisting medical conditions. No rash was noted at autopsy, although some atherosclerosis was present. Interviews with next-of-kin revealed that the patient had described a nonspecific illness with malaise and muscle and joint pain during the 2 weeks preceding death. The patient lived alone with a dog that was reported to have ticks frequently.
The decedent's corneas and skin, musculoskeletal, cardiac, and vascular tissues were recovered for potential transplantation. The heart was sent to tissue bank A for valve recovery. Microscopic examination of cardiac tissue found extensive myocarditis with mixed perivascular lymphoplasmacytic inflammation suggestive of Lyme carditis. A postmortem serum sample tested at CDC yielded serologic evidence of recent infection with B. burgdorferi, reacting strongly in both whole cell sonicate (WCS) and C6 enzyme immunoassay (EIA), and against all three scored bands (23 kDa, 39 kDa, and 41 kDa) by immunoglobulin M (IgM) Western blot. Western blot testing for immunoglobulin G (IgG) antibodies demonstrated reactivity against four of 10 scored bands (23 kDa, 39 kDa, 41 kDa, and 45 kDa); these serologic findings were consistent with early disseminated Lyme disease.
Histopathologic evaluation of postmortem tissues at CDC also was suggestive of Lyme pancarditis (Figure 1) and abundant spirochetes were observed by Warthin-Starry silver stain (Figure 2). Spirochetes also were detected in the myocardium by immunohistochemistry (IHC). Polymerase chain reaction (PCR) assays detected B. burgdorferi in extracts of formalin-fixed, paraffin-embedded heart tissue based on outer surface protein A, flagellin, and plasminogen-binding protein gene targets. No donor tissues were transplanted.
Patient 2. In July 2013, a New York state resident experienced chest pain and collapsed at home. Cardiopulmonary resuscitation was unsuccessful, and the patient was pronounced dead at a local hospital. The patient's past medical history included a diagnosis of Wolff-Parkinson-White syndrome, a cardiac conduction abnormality. The patient had no known tick contact or rash but was reported to be a hiker. Evidence of hypertensive and atherosclerotic cardiovascular disease was noted at autopsy. The decedent's corneas and skin, musculoskeletal, vascular, and cardiac tissue were recovered for potential transplantation. Examination of cardiac tissue at tissue bank A revealed moderate diffuse, perivascular lymphoplasmacytic pancarditis, similar to that seen in patient 1. Serologic testing at CDC was consistent with recent infection with B. burgdorferi; WCS and C6 EIAs were strongly reactive, IgM Western blot demonstrated strong reactivity to all three scored bands, and IgG Western blot demonstrated reactivity to four scored bands (23 kDa, 41 kDa, 58 kDa, and 66 kDa). Rare spirochetes were identified in cardiac tissue by Warthin-Starry silver stain and IHC; heart tissues tested positive for B. burgdorferi by PCR.
Before diagnosis of B. burgdorferi infection, the decedent's corneas were transplanted to two recipients. The transplanting physicians and cornea recipients subsequently were notified of the donor's infection. Neither recipient 1 nor recipient 2 reported signs or symptoms of Lyme disease or problems with the transplanted cornea. Both recipients elected to receive antibiotic therapy with doxycycline. None of the remaining donated tissues were transplanted.
Patient 3. In July 2013, a Connecticut resident collapsed while visiting New Hampshire and was pronounced dead at a local hospital. The patient had complained of episodic shortness of breath and anxiety during the 7–10 days before death. No rash, arthralgia, or neurologic symptoms were noted. A physician consulted 1 day before death prescribed clonazepam for anxiety; an EKG was not performed, nor were any antibiotics prescribed. The patient lived on a heavily wooded lot and had frequent tick exposure; there was no known history of cardiovascular disease. Autopsy revealed myocarditis, and the medical examiner submitted heart tissues to CDC for evaluation of suspected viral myocarditis. Corneas and skin were recovered for donation, and one cornea was transplanted to recipient 3. No other tissue was transplanted. Recipient 3 was examined 1 week after corneal transplant and was recovering as anticipated. Examination of heart tissues at CDC again demonstrated diffuse mixed perivascular lymphoplasmacytic pancarditis. Warthin-Starry stain revealed spirochetes in the myocardium, and IHC and PCR assays confirmed the spirochete as B. burgdorferi. WCS and C6 EIAs were positive, IgM Western blot was positive for all three scored bands, and IgG Western blot demonstrated reactivity to one scored band (41 kDa).
The eye bank was informed of the Lyme disease status of the donor and the recommendations for therapy. Before notification of the Lyme disease status of the donor, recipient 3 died of unrelated causes. No tissues or serum from recipient 3 were available for evaluation.
