Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail.
Prevention of Perinatal Group B Streptococcal Disease: Revised Guidelines from CDC, 2010
Please note: Updates to this report are now available. To view, please click here and here.
Summary
Despite substantial progress in prevention of perinatal group B streptococcal (GBS) disease since the 1990s, GBS remains the leading cause of early-onset neonatal sepsis in the United States. In 1996, CDC, in collaboration with relevant professional societies, published guidelines for the prevention of perinatal group B streptococcal disease (CDC. Prevention of perinatal group B streptococcal disease: a public health perspective. MMWR 1996;45[No. RR-7]); those guidelines were updated and republished in 2002 (CDC. Prevention of perinatal group B streptococcal disease: revised guidelines from CDC. MMWR 2002;51[No. RR-11]). In June 2009, a meeting of clinical and public health representatives was held to reevaluate prevention strategies on the basis of data collected after the issuance of the 2002 guidelines. This report presents CDC's updated guidelines, which have been endorsed by the American College of Obstetricians and Gynecologists, the American Academy of Pediatrics, the American College of Nurse-Midwives, the American Academy of Family Physicians, and the American Society for Microbiology. The recommendations were made on the basis of available evidence when such evidence was sufficient and on expert opinion when available evidence was insufficient. The key changes in the 2010 guidelines include the following:
-
expanded recommendations on laboratory methods for the identification of GBS,
-
clarification of the colony-count threshold required for reporting GBS detected in the urine of pregnant women,
-
pdated algorithms for GBS screening and intrapartum chemoprophylaxis for women with preterm labor or preterm premature rupture of membranes,
-
a change in the recommended dose of penicillin-G for chemoprophylaxis,
-
updated prophylaxis regimens for women with penicillin allergy, and
-
a revised algorithm for management of newborns with respect to risk for early-onset GBS disease.
Universal screening at 35--37 weeks' gestation for maternal GBS colonization and use of intrapartum antibiotic prophylaxis has resulted in substantial reductions in the burden of early-onset GBS disease among newborns. Although early-onset GBS disease has become relatively uncommon in recent years, the rates of maternal GBS colonization (and therefore the risk for early-onset GBS disease in the absence of intrapartum antibiotic prophylaxis) remain unchanged since the 1970s. Continued efforts are needed to sustain and improve on the progress achieved in the prevention of GBS disease. There also is a need to monitor for potential adverse consequences of intrapartum antibiotic prophylaxis (e.g., emergence of bacterial antimicrobial resistance or increased incidence or severity of non-GBS neonatal pathogens). In the absence of a licensed GBS vaccine, universal screening and intrapartum antibiotic prophylaxis continue to be the cornerstones of early-onset GBS disease prevention.
Introduction
In the 1970s, the bacterium group B Streptococcus (GBS) emerged as the leading infectious cause of early neonatal morbidity and mortality in the United States (1--4). Initial case series reported case-fatality ratios as high as 50% (5). Maternal colonization with GBS in the genitourinary or gastrointestinal tracts is the primary risk factor for disease. Beginning in the mid 1980s, clinical trials and well-designed observational studies demonstrated that administering intravenous antibiotics during labor to women at risk for transmitting GBS to their newborns could prevent invasive disease in the first week of life (i.e., early-onset disease) (6--11). As a result of the collaborative efforts of clinicians, researchers, professional organizations, parent advocacy groups, and the public health community in the 1990s, recommendations for intrapartum prophylaxis to prevent perinatal GBS disease were issued in 1996 by the American College of Obstetricians and Gynecologists (ACOG) (12) and CDC (13) and in 1997 by the American Academy of Pediatrics (AAP) (14). Revised guidelines for the prevention of early-onset GBS disease issued in 2002 recommended universal culture-based screening of all pregnant women at 35--37 weeks' gestation to optimize the identification of women who should receive intrapartum antibiotic prophylaxis (15).
Before active prevention was initiated, an estimated 7,500 cases of neonatal GBS disease occurred annually in the United States (16). Striking declines in disease incidence coincided with increased prevention activities in the 1990s (17), and a further reduction occurred following the issuance of the recommendation for universal screening in 2002 (18). However, GBS disease remains the leading infectious cause of morbidity and mortality among newborns in the United States (19,20). The continued burden of disease and newly available data relevant to early-onset GBS disease prevention from the fields of epidemiology, obstetrics, neonatology, microbiology, molecular biology, and pharmacology prompted revision of the guidelines for early-onset GBS disease prevention.
Methods
In November 2008, CDC formed a technical working group* to revise the 2002 guidelines (15). The group consisted of representatives from the ACOG Committee on Obstetric Practice, the American College of Nurse-Midwives (ACNM), the AAP Committee on Infectious Diseases and Committee on the Fetus and Newborn, the American Academy of Family Physicians (AAFP), the Society for Healthcare Epidemiology of America, the American Society for Microbiology (ASM), and CDC's Active Bacterial Core surveillance system, as well as experts in GBS epidemiology, clinical microbiology, and pharmacology. The group held regular telephone conference calls to identify potential areas of change in the recommendations to prevent GBS disease, and to define sources of newly available data (published and unpublished) to inform the revision of the guidelines.
The working group identified a subset of topics for in-depth review, including areas in which new technologies and/or evidence had become available since the publication of the 2002 guidelines, areas in which implementation of the 2002 guidelines was found to be suboptimal on the basis of published and unpublished data, and areas in which interpretation of the 2002 guidelines was found to be variable on the basis of inquiries received at CDC and the experience of experts in the field. For these topics, a thorough review was conducted of published literature through PubMed searches, other sources (including abstracts and conference proceedings), and unpublished data from ongoing surveillance and research activities of which the working group was aware. For topics on which several sources of data were available, evidence was summarized in tables. For topics on which relatively little new evidence was available, summaries of pertinent data were provided to working group members. Expert opinion was sought from working group members regarding topics on which no new evidence was available.
In June 2009, an in-person meeting of the technical working group was held to review available data and develop updated recommendations using an evidence-based approach when possible and relying on expert scientific opinion when sufficient data were lacking (Table 1). These updated guidelines replace CDC's 2002 guidelines. They are intended for providers of prenatal, obstetric, and neonatal care; supporting microbiology laboratories, hospital administrators, and managed-care organizations; childbirth educators; public health authorities; and expectant parents and their advocates.
Invasive Group B Streptococcal Disease
Group B Streptococcus, or Streptococcus agalactiae, is a gram-positive bacterium that causes invasive disease primarily in infants, pregnant or postpartum women (19,21--27), and older adults, with the highest incidence among young infants (19). Infections in newborns occurring within the first week of life are designated early-onset disease. Late-onset infections occur in infants aged >1 week, with most infections evident during the first 3 months of life. Because of the burden of disease among infants and the availability of effective interventions to prevent early-onset GBS disease, these guidelines concern only early-onset disease. The measures used to prevent early-onset GBS disease also might prevent some perinatal maternal infections (17,28); however, they do not prevent late-onset infant disease (29).
Early-Onset GBS Disease
GBS is the leading infectious cause of morbidity and mortality among infants in the United States. As a result of prevention efforts, incidence of GBS has declined dramatically over the past 15 years, from 1.7 cases per 1,000 live births in the early 1990s to 0.34--0.37 cases per 1,000 live births in recent years (Figure 1). On the basis of data from CDC's Active Bacterial Core surveillance (ABCs) system, a network of 10 sites across the United States that conduct active, population-based surveillance, CDC estimates that in recent years, GBS has caused approximately 1,200 cases of early-onset invasive disease per year (30); approximately 70% of cases are among babies born at term (≥37 weeks' gestation) (19).
Infants with early-onset GBS disease generally present with respiratory distress, apnea, or other signs of sepsis within the first 24--48 hours of life (3,31). The most common clinical syndromes of early-onset disease are sepsis and pneumonia; less frequently, early-onset infections can lead to meningitis. The case-fatality ratio of early-onset disease has declined from as high as 50% in the 1970s (5) to 4%--6% in recent years, primarily because of advances in neonatal care (17,19). Mortality is higher among preterm infants, with case-fatality rates of approximately 20% and as high as 30% among those ≤33 weeks' gestation, compared with 2%--3% among full-term infants (17,19).
Early-onset infections are acquired vertically through exposure to GBS from the vagina of a colonized woman. Neonatal infection occurs primarily when GBS ascends from the vagina to the amniotic fluid after onset of labor or rupture of membranes, although GBS also can invade through intact membranes (32,33). GBS can be aspirated into the fetal lungs, which in turn can lead to bacteremia. Infants also can become infected with GBS during passage through the birth canal; infants who are exposed to the organism through this route can become colonized at mucus membrane sites in the gastrointestinal or respiratory tracts, but these colonized infants most commonly remain healthy.
Risk Factors for Early-Onset GBS Disease
Maternal intrapartum GBS colonization is the primary risk factor for early-onset disease in infants. A classic prospective cohort study conducted during the 1980s revealed that pregnant women with GBS colonization were >25 times more likely than pregnant women with negative prenatal cultures to deliver infants with early-onset GBS disease (34). In the absence of any intervention, an estimated 1%--2% of infants born to colonized mothers develop early-onset GBS infections (13,34,35). Approximately 10%--30% of pregnant women are colonized with GBS in the vagina or rectum (36--38). GBS colonization during pregnancy can be transient, intermittent, or persistent (39--41). Although some women with GBS colonization during a pregnancy will be colonized during subsequent pregnancies, a substantial proportion will not (42,43). The gastrointestinal tract serves as the primary reservoir for GBS and is the likely source of vaginal colonization. Heavy colonization, defined as culture of GBS from direct plating rather than from selective broth only, is associated with higher risk for early-onset disease (44,45). GBS identified in clean-catch urine specimens during any trimester is considered a surrogate for heavy maternal colonization and also is associated with a higher risk for early-onset GBS disease (46--50).
In addition to maternal colonization with GBS, other factors that increase the risk for early-onset disease include gestational age <37 completed weeks, longer duration of membrane rupture, intra-amniotic infection, young maternal age, black race, and low maternal levels of GBS-specific anticapsular antibody (51--58). Previous delivery of an infant with invasive GBS disease is a risk factor for early-onset disease in subsequent deliveries (59--62). In a 1985 report of predictors of early-onset disease, women with gestation <37 weeks, membrane rupture of >12 hours, or intrapartum temperature >99.5ºF (>37.5ºC) had 6.5 times the risk for having an infant with early-onset GBS disease compared with women who had none of these risk factors (34). Of note, women who had one of these risk factors but who had negative prenatal screening cultures were at relatively low risk for early-onset GBS disease (incidence: 0.9 cases per 1,000 births) compared with women who were colonized prenatally but had none of the risk factors (incidence: 5.1 cases per 1,000 births) (34).
Some observational studies have reported an association between early-onset GBS disease and certain obstetric procedures, such as the use of internal fetal monitoring devices (58,63) and more than five or six digital vaginal examinations after onset of labor or rupture of membranes (55,63). However, lack of randomization in observational studies can result in confounding, because certain procedures might be used more frequently in high-risk settings (64). Although concern has been raised about performing other obstetric procedures (e.g., membrane stripping and mechanical and/or pharmacologic cervical ripening) on GBS-colonized women, available data are not sufficient to determine whether these procedures are associated with an increased risk for early-onset disease (65,66).
Prevention of Early-Onset Group B Streptococcal Disease
Intravenous Intrapartum Antibiotic Prophylaxis
The use of intravenous intrapartum antibiotic prophylaxis to prevent early-onset GBS disease in the infant was first studied in the 1980s. Clinical trials and well-designed observational studies found that intrapartum antibiotic prophylaxis reduced vertical transmission of GBS, as measured by infant colonization (6,8,11,67) or by protection against early-onset disease (6--11). Early trials suggested an efficacy of 100% for intrapartum antibiotic prophylaxis to prevent early-onset disease among infants born to women with GBS colonization (7,8,10,11). Subsequent observational studies have found the effectiveness to be 86%--89% among infants born to women who received intrapartum GBS prophylaxis (62,68).
Other strategies to reduce maternal colonization and vertical transmission have been studied, including intramuscular intrapartum antibiotic prophylaxis (67), antenatal (oral or intramuscular) antibiotics (69--71), and chlorhexidine vaginal wipes or douches (72--76); however, none has proven to be effective at preventing early-onset disease. Although some nonrandomized studies on chlorhexidine have yielded promising results (72,75), randomized clinical trials have found no protection against early-onset GBS disease or neonatal sepsis (76,77).
Intrapartum Antibiotic Prophylaxis Agents
The efficacy of both penicillin (10) and ampicillin (7) as intravenously administered intrapartum agents for the prevention of early-onset neonatal GBS disease was demonstrated in clinical trials. Penicillin has a narrower spectrum of antimicrobial activity and therefore might be less likely to select for resistant organisms, although one clinical trial found that penicillin and ampicillin administered intravenously intrapartum were associated equally with the presence of ampicillin-resistant gram-negative organisms on postpartum vaginal-perineal culture (78). The dosages of penicillin and ampicillin used for intrapartum GBS prophylaxis are aimed at achieving adequate levels in the fetal circulation and amniotic fluid rapidly while avoiding potentially neurotoxic serum levels in the mother or fetus (79--83). Although the exact duration of antibiotics needed to prevent vertical transmission of GBS has been debated (84,85), beta-lactam antibiotics for GBS prophylaxis administered for ≥4 hours before delivery have been found to be highly effective at preventing vertical transmission of GBS (86) and early-onset GBS disease (68). Shorter durations of appropriate antibiotics might provide some protection; in particular, colonization data suggest durations of ≥2 hours before delivery might confer some protection (86).
The efficacy of alternatives to penicillin or ampicillin that have been used to prevent early-onset GBS disease among infants born to penicillin-allergic mothers (including cefazolin, clindamycin, erythromycin, and vancomycin) has not been measured in controlled trials. Cefazolin has a relatively narrow spectrum of activity, similar pharmacokinetics and dynamics to penicillin and ampicillin, and achieves high intra-amniotic concentrations (87--89). However, an estimated 10% of persons with penicillin allergy also have immediate hypersensitivity reactions to cephalosporins (90). In contrast, data on the ability of clindamycin, erythromycin and vancomycin to reach bactericidal levels in the fetal circulation and amniotic fluid are very limited; available data suggest that erythromycin and clindamycin provided to pregnant women do not reach fetal tissues reliably (91--95).
Safety
Maternal anaphylaxis associated with GBS intrapartum chemoprophylaxis occurs but is sufficiently rare that any morbidity associated with anaphylaxis is offset greatly by reductions in the incidence of maternal and neonatal invasive GBS disease. Anaphylaxis-related mortality is likely to be a rare event because the majority of women receiving intrapartum antibiotics will be in hospital settings where rapid intervention is readily available. Allergic reactions occur in an estimated 0.7%--4.0% of all treatment courses with penicillin, the most common of which is a maculopapular rash (96). Estimates of the rate of anaphylaxis caused by penicillin range from four per 10,000 to four per 100,000 recipients (96). Maternal anaphylaxis associated with GBS prophylaxis was reported in the early 1990s (97); since the release of the 1996 guidelines, four reports of nonfatal cases of anaphylaxis associated with GBS chemoprophylaxis in the United States have been published (98--101). In a CDC multistate sample of approximately 5,000 live births occurring during 1998--1999, a single, nonfatal anaphylactic reaction was noted among the 27% of deliveries in which intrapartum antibiotics were administered (62). In that case, a single dose of penicillin was administered approximately 4 hours before a preterm cesarean delivery, and an anaphylactic reaction occurred shortly after the mother received a single dose of a cephalosporin following umbilical cord clamping. A similar sample of approximately 7,600 live births occurring during 2003--2004 revealed no cases of anaphylaxis among the 32% of deliveries in which mothers received intrapartum antibiotic prophylaxis for GBS (102).
Because a fetus or newborn is unlikely to have had a previous exposure to the antibiotic, and because specific maternal IgE antibodies are not transmitted across the placenta (103), there is no risk for anaphylaxis in the fetus or newborn resulting from intrapartum antibiotic prophylaxis. Although limited data are available on the impact of intrapartum antibiotics on neonatal gastrointestinal flora, one study comparing stool from infants born to women who received intrapartum GBS prophylaxis with stool from infants whose mothers received no intrapartum antibiotics found no significant difference in colonization with antibiotic-resistant enterobacteria between the two groups (104).
Antibiotic Resistance of GBS
The widespread use of intrapartum antibiotic prophylaxis to prevent early-onset GBS disease has raised concern about the development of antibiotic resistance among GBS isolates. GBS continues to be susceptible to penicillin, ampicillin, and first-generation cephalosporins (19,105--109). However, isolates with increasing minimum inhibitory concentrations (MICs) to penicillin or ampicillin have been reported, including 14 noninvasive isolates during 1995--2005 among adults in Japan (110), and 11 (0.2%) of 5,631 invasive isolates recovered during 1999--2005 from patients of varying ages in the United States (111). Alterations in a penicillin-binding protein (PBP 2X) were found in all of the isolates from Japan and four of those from the United States. The measured MICs from the 11 invasive isolates from the United States are just at the threshold of susceptibility (≤0.12 µg/ml for penicillin and ≤0.25 µg/ml for ampicillin) (112), but the clinical significance of these MIC values is as yet unclear.
Relatively elevated MICs to cefazolin (1 µg/ml) also were reported among three (0.05%) of 5,631 invasive GBS isolates collected through CDC's active surveillance during 1999--2005; two of the three isolates also had elevated MICs to penicillin (0.12 µg/ml) (111). Although Clinical and Laboratory Standards Institute guidelines do not specify susceptibility breakpoints for cefazolin, they recommend that all isolates susceptible to penicillin be considered susceptible to cefazolin (112). As with the elevated MICs to penicillin and ampicillin, the clinical significance of higher MICs to cefazolin among GBS isolates remains unclear.
The proportions of GBS isolates with in vitro resistance to clindamycin or erythromycin have increased over the past 20 years. The prevalence of resistance among invasive GBS isolates in the United States ranged from 25% to 32% for erythromycin and from 13% to 20% for clindamycin in reports published during 2006--2009 (19,106,108). Resistance to erythromycin is associated frequently but not always with resistance to clindamycin. One longitudinal study of GBS early-onset sepsis found that although the overall rate of GBS early-onset disease declined over time, erythromycin-resistant GBS caused an increasing proportion of disease during this interval; however, the incidence of antibiotic-resistant GBS early-onset sepsis remained stable (105).
