FoodNet Surveillance
Active Laboratory Surveillance
FoodNet has conducted population-based surveillance for laboratory-diagnosed infections caused by Campylobacter, Listeria, Salmonella, Shiga toxin-producing E. coli, Shigella, Vibrio, and Yersinia since 1996; Cyclospora since 1997; and STEC non-O157 since 2000. FoodNet also conducted surveillance for Cryptosporidium from 1997 through 2017. FoodNet began to collect information on infections identified by culture-independent methods in 2009 for STEC and Campylobacter and in 2011 for Listeria, Salmonella, Shigella, Yersinia, and Vibrio.
FoodNet is an active surveillance system, meaning that public health officials routinely communicate with more than 700 clinical laboratories serving the surveillance area to identify new infections and conduct periodic audits to ensure that all infections are reported.
FoodNet collects information on laboratory-diagnosed infections identified by culture or culture-independent diagnostic test (CIDT) for bacterial pathogens and microscopy or polymerase chain reaction (PCR) for parasites. Personnel at each FoodNet site collect information about cases of infection and share that information with CDC through FoodNet’s database. The information includes
- hospitalizations occurring within 7 days of the specimen collection date,
- the patient’s status (alive or dead) at hospital discharge (or at 7 days after the specimen collection date if the patient is not hospitalized),
- whether the patient traveled abroad in the 7 days before illness began, and
- selected food and environmental exposures.
Hemolytic Uremic Syndrome Surveillance
FoodNet conducts surveillance for physician-diagnosed hemolytic uremic syndrome (HUS) through a network of pediatric nephrologists and infection-control practitioners. FoodNet staff also review hospital discharge data for pediatric HUS cases to validate surveillance reports and identify additional cases by using ICD-9-CM/ICD-10 codes specifying HUS, acute renal failure with the hemolytic anemia and thrombocytopenia, or thrombotic thrombocytopenic purpura with diarrhea caused by an unknown pathogen or E. coli.
Surveillance Projects
In addition to routine surveillance, FoodNet occasionally conducts special surveillance projects. In 2002, two sites conducted population-based surveillance for reactive arthritis associated with Campylobacter, Salmonella, Shigella, Yersinia, and STEC infections. In 2009, FoodNet conducted a pilot surveillance program for community-acquired Clostridioides difficile infections (formerly known as Clostridium difficile) in Connecticut and New York. In 2010, FoodNet conducted a pilot surveillance program for Cronobacter sakazakii infections in selected sites.
Burden of Illness
The burden of illness pyramid is a model for understanding foodborne disease reporting, and illustrates steps that must occur for an episode of illness in the population to be registered in surveillance.
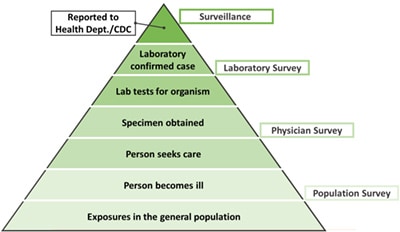
The burden of illness pyramid is a model for understanding foodborne disease reporting.
Starting from the bottom of the pyramid:
- Some members of the general population are exposed to an organism;
- Some of these exposed people become ill;
- Some of these ill people seek medical care;
- A specimen is obtained from some of these people and submitted to a clinical laboratory;
- A laboratory tests some of these specimens for a given pathogen;
- The laboratory identifies the causative organism in some of these tested specimens and thereby confirms the case;
- The laboratory-confirmed case is reported to a local or state health department.
FoodNet conducts laboratory surveys, physician surveys, and population surveys to collect information about each of these steps. This information is used to calculate estimates of the actual number of people who become ill. Other information is used to estimate the proportion of these illnesses transmitted by food.