Reported by
Gregory Ray, MD, Thadeus Schulz, MD, Wayne Daniels, DO, Cryolife, Inc. Kennesaw, GA. Elizabeth R. Daly, MPH, New Hampshire Dept of Health and Human Svcs; Thomas A. Andrew, MD, New Hampshire Office of the Chief Medical Examiner. Catherine M. Brown, DVM, Massachusetts Dept of Public Health; Peter Cummings, MD, Massachusetts Office of the Chief Medical Examiner. Randall Nelson, DVM, Matthew L. Cartter, MD, Connecticut Dept of Public Health. P. Bryon Backenson, MS, Jennifer L. White, MPH, Philip M. Kurpiel, MPH, Russell Rockwell, PhD, New York State Dept of Health; Andrew S. Rotans, MPH, Christen Hertzog, Linda S. Squires, Dutchess County Dept of Health; Jeanne V. Linden, MD, Wadsworth Center, New York State Dept of Health; Margaret Prial, MD, Office of the Medical Examiner, Orange County, New York. Jennifer House, DVM, Pam Pontones, MA, Indiana State Dept of Health. Brigid Batten, MPH, Dianna Blau, DVM, PhD, Marlene DeLeon-Carnes, Atis Muehlenbachs, MD, PhD, Jana Ritter, DVM, Jeanine Sanders, Sherif R. Zaki, MD, PhD, Div of High-Consequence Pathogens and Pathology; Paul Mead, MD, Alison Hinckley, PhD, Christina Nelson, MD, Anna Perea, MSc, Martin Schriefer, PhD, Claudia Molins, PhD, Div of Vector-Borne Infectious Diseases, National Center for Emerging and Zoonotic Infectious Disease; Joseph D. Forrester, MD, EIS Officer, CDC. Corresponding contributor: Joseph D. Forrester, jforrester@cdc.gov, 970-266-3587.
Editorial Note
This report describes three cases of sudden cardiac death associated with Lyme carditis, with subsequent transplantation of corneas from two of the decedents into three recipients. Only rarely has death been attributed to Lyme carditis (3–6), and review of pathology reports at tissue bank A did not identify any additional confirmed cases among 20,000 cardiac specimens received since 2004. Whether the preexisting heart conditions found in two patients increased their risk for death is unclear.
Borrelia burgdorferi has been shown to affect all layers of the heart, but tends to spare the great vessels and heart valves (7). Inflammation is characteristically diffuse, perivascular, lymphohistiocytic, and plasma cell-rich. Spirochetes can be found within the myocardial cellular infiltrates; IHC and PCR testing can provide additional evidence of infection. Although Lyme carditis usually is present in conjunction with other features of the disease, such as erythema migrans, arthritis, or neurologic disease, it can be observed independently (8). The most common cardiac manifestation is atrioventricular block, which can fluctuate between first, second, and third degree (7,8). Second-degree or third-degree atrioventricular block occurs in approximately 0.8% of all Lyme disease cases reported to CDC (2). Symptoms of atrioventricular block, including lightheadedness, palpitations, shortness of breath, chest pain, and syncope can occur 4 days to 7 months after onset of disease, with a median of 21 days (7,8). With appropriate therapy (9), prognosis is excellent, and signs of cardiac involvement typically resolve within 1–6 weeks, depending on the degree of conduction disturbance (10). Some cases of complete heart block might require temporary pacing.
Although no cases of Lyme disease transmission through organ or tissue transplantation have been reported, the identification of organisms in tissue suggests the risk for transmission could exist. Ophthalmologic manifestations of Lyme disease are rare but can involve any of the ocular structures and occur during any stage of Lyme disease.¶ Given the rarity of ocular Lyme disease, and of corneal Lyme disease in particular, and the absence of ocular symptoms in the deceased patients, the need for antibiotics in this setting was equivocal. However, if administered, oral doxycycline would be expected to penetrate eye structures well.
Medical examiners and pathologists should be aware that Lyme carditis is a potential, albeit rare, cause for sudden cardiac death in persons from high-incidence Lyme disease areas. Diffuse, mixed perivascular lymphoplasmacytic infiltrates seen on pathologic examination of heart tissue from patients who have sudden cardiac death in high-incidence Lyme disease areas should prompt serologic evaluation for Lyme disease and further histopathologic examination for spirochetes, including IHC evaluation and PCR. Lyme disease is a nationally notifiable disease; all suspected cases of fatal Lyme carditis should be reported to state or local public health authorities, and the cases should be investigated.
Prompt recognition and early, appropriate therapy for Lyme disease is essential. Health-care providers should ask patients with suspected Lyme disease about cardiac symptoms and obtain an EKG if indicated. Conversely, they should ask patients with unexplained heart block about possible exposure to infected ticks. Health-care providers also should remind their patients of steps to prevent infection, including use of repellent, daily tick checks, prompt showering after potential exposure, and landscape management. The three deaths described in this report underscore the need for better methods of primary prevention of Lyme disease and other tickborne infections.
References
- CDC. Notice to readers: final 2012 reports of nationally notifiable infectious diseases. MMWR 2013;62:669–82.
- CDC. Surveillance for Lyme disease—United States, 1992–2006. MMWR 2008;57(No. SS-10):1–9.
- Cary NR, Fox B, Wright DJ, Cutler SJ, Shapiro LM, Grace AA. Fatal Lyme carditis and endodermal heterotopia of the atrioventricular node. Postgrad Med J 1990;66:134–6.