Vaccines to Prevent GBS Disease
GBS vaccines have been investigated as a tool for reducing maternal colonization and preventing transmission to neonates (113,114); however, no licensed vaccine is available currently. Sufficient amounts of GBS capsular polysaccharide type-specific serum IgG in mothers have been shown to protect against invasive disease in their infants (51,115--118). Phase I and II clinical trials among healthy, nonpregnant adults of monovalent polysaccharide-protein conjugate vaccines of GBS disease-associated types have shown these vaccines to be well tolerated and immunogenic (116--121). A recent, double-blind randomized trial of a conjugate vaccine against GBS serotype III among nonpregnant women of reproductive age found a significant delay in acquisition of colonization with the vaccine-serotype among vaccine recipients (122). Although an effective GBS vaccine would be a powerful tool against GBS disease, no licensed vaccine is yet available.
Identification of Candidates for Intrapartum Antibiotic Prophylaxis
Culture- Versus Risk-Based Screening
Early guidelines recommended the use of one of two approaches to identifying women who should receive intrapartum antibiotic prophylaxis: a risk-based approach or a culture-based screening approach (13). Providers using the risk-based method identified candidates for intrapartum chemoprophylaxis according to the presence of any of the following intrapartum risk factors: delivery at <37 weeks' gestation, intrapartum temperature ≥100.4ºF (≥38.0ºC), or rupture of membranes for ≥18 hours. Providers using the culture-based screening method screened all pregnant women for vaginal and rectal GBS colonization between 35 and 37 week's gestation. Colonized women were offered intrapartum antibiotics at the time of labor onset or rupture of membranes if before labor. Under both strategies, intrapartum antibiotic prophylaxis was recommended for women with GBS bacteriuria at any time during their current pregnancy or for women who had given birth previously to an infant with invasive early-onset GBS disease.
A large population-based study conducted during 1998--1999 demonstrated the superiority of culture-based screening over the risk-based approach to prevention of early-onset GBS disease (62). The study found that culture-based screening resulted in the identification of a greater proportion of women at risk for transmitting GBS to their newborns. Furthermore, women with a positive antenatal GBS culture were more likely to receive intrapartum antibiotic prophylaxis than those women with a risk-based indication for chemoprophylaxis. In 2002, CDC's guidelines for GBS prevention were updated to recommend universal culture-based screening to determine which women should receive intrapartum GBS chemoprophylaxis (15). CDC recommended that women with unknown GBS colonization status at the time of delivery be managed according to the presence of intrapartum risk factors.
Preterm Delivery
Because preterm (at <37 weeks and 0 days' gestation) delivery is an important risk factor for early-onset GBS disease, and because assessing whether preterm labor or rupture of membranes will result in preterm delivery can be difficult, management of intrapartum antibiotic prophylaxis for women with threatened preterm delivery is challenging. Assessing the need for intrapartum prophylaxis for these women also can be difficult because GBS colonization status often is unknown when labor or rupture of membranes occur before 35--37 weeks' gestation. In addition, appropriate use of antibiotic prophylaxis for women with threatened preterm delivery is critical. For women remote from term with premature rupture of membranes, clinical trials have demonstrated that certain antibiotic regimens prolong latency (123,124). However, data from clinical trials also have suggested that certain antibiotics administered for preterm premature rupture of membranes can be associated with necrotizing enterocolitis in the neonate (125,126) and that antibiotics administered in the setting of spontaneous preterm labor can be associated with adverse neonatal outcomes, such as increased need for supplementary oxygen (127) or cerebral palsy (128).
The 2002 guidelines recommended that if GBS colonization status from the current pregnancy is not known, and if onset of labor or rupture of membranes occurred before 37 weeks' gestation with a substantial risk for preterm delivery, then GBS screening should be performed and intrapartum antibiotic prophylaxis for GBS should be provided pending culture results. The implementation of those recommendations has been suboptimal, with limited GBS screening on hospital admission and limited administration of intrapartum antibiotic prophylaxis (102). However, when penicillin, ampicillin, or cefazolin prophylaxis was administered for ≥4 hours before delivery to women delivering at <37 weeks' gestation, antibiotic prophylaxis was 78% (95% confidence interval: 44%--91%) effective in preventing early-onset GBS disease (CDC, unpublished data, 2009). No data are available on the effectiveness of antibiotics given before the intrapartum period in GBS-colonized women with preterm premature rupture of membranes for preventing early-onset GBS disease in the infant.
Bacteriuria
GBS is found in the urine of 2%--7% of pregnant women (46--48,129,130). GBS bacteriuria in a pregnant woman is a marker for heavy genital tract colonization, and maternal GBS bacteriuria (including pure and predominant growth of GBS in the urine) has been associated with GBS colonization and an increased risk for early-onset disease in the newborn (46--50,129). Although some women receive antibiotics to treat GBS bacteriuria during pregnancy, antibiotics do not eliminate GBS from the genitourinary and gastrointestinal tracts, and recolonization after a course of antibiotics is typical (71,131,132). Studies have found that some women with GBS bacteriuria during the first trimester might not have vaginal-rectal colonization detected at 35--37 weeks' gestation (130) or at the time of delivery (133). However, maternal GBS bacteriuria at any point during pregnancy is a recognized risk factor for early-onset GBS disease and therefore has been included as an indication for intrapartum antibiotic prophylaxis since 1996 (13,15).
The 1996 guidelines did not specify a colony-count threshold for defining GBS bacteriuria. In 2002, the guidelines recommended that laboratory personnel report GBS present in any concentration in the urine. Most data on the risk for early-onset GBS disease among infants born to women with GBS bacteriuria are derived from studies of significant GBS bacteriuria (generally >105 colony-forming units per millimeter of urine) (47--49). Although lower concentrations (<104 cfu/ml) of GBS in the urine can be associated with vaginal-rectal colonization (134), relatively few data are available on the risk for early-onset GBS disease among infants born to women with low colony-count GBS bacteriuria (48). One study from a vertically integrated health system in Utah found an elevated risk for early-onset GBS disease among infants born to women with low colony-count GBS bacteriuria compared with those whose mothers did not have GBS bacteriuria (135). However, because the majority of pregnant women in the study population had no urine culture performed, those with urine culture results might have been a biased subset. Therefore, the findings on women with low colony-count bacteriuria in this study might not be generalizable to all pregnant women with low colony-count bacteriuria. The recommendation to report any colony count of GBS in the urine represents increased workload for clinical microbiology laboratories, which generally do not report bacterial growth in urine of other pathogens at concentrations <104 cfu/ml (136) and rarely know whether urine samples are from pregnant women; as a result, some laboratories search for any GBS colonies in urine cultures from all women of reproductive age. Routine screening for asymptomatic bacteriuria is recommended in pregnant women (137); the identification of GBS through this screening represents an opportunity to detect women at high risk for transmitting GBS to their infant. However, in the context of universal late antenatal GBS screening, it is unclear how much additional disease is prevented by screening for low colony-count GBS bacteriuria and whether identification of low colony-count bacteriuria is cost-effective.
Cesarean Delivery Performed Before Labor Onset on a Woman With Intact Amniotic Membranes
Cesarean delivery does not prevent mother-to-child transmission of GBS because GBS can cross intact amniotic membranes (32,33). A risk does exist for transmission of GBS from a colonized mother to her infant during a cesarean delivery. However, a retrospective study at a single hospital (138), a national population-based study from Sweden (139), and a review of CDC active, population-based surveillance data (CDC, unpublished data, 1998--1999 and 2003--2004) indicated that when a cesarean delivery is performed before onset of labor on a woman with intact amniotic membranes, the risk for early-onset GBS disease among full-term infants is extremely low. Data on risk for transmission to preterm infants born via cesarean delivery performed before onset of labor on a woman with intact amniotic membranes are limited; however, the risk for transmission is likely much lower than in the setting of vaginal delivery or cesarean delivery following rupture of membranes or onset of labor.
Specimen Collection and Processing for GBS Screening
Timing of Screening
Because GBS colonization status can change over the course of a pregnancy, the timing of specimen collection for determination of colonization status is important. Because colonization can be transient, colonization early in pregnancy is not predictive of early-onset GBS disease (44). Late third trimester colonization status has been used as a proxy for intrapartum colonization (140). The negative predictive value of GBS cultures performed ≤5 weeks before delivery is 95%--98%; however, the clinical utility decreases when a prenatal culture is performed more than 5 weeks before delivery because the negative predictive value declines (37).
Specimen Collection
Swabbing both the lower vagina and rectum (through the anal sphincter) increases the culture yield substantially compared with sampling the cervix or the vagina without also swabbing the rectum (40,141--146). Although a small number of studies have examined the ability of perianal or vaginal-perianal cultures to detect GBS colonization (147,148), the available data on their performance compared with vaginal-rectal cultures are limited. Studies have indicated that when women in the outpatient clinic setting collect their own vaginal-rectal screening specimens, with appropriate instruction, GBS yield is similar to when specimens are collected by a health-care provider (149--152).
The use of appropriate transport media can help sustain the viability of GBS in settings where immediate laboratory processing is not possible (153,154). GBS isolates can remain viable in transport media for several days at room temperature; however, the recovery of isolates declines during 1--4 days, particularly at high temperatures. Even when appropriate transport media are used, the sensitivity of culture is greatest when the specimen is stored at 4°C before culture and processed within 24 hours of collection (139,155--157).
Specimen Processing
Regardless of the test selected to identify GBS, use of an enrichment broth improves detection substantially. When direct agar plating is used instead of selective enrichment broth, as many as 50% of women who are GBS carriers have false-negative culture results (143,144,158,159). Examples of selective enrichment broths include Todd-Hewitt broth supplemented either with gentamicin (8 µg/ml) and nalidixic acid (15 µg/ml) [TransVag broth] or with colistin (10 µg/ml) and nalidixic acid (15 µg/ml) [Lim broth] (160). Although TransVag and Lim broth media are often available without blood, the addition of 5% sheep blood can increase the recovery of GBS (161). Selective enrichment broth also can contain chromogenic substrates that provide for a change in color in the setting of beta-hemolytic GBS. Such broths can facilitate the identification of beta-hemolytic GBS; however, nonhemolytic isolates will not be detected by these broths alone (162--168). Among 265 GBS isolates from invasive early-onset cases that occurred in the 10 ABCs system areas during 2006--2008, a total of 4% were nonhemolytic (CDC, unpublished data, 2006--2008).
Following enrichment, the conventional means for identifying GBS is through isolation on subculture to blood agar plates and presumptive identification by the CAMP test (169) or serologic identification using latex agglutination with group B streptococcal antisera (170). More recently, chromogenic agars that undergo color change in the presence of beta-hemolytic colonies of GBS have become available (171,172). As with pigmented enrichment broths, these chromogenic agars can facilitate detection of beta-hemolytic GBS, but the majority will not detect nonhemolytic strains. In addition more rapid techniques for identifying GBS directly from enrichment broth, or after subculture have been developed, including DNA probes (173--176) and nucleic acid amplification tests (NAAT) such as polymerase chain reaction (177,178).
Published studies on the performance of commercially available NAAT on nonenriched samples have demonstrated varying sensitivities (range: 62.5%--98.5%) and specificities (range: 64.5%--99.6%) compared with the gold standard of enrichment followed by subculture (179--188) (Table 2). Three studies have compared both intrapartum NAAT on nonenriched samples and late antepartum enriched culture results to intrapartum enriched culture (179,182,185). When comparing swabs collected at the two different time points, two of the studies found intrapartum NAAT to be slightly more sensitive (95.8% and 90.7%, respectively) than antepartum culture (83.3% and 84.3%, respectively) (182,185), although with widely overlapping confidence intervals. One study reported a statistically significant difference between the sensitivity of swabs collected intrapartum and tested with NAAT (94.0%) compared with enriched culture performed on swabs collected prenatally (54.3%) (179). The sensitivity of NAAT for GBS increases to 92.5%--100.0% with use of an enrichment step before testing the sample (177,178,188). Use of an enrichment step lengthens the time to obtain a final result; however, for antenatal testing, the accuracy of results is much more important than timeliness.
Despite the availability of NAAT for GBS, utility of such assays in the intrapartum setting remains limited. Although a highly sensitive and specific test with rapid turnaround time could be used to assess intrapartum GBS colonization and therefore obviate the need for antenatal screening, data on currently available assays do not support their use in replacement of antenatal culture or risk-based assessment of women with unknown GBS status on admission for labor. The additional time required for enrichment of samples makes it not feasible for intrapartum testing, and the sensitivity of assays in the absence of enrichment is not adequate in comparison to culture. In addition, concerns remain regarding real-world turnaround time, test complexity, availability of testing at all times, staffing requirements, and costs. In settings that can perform NAAT, such tests might prove useful for the limited circumstance of a woman at term with unknown colonization status and no other risk factors. Even optimal NAAT would have drawbacks in the intrapartum setting, including a delay in administration of antibiotics while waiting for the result, and no antimicrobial susceptibility testing for penicillin-allergic women. Other rapid tests in addition to NAAT have been developed to detect GBS rapidly from nonenriched samples, including optical immunoassays and enzyme immunoassays; however, none is sufficiently sensitive when used on a direct specimen to detect GBS colonization reliably in the intrapartum setting (180,189--192).
Antimicrobial Susceptibility Testing
Antimicrobial susceptibility testing of GBS isolates is crucial for appropriate antibiotic prophylaxis selection for penicillin-allergic women who are at high risk for anaphylaxis because resistance to clindamycin, the most common agent used in this population, is increasing among GBS isolates. In addition, appropriate methodologies for susceptibility testing are important because inducible clindamycin resistance can occur in some strains that appear susceptible in broth susceptibility tests (193,194). D-zone testing using the double-disk diffusion method has been used to identify isolates that are erythromycin-resistant and clindamycin-susceptible, yet have inducible resistance to clindamycin (195). Isolates that are D-zone positive are considered to have inducible clindamycin resistance and are presumed to be resistant although the clinical significance of this resistance is not clear (196).
Secondary Prevention of Early-Onset GBS Among Infants
Currently available GBS prevention strategies will not prevent all cases of early-onset disease. Rapid detection of neonatal infections and initiation of appropriate treatment is needed to minimize morbidity and mortality among the cases that continue to occur. The detection of early-onset GBS disease poses certain clinical challenges, because neonatal providers must take into account the clinical appearance of the infant, the presence of maternal risk factors for GBS disease, and infant exposure to intrapartum antibiotics.
Infants with Signs of Sepsis
As use of intrapartum antibiotics to prevent early-onset GBS disease increased, concern was expressed that signs of sepsis in the newborn could be delayed or masked, impairing the ability of clinicians to detect early-onset GBS disease (197--199). However, several studies conducted since 1996 have found no significant difference in the clinical presentation of early-onset GBS disease between infants exposed to intrapartum antibiotics and those not exposed (200--204). Approximately 90% of cases of early-onset disease continue to manifest within the first 24 hours of life.
Although maternal GBS colonization might increase clinical suspicion for early-onset GBS disease in an infant, in the era of universal screening, >60% of early-onset GBS cases have occurred among infants born to women who had a negative prenatal GBS culture screen (102,203,204). False-negative cases are not unexpected because culture at 35--37 weeks' gestation will fail to detect some women with intrapartum GBS colonization. As effective prevention strategies are increasingly implemented, a growing proportion of the remaining relatively low burden of disease will reflect inherent limitations in the strategies. Signs of sepsis in any newborn can be an indication of early-onset GBS disease, regardless of maternal colonization status.
Among infants with signs of early-onset disease, the detection of GBS can be increased by performing culture of both blood and cerebrospinal fluid (CSF). Blood cultures can be sterile in as many as 15%--33% of newborns with meningitis (205--209), and the clinical management of an infant with abnormal CSF findings differs from that of an infant with normal CSF.
Infants Born to Women with Chorioamnionitis
Chorioamnionitis is an important risk factor for early-onset GBS disease in women with GBS colonization and can reflect an intrauterine onset of infection in the neonate (45,63,210--212). Intrapartum fever, one sign of chorioamnionitis in parturient women, has been associated with failure of intrapartum antibiotics to prevent GBS disease in the newborn (68,213). Intrapartum treatment of chorioamnionitis can prevent neonatal sepsis (214,215). The diagnosis of chorioamnionitis usually is made clinically on the basis of signs and symptoms such as fever (which might be low-grade), uterine tenderness, fetal tachycardia, maternal tachycardia, and foul-smelling or purulent amniotic fluid. In an effort to avert neonatal infections, maternal fever alone in labor may be used as a sign of chorioamnionitis and hence indication for antibiotic treatment, particularly among women with a significant risk factor for chorioamnionitis (e.g., prolonged labor or prolonged rupture of membranes).
Because an association has been observed between epidural labor analgesia and fever, chorioamnionitis might be overdiagnosed in women with epidurals, which could lead to unnecessary diagnostic evaluations and unnecessary exposure to empirical antibiotics in neonates (216). However, multistate surveillance data suggest that although epidural use is common (in 67% of births), intrapartum temperature of ≥100.4ºF [≥38.0ºC] (3.3% of births) and physician diagnoses of chorioamnionitis (3.1% of births) remain relatively rare (102) (CDC, unpublished data, 2009). Consultation with obstetric providers to determine whether chorioamnionitis is suspected is important for guiding neonatal management.
Well-Appearing Infants Exposed to Inadequate Intrapartum Antibiotics
The management of well-appearing infants whose mothers received inadequate intrapartum antibiotic prophylaxis (because of either a short duration of exposure before delivery or use of an agent with limited efficacy data) can be challenging. Previous GBS prevention guidelines have recommended that infants whose mothers received inadequate intrapartum antibiotic prophylaxis and those <35 weeks' gestational age exposed to intrapartum antibiotics be evaluated with a blood culture and complete blood count (CBC) with differential (13,15). There are limitations to this diagnostic approach. The sensitivity of blood culture can be low among newborns exposed to intrapartum antibiotics (217,218). Available data on the performance of the CBC as a screening test for neonatal sepsis suggest that although the negative predictive value is high, the positive predictive value is low, particularly among healthy-appearing term infants (219--221). The sensitivity of the CBC is lowest immediately after birth, and its performance as a screen for sepsis can be improved by obtaining the blood specimen between 6--12 hours of life (220,222,223). Clinical signs of sepsis have been found to be a more sensitive indicator of neonatal sepsis than hematologic tests (201).
Certain centers provide intramuscular penicillin to asymptomatic infants within 1 hour of birth; this practice is based on results of observational studies demonstrating declines in early-onset GBS disease coincident with a policy of universal administration of intramuscular penicillin to newborns (224--226). However, because the studies used historic control groups and were conducted at a single center that does not screen pregnant women routinely for antenatal GBS colonization, the findings are not generalizable to other settings.
Implementation and Impact of GBS Prevention Efforts
Implementation of the 2002 Guidelines
After the issuance of the 2002 recommendation for universal culture screening, implementation was rapid and widespread. The most robust evaluation comes from a multistate, population-based analysis of 819,000 live births during 2003--2004 (102) and a similarly designed study of births during 1998--1999 (62). The proportion of infants whose mothers were screened for GBS colonization before delivery increased from 48.1% during 1998--1999 to 85.0% during 2003--2004 (Figure 2); among women screened during 2003--2004, a total of 98.4% had a result available at labor. Among screened women, 24.2% were documented as GBS-positive, within the range of expected colonization rates. The proportion of mothers with an indication for intrapartum antibiotic prophylaxis who received them also increased substantially, from 73.8% during 1998--1999 to 85.1% during 2003--2004 (Figure 3).
Despite widespread uptake of universal screening, implementation fell short in several key areas. Infants born preterm have an elevated risk for early-onset disease, and because antenatal screening is recommended at 35--37 weeks of gestation, only 50.3% of women delivering preterm had a known colonization status at the time of hospital admission. Although it is recommended that women with unknown GBS status who deliver preterm receive intrapartum antibiotic prophylaxis, only 63.4% received prophylaxis. In addition, intrapartum antibiotic prophylaxis administration for the indications of GBS bacteriuria or having delivered a previous infant with GBS disease was also low (73.5%) among preterm deliveries. Intrapartum antibiotic prophylaxis was provided to a greater proportion (84.5%) of women delivering preterm who had a positive GBS screening result. Screening for GBS on admission among women with threatened preterm delivery and unknown colonization status was suboptimal; only 18% of women who progressed to delivery and 31% of women who did not progress to delivery were screened despite a recommendation to perform cultures for GBS at hospital admission for this population (15,102).
As anticipated, the proportion of laboring women who received intrapartum antibiotics increased only slightly, from 26.8% to 31.7%, under universal screening. Penicillin and ampicillin, the recommended agents for intrapartum GBS prophylaxis for women with no allergy to penicillin, remained the most common agents administered (76.7% of women receiving intrapartum antibiotic prophylaxis received these agents). However, among penicillin-allergic women, the agents most often administered did not reflect the 2002 recommendations. In particular, only 13.8% of penicillin-allergic women who were not at high risk for anaphylaxis received cefazolin, despite a recommendation that this more effective agent be used. Clindamycin remained the leading agent among penicillin-allergic women (69.9% of those at low risk for anaphylaxis and 83.5% of those at high risk). Among women receiving clindamycin for prophylaxis, clindamycin and erythromycin susceptibility testing were performed rarely despite recommendations that susceptibility testing be conducted on all vaginal-rectal specimens from women who are allergic to penicillin and at high risk for anaphylaxis (15,102). A single-hospital study in Rhode Island reported similar findings (227).
The multistate population-based study conducted during 2003--2004 also identified a greater-than-expected number of cases of early-onset GBS occurring among infants born to women with negative prenatal screening results (61% observed compared with 23%--46% expected cases of early-onset GBS disease among full-term infants) (102). Some false-negative results are expected because culture is not perfectly sensitive and GBS can be acquired by the mother during the period between screening and delivery. However, the high proportion of cases born to women with negative screening results suggests possible problems in the steps required to identify GBS colonization. Suboptimal specimen collection timing, methods, transport, and/or laboratory processing might be contributing factors. Among screened women, the date of the antenatal screening test was missing from 36% of labor and delivery charts. Documentation of the date allows for an assessment of whether screening was performed during the recommended gestation time window.
Trends in Neonatal GBS Disease
Incidence of invasive early-onset GBS disease has declined approximately 80% (Figure 1) since the early 1990s, when implementation of intrapartum antibiotic prophylaxis to prevent GBS disease began. Nationally representative hospital discharge diagnostic code data also demonstrated a steady decrease in clinical sepsis rates during 1990--2002, with a marked decline in clinical sepsis among term infants during the 2 years following the issuance of the 1996 GBS prevention guidelines (228); these data suggest that the observed decline in early-onset GBS disease is a result of prevented cases of illness and not simply of sterilization of neonatal blood cultures as a result of exposure to maternal antibiotics. During 1999--2001, incidence of early-onset GBS disease achieved a plateau of approximately 0.5 cases per 1,000 live births. After the 2002 guidelines were issued, incidence declined further and in recent years has ranged from 0.3 to 0.4 cases per 1,000 live births. This additional decline of 20%--40% is consistent with that predicted for the transition from the 1996 prevention strategy to the universal screening approach recommended in 2002 (62). Similar trends have been reported among infants delivered in all U.S. military hospitals (229). However, the disparity in early-onset GBS disease incidence between black and white infants has persisted (Figure 4) and is evident among both term and preterm infants (18,20). Preliminary surveillance data from 2008 suggest that the racial disparity was reduced somewhat in 2008 (30). Incidence among all black infants declined to 0.49 cases per 1,000 live births, showing progress towards the Healthy People 2010 objective of 0.5 cases per 1,000 live births for all racial and ethnic groups (230). However final data from 2008, including enhanced race/ethnicity reporting on cases and the 2008 live birth denominators, and more years of data are needed to determine whether this trend is sustained.
Trends in Non-GBS Pathogens
Decreases in the incidence of early-onset GBS sepsis have not been accompanied by increases in incidence of early-onset sepsis caused by other pathogens, including those that are antimicrobial-resistant. Most studies, including population-based multicenter studies, have found stable (231--239) or decreasing (240,241) rates of non-GBS early-onset sepsis during a period of increasing use of intrapartum antibiotic prophylaxis for GBS. Increases in invasive Escherichia coli infections have been reported among preterm and low-birth-weight or very low-birth-weight infants (242--246), and some studies have found an increasing proportion of ampicillin-resistant isolates among preterm or very low birth-weight infants with E. coli sepsis (235,245,247). However, the trends have not been consistent over time or across studies. A multicenter study of sepsis in preterm infants that reported an increase in E. coli incidence from 1991--1993 to 1998--2000 (246) found stable rates of E. coli sepsis from 1998--2000 to 2002--2003 and reported no significant change in the proportion of E. coli isolates that were resistant to ampicillin (248). Whether any observed increase in ampicillin-resistant E. coli is attributable to the use of intrapartum antibiotics for GBS prophylaxis is unclear because ampicillin resistance among E. coli isolates has increased communitywide (249). Currently available evidence does not suggest any increase in non-GBS early-onset sepsis among term infants.
An association between intrapartum antibiotic exposure and ampicillin resistance in newborns with E. coli or other non-GBS early-onset sepsis has been observed in several studies among all newborns (55,239,242,250--252) and among preterm or very low birth-weight infants (245,246). However, studies using infants infected with nonresistant pathogens as a control group do not account for ampicillin-susceptible infections prevented by intrapartum antibiotic prophylaxis and therefore might overestimate an association between antibiotic exposure and antibiotic resistance (253). A multicenter case-control study of early-onset E. coli cases that enrolled uninfected infants born at the same hospitals found no association between intrapartum antibiotic prophylaxis exposure and infection with ampicillin-resistant E. coli (254).
The reported increases in E. coli early-onset sepsis among preterm infants and antibiotic-resistant early-onset infections are not of sufficient magnitude to outweigh the benefits of intrapartum antibiotic prophylaxis to prevent early-onset GBS disease. Among all neonates, rates of E. coli early-onset sepsis have remained stable and lower than those of GBS early-onset disease, despite declines in GBS (CDC, unpublished data, 2009). However, to ensure early detection of increases in the rate of disease or deaths caused by organisms other than GBS, continued surveillance of neonatal sepsis caused by organisms other than GBS is needed.
Impact of GBS Prevention Efforts on Infant Management
Provider surveys conducted in the early to mid 1990s indicated that pediatricians and neonatologists were more likely to conduct diagnostic evaluations and initiate empiric antibiotics for an infant whose mother received intrapartum antibiotic prophylaxis than they were for an infant whose mother who did not receive prophylaxis (197--199). Results of studies conducted during 1996--2002 were inconsistent, reporting increased (255), stable (256), or decreased (257) use of health services (including diagnostic tests, antibiotics, and/or length of hospital stay) for neonates born to women receiving intrapartum antibiotics. No studies have reported on the impact of the 2002 guidelines on health-care services for neonates. Continued monitoring of the influence of GBS prevention recommendations on the management of newborns is needed.
Recommendations
The following updated recommendations for the prevention of early-onset GBS disease are based on critical appraisal of data that have become available since publication of previous CDC (13,15) and ACOG (258) recommendations and replace previous recommendations from CDC. These recommendations have been endorsed by ACOG, AAP, ACNM, AAFP, and ASM. After each recommendation, its strength (indicated by a letter) and the quality of supporting evidence (indicated by a Roman numeral) are shown in parentheses according to the evidence-based rating system used (Table 1).
Obstetric and neonatal health-care providers, in conjunction with supporting laboratories and labor and delivery facilities, should adopt the following recommendations for the prevention of early-onset GBS disease.
Identification of Candidates for Intrapartum Antibiotic Prophylaxis
Universal Screening for GBS
Candidates to receive intrapartum antibiotic prophylaxis to prevent early-onset GBS disease should be identified according to the indications and nonindications provided (Table 3).
The following are key components of the screening strategy:
-
Women with GBS isolated from the urine at any time during the current pregnancy or who had a previous infant with invasive GBS disease should receive intrapartum antibiotic prophylaxis and do not need third trimester screening for GBS colonization (AII). Women with symptomatic or asymptomatic GBS urinary tract infection detected during pregnancy should be treated according to current standards of care for urinary tract infection during pregnancy and should receive intrapartum antibiotic prophylaxis to prevent early-onset GBS disease (AIII).
-
All other pregnant women should be screened at 35--37 weeks' gestation for vaginal and rectal GBS colonization (AII).
-
At the time of labor or rupture of membranes, intrapartum antibiotic prophylaxis should be given to all pregnant women who tested positive for GBS colonization (AII), except in the instance of cesarean delivery performed before onset of labor on a woman with intact amniotic membranes.
-
For circumstances in which screening results are not available at the time of labor and delivery, intrapartum antibiotic prophylaxis should be given to women who are <37 weeks and 0 days' gestation, have a duration of membrane rupture ≥18 hours, or have a temperature of ≥100.4º F (≥38.0ºC) (AII).
-
In the absence of GBS urinary tract infection, antimicrobial agents should not be used before the intrapartum period to eradicate GBS genitorectal colonization, because such treatment is not effective in eliminating carriage or preventing neonatal disease and can cause adverse consequences (DI).
-
Intrapartum antibiotic prophylaxis to prevent early-onset GBS disease is not recommended as a routine practice for cesarean deliveries performed before labor onset on women with intact amniotic membranes, regardless of the GBS colonization status of the woman or the gestational age of the pregnancy (CIII). The use of perioperative prophylactic antibiotics to prevent infectious complications of cesarean delivery should not be altered or affected by GBS status. Women expected to undergo cesarean deliveries should undergo routine vaginal and rectal screening for GBS at 35--37 weeks' gestation because onset of labor or rupture of membranes can occur before the planned cesarean delivery, and under those circumstances GBS-colonized women should receive intrapartum antibiotic prophylaxis (AII).
-
Health-care providers should inform women of their GBS screening test result and the recommended interventions (BIII).
The following key changes were made from the 2002 guidelines:
-
Guidance regarding cesarean deliveries performed before onset of labor on a woman with intact amniotic membranes is clarified as applying to cesarean deliveries performed at any gestational age (CIII).
-
In settings in which NAAT for GBS is available, obstetric providers can choose to perform intrapartum testing of vaginal-rectal samples from women with unknown GBS colonization status and no intrapartum risk factors (temperature of ≥100.4º F [≥38.0ºC] or rupture of amniotic membranes ≥18 hours) at the time of testing and who are delivering at term (CII). If an intrapartum risk factor subsequently develops, antibiotic prophylaxis should be administered regardless of the intrapartum testing results (AIII).
-
Women with positive intrapartum NAAT results for GBS should receive antibiotic prophylaxis (AII). NAAT testing is optional and might not be available in all settings.
Threatened Preterm Delivery
Women admitted with signs and symptoms of preterm labor (before 37 weeks and 0 days' gestation) should be managed according to the algorithm provided (Figure 5). Women with rupture of membranes at <37 weeks and 0 days' gestation should be managed according to the algorithm provided (Figure 6).
The following are key components of threatened preterm delivery GBS management:
-
Women admitted with signs and symptoms of labor or with rupture of membranes at <37 weeks and 0 days' gestation should be screened for GBS colonization at hospital admission unless a vaginal-rectal GBS screen was performed within the preceding 5 weeks (AII).
-
Women admitted with signs and symptoms of preterm labor who have unknown GBS colonization status at admission or a positive GBS screen within the preceding 5 weeks should receive GBS prophylaxis at hospital admission (AII).
-
Antibiotics given for GBS prophylaxis to a woman with preterm labor should be discontinued immediately if at any point it is determined that she is not in true labor or if the GBS culture at admission is negative (AII).
-
Negative GBS colonization status should not affect the administration of antibiotics for other indications (AIII).
-
Women with threatened preterm delivery who have a GBS screen performed that is positive and do not deliver at that time should receive GBS prophylaxis when true labor begins (AII).
-
Women with threatened preterm delivery who have a GBS screen performed that is negative but do not deliver at that time should undergo repeat screening at 35--37 weeks' gestation. If such women are re-admitted at a later date with threatened preterm delivery, they should undergo repeat screening if the previous culture was performed >5 weeks prior (AIII).
The following key changes were made from the 2002 guidelines:
-
Separate algorithms are presented for GBS prophylaxis in the setting of threatened preterm delivery, one for spontaneous preterm labor (Figure 5) and one for preterm premature rupture of membranes (Figure 6).
-
GBS prophylaxis provided to women with signs and symptoms of preterm labor should be discontinued if it is determined that the patient is not in true labor (AI).
-
Antibiotics given to prolong latency for preterm premature rupture of membranes with adequate GBS coverage (specifically 2 g ampicillin administered intravenously followed by 1 g administered intravenously every 6 hours for 48 hours) are sufficient for GBS prophylaxis if delivery occurs while the patient is receiving that antibiotic regime (CIII). Oral antibiotics alone are not adequate for GBS prophylaxis (DII).
-
Women with preterm premature rupture of membranes who are not in labor and are receiving antibiotics to prolong latency with adequate GBS coverage should be managed according to standard of care for preterm premature rupture of membranes; GBS testing results should not affect the duration of antibiotics (BIII).
-
Women with preterm premature rupture of membranes who are not in labor and are not receiving antibiotics to prolong latency (or are receiving antibiotics that do not have adequate GBS coverage) should receive GBS prophylaxis for 48 hours, unless a GBS screen performed within the preceding 5 weeks was negative (CIII). If the results from a GBS screen performed on admission become available during that 48-hour period and are negative, then GBS prophylaxis should be discontinued at that time.
GBS Specimen Collection and Processing
GBS specimen collection and processing should be conducted according to the recommendations provided (Boxes 1--3 and Figure 7).
The following are key components of specimen collection and processing:
-
GBS colonization status should be determined by collecting both vaginal and rectal specimens at 35--37 weeks' gestation. A single combined vaginal-rectal specimen can be collected (AII).
-
Specimens should undergo 18--24 hour incubation at 35°--37°C in an appropriate enrichment broth medium to enhance the recovery of GBS (AI).
-
Accurate results are more important than rapid turnaround time for antenatal screening (AIII).
-
To ensure proper testing of specimens, clinicians must inform laboratories when submitted urine specimens are from pregnant women (AIII).
-
Antimicrobial susceptibility testing should be performed on antenatal GBS isolates from penicillin-allergic women at high risk for anaphylaxis because of a history of anaphylaxis, angioedema, respiratory distress, or urticaria following administration of a penicillin or a cephalosporin. (AII) (Box 3).
The following key changes were made from the 2002 guidelines:
-
Specimen transport options and timing until processing are clarified.
-
GBS identification options are expanded to include a positive identification from chromogenic media and identification directly from enriched broth. NAAT, such as commercially available PCR assays, can also be used after enrichment, if laboratories have validated NAAT performance and instituted appropriate quality controls (CII).
-
A direct plating option can be included in addition to enriched culture (CII). Direct plating has a lower sensitivity than enriched culture and should not be used as sole means to identify GBS.
-
Testing for inducible clindamycin resistance should be performed on antenatal GBS isolates that are susceptible to clindamycin, resistant to erythromycin, and are from penicillin-allergic women at high risk for anaphylaxis (CIII).
-
Laboratories should report GBS in urine culture specimens when present at concentrations of ≥104 colony-forming units/ml in pure culture or mixed with a second microorganism (AII) (Box 4).
Intrapartum Antibiotic Prophylaxis
Intrapartum antibiotic prophylaxis agents and dosing should be administered according to the recommendations provided (Figure 8).
The following are key components of intrapartum antibiotic prophylaxis agents and dosing:
-
Penicillin remains the agent of choice for intrapartum antibiotic prophylaxis, with ampicillin as an acceptable alternative (AI).
-
Penicillin-allergic women who do not have a history of anaphylaxis, angioedema, respiratory distress or urticaria following administration of a penicillin or a cephalosporin should receive cefazolin (BII).
-
Antimicrobial susceptibility testing should be ordered for antenatal GBS cultures performed on penicillin-allergic women at high risk for anaphylaxis because of a history of anaphylaxis, angioedema, respiratory distress or urticaria following administration of a penicillin or a cephalosporin (AII). To ensure proper testing, clinicians must inform laboratories of the need for antimicrobial susceptibility testing in such cases (AIII).