- Marcus LC, Steere AC, Duray PH, Anderson AE, Mahoney EB. Fatal pancarditis in a patient with coexistent Lyme disease and babesiosis. Demonstration of spirochetes in the myocardium. Ann Intern Med 1985;103:374–6.
- Tavora F, Burke A, Li L, Franks TJ, Virmani R. Postmortem confirmation of Lyme carditis with polymerase chain reaction. Cardiovasc Pathol 2008;17:103–7.
- Reimers CD, de Koning J, Neubert U, et al. Borrelia burgdorferi myositis: report of eight patients. J Neurol 1993;240:278–83.
- Steere AC, Batsford WP, Weinberg M, et al. Lyme carditis: cardiac abnormalities of Lyme disease. Ann Intern Med 1980;93:8–16.
- Fish AE, Pride YB, Pinto DS. Lyme carditis. Infect Dis Clin N Am 2008;22:275–88.
- Wormser GP, Dattwyler RJ, Shapiro ED, et al. The clinical assessment, treatment, and prevention of Lyme disease, human granulocytic anaplasmosis, and babesiosis: clinical practice guidelines by the Infectious Diseases Society of America. Clin Infect Dis 2006;43:1089–134.
- McAlister HF, Klementowicz PT, Andrews C, Fisher JD, Feld M, Furman S. Lyme carditis: an important cause of reversible heart block. Ann Intern Med 1989;1110:339–45.
* Additional information available at http://www.cdc.gov/lyme.
† Additional information regarding how many persons receive a diagnosis each year of Lyme disease is available at http://www.cdc.gov/lyme/faq/index.html#humancases.
§ Additional information available at http://www.cdc.gov/lyme/prev/index.html.
¶ Additional information available at http://www.sciencedirect.com/science/article/pii/S0161642099001281.
What is already known on this topic?
Carditis with heart block is a known but uncommon complication of early disseminated Lyme disease that is generally treated effectively with appropriate antibiotic therapy. Four deaths from Lyme carditis have been reported.
What is added by this report?
This report describes three new cases of sudden cardiac death associated with Lyme carditis. The decedents were aged 26 to 38 years and lived in high-incidence Lyme disease areas.
What are the implications for public health practice?
Pathologists and medical examiners should be aware that Lyme carditis can be a cause of sudden cardiac death. All suspected cases of fatal Lyme carditis should be reported to state or local public health authorities, and the cases should be investigated. Physicians and health-care providers should ask patients with suspected Lyme disease about cardiac symptoms, and conversely, ask patients with acute, unexplained cardiac symptoms about possible tick exposure and symptoms of Lyme disease. Clinicians should encourage all patients to practice recommended tick bite prevention strategies.
FIGURE 1. Hematoxylin and eosin stain at 6.25X magnification demonstrating interstitial perivascular lymphoplasmacytic pancarditis in postmortem tissue of one of three patients whose death was associated with Lyme carditis — United States, 2013
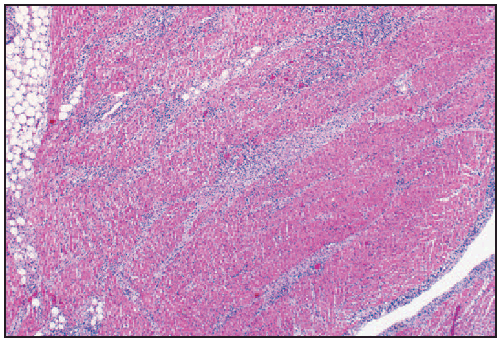
Alternate Text: The figure above shows Hematoxylin and eosin stain, demonstrating interstitial perivascular lymphoplasmacytic pancarditis in postmortem tissue of one of three patients whose death was associated with Lyme carditis in the United States in 2012.
FIGURE 2. Warthin-Starry stain of cardiac tissue at 158X magnification demonstrating Borrelia burgdorferi spirochetes (arrow) in one of three patients whose death was associated with Lyme carditis — United States, 2013
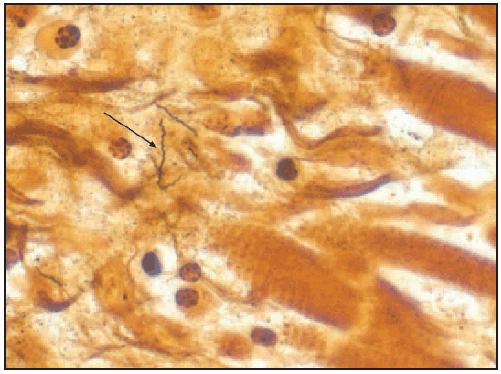
Alternate Text: The figure above shows a Warthin-Starry stain of cardiac tissue demonstrating Borrelia burgdorferi spirochetes in one of three patients whose death was associated with Lyme carditis during November 12–July 2013.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All MMWR HTML versions of articles are electronic conversions from typeset documents.
This conversion might result in character translation or format errors in the HTML version.
Users are referred to the electronic PDF version (http://www.cdc.gov/mmwr)
and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S.
Government Printing Office (GPO), Washington, DC 20402-9371;
telephone: (202) 512-1800. Contact GPO for current prices.
**Questions or messages regarding errors in formatting should be addressed to
mmwrq@cdc.gov.