-
Penicillin-allergic women at high risk for anaphylaxis should receive clindamycin if their GBS isolate is susceptible to clindamycin and erythromycin, as determined by antimicrobial susceptibility testing; if the isolate is sensitive to clindamycin but resistant to erythromycin, clindamycin may be used if testing for inducible clindamycin resistance is negative (CIII). Penicillin-allergic women at high risk for anaphylaxis should receive vancomycin if their isolate is intrinsically resistant to clindamycin as determined by antimicrobial susceptibility testing, if the isolate demonstrates inducible resistance to clindamycin, or if susceptibility to both agents is unknown (CIII) (Box 3).
The following key changes were made from the 2002 guidelines:
-
The definition of high risk for anaphylaxis is clarified as a history of anaphylaxis, angioedema, respiratory distress or urticaria following administration of a penicillin or a cephalosporin.
-
The recommended dosing regimen of penicillin G is 5 million units intravenously, followed by 2.5--3.0 million units intravenously every 4 hours (AII). The range of 2.5--3.0 million units is recommended to achieve adequate drug levels in the fetal circulation and amniotic fluid while avoiding neurotoxicity. The choice of dose within that range should be guided by which formulations of penicillin G are readily available in order to reduce the need for pharmacies to specially prepare doses.
-
Erythromycin is no longer an acceptable alternative for intrapartum GBS prophylaxis for penicillin-allergic women at high risk for anaphylaxis.
Other Obstetric Management Issues
-
Available data are not sufficient to suggest that GBS colonization should differentially affect the use of obstetric procedures for monitoring, cervical ripening or labor induction. These procedures should be reserved for appropriate indications and not altered for GBS-colonized women (CIII).
-
Data are not sufficient to make recommendations regarding the timing of procedures intended to facilitate progression of labor, such as amniotomy, in GBS-colonized women. Intrapartum antibiotic prophylaxis is optimal if administered for at least 4 hours before delivery; therefore, such procedures should be timed accordingly, if possible (CIII).
-
No medically necessary obstetric procedure should be delayed in order to achieve 4 hours of GBS prophylaxis before delivery (AIII).
Secondary Prevention Among Infants
To detect potential sepsis cases in newborns as early as possible, newborns should be managed according to the algorithm provided (Figure 9).The following are key components of the neonatal management algorithm:
-
Any newborn with signs of sepsis should receive a full diagnostic evaluation and receive antibiotic therapy pending the results of the evaluation. The evaluation should include a blood culture; a CBC including white blood cell differential and platelet count; a chest radiograph if any abnormal respiratory signs are present; and a lumbar puncture if the newborn is stable enough to tolerate the procedure and sepsis is suspected. Therapy for the infant should include antimicrobial agents active against GBS (including intravenous ampicillin) as well as other organisms that might cause neonatal sepsis, such as E. coli (AII).
-
Well-appearing newborns whose mothers had suspected chorioamnionitis should undergo a limited evaluation and receive antibiotic therapy pending culture results (AII). The evaluation should include a blood culture and a CBC including white blood cell differential and platelet count; no chest radiograph or lumbar puncture is needed. Consultation with obstetric providers to assess whether chorioamnionitis was suspected is important to determine neonatal management (CIII).
-
Well-appearing infants whose mothers had no chorioamnionitis and no indication for GBS prophylaxis should be managed according to routine clinical care (CIII).
-
Well-appearing infants of any gestational age whose mother received adequate intrapartum GBS prophylaxis (≥4 hours of penicillin, ampicillin, or cefazolin before delivery) should be observed for ≥48 hours, and no routine diagnostic testing is recommended (BIII). Such infants can be discharged home as early as 24 hours after delivery, assuming that other discharge criteria have been met, ready access to medical care exists, and that a person able to comply fully with instructions for home observation will be present (CIII).
-
For well-appearing infants born to mothers who had an indication for GBS prophylaxis but received no or inadequate prophylaxis, if the infant is well-appearing and ≥37 weeks and 0 days' gestational age and the duration of membrane rupture before delivery was <18 hours, then the infant should be observed for ≥48 hours, and no routine diagnostic testing is recommended (BIII). If the infant is well-appearing and either <37 weeks and 0 days' gestational age or the duration of membrane rupture before delivery was ≥18 hours, then the infant should undergo a limited evaluation and observation for ≥48 hours (BIII).
The following key changes were made from the 2002 guidelines:
-
The algorithm now applies to all newborns.
-
he definition of adequate intrapartum antibiotic prophylaxis is clarified as ≥4 hours of IV penicillin, ampicillin, or cefazolin before delivery (AII). All other agents or durations are considered inadequate for purposes of neonatal management.
-
Well-appearing infants whose mother had an indication for GBS prophylaxis but received no or inadequate intrapartum antibiotics can be managed with observation for ≥48 hours, unless the infant is <37 weeks and 0 days' gestational age or membranes were ruptured ≥18 hours before delivery, in which case a limited evaluation and observation for ≥48 hours is recommended (BIII).
-
Well-appearing infants with a gestational age of 35--36 weeks whose mothers received adequate intrapartum antibiotic prophylaxis do not routinely require diagnostic evaluations (CIII).
Monitoring Implementation and Impact of Guidelines
-
Local and state public health agencies, in conjunction with appropriate groups of hospitals, are encouraged to establish surveillance for early-onset GBS disease and to take other steps to promote perinatal GBS disease prevention and education to reduce the incidence of early-onset GBS disease in their states (CIII).
-
Efforts to monitor the emergence of perinatal infections caused by other organisms are also encouraged (CIII).
Future of GBS Prevention
Although much progress has been made in the prevention of early-onset GBS disease, important challenges remain. Early-onset disease has declined among all racial and ethnic groups, yet significant disparities persist. Research aimed at better understanding racial or ethnic differences in GBS disease might lead to opportunities for more effective prevention efforts. In addition, the evidence is incomplete for several key areas related to GBS prevention, including: strategies to prevent early-onset GBS disease among preterm infants, the role of bacteriuria as a risk factor in the era of universal screening, effectiveness of recommended intrapartum antibiotic prophylaxis agents for penicillin-allergic women at high risk for anaphylaxis, the impact and effectiveness of recommendations for secondary prevention of early-onset GBS disease among neonates, and factors contributing to the higher-than-anticipated proportion of early-onset GBS disease cases occurring among infants born to women with negative prenatal GBS screens.
The development of relatively rapid laboratory tests to identify GBS moves us closer to the possibility of an intrapartum test for GBS colonization screening. A highly sensitive, low-complexity test with a rapid turnaround time could be used to determine intrapartum GBS colonization, thereby overcoming some of the inherent limitations in late antenatal screening. Although available NAATs have demonstrated high sensitivity when performed on enriched samples, enrichment is not feasible in the intrapartum setting when results are needed quickly. Manufacturers and some researchers (180,185) have reported turn-around-times of <2 hours; however, the complexity of available NAAT for GBS is still moderate to high. To be clinically useful in the intrapartum period, a screening test for GBS should consist of a simple bedside kit that enables labor and delivery staff to perform a test, have a turn-around time of <30 minutes, and have a sensitivity and specificity of ≥90%. Ideally, a rapid test for intrapartum use also would be able to detect mutations likely to confer resistance to clindamycin and/or erythromycin in order to guide antibiotic choice for penicillin-allergic women.
Universal screening and intrapartum antibiotic prophylaxis have had no measurable impact on late-onset GBS disease, prenatal-onset disease (including stillbirths and miscarriages), or GBS disease among nonpregnant adults. Because of declines in early-onset GBS disease, the burden of late-onset disease is now similar to that of early-onset disease. More research on preventive measures against late-onset disease is needed. The burden of prenatal-onset GBS disease has not been assessed adequately (32,33,259--262), and no effective prevention tools have been identified before the intrapartum period. GBS disease among nonpregnant adults has increased in recent years. Although GBS vaccines might be expected to aid in reduction of racial disparities and prevention of invasive GBS disease among adults and infants (both early- and late-onset), continued exploration of other means to improve and strengthen GBS prevention efforts is warranted.
Until a safe and efficacious vaccine achieves licensure, continued monitoring for potential unintended consequences of intrapartum antibiotic chemoprophylaxis is needed, with an emphasis on tracking key sentinel events signaling a need for revision of the guidelines. Such sentinel events include the emergence of penicillin resistance among GBS isolates and an increase in the incidence of disease or deaths due to neonatal pathogens other than GBS that offsets the burden of early-onset disease prevented by intrapartum antibiotic prophylaxis. Monitoring for the latter will require long-term surveillance of a large population of term and preterm births (246,248).
States are encouraged to monitor incidence of GBS disease, to promote activities that enhance perinatal GBS disease prevention and education, and to assess progress toward national objectives for disease reduction, such as objectives for Healthy People 2010 (230) and the forthcoming Healthy People 2020 (263). Practical tools to assist with monitoring for missed opportunities for perinatal GBS prevention within hospitals have been published (264); additional prevention information and tools for providers, patients and clinical microbiologists are available at http://www.cdc.gov/groupbstrep, http://www.acog.org, http://www.aap.org, http://www.aafp.org, http://www.midwife.org, and http://www.asm.org.
References
- Baker CJ, Barrett FF, Gordon RC, Yow MD. Suppurative meningitis due to streptococci of Lancefield group B: a study of 33 infants. J Pediatr 1973;82:724--9.
- Barton LL, Feigin RD, Lins R. Group B beta hemolytic streptococcal meningitis in infants. J Pediatr 1973;82:719--23.
- Franciosi RA, Knostman JD, Zimmerman RA. Group B streptococcal neonatal and infant infections. J Pediatr 1973;82:707--18.
- McCracken GH, Jr. Group B streptococci: the new challenge in neonatal infections. J Pediatr 1973;82:703--6.
- Baker CJ, Barrett FF. Group B streptococcal infections in infants. The importance of the various serotypes. JAMA 1974;230:1158--60.
- Allardice JG, Baskett TF, Seshia MM, Bowman N, Malazdrewicz R. Perinatal group B streptococcal colonization and infection. Am J Obstet Gynecol1982;142:617--20.
- Boyer KM, Gotoff SP. Prevention of early-onset neonatal group B streptococcal disease with selective intrapartum chemoprophylaxis. N Engl J Med 1986;314:1665--9.
- Lim DV, Morales WJ, Walsh AF, Kazanis D. Reduction of morbidity and mortality rates for neonatal group B streptococcal disease through early diagnosis and chemoprophylaxis. J Clin Microbiol 1986;23:489--92.
- Tuppurainen N, Hallman M. Prevention of neonatal group B streptococcal disease: intrapartum detection and chemoprophylaxis of heavily colonized parturients. Obstet Gynecol 1989;73:583--7.
- Garland SM, Fliegner JR. Group B Streptococcus (GBS) and neonatal infections: the case for intrapartum chemoprophylaxis. Aust N Z J Obstet Gynaecol 1991;31:119--22.
- Matorras R, Garca-Perea A, Omeaca F, Diez-Enciso M, Madero R, Usandizaga JA. Intrapartum chemoprophylaxis of early-onset group B streptococcal disease. Eur J Obstet Gynecol Reprod Biol 1991;40:57--62.
- American College of Obstetricians and Gynecologists. ACOG committee opinion. Prevention of early-onset group B streptococcal disease in newborns. Number 173,June 1996. Committee on Obstetric Practice. American College of Obstetrics and Gynecologists. Int J Gynaecol Obstet 1996;54:197--205.
- CDC. Prevention of perinatal group B streptococcal disease: a public health perspective. MMWR 1996;45(No. RR-7).
- American Academy of Pediatrics. Revised guidelines for prevention of early-onset group B streptococcal (GBS) infection. American Academy of Pediatrics Committee on Infectious Diseases and Committee on Fetus and Newborn. Pediatrics 1997;99:489--96.
- CDC. Prevention of perinatal group B streptococcal disease: revised guidelines from CDC. MMWR 2002;51(No. RR-11).
- Zangwill KM, Schuchat A, Wenger JD. Group B streptococcal disease in the United States, 1990: report from a multistate active surveillance system. In Surveillance Summaries, November 20, 1992. MMWR 1992;41:25--32.
- Schrag SJ, Zywicki S, Farley MM, Reingold AL, Harrison LH, Lefkowitz LB, et al. Group B streptococcal disease in the era of intrapartum antibiotic prophylaxis. N Engl J Med 2000;342:15--20.
- CDC. Perinatal group B streptococcal disease after universal screening recommendations---United States, 2003--2005. MMWR 2007;56:701--5.
- Phares CR, Lynfield R, Farley MM, Mohle-Boetani J, Harrison LH, Petit S, et al. Epidemiology of invasive group B streptococcal disease in the United States, 1999--2005. JAMA 2008;299:2056--65.
- CDC. Trends in perinatal group B streptococcal disease---United States, 2000--2006. MMWR 2009;58:109--12.
- Pass MA, Gray BM, Dillon HC, Jr. Puerperal and perinatal infections with group B streptococci. Am J Obstet Gynecol 1982;143:147--52.
- Braun TI, Pinover W, Sih P. Group B streptococcal meningitis in a pregnant woman before the onset of labor. Clin Infect Dis 1995;21:1042--3.
- Strasberg GD. Postpartum group B streptococcal endocarditis associated with mitral valve prolapse. Obstet Gynecol 1987;70(3 Pt 2):485--7.
- Aharoni A, Potasman I, Levitan Z, Golan D, Sharf M. Postpartum maternal group B streptococcal meningitis. Rev Infect Dis 1990;12:273--6.
- Yancey MK, Duff P, Clark P, Kurtzer T, Frentzen BH, Kubilis P. Peripartum infection associated with vaginal group B streptococcal colonization. Obstet Gynecol 1994;84:816--9.
- Krohn MA, Hillier SL, Baker CJ. Maternal peripartum complications associated with vaginal group B streptococci colonization. J Infect Dis 1999;179:1410--5.
- Shimoni Z, Ben David M, Niven MJ. Postpartum group B streptococcal tricuspid valve endocarditis. Isr Med Assoc J 2006;8:883--4.
- Locksmith GJ, Clark P, Duff P. Maternal and neonatal infection rates with three different protocols for prevention of group B streptococcal disease. Am J Obstet Gynecol 1999;180:416--22.
- Jordan HT, Farley MM, Craig A, et al. Revisiting the need for vaccine prevention of late-onset neonatal group B streptococcal disease: a multistate, population-based analysis. Pediat Infect Dis J 2008;27:1057--64.
- CDC. Active Bacterial Core Surveillance Report, Emerging Infections Program Network, Group B Streptococcus, 2008. Atlanta, GA: US Department of Health and Human Services, CDC; 2009. Available at http://www.cdc.gov/abcs/reports-findings/survreports/gbs08.html.
- Baker CJ. Early onset group B streptococcal disease. J Pediatr 1978;93:124--5.
- Desa DJ, Trevenen CL. Intrauterine infections with group B beta-haemolytic streptococci. Br J Obstet Gynaecol 1984;91:237--9.
- Katz V, Bowes WA Jr. Perinatal group B streptococcal infections across intact amniotic membranes. J Reprod Med 1988;33:445--9.
- Boyer KM, Gotoff SP. Strategies for chemoprophylaxis of GBS early-onset infections. Antibiot Chemother 1985;35:267--80.
- National Institutes of Health. Summary of the workshop on perinatal infections due to group B Streptococcus. J Infect Dis 1977;136:137--52.
- Regan JA, Klebanoff MA, Nugent RP. The epidemiology of group B streptococcal colonization in pregnancy. Vaginal Infections and Prematurity Study Group. Obstet Gynecol 1991;77:604--10.
- Yancey MK, Schuchat A, Brown LK, Ventura VL, Markenson GR. The accuracy of late antenatal screening cultures in predicting genital group B streptococcal colonization at delivery. Obstet Gynecol 1996;88):811--5.
- Campbell JR, Hillier SL, Krohn MA, Ferrieri P, Zaleznik DF, Baker CJ. Group B streptococcal colonization and serotype-specific immunity in pregnant women at delivery. Obstet Gynecol 2000 Oct;96(4):498--503.
- Lewin EB, Amstey MS. Natural history of group B Streptococcus colonization and its therapy during pregnancy. Am J Obstet Gynecol 1981;139:512--5.
- Hoogkamp-Korstanje JA, Gerards LJ, Cats BP. Maternal carriage and neonatal acquisition of group B streptococci. J Infect Dis 1982;145:800--3.
- Hansen SM, Uldbjerg N, Kilian M, Sorensen UB. Dynamics of Streptococcus agalactiae colonization in women during and after pregnancy and in their infants. J Clin Microbiol 2004;42:83--9.
- Cheng PJ, Chueh HY, Liu CM, Hsu JJ, Hsieh TT, Soong YK. Risk factors for recurrence of group B Streptococcus colonization in a subsequent pregnancy. Obstet Gynecol 2008;111:704--9.
- Turrentine MA, Ramirez MM. Recurrence of group B streptococci colonization in subsequent pregnancy. Obstet Gynecol 2008;112(2 Pt 1):259--64.
- Regan JA, Klebanoff MA, Nugent RP, et al. Colonization with group B streptococci in pregnancy and adverse outcome. VIP Study Group. Am J Obstet Gynecol 1996;174:1354--60.
- Yancey MK, Duff P, Kubilis P, Clark P, Frentzen BH. Risk factors for neonatal sepsis. Obstet Gynecol 1996;87:188--94.
- Liston TE, Harris RE, Foshee S, Null DM, Jr. Relationship of neonatal pneumonia to maternal urinary and neonatal isolates of group B streptococci. South Med J 1979;72:1410--2.
- Wood EG, Dillon HC, Jr. A prospective study of group B streptococcal bacteriuria in pregnancy. Am J Obstet Gynecol 1981;140:515--20.
- Persson K, Bjerre B, Elfstrom L, Polberger S, Forsgren A. Group B streptococci at delivery: high count in urine increases risk for neonatal colonization. Scand J Infect Dis 1986;18:525--31.
- Persson K, Christensen KK, Christensen P, Forsgren A, Jorgensen C, Persson PH. Asymptomatic bacteriuria during pregnancy with special reference to group B streptococci. Scand J Infect Dis 1985;17:195--9.
- Heath PT, Balfour GF, Tighe H, Verlander NQ, Lamagni TL, Efstratiou A. Group B streptococcal disease in infants: a case control study. Arch Dis Child 2009;94:674--80.
- Baker CJ, Edwards MS, Kasper DL. Role of antibody to native type III polysaccharide of group B Streptococcus in infant infection. Pediatrics 1981;68:544--9.
- Boyer KM, Gadzala CA, Burd LI, Fisher DE, Paton JB, Gotoff SP. Selective intrapartum chemoprophylaxis of neonatal group B streptococcal early-onset disease. I. Epidemiologic rationale. J Infect Dis 1983;148:795--801.
- Schuchat A, Oxtoby M, Cochi S, Sikes RK, Hightower A, Plikaytis B, et al. Population-based risk factors for neonatal group B streptococcal disease: results of a cohort study in metropolitan Atlanta. J Infect Dis 1990;162:672--7.
- Schuchat A, Deaver-Robinson K, Plikaytis BD, Zangwill KM, Mohle-Boetani J, Wenger JD. Multistate case-control study of maternal risk factors for neonatal group B streptococcal disease. The Active Surveillance Study Group. Pediatr Infect Dis J 1994;13:623--9.
- Schuchat A, Zywicki SS, Dinsmoor MJ, et al. Risk factors and opportunities for prevention of early-onset neonatal sepsis: a multicenter case-control study. Pediatrics 2000;105(1 Pt 1):21--6.
- Zaleznik DF, Rench MA, Hillier S, et al. Invasive disease due to group B Streptococcus in pregnant women and neonates from diverse population groups. Clin Infect Dis 2000;30:276--81.
- Oddie S, Embleton ND. Risk factors for early onset neonatal group B streptococcal sepsis: case-control study. BMJ (Clinical research ed 2002;325(7359):308.
- Adair CE, Kowalsky L, Quon H, et al. Risk factors for early-onset group B streptococcal disease in neonates: a population-based case-control study. CMAJ 2003;169:198--203.
- Carstensen H, Christensen KK, Grennert L, Persson K, Polberger S. Early-onset neonatal group B streptococcal septicaemia in siblings. J Infect 1988;17:201--4.
- Christensen KK, Dahlander K, Linden V, Svenningsen N, Christensen P. Obstetrical care in future pregnancies after fetal loss in group B streptococcal septicemia. A prevention program based on bacteriological and immunological follow-up. Eur J Obstet Gynecol Reprod Biol 1981;12:143--50.
- Faxelius G, Bremme K, Kvist-Christensen K, Christensen P, Ringertz S. Neonatal septicemia due to group B streptococci---perinatal risk factors and outcome of subsequent pregnancies. J Perinat Med 1988;16:423--30.
- Schrag SJ, Zell ER, Lynfield R, et al. A population-based comparison of strategies to prevent early-onset group B streptococcal disease in neonates. N Engl J Med 2002;347:233--9.
- Adams WG, Kinney JS, Schuchat A, et al. Outbreak of early onset group B streptococcal sepsis. Pediat Infect Dis J 1993;12:565--70.
- Gibbs RS, Schrag S, Schuchat A. Perinatal infections due to group B streptococci. Obstet Gynecol 2004;104(5 Pt 1):1062--76.
- Boulvain M, Stan C, Irion O. Membrane sweeping for induction of labour. Cochrane database of systematic reviews (Online) 2005(1):CD000451.
- Heinemann J, Gillen G, Sanchez-Ramos L, Kaunitz A. Do mechanical methods of cervical ripening increase infectious morbidity? A systematic review. Am J Obstet Gynecol 2008;199:177--87.
- Easmon CS, Hastings MJ, Deeley J, Bloxham B, Rivers RP, Marwood R. The effect of intrapartum chemoprophylaxis on the vertical transmission of group B streptococci. Br J Obstet Gynaecol 1983;90:633--5.
- Lin FY, Brenner RA, Johnson YR, et al. The effectiveness of risk-based intrapartum chemoprophylaxis for the prevention of early-onset neonatal group B streptococcal disease. Am J Obstet Gynecol 2001;184:1204--10.
- Weeks JW, Myers SR, Lasher L, Goldsmith J, Watkins C, Gall SA. Persistence of penicillin G benzathine in pregnant group B Streptococcus carriers. Obstet Gynecol 1997;90:240--3.
- Bland ML, Vermillion ST, Soper DE. Late third-trimester treatment of rectovaginal group B streptococci with benzathine penicillin G. Am J Obstet Gynecol 2000;183:372--6.
- Baecher L, Grobman W. Prenatal antibiotic treatment does not decrease group B Streptococcus colonization at delivery. Int J Gynaecol Obstet 2008;101:125--8.
- Taha TE, Biggar RJ, Broadhead RL, et al. Effect of cleansing the birth canal with antiseptic solution on maternal and newborn morbidity and mortality in Malawi: clinical trial. BMJ (Clinical research ed) 1997;315(7102):216--9; discussion 20.
- Facchinetti F, Piccinini F, Mordini B, Volpe A. Chlorhexidine vaginal flushings versus systemic ampicillin in the prevention of vertical transmission of neonatal group B Streptococcus, at term. J Matern Fetal Neonatal Med 2002;11:84--8.
- Stade B, Shah V, Ohlsson A. Vaginal chlorhexidine during labour to prevent early-onset neonatal group B streptococcal infection. Cochrane database of systematic reviews (Online) 2004(3):CD003520.
- Bakr AF, Karkour T. Effect of predelivery vaginal antisepsis on maternal and neonatal morbidity and mortality in Egypt. J Women's Health 2005;14:496--501.
- Cutland CL, Madhi SA, Zell ER, et al. Chlorhexidine maternal-vaginal and neonate body wipes in sepsis and vertical transmission of pathogenic bacteria in South Africa: a randomised, controlled trial. Lancet 374 (9705):1909--1916.
- Saleem S, Rouse D, McClure E, et al. Chlorhexidine vaginal and infant wipes to reduce perinatal mortality and morbidity: a randomized controlled trial. Obstet Gynecol 2010;115:1225--32.
- Edwards RK, Clark P, Sistrom CL, Duff P. Intrapartum antibiotic prophylaxis 1: relative effects of recommended antibiotics on gram-negative pathogens. Obstet Gynecol 2002;100:534--9.
- Bray RE, Boe RW, Johnson WL. Transfer of ampicillin into fetus and amniotic fluid from maternal plasma in late pregnancy. Am J Obstet Gynecol 1966;96:938--42.
- Bloom SL, Cox SM, Bawdon RE, Gilstrap LC. Ampicillin for neonatal group B streptococcal prophylaxis: how rapidly can bactericidal concentrations be achieved? Am J Obstet Gynecol 1996;175(4 Pt 1):974--6.
- Colombo DF, Lew JL, Pedersen CA, Johnson JR, Fan-Havard P. Optimal timing of ampicillin administration to pregnant women for establishing bactericidal levels in the prophylaxis of group B Streptococcus. Am J Obstet Gynecol 2006;194:466--70.
- Fossieck B, Parker RH. Neurotoxicity during intravenous infusion of penicillin. A review. J Clin Pharmacol 1974;14:504--12.
- Chow KM, Hui AC, Szeto CC. Neurotoxicity induced by beta-lactam antibiotics: from bench to bedside. Eur J Clin Microbiol Infect Dis 2005;24:649--53.
- Illuzzi JL, Bracken MB. Duration of intrapartum prophylaxis for neonatal group B streptococcal disease: a systematic review. Obstet Gynecol 2006;108:1254--65.
- Barber EL, Zhao G, Buhimschi IA, Illuzzi JL. Duration of intrapartum prophylaxis and concentration of penicillin G in fetal serum at delivery. Obstet Gynecol 2008;112(2 Pt 1):265--70.
- de Cueto M, Sanchez MJ, Sampedro A, Miranda JA, Herruzo AJ, Rosa-Fraile M. Timing of intrapartum ampicillin and prevention of vertical transmission of group B Streptococcus. Obstet Gynecol 1998;91:112--4.
- Fiore Mitchell T, Pearlman MD, Chapman RL, Bhatt-Mehta V, Faix RG. Maternal and transplacental pharmacokinetics of cefazolin. Obstet Gynecol 2001;98:1075--9.
- Allegaert K, van Mieghem T, Verbesselt R, et al. Cefazolin pharmacokinetics in maternal plasma and amniotic fluid during pregnancy. Am J Obstet Gynecol 2009;200:170 e1--7.
- Popovic J, Grujic Z, Sabo A. Influence of pregnancy on ceftriaxone, cefazolin and gentamicin pharmacokinetics in caesarean vs. non-pregnant sectioned women. J Clin Pharm Ther 2007;32:595--602.
- Kelkar PS, Li JT. Cephalosporin allergy. N Engl J Med 2001;345:804--9.
- Pacifici GM. Placental transfer of antibiotics administered to the mother: a review. Int J Clin Pharm Ther 2006;44:57--63.
- Laiprasert J, Klein K, Mueller BA, Pearlman MD. Transplacental passage of vancomycin in noninfected term pregnant women. Obstet Gynecol 2007;109:1105--10.
- Philipson A. Pharmacokinetics of antibiotics in pregnancy and labour. Clin Pharmacokinet 1979;4:297--309.
- Philipson A, Sabath LD, Charles D. Transplacental passage of erythromycin and clindamycin. N Engl J Med 1973;288:1219--21.
- Muller A, Mouton J, Oostvogel P, et al. Pharmacokinetics of clindamycin in pregnant women in the peripartum period. Antimicrob Agents Chemother 2010;54:2175--81.
- Petri W. Penicillins, Cephalosporins, and other B-lactam antibiotics. In: Brunton L, Lazo J, Parker K, eds. Goodman & Gilman's The pharmacologicical basis of therapeutics. 11th ed. New York, NY: McGraw-Hill; 2006.
- Pylipow M, Gaddis M, Kinney JS. Selective intrapartum prophylaxis for group B Streptococcus colonization: management and outcome of newborns. Pediatrics 1994;93:631--5.
- Dunn AB, Blomquist J, Khouzami V. Anaphylaxis in labor secondary to prophylaxis against group B Streptococcus. A case report. J Reprod Med 1999;44:381--4.
- Gei AF, Pacheco LD, Vanhook JW, Hankins GD. The use of a continuous infusion of epinephrine for anaphylactic shock during labor. Obstet Gynecol 2003;102:1332--5.
- Sheikh J. Intrapartum anaphylaxis to penicillin in a woman with rheumatoid arthritis who had no prior penicillin allergy. Ann Allergy Asthma Immunol 2007;99:287--9.
- Chaudhuri K, Gonzales J, Jesurun CA, Ambat MT, Mandal-Chaudhuri S. Anaphylactic shock in pregnancy: a case study and review of the literature. Int J Obstet Anesth 2008;17:350--7.
- Van Dyke MK, Phares CR, Lynfield R, et al. Evaluation of universal antenatal screening for group B Streptococcus. N Engl J Med 2009;360:2626--36.
- Schatz M, Zeiger R, Falkoff R, et al. Asthma and allergic diseases during pregnancy. In: Adkinson N, Bochner B, Busse W, Holgate S, Simons F, eds. Middleton's allergy: principles and practice. 7th ed. Maryland Heights, MO: Mosby; 2008:1423--33.
- Jaureguy F, Carton M, Panel P, Foucaud P, Butel MJ, Doucet-Populaire F. Effects of intrapartum penicillin prophylaxis on intestinal bacterial colonization in infants. J Clin Microbiol 2004;42:5184--8.
- Chen KT, Puopolo KM, Eichenwald EC, Onderdonk AB, Lieberman E. No increase in rates of early-onset neonatal sepsis by antibiotic-resistant group B Streptococcus in the era of intrapartum antibiotic prophylaxis. Am J Obstet Gynecol 2005;192:1167--71.
- Borchardt SM, DeBusscher JH, Tallman PA, et al. Frequency of antimicrobial resistance among invasive and colonizing group B streptococcal isolates. BMC Infect Dis 2006;6:57.
- Chohan L, Hollier LM, Bishop K, Kilpatrick CC. Patterns of antibiotic resistance among group B Streptococcus isolates: 2001--2004. Infect Dis Obstet Gynecol 2006;57492.
- Castor ML, Whitney CG, Como-Sabetti K. Antibiotic resistance patterns in invasive group B streptococcal isolates. Infect Dis Obstet Gynecol 2008;727505.
- Panda B, Iruretagoyena I, Stiller R, Panda A. Antibiotic resistance and penicillin tolerance in ano-vaginal group B streptococci. J Matern Fetal Neonatal Med 2009;22:111--4.
- Kimura K, Suzuki S, Wachino J, et al. First molecular characterization of group B streptococci with reduced penicillin susceptibility. Antimicrob Agents Chemoth 2008;52:2890--7.
- Dahesh S, Hensler ME, Van Sorge NM, et al. Point mutation in the group B streptococcal pbp2x gene conferring decreased susceptibility to beta-lactam antibiotics. Antimicrob Agents Chemother 2008;52:2915--8.
- Clinical and Laboratory Standards Institute. Performance standards for antimicrobial susceptibility testing. CLSI M100-S20. Wayne, PA; 2010.
- Baker CJ, Rench MA, Edwards MS, Carpenter RJ, Hays BM, Kasper DL. Immunization of pregnant women with a polysaccharide vaccine of group B Streptococcus. N Engl J Med 1988;319:1180--5.
- Schuchat A, Wenger JD. Epidemiology of group B streptococcal disease: risk factors, prevention strategies, and vaccine development. Epidemiol Rev 1994;16:374--402.
- Baker CJ, Kasper DL. Correlation of maternal antibody deficiency with susceptibility to neonatal group B streptococcal infection. N Engl J Med 1976 Apr 1;294:753--6.
- Baker CJ, Edwards MS. Group B streptococcal conjugate vaccines. Arch Dis Child 2003;88:375--8.
- Heath PT, Feldman RG. Vaccination against group B Streptococcus. Expert Review of Vaccines 2005;4:207--18.
- Edwards MS. Group B streptococcal conjugate vaccine: a timely concept for which the time has come. Human Vaccines 2008;4:444--8.
- Kasper DL, Paoletti LC, Wessels MR, et al. Immune response to type III group B streptococcal polysaccharide-tetanus toxoid conjugate vaccine. J Clin Invest 1996;98:2308--14.
- Baker CJ, Paoletti LC, Wessels MR, et al. Safety and immunogenicity of capsular polysaccharide-tetanus toxoid conjugate vaccines for group B streptococcal types Ia and Ib. J Infect Dis 1999;179:142--50.
- Baker CJ, Paoletti LC, Rench MA, et al. Use of capsular polysaccharide-tetanus toxoid conjugate vaccine for type II group B Streptococcus in healthy women. J Infect Dis 2000;182:1129--38.
- Hillier S, Ferris D, Fine D, Ferrieri P, et al. Women receiving group B Streptococcus serotype III tetanus toxoid (GBS III-TT) vaccine have reduced vaginal and rectal acquisition of GBS type III [Presentation]. Annual meeting of the Infectious Diseases Society of America, Philadelphia, Pennsylvania; October 20--November 1, 2009.
- Mercer BM, Miodovnik M, Thurnau GR, et al. Antibiotic therapy for reduction of infant morbidity after preterm premature rupture of the membranes: a randomized controlled trial. National Institute of Child Health and Human Development Maternal-Fetal Medicine Units Network. JAMA 1997;278:989--95.
- American College of Obstetricians and Gynecologists. ACOG practice bulletin number 47, October 2003: prophylactic antibiotics in labor and delivery. Obstet Gynecol 2003;102:875--82.
- Owen J, Groome LJ, Hauth JC. Randomized trial of prophylactic antibiotic therapy after preterm amnion rupture. Am J Obstet Gynecol 1993;169:976--81.
- Kenyon SL, Taylor DJ, Tarnow-Mordi W. Broad-spectrum antibiotics for preterm, prelabour rupture of fetal membranes: the ORACLE I randomised trial. ORACLE Collaborative Group. Lancet 2001;357(9261):979--88.
- Kenyon SL, Taylor DJ, Tarnow-Mordi W. Broad-spectrum antibiotics for spontaneous preterm labour: the ORACLE II randomised trial. ORACLE Collaborative Group. Lancet 2001;357(9261):989--94.
- Kenyon S, Pike K, Jones DR, et al. Childhood outcomes after prescription of antibiotics to pregnant women with spontaneous preterm labour: 7-year follow-up of the ORACLE II trial. Lancet 2008;372(9646):1319--27.
- Moller M, Thomsen AC, Borch K, Dinesen K, Zdravkovic M. Rupture of fetal membranes and premature delivery associated with group B streptococci in urine of pregnant women. Lancet 1984;2(8394):69--70.
- McKenna DS, Matson S, Northern I. Maternal group B streptococcal (GBS) genital tract colonization at term in women who have asymptomatic GBS bacteriuria. Infectious diseases in Obstet Gynecol 2003;11(4):203--7.
- Hall RT, Barnes W, Krishnan L, Harris DJ, Rhodes PG, Fayez J, et al. Antibiotic treatment of parturient women colonized with group B streptococci. Am J Obstet Gynecol 1976;124:630--4.
- Gardner SE, Yow MD, Leeds LJ, Thompson PK, Mason EO Jr, Clark DJ. Failure of penicillin to eradicate group B streptococcal colonization in the pregnant woman. A couple study. Am J Obstet Gynecol 1979;135:1062--5.
- Edwards RK, Clark P, Duff P. Intrapartum antibiotic prophylaxis 2: positive predictive value of antenatal group B streptococci cultures and antibiotic susceptibility of clinical isolates. Obstet Gynecol 2002;100:540--4.
- Centelles-Serrano MJ, Perez-Moreno MO, Llovet-Lombarte MI, Cortell-Ortola M, Jardi-Baiges AM, Buj-Gonzalez JI. [Effectiveness of systematic investigation for group B Streptococcus in urine samples to identify colonized pregnant women]. Enferm Infecc Microbiol Clin 2009;27:394--8.
- Weng C, Korgenski K, Sheng X, Byington C. Pregnancy outcomes in women with group B streptococcal bacteriuria. Annual Meeting of the Pediatric Academic Societies, Vancouver, Canada; May 1--4, 2010.
- McCarter YS, Burd EM, Hall GS, Zervos M. Cumitech 2C: laboratory diagnosis of urinary tract infections. Washington, DC: ASM Press; 2009.
- Lin K, Fajardo K. Screening for asymptomatic bacteriuria in adults: evidence for the U.S. Preventive Services Task Force reaffirmation recommendation statement. Ann Inter Med 2008;149:W20--4.
- Ramus R, McIntire D, Wendell GJ. Antibiotic chemoprophylaxis for group B strep is not necessary with elective cesarean section at term [Abstract]. Am J Obstet Gynecol 1999;180(Suppl):85.
- Hakansson S, Axemo P, Bremme K, et al. Group B streptococcal carriage in Sweden: a national study on risk factors for mother and infant colonisation. Acta Obstet Gynecol Scand 2008;87:50--8.
- Boyer KM, Gadzala CA, Kelly PD, Burd LI, Gotoff SP. Selective intrapartum chemoprophylaxis of neonatal group B streptococcal early-onset disease. II. Predictive value of prenatal cultures. J Infect Dis 1983;148:802--9.
- Badri MS, Zawaneh S, Cruz AC, Mantilla G, Baer H, Spellacy WN, et al. Rectal colonization with group B Streptococcus: relation to vaginal colonization of pregnant women. J Infect Dis 1977;135:308--12.
- Dillon HC, Gray E, Pass MA, Gray BM. Anorectal and vaginal carriage of group B streptococci during pregnancy. J Infect Dis 1982;145:794--9.
- Philipson EH, Palermino DA, Robinson A. Enhanced antenatal detection of group B Streptococcus colonization. Obstet Gynecol 1995;85:437--9.
- Platt MW, McLaughlin JC, Gilson GJ, Wellhoner MF, Nims LJ. Increased recovery of group B Streptococcus by the inclusion of rectal culturing and enrichment. Diagn Microbiol Infect Dis 1995;21:65--8.
- Quinlan JD, Hill DA, Maxwell BD, Boone S, Hoover F, Lense JJ. The necessity of both anorectal and vaginal cultures for group B Streptococcus screening during pregnancy. J Fam Pract 2000;49:447--8.
- Kovavisarach E, Sa-adying W, Kanjanahareutai S. Comparison of combined vaginal-anorectal, vaginal and anorectal cultures in detecting of group B streptococci in pregnant women in labor. Journal of the Medical Association of Thailand [Chotmaihet thangphaet] 2007;90:1710--4.
- Orafu C, Gill P, Nelson K, Hecht B, Hopkins M. Perianal versus anorectal specimens: is there a difference in group B streptococcal detection? Obstet Gynecol 2002;99:1036--9.
- Jamie WE, Edwards RK, Duff P. Vaginal-perianal compared with vaginal-rectal cultures for identification of group B streptococci. Obstet Gynecol 2004;104(5 Pt 1):1058--61.
- Mercer BM, Taylor MC, Fricke JL, Baselski VS, Sibai BM. The accuracy and patient preference for self-collected group B Streptococcus cultures. American journal of Obstet Gynecol 1995;173:1325--8.
- Molnar P, Biringer A, McGeer A, McIsaac W. Can pregnant women obtain their own specimens for group B Streptococcus? A comparison of maternal versus physician screening. The Mount Sinai GBS Screening Group. Fam Pract 1997;14:403--6.
- Price D, Shaw E, Howard M, Zazulak J, Waters H, Kaczorowski J. Self-sampling for group B Streptococcus in women 35 to 37 weeks pregnant is accurate and acceptable: a randomized cross-over trial. J Obstet Gynaecol Can 2006;28:1083--8.
- Arya A, Cryan B, O'Sullivan K, Greene RA, Higgins JR. Self-collected versus health professional-collected genital swabs to identify the prevalence of group B Streptococcus: a comparison of patient preference and efficacy. Eur J Obstet, Gynecol Reprod Biol 2008;139:43--5.
- Teese N, Henessey D, Pearce C, Kelly N, Garland S. Screening protocols for group B Streptococcus: are transport media appropriate? Infect Dis Obstet Gynecol 2003;11:199--202.
- Crisp BJ, Yancey MK, Uyehara C, Nauschuetz WF. Effect of delayed inoculation of selective media in antenatal detection of group B streptococci. Obstet Gynecol 1998;92:923--5.
- Ostroff RM, Steaffens JW. Effect of specimen storage, antibiotics, and feminine hygiene products on the detection of group B Streptococcus by culture and the strep B OIA test. Diagn Microbiol Infect Dis 1995l;22:253--9.
- Stoner KA, Rabe LK, Hillier SL. Effect of transport time, temperature, and concentration on the survival of group B streptococci in Amies transport medium. J Clin Microbiol 2004;42:5385--7.
- Rosa-Fraile M, Camacho-Munoz E, Rodriguez-Granger J, Liebana-Martos C. Specimen storage in transport medium and detection of group B streptococci by culture. J Clin Microbiol 2005;43:928--30.
- Baker CJ, Clark DJ, Barrett FF. Selective broth medium for isolation of group B streptococci. Appl Microbiol 1973;26:884--5.
- Altaie SS, Dryja D. Detection of group B Streptococcus. Comparison of solid and liquid culture media with and without selective antibiotics. Diagn Microbiol Infect Dis 1994;18:141--4.
- Fenton LJ, Harper MH. Evaluation of colistin and nalidixic acid in Todd-Hewitt broth for selective isolation of group B streptocci. J Clin Microbiol 1979;9:167--9.
- MacfFaddin J. Media for isolation-cultivation-identification-maintenance of medical bacteria. Baltimore, MD: Williams & Wilkins; 1985.
- de la Rosa M, Perez M, Carazo C, Pareja L, Peis JI, Hernandez F. New Granada medium for detection and identification of group B streptococci. J Clin Microbiol 1992 Apr;30:1019--21.
- Rosa-Fraile M, Rodrguez-Granger J, Haidour-Benamin A, Cuerva J, Sampedro A. Granadaene: proposed structure of the group B Streptococcus polyenic pigment. Appl Environ Microbiol 2006;72:6367--70.
- Church DL, Baxter H, Lloyd T, Miller B, Elsayed S. Evaluation of StrepB carrot broth versus Lim broth for detection of group B Streptococcus colonization status of near-term pregnant women. J Clin Microbiol 2008;46:2780--2.
- Martinho F, Prieto E, Pinto D, et al. Evaluation of liquid biphasic Granada medium and instant liquid biphasic Granada medium for group B Streptococcus detection. Enferm Infecc Microbiol Clin 2008;26:69--71.
- Adler A, Block C, Engelstein D, Hochner-Celnikcier D, Drai-Hassid R, Moses AE. Culture-based methods for detection and identification of Streptococcus agalactiae in pregnant women---what are we missing? Eur J Clin Microbiol Infect Dis 2008;27:241--3.
- Smith D, Perry J, Laine L, Galloway A, Gould FK. Comparison of BD GeneOhm real-time polymerase chain reaction with chromogenic and conventional culture methods for detection of group B Streptococcus in clinical samples. Diagn Microbiol Infect Dis2008;61:369--72.
- Carvalho MD, Facklam R, Jackson D, Beall B, McGee L. Evaluation of three commercial broth media for pigment detection and identification of group B streptococci (GBS), Streptococcus agalactiae. J Clin Microbiol 2009;47:4161--3.
- Wilkinson HW. CAMP-disk test for presumptive identification of group B streptococci. J Clin Microbiol 1977;6:42--5.
- Guerrero C, Martinez J, Menasalvas A, Blazquez R, Rodriguez T, Segovia M. Use of direct latex agglutination testing of selective broth in the detection of group B streptococcal carriage in pregnant women. Eur J Clin Microbiol Infect Dis 2004;23:61--2.
- Votava M, Tejkalov M, Drbkov M, Unzeitig V, Braveny I. Use of GBS media for rapid detection of group B streptococci in vaginal and rectal swabs from women in labor. Eur J Clin Microbiol Infect Dis 2001;20:120--2.
- Tazi A, Reglier-Poupet H, Dautezac F, Raymond J, Poyart C. Comparative evaluation of Strepto B ID chromogenic medium and Granada media for the detection of group B Streptococcus from vaginal samples of pregnant women. J Microbiol Methods 2008;73:263--5.
- Ryan KM, Lencki SG, Elder BL, Northern WI, Khamis HJ, Bofill JA. DNA probe for beta-hemolytic group B Streptococcus. Diagnostic accuracy in threatened preterm labor. J Reprod Med 1999;44:587--91.
- Williams-Bouyer N, Reisner BS, Woods GL. Comparison of gen-probe AccuProbe group B Streptococcus culture identification test with conventional culture for the detection of group B streptococci in broth cultures of vaginal-anorectal specimens from pregnant women. Diagn Microbiol Infect Dis2000;36:159--62.
- Montague N, Cleary T, Martinez O, Procop G. Detection of group B streptococci in Lim broth by use of group B Streptococcus peptide nucleic acid fluorescent in situ hybridization and selective and nonselective agars. J Clin Microbiol 2008;46:3470--2.
- Peltroche-Llacsahuanga H, Fiandaca M, von Oy S, Ltticken R, Haase G. Rapid detection of Streptococcus agalactiae from swabs by peptide nucleic acid fluorescence in situ hybridization. J Med Microbiol 59:179--84.
- Goodrich JS, Miller MB. Comparison of culture and 2 real-time polymerase chain reaction assays to detect group B Streptococcus during antepartum screening. Diagn Microbiol Infect Dis 2007;59:17--22.
- Block T, Munson E, Culver A, Vaughan K, Hryciuk JE. Comparison of carrot broth- and selective Todd-Hewitt broth-enhanced PCR protocols for real-time detection of Streptococcus agalactiae in prenatal vaginal/anorectal specimens. J Clin Microbiol 2008;46:3615--20.
- Davies HD, Miller MA, Faro S, Gregson D, Kehl SC, Jordan JA. Multicenter study of a rapid molecular-based assay for the diagnosis of group B Streptococcus colonization in pregnant women. Clin Infect Dis 2004;39:1129--35.
- Aziz N, Baron EJ, D'Souza H, Nourbakhsh M, Druzin ML, Benitz WE. Comparison of rapid intrapartum screening methods for group B streptococcal vaginal colonization. J Matern Fetal Neonatal Med 2005;18:225--9.
- Atkins KL, Atkinson RM, Shanks A, Parvin CA, Dunne WM, Gross G. Evaluation of polymerase chain reaction for group B Streptococcus detection using an improved culture method. Obstet Gynecol 2006;108(3 Pt 1):488--91.
- Gavino M, Wang E. A comparison of a new rapid real-time polymerase chain reaction system to traditional culture in determining group B Streptococcus colonization. Am J Obstet Gynecol 2007;197:388 e1--4.
- Smith D, Perry JD, Laine L, Galloway A, Gould FK. Comparison of BD GeneOhm real-time polymerase chain reaction with chromogenic and conventional culture methods for detection of group B Streptococcus in clinical samples. Diagn Microbiol Infect Dis 2008;61:369--72.
- Edwards RK, Novak-Weekley SM, Koty PP, Davis T, Leeds LJ, Jordan JA. Rapid group B streptococci screening using a real-time polymerase chain reaction assay. Obstet Gynecol 2008;111:1335--41.
- Money D, Dobson S, Cole L, et al. An evaluation of a rapid real time polymerase chain reaction assay for detection of group B Streptococcus as part of a neonatal group B Streptococcus prevention strategy. J Obstet Gynaecol Can 2008;30:770--5.
- El Helali N, Nguyen JC, Ly A, Giovangrandi Y, Trinquart L. Diagnostic accuracy of a rapid real-time polymerase chain reaction assay for universal intrapartum group B Streptococcus screening. Clin Infect Dis 2009;49:417--23l.
- Alfa MJ, Sepehri S, De Gagne P, Helawa M, Sandhu G, Harding GK. Real-time PCR assay provides reliable assessment of intrapartum carriage of group BStreptococcus. J Clin Microbiol 2010 Jun 30. [Epub ahead of print].
- Scicchitano L, Bourbeau P. Comparative evaluation of the AccuProbe group B Streptococcus culture test, the BD GeneOhm Strep B assay, and culture for detection of group B streptococci in pregnant women. J Clin Microbiol 2009;47:3021--3.
- Baker CJ. Inadequacy of rapid immunoassays for intrapartum detection of group B streptococcal carriers. Obstet Gynecol 1996;88:51--5.
- Thinkhamrop J, Limpongsanurak S, Festin M, et al. Infections in international pregnancy study: performance of the optical immunoassay test for detection of group B Streptococcus. J Clin Microbiol 2003;41:5288--90.
- Honest H, Sharma S, Khan K. Rapid tests for group B Streptococcus colonization in laboring women: a systematic review. Pediatrics 2006;117:1055--66.
- Daniels J, Gray J, Pattison H, et al. Rapid testing for group B Streptococcus during labour: a test accuracy study with evaluation of acceptability and cost-effectiveness. Health Technol Assess 2009;13:1--154, iii.
- Tang P, Ng P, Lum M, et al. Use of the Vitek-1 and Vitek-2 systems for detection of constitutive and inducible macrolide resistance in group B streptococci. J Clin Microbiol 2004;42(5):2282--4.
- Richter S, Howard W, Weinstein M, et al. Multicenter evaluation of the BD Phoenix Automated Microbiology System for antimicrobial susceptibility testing of Streptococcus species. J Clin Microbiol 2007;45:2863--71.
- Clinical and Laboratory Standards Institute. Performance standard for antimicrobial susceptability testing, M100--S20. Wayne, PA; 2010.
- Desjardins M, Delgaty KL, Ramotar K, Seetaram C, Toye B. Prevalence and mechanisms of erythromycin resistance in group A and group B Streptococcus: implications for reporting susceptibility results. J Clin Microbiol 2004;42:5620--3.
- Wiswell TE, Stoll BJ, Tuggle JM. Management of asymptomatic, term gestation neonates born to mothers treated with intrapartum antibiotics. Pediatr Infect Dis J 1990;9:826--31.
- Mercer BM, Ramsey RD, Sibai BM. Prenatal screening for group B Streptococcus. II. Impact of antepartum screening and prophylaxis on neonatal care. Am J Obstet Gynecol 1995;173(3 Pt 1):842--6.
- Peralta-Carcelen M, Fargason CA Jr, Cliver SP, Cutter GR, Gigante J, Goldenberg RL. Impact of maternal group B streptococcal screening on pediatric management in full-term newborns. Arch Pediatr Adolesc Med 1996;150:802--8.
- Bromberger P, Lawrence JM, Braun D, Saunders B, Contreras R, Petitti DB. The influence of intrapartum antibiotics on the clinical spectrum of early-onset group B streptococcal infection in term infants. Pediatrics 2000;106(2 Pt 1):244--50.
- Escobar GJ, Li DK, Armstrong MA, et al. Neonatal sepsis workups in infants >/=2000 grams at birth: a population-based study. Pediatrics 2000;106(2 Pt 1):256--63.
- Pinto NM, Soskolne EI, Pearlman MD, Faix RG. Neonatal early-onset group B streptococcal disease in the era of intrapartum chemoprophylaxis: residual problems. J Perinatol 2003;23:265--71.
- Pulver LS, Hopfenbeck MM, Young PC, Stoddard GJ, Korgenski K, Daly J, et al. Continued early onset group B streptococcal infections in the era of intrapartum prophylaxis. J Perinatol 2009;29:20--5.
- Puopolo KM, Madoff LC, Eichenwald EC. Early-onset group B streptococcal disease in the era of maternal screening. Pediatrics 2005;115:1240--6.
- Visser VE, Hall RT. Lumbar puncture in the evaluation of suspected neonatal sepsis. J Pediatr 1980;96:1063--7.
- Hristeva L, Booy R, Bowler I, Wilkinson AR. Prospective surveillance of neonatal meningitis. Arch Dis Child 1993;69(1 Spec No):14--8.
- Wiswell TE, Baumgart S, Gannon CM, Spitzer AR. No lumbar puncture in the evaluation for early neonatal sepsis: will meningitis be missed? Pediatrics 1995;95:803--6.
- Stoll B, Hansen N, Fanaroff A, et al. To tap or not to tap: high likelihood of meningitis without sepsis among very low birth weight infants. Pediatrics 2004;113:1181--6.
- Ansong A, Smith PB, Benjamin D, Clark R, Li J, Cotten CM, et al. Group B streptococcal meningitis: cerebrospinal fluid parameters in the era of intrapartum antibiotic prophylaxis. Early Hum Dev 2009;85(10 Suppl):S5--7.
- Benitz WE, Gould JB, Druzin ML. Risk factors for early-onset group B streptococcal sepsis: estimation of odds ratios by critical literature review. Pediatrics 1999;103:e77.
- Dillon HC, Jr., Khare S, Gray BM. Group B streptococcal carriage and disease: a 6-year prospective study. J Pediatr 1987;110:31--6.
- Gilstrap LC, 3rd, Leveno KJ, Cox SM, Burris JS, Mashburn M, Rosenfeld CR. Intrapartum treatment of acute chorioamnionitis: impact on neonatal sepsis. Am J Obstet Gynecol 1988;159:579--83.
- Ascher DP, Becker JA, Yoder BA, Weisse M, Waecker NJ, Heroman WM, et al. Failure of intrapartum antibiotics to prevent culture-proved neonatal group B streptococcal sepsis. J Perinatol 1993;13:212--6.
- Gibbs RS, Dinsmoor MJ, Newton ER, Ramamurthy RS. A randomized trial of intrapartum versus immediate postpartum treatment of women with intra-amniotic infection. Obstet Gynecol 1988;72:823--8.
- Sperling RS, Ramamurthy RS, Gibbs RS. A comparison of intrapartum versus immediate postpartum treatment of intra-amniotic infection. Obstet Gynecol 1987;70:861--5.
- Lieberman E, Lang JM, Frigoletto F Jr, Richardson DK, Ringer SA, Cohen A. Epidural analgesia, intrapartum fever, and neonatal sepsis evaluation. Pediatrics 1997;99:415--9.
- Safier R, Robins S, Picone C, Tafari N. blood culture screening of newborns at risk for early onset neonatal group B streptococcal disease [Abstract]. Annual meeting of the Pediatric Academic Societies, Baltimore, Maryland; May 4--7, 2002.
- Hsu KK, Pelton SI, Shapiro DS. Detection of group B streptococcal bacteremia in simulated intrapartum antimicrobial prophylaxis. Diagn Microbiol Infect Dis 2003;45:23--7.
- Gerdes JS, Polin RA. Sepsis screen in neonates with evaluation of plasma fibronectin. Pediatr Infect Dis J 1987;6:443--6.
- Greenberg DN, Yoder BA. Changes in the differential white blood cell count in screening for group B streptococcal sepsis. Pediatr Infect Dis J 1990;9:886--9.
- Ottolini MC, Lundgren K, Mirkinson LJ, Cason S, Ottolini MG. Utility of complete blood count and blood culture screening to diagnose neonatal sepsis in the asymptomatic at risk newborn. Pediatr Infect Dis J 2003;22:430--4.
- Christensen RD, Rothstein G, Hill HR, Hall RT. Fatal early onset group B streptococcal sepsis with normal leukocyte counts. Pediatr Infect Dis 1985;4:242--5.
- Newman TB, Puopolo KM, Wi S, Draper D, Escobar GJ. Interpreting complete blood counts soon after birth in newborns at risk for sepsis. Pediatrics 2010. In press.
- Siegel JD, Cushion NB. Prevention of early-onset group B streptococcal disease: another look at single-dose penicillin at birth. Obstet Gynecol 1996;87:692--8.
- Wendel GD Jr, Leveno KJ, Sanchez PJ, Jackson GL, McIntire DD, Siegel JD. Prevention of neonatal group B streptococcal disease: A combined intrapartum and neonatal protocol. Am J Obstet Gynecol 2002;186:618--26.
- Velaphi S, Siegel JD, Wendel GD Jr, Cushion N, Eid WM, Sanchez PJ. Early-onset group B streptococcal infection after a combined maternal and neonatal group B streptococcal chemoprophylaxis strategy. Pediatrics 2003;111:541--7.
- Matteson KA, Lievense SP, Catanzaro B, Phipps MG. Intrapartum group B streptococci prophylaxis in patients reporting a penicillin allergy. Obstet Gynecol 2008;111(2 Pt 1):356--64.
- Lukacs S, Schuchat A, Schoendorf K. National estimates of newborn sepsis: United States, 1990--2002. Meeting of the Society for Pediatric and Perinatal Epidemiologic Research, Salt Lake City, Utah; June 14--15, 2004.
- Eberly MD, Rajnik M. The effect of universal maternal screening on the incidence of neonatal early-onset group B streptococcal disease. Clin Pediatr (Phila) 2009;48:369--75.
- US Department of Health and Human Services. Healthy people 2010: understanding and improving health. 2nd ed. United States Government Printing Office; 2000.
- Cordero L, Sananes M, Ayers LW. Bloodstream infections in a neonatal intensive-care unit: 12 years' experience with an antibiotic control program. Infect Control Hosp Epidemiol 1999;20:242--6.
- Main EK, Slagle T. Prevention of early-onset invasive neonatal group B streptococcal disease in a private hospital setting: the superiority of culture-based protocols. Am J Obstet Gynecol 2000;182:1344--54.
- Baltimore RS, Huie SM, Meek JI, Schuchat A, O'Brien KL. Early-onset neonatal sepsis in the era of group B streptococcal prevention. Pediatrics 2001;108:1094--8.
- Edwards RK, Jamie WE, Sterner D, Gentry S, Counts K, Duff P. Intrapartum antibiotic prophylaxis and early-onset neonatal sepsis patterns. Infect Dis Obstet Gynecol 2003;11:221--6.
- Alarcon A, Pena P, Salas S, Sancha M, Omenaca F. Neonatal early onset Escherichia coli sepsis: trends in incidence and antimicrobial resistance in the era of intrapartum antimicrobial prophylaxis. Pediatr Infect Dis J 2004;23:295--9.
- Rentz AC, Samore MH, Stoddard GJ, Faix RG, Byington CL. Risk factors associated with ampicillin-resistant infection in newborns in the era of group B streptococcal prophylaxis. Arch Pediatr Adolesc Med 2004;158:556--60.
- Sutkin G, Krohn MA, Heine RP, Sweet RL. Antibiotic prophylaxis and non-group B streptococcal neonatal sepsis. Obstet Gynecol 2005;105:581--6.
- Angstetra D, Ferguson J, Giles WB. Institution of universal screening for group B Streptococcus (GBS) from a risk management protocol results in reduction of early-onset GBS disease in a tertiary obstetric unit. Aust N Z J Obstet Gynaecol 2007;47:378--82.
- Puopolo K, Eichenwald E. No change in the incidence of ampicillin-resistant, neonatal, early-onset sepsis over 18 years. Pediatrics 2010;125:e1031--8.
- Isaacs D, Royle JA. Intrapartum antibiotics and early onset neonatal sepsis caused by group B Streptococcus and by other organisms in Australia. Australasian Study Group for Neonatal Infections. Pediatr Infect Dis J 1999;18:524--8.
- Daley AJ, Isaacs D. Ten-year study on the effect of intrapartum antibiotic prophylaxis on early onset group B streptococcal and Escherichia coli neonatal sepsis in Australasia. Pediatr Infect Dis J 2004;23:630--4.
- Joseph TA, Pyati SP, Jacobs N. Neonatal early-onset Escherichia coli disease: the effect of intrapartum ampicillin. Arch Pediatr Adolesc Med 1998 Jan;152:35--40.
- Towers CV, Carr MH, Padilla G, Asrat T. Potential consequences of widespread antepartal use of ampicillin. Am J Obstet Gynecol 1998;179:879--83.
- Levine EM, Ghai V, Barton JJ, Strom CM. Intrapartum antibiotic prophylaxis increases the incidence of gram-negative neonatal sepsis. Infectious diseases in Obstet Gynecol 1999;7:210--3.
- Bizzarro MJ, Dembry LM, Baltimore RS, Gallagher PG. Changing patterns in neonatal Escherichia coli sepsis and ampicillin resistance in the era of intrapartum antibiotic prophylaxis. Pediatrics 2008 Apr;121:689--96.
- Stoll BJ, Hansen N, Fanaroff AA, et al. Changes in pathogens causing early-onset sepsis in very-low-birth-weight infants. N Engl J Med 2002 ;347:240--7.
- Hyde TB, Hilger TM, Reingold A, Farley MM, O'Brien KL, Schuchat A. Trends in incidence and antimicrobial resistance of early-onset sepsis: population-based surveillance in San Francisco and Atlanta. Pediatrics 2002 Oct;110:690--5.
- Stoll BJ, Hansen NI, Higgins RD, et al. Very low birth weight preterm infants with early onset neonatal sepsis: the predominance of gram-negative infections continues in the National Institute of Child Health and Human Development Neonatal Research Network, 2002--2003. Pediatr Infect Dis J 2005;24:635--9.
- Al-Hasan MN, Lahr BD, Eckel-Passow JE, Baddour LM. Antimicrobial resistance trends of Escherichia coli bloodstream isolates: a population-based study, 1998--2007. J Antimicrob Chemother 2009;64:169--74.
- Mercer BM, Carr TL, Beazley DD, Crouse DT, Sibai BM. Antibiotic use in pregnancy and drug-resistant infant sepsis. Am J Obstet Gynecol 1999;181:816--21.
- Terrone DA, Rinehart BK, Einstein MH, Britt LB, Martin JN Jr, Perry KG. Neonatal sepsis and death caused by resistant Escherichia coli: possible consequences of extended maternal ampicillin administration. Am J Obstet Gynecol 1999;180(6 Pt 1):1345--8.
- Towers CV, Briggs GG. Antepartum use of antibiotics and early-onset neonatal sepsis: the next 4 years. Am J Obstet Gynecol 2002;187:495--500.
- Moore MR, Schrag SJ, Schuchat A. Effects of intrapartum antimicrobial prophylaxis for prevention of group-B-streptococcal disease on the incidence and ecology of early-onset neonatal sepsis. Lancet Infect Dis 2003;3:201--13.
- Schrag SJ, Hadler JL, Arnold KE, Martell-Cleary P, Reingold A, Schuchat A. Risk factors for invasive, early-onset Escherichia coli infections in the era of widespread intrapartum antibiotic use. Pediatrics 2006 ;118:570--6.
- Glasgow TS, Speakman M, Firth S, James B, Byington CL, Young PC. Clinical and economic outcomes for term infants associated with increasing administration of antibiotics to their mothers. Paediatr Perinat Epidemiol 2007;21:338--46.
- Balter S, Zell ER, O'Brien KL, et al. Impact of intrapartum antibiotics on the care and evaluation of the neonate. Pediatr Infect Dis J 2003;22:853--7.
- Davis RL, Hasselquist MB, Cardenas V, et al. Introduction of the new Centers for Disease Control and Prevention group B streptococcal prevention guideline at a large West Coast health maintenance organization. Am J Obstet Gynecol 2001;184:603--10.
- American College of Obstetricians and Gynecologists. Prevention of early-onset group B streptococcal disease in newborns. Obstet Gynecol 2002;100:1405--12.
- Bergqvist G, Holmberg G, Rydner T, Vaclavinkova V. Intrauterine death due to infection with group B Streptococci. Acta Obstet Gynecol Scand 1978;57:127--8.
- Tolockiene E, Morsing E, Holst E, et al. Intrauterine infection may be a major cause of stillbirth in Sweden. Acta obstetricia et gynecologica Scandinavica. 2001 Jun;80(6):511--8.
- Gibbs RS. The origins of stillbirth: infectious diseases. Seminars in perinatology. 2002 Feb;26(1):75--8.
- Goldenberg RL, Thompson C. The infectious origins of stillbirth. Am J Obstet Gynecol 2003 Sep;189(3):861--73.
- US Department of Health and Human Services. Proposed Healthy People 2020 objectives. Available at http://www.healthypeople.gov/hp2020/Objectives/TopicAreas.aspx.
- Schrag SJ, Whitney CG, Schuchat A. Neonatal group B streptococcal disease: how infection control teams can contribute to prevention efforts. Infect Control Hosp Epidemiol 2000;21:473--83.
FIGURE 1. Incidence of early- and late-onset invasive group B streptococcal (GBS) disease --- Active Bacterial Core surveillance areas, 1990--2008, and activities for prevention of GBS disease
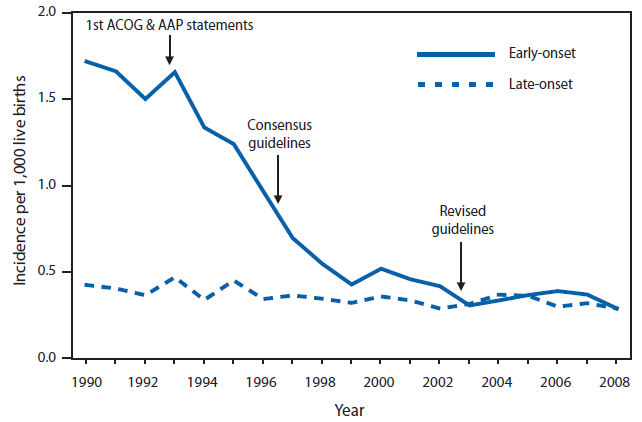
Abbreviations: ACOG = American College of Obstetricians and Gynecologists and AAP = American Academy of Pediatrics.
Source: Adapted from Jordan HT, Farley MM, Craig A, et al. Revisiting the need for vaccine prevention of late-onset neonatal group B streptococcal disease. Pediatr Infect Dis J 2008;27:1057--64.
* Incidence rates for 2008 are preliminary because the live birth denominator has not been finalized.
Alternate Text: This figure shows incidence per 1,000 live births of early- and late-onset invasive group B streptococcal (GBS) disease in the 10 Active Bacterial Core surveillance areas during 1990-2008. The figure tracks the steady decline in early-onset GBS as GBS-prevention recommendations were implemented.
FIGURE 2. Percentage of pregnant women screened for group B streptococcal colonization --- Active Bacterial Core surveillance areas, 1998--1999 and 2003--2004*
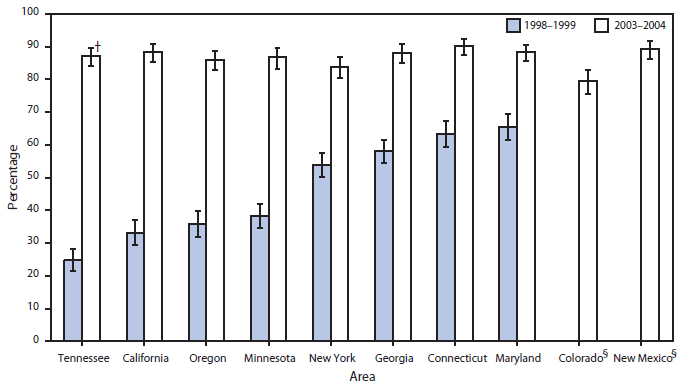
Source: Van Dyke MK, Phares CR, Lynfield R, Thomas AR, Arnold KE, Craig AS, et al. Evaluation of universal antenatal screening for group B Streptococcus. N Engl J Med 2009;360:2626--36.
* Reported values are weighted to account for the stratified survey design. The number of charts abstracted was 5,144 for 1998--1999 and 7,691 for 2003--2005.
† 95% confidence inerval.
§ Data for 1998--1999 not available.
Alternate Text: The figure shows the percentage of pregnant women who were screened for group B streptococcal colonization in the 10 Active Bacterial Core surveillance areas during 1998-1999 and 2003-2004. In the eight areas that conducted screening in both periods, the percentage of women screened increased from 1998-1999 to 2003-2004.
FIGURE 3. Percentage of women with an indication who received intrapartum antibiotic prophylaxis --- Active Bacterial Core surveillance areas, 1998--1999 and 2003--2004*
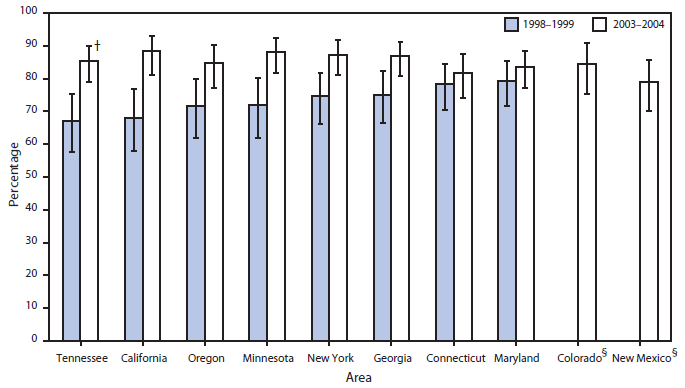
Source: Van Dyke MK, Phares CR, Lynfield R, Thomas AR, Arnold KE, Craig AS, et al. Evaluation of universal antenatal screening for group B Streptococcus. N Engl J Med 2009;360:2626--36.
* Reported values are weighted to account for the stratified survey design. The number of charts abstracted was 5,144 for 1998--1999 and 7,691 for 2003--2005.
† 95% confidence inerval.
§ Data for 1998--1999 not available.
Alternate Text: The figure shows the percentage of women with an indication who received intrapartum antibiotic prophylaxis in the 10 Active Bacterial Core surveillance areas during 1998-1999 and 2003-2004. In the eight areas that provided intrapartum antibiotic prophylaxis in both periods, the percentage of women who received prophylaxis increased from 1998-1999 to 2003-2004.
FIGURE 4. Incidence of early-onset invasive group B streptococcal disease, stratified by race and term --- Active Bacterial Core surveillance areas, 2000--2007
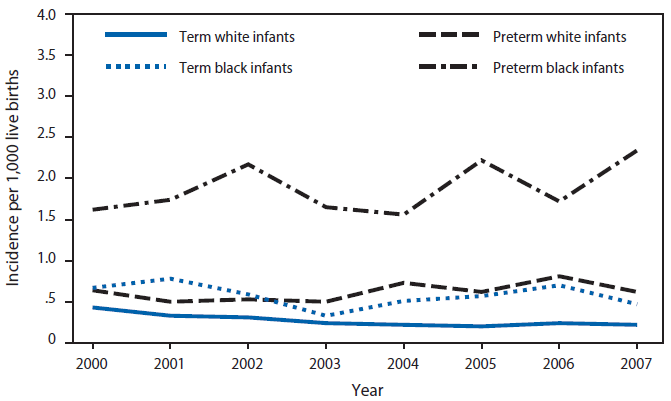
Source: Adapted from CDC. Trends in perinatal group B streptococcal disease---United States, 2000--2006. MMWR 2009;58:109--12.
Alternate Text: The figure shows incidence per 1,000 live births of early-onset invasive group B streptococcal disease in the 10 Active Bacterial Core surveillance areas during 2000-2007. Data are displayed for four demographic subsets: term white infants, term black infants, preterm white infants, and preterm black infants.
FIGURE 5. Algorithm for screening for group B streptococcal (GBS) colonization and use of intrapartum prophylaxis for women with preterm* labor (PTL)
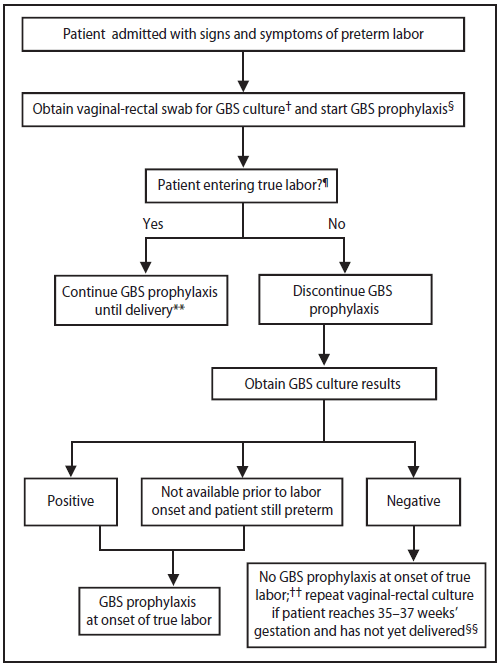
* At <37 weeks and 0 days' gestation.
† If patient has undergone vaginal-rectal GBS culture within the preceding 5 weeks, the results of that culture should guide management. GBS-colonized women should receive intrapartum antibiotic prophylaxis. No antibiotics are indicated for GBS prophylaxis if a vaginal-rectal screen within 5 weeks was negative.
§ See Figure 8 for recommended antibiotic regimens.
¶ Patient should be regularly assessed for progression to true labor; if the patient is considered not to be in true labor, discontinue GBS prophylaxis.
** If GBS culture results become available prior to delivery and are negative, then discontinue GBS prophylaxis.
†† Unless subsequent GBS culture prior to delivery is positive.
§§ A negative GBS screen is considered valid for 5 weeks. If a patient with a history of PTL is re-admitted with signs and symptoms of PTL and had a negative GBS screen >5 weeks prior, she should be rescreened and managed according to this algorithm at that time.
Alternate Text: The figure presents an algorithm for clinicians to use to determine whether to administer GBS intrapartum prophylaxis for women with preterm labor.
FIGURE 6. Algorithm for screening for group B streptococcal (GBS) colonization and use of intrapartum prophylaxis for women with preterm* premature rupture of membranes (pPROM)
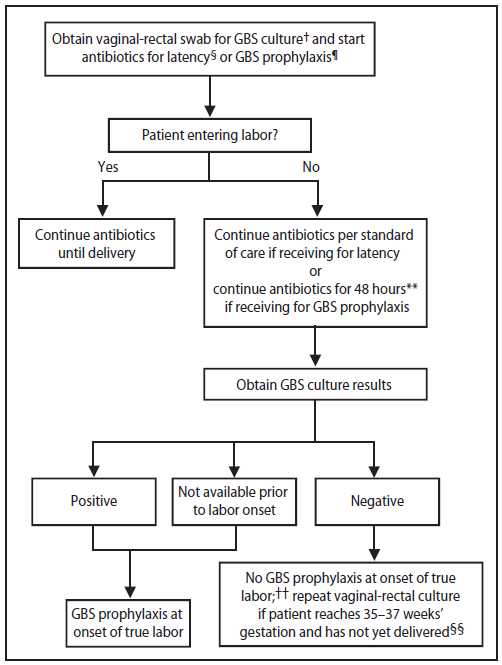
* At <37 weeks and 0 days' gestation.
† If patient has undergone vaginal-rectal GBS culture within the preceding 5 weeks, the results of that culture should guide management. GBS-colonized women should receive intrapartum antibiotic prophylaxis. No antibiotics are indicated for GBS prophylaxis if a vaginal-rectal screen within 5 weeks was negative.
§ Antibiotics given for latency in the setting of pPROM that include ampicillin 2 g intravenously (IV) once, followed by 1 g IV every 6 hours for at least 48 hours are adequate for GBS prophylaxis. If other regimens are used, GBS prophylaxis should be initiated in addition.
¶ See Figure 8 for recommended antibiotic regimens.
** GBS prophylaxis should be discontinued at 48 hours for women with pPROM who are not in labor. If results from a GBS screen performed on admission become available during the 48-hour period and are negative, GBS prophylaxis should be discontinued at that time.
†† Unless subsequent GBS culture prior to delivery is positive.
§§ A negative GBS screen is considered valid for 5 weeks. If a patient with pPROM is entering labor and had a negative GBS screen >5 weeks prior, she should be rescreened and managed according to this algorithm at that time.
Alternate Text: The figure presents an algorithm for clinicians to use to determine whether to administer GBS intrapartum prophylaxis for women with preterm pPROM.
|
BOX 2. Procedures for processing clinical specimens for culture of group B Streptococcus (GBS) (see Figure 7) |
|
|
* Before the inoculation step, laboratories may choose to roll the vaginal-rectal swab(s) on a blood agar plate with or without colistin and nalidixic acid or commercially available chromogenic agar (appropriate recommendations include chromID Strepto B [which might detect both hemolytic and nonhemolytic GBS] or Granada Agar [which detects hemolytic GBS]. Source: Tazi A, Réglier-Poupet H, Dautezac F, Raymond J, Poyart C. Comparative evaluation of Strepto B ID chromogenic medium and Granada media for the detection of group B Streptococcus from vaginal samples of pregnant women. J Microbiol Methods 2008;73:263--5). This approach should be taken only in addition to, and not instead of, inoculation into selective broth. The directly inoculated blood agar plate should be streaked for isolation, incubated at 35°--37°C in ambient air or 5% CO2 for 18--24 hours and inspected for organisms suggestive of GBS as described above. If suspected colonies are confirmed as GBS, the selective broth can be discarded, thus shortening the time to obtaining culture results. The directly inoculated chromogenic agar should be streaked for isolation and incubated at 35°--37°C for 18--24 hours. Hemolytic GBS isolates are identified by colored colonies as directed by specific manufacturers' instructions, and selective broth can be discarded if GBS positive. † Source: Fenton LJ, Harper MH. Evaluation of colistin and nalidixic acid in Todd-Hewitt broth for selective isolation of groupB streptococci. J Clin Microbiol 1979;9:167--9. Although Trans-Vag medium often is available without sheep blood, direct comparison of medium with and without sheep blood has shown higher yield when blood is added. Lim broth also might benefit from the addition of sheep blood, although the improvement in yield is smaller, and sufficient data are not yet available to support a recommendation. § Sources: Church DL, Baxter H, Lloyd T, Miller B, Elsayed S. Evaluation of StrepB carrot broth versus Lim broth for detection of group B Streptococcus colonization status of near-term pregnant women. J Clin Microbiol 2008;46:2780--2. Martinho F, Prieto E, Pinto D, Castro RM, Morais AM, Salgado L, Exposto Fda L. Evaluation of liquid biphasic Granada medium and instant liquid biphasic Granada medium for group B Streptococcus detection. Enferm Infecc Microbiol Clin 2008;26:69--71. ¶ Source: de la Rosa M, Perez M, Carazo C, Pareja L, Peis JI, Hernandez F. New Granada medium for detection and identification of group B streptococci. J Clin Microbiol 1992;30:1019--21. ** Direct latex agglutination, probe detection or nucleic acid amplification testing on enriched selective broth is an additional option. Sources: Guerrero C, Martinez J, Menasalvas A, Blazquez R, Rodriguez, Segovia M. Use of direct latex agglutination testing of selective broth in the detection of group B streptococcal carriage in pregnant women. Eur J Clin Microbiol Infect Dis 2004;23:61--2. Goodrich JS, Miller MB. Comprison of culture and 2 real-time polymerase chain reaction assays to detect group B Streptococcus during antepartum screening. Diagn Microbiol Infect Dis 2007;59:17--22. Block T, Munson E, Culver A, Vaughan K, Hryciuk JE. Comparison of carrot broth- and selective Todd-Hewitt broth-enhanced PCR protocols for real-time detection of Streptococcus agalactiae in prenatal vaginal/anorectal specimens. J Clin Microbiol 2008;46:3615--20. Montague NS, Cleary TJ, Martinez OV, Procop GW. Detection of group B streptococci in Lim broth by use of group B Streptococcus peptide nucleic acid fluorescent in situ hybridization and selective and nonselective agars. J Clin Microbiol 2008 46:3470--2. If a rapid test performed on enriched broth yields positive results and antimicrobial susceptibility testing is recommended (for penicillan-allergic women at high risk for anaphylaxis), the enriched broth should be subcultured to obtain an isolate. |
FIGURE 7. Algorithm for recommended laboratory testing for prenatal screening for group B streptococcal (GBS) colonization*
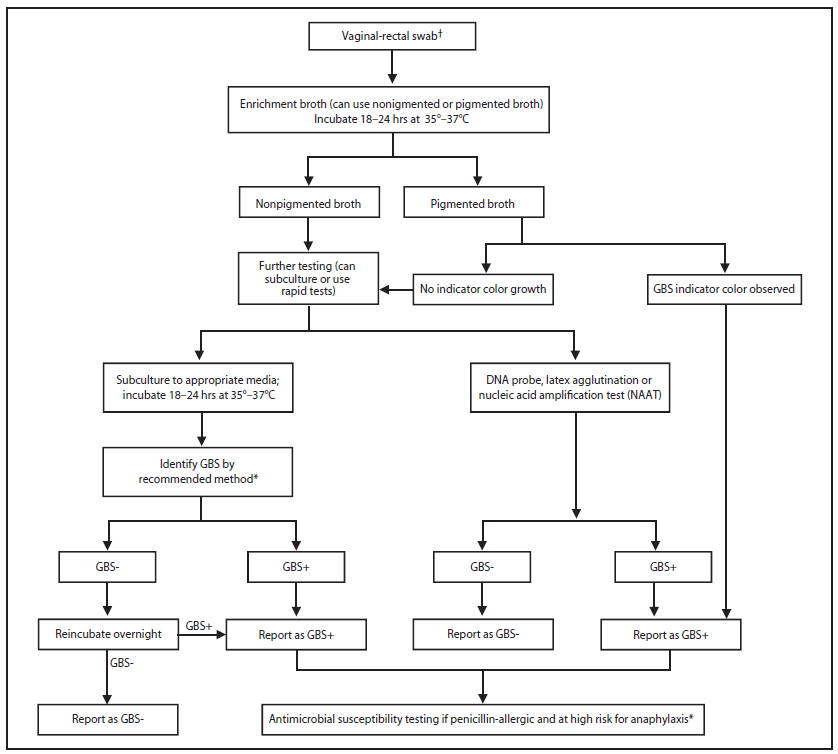
* See Boxes 1--3 for details on specimen processing and antimicrobial susceptibility testing.
† Direct plating with appropriate media may be done in addition to enriched culture. Direct plating should not be used as the sole means to identify GBS.
Alternate Text: The figure presents an algorithm for laboratorians to use when testing for prenatal screening for group B streptococcal (GBS) colonization.
FIGURE 8. Recommended regimens for intrapartum antibiotic prophylaxis for prevention of early-onset group B streptococcal (GBS) disease*
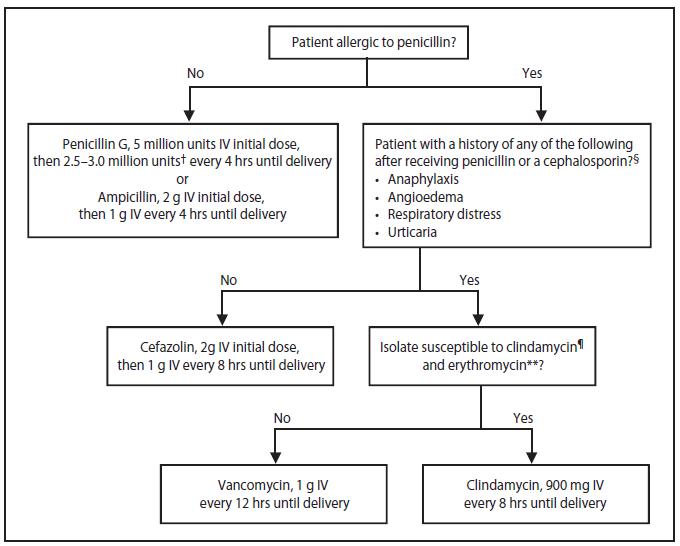
Abbreviation: IV = intravenously.
* Broader spectrum agents, including an agent active against GBS, might be necessary for treatment of chorioamnionitis.
† Doses ranging from 2.5 to 3.0 million units are acceptable for the doses administered every 4 hours following the initial dose. The choice of dose within that range should be guided by which formulations of penicillin G are readily available to reduce the need for pharmacies to specially prepare doses.
§ Penicillin-allergic patients with a history of anaphylaxis, angioedema, respiratory distress, or urticaria following administration of penicillin or a cephalosporin are considered to be at high risk for anaphylaxis and should not receive penicillin, ampicillin, or cefazolin for GBS intrapartum prophylaxis. For penicillin-allergic patients who do not have a history of those reactions, cefazolin is the preferred agent because pharmacologic data suggest it achieves effective intraamniotic concentrations. Vancomycin and clindamycin should be reserved for penicillin-allergic women at high risk for anaphylaxis.
¶ If laboratory facilities are adequate, clindamycin and erythromycin susceptibility testing (Box 3) should be performed on prenatal GBS isolates from penicillin-allergic women at high risk for anaphylaxis. If no susceptibility testing is performed, or the results are not available at the time of labor, vancomycin is the preferred agent for GBS intrapartum prophylaxis for penicillin-allergic women at high risk for anaphylaxis.
** Resistance to erythromycin is often but not always associated with clindamycin resistance. If an isolate is resistant to erythromycin, it might have inducible resistance to clindamycin, even if it appears susceptible to clindamycin. If a GBS isolate is susceptible to clindamycin, resistant to erythromycin, and testing for inducible clindamycin resistance has been performed and is negative (no inducible resistance), then clindamycin can be used for GBS intrapartum prophylaxis instead of vancomycin.
Alternate Text: The figure presents an algorithm for clinicians to use in determining which regimen to follow for administering intrapartum antibiotic prophylaxis to prevent early-onset GBS disease.
FIGURE 9. Algorithm for secondary prevention of early-onset group B streptococcal (GBS) disease among newborns
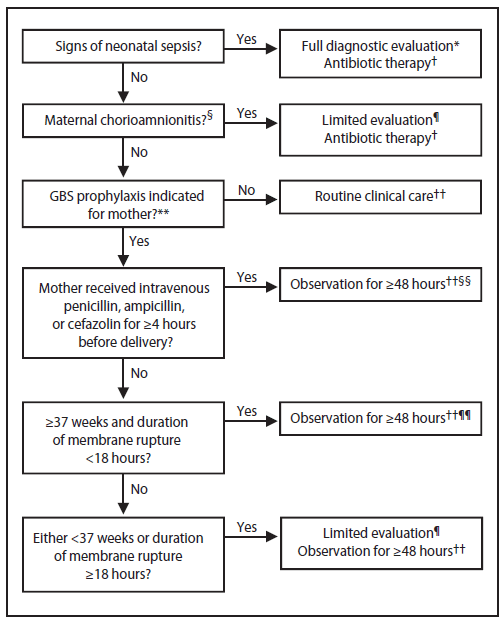
* Full diagnostic evaluation includes a blood culture, a complete blood count (CBC) including white blood cell differential and platelet counts, chest radiograph (if respiratory abnormalities are present), and lumbar puncture (if patient is stable enough to tolerate procedure and sepsis is suspected).
† Antibiotic therapy should be directed toward the most common causes of neonatal sepsis, including intravenous ampicillin for GBS and coverage for other organisms (including Escherichia coli and other gram-negative pathogens) and should take into account local antibiotic resistance patterns.
§ Consultation with obstetric providers is important to determine the level of clinical suspicion for chorioamnionitis. Chorioamnionitis is diagnosed clinically and some of the signs are nonspecific.
¶ Limited evaluation includes blood culture (at birth) and CBC with differential and platelets (at birth and/or at 6--12 hours of life).
** See table 3 for indications for intrapartum GBS prophylaxis.
†† If signs of sepsis develop, a full diagnostic evaluation should be conducted and antibiotic therapy initiated.
§§ If ≥37 weeks' gestation, observation may occur at home after 24 hours if other discharge criteria have been met, access to medical care is readily available, and a person who is able to comply fully with instructions for home observation will be present. If any of these conditions is not met, the infant should be observed in the hospital for at least 48 hours and until discharge criteria are achieved.
¶¶ Some experts recommend a CBC with differential and platelets at age 6--12 hours.
Alternate Text: The figure presents an algorithm for clinicians to use for secondary prevention of early-onset group B streptococcal (GBS) disease among newborns.
Group B Streptococcus Technical Working Group*
Members: Kathryn Arnold, MD, Georgia Division of Public Health, Barbara Stoll, MD, Yun Wang, MD, PhD, Emory University School of Medicine, Atlanta Georgia; Carol Baker, MD Baylor College of Medicine, Houston, Texas; Carrie Byington, MD, American Academy of Pediatrics/Committee on Infectious Diseases, Richard Polin MD, American Academy of Pediatrics/Committee on Fetus and Newborn, Elk Grove Village, Illinois; Ronald Gibbs, MD, University of Colorado School of Medicine, Denver, Colorado; Jeanne Jordan, PhD, George Washington University School of Public Health and Health Services, Sarah Kilpatrick, MD, PhD, American College of Obstetricians and Gynecologists, District of Columbia; Geraldine Hall, PhD, Cleveland Clinic Lerner College of Medicine of Case Western Reserve University, Cleveland, Ohio; Tekoa King, MPH, American College of Nurse Midwives, Silver Spring, Maryland; Ruth Lynfield, MD, Minnesota Department of Health, Minneapolis, Minnesota; Marti Perhach, Group B Strep International, Pomona, California; Laura Riley, MD, Massachusetts General Hospital, Boston, Massachusetts; Pablo Sanchez, MD; Society for Healthcare Epidemiology of America, Arlington, Virginia; Pamela Simms, PhD, PharmD, Samford University McWhorter School of Pharmacy, Birmingham, Alabama; Julie Wood, MD, American Academy of Family Physicians, Leawood, Kansas; Rex Astles, PhD, Bernard Beall, PhD, Roberta Carey, PhD, Janine Corey, MPH, Lee Hampton, MD, Denise Jamieson, MD, Melissa Lewis, MPH, Michael Miller, PhD, Christine Olson, MD, Alison Patti, MPH, Emily Weston, MPH, Cynthia Whitney, MD, Elizabeth Zell, MStat, CDC, Atlanta, Georgia.
* All working group members were asked to disclose any potential conflict of interest. Ronald Gibbs disclosed receiving a consulting fee from Novartis for consulting on potential vaccine complications (unrelated to GBS); Lee Hampton disclosed owning shares in General Electric; and Laura Riley disclosed receiving an honorarium from Up To Date for services as a writer.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All MMWR HTML versions of articles are electronic conversions from typeset documents.
This conversion might result in character translation or format errors in the HTML version.
Users are referred to the electronic PDF version (http://www.cdc.gov/mmwr)
and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S.
Government Printing Office (GPO), Washington, DC 20402-9371;
telephone: (202) 512-1800. Contact GPO for current prices.
**Questions or messages regarding errors in formatting should be addressed to
mmwrq@cdc.gov.